Causes of peri orbial region swelling and what would be treatment
Reading File
Finding Sources
Finding Sources
Searching PubMed
periorbital edema causes management
Finding Sources
Finding Sources
Searching the Web
periorbital swelling causes differential diagnosis treatment 2024
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive overview of periorbital (periocular) region swelling — its causes and treatment:
Periorbital (Periocular) Region Swelling
Anatomy — The Key Landmark: The Orbital Septum
The orbital septum is a connective tissue extension of the orbital periosteum that extends into the upper and lower eyelids. It divides periorbital swelling into two critical categories:
- Preseptal (periorbital/anterior) — anterior to the orbital septum → generally manageable, lower risk
- Postseptal (orbital/posterior) — posterior to the orbital septum → vision- and life-threatening emergency
Causes of Periorbital Swelling
1. Infectious Causes
A. Preseptal (Periorbital) Cellulitis — Most Common Infectious Cause
The infection is anterior to the orbital septum, confined to eyelid and periocular soft tissues.
Sources of infection:
- Upper respiratory tract infections / paranasal sinusitis (most common)
- Local spread from hordeolum (stye), chalazion, conjunctivitis, dacryoadenitis, dacryocystitis
- Insect bites, minor trauma, small scratches
- Hematogenous spread (especially in children <18 months)
Organisms: S. aureus, S. epidermidis, Streptococcus spp., S. pneumoniae, anaerobes; H. influenzae (now rare since Hib vaccine)
Clinical features: Erythema, warmth, tenderness, eyelid edema — no proptosis, no restricted eye movement, no pain on eye movement, normal visual acuity
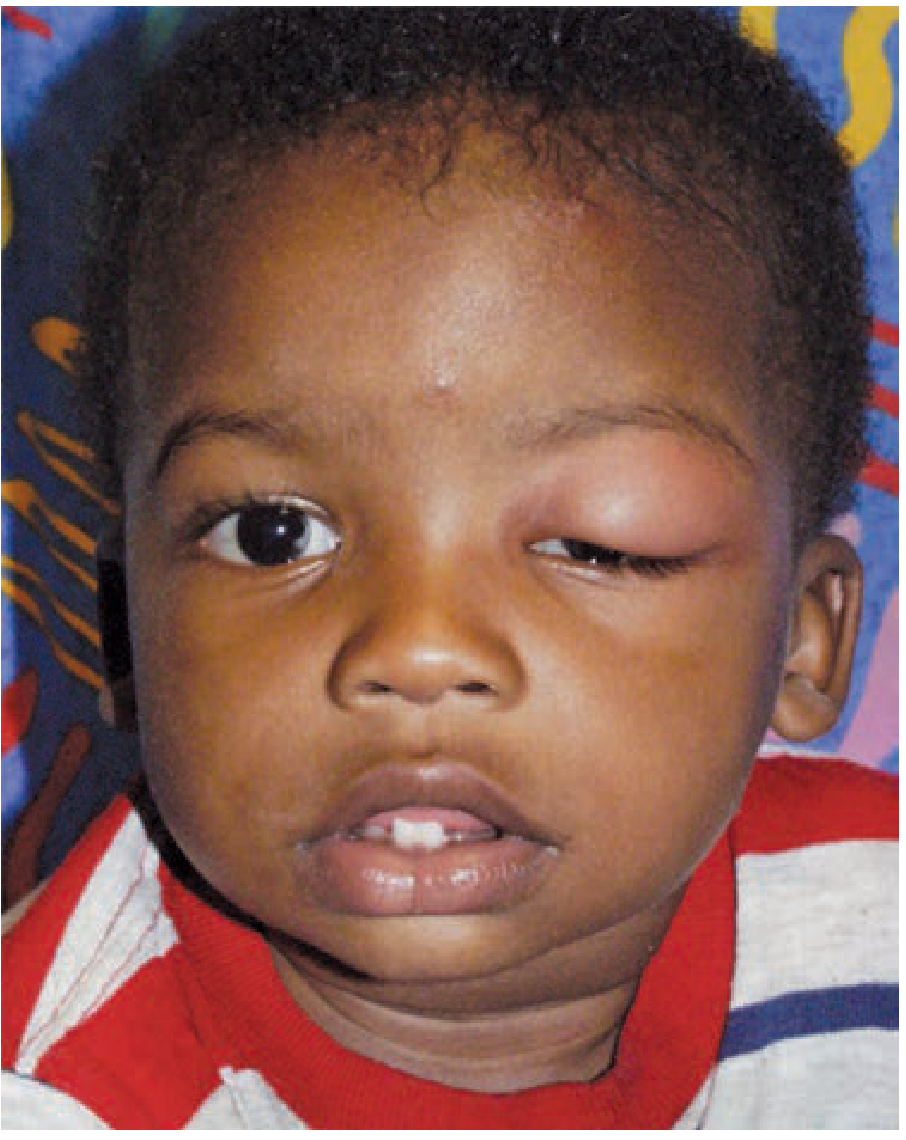
B. Postseptal (Orbital) Cellulitis — Emergent
Infection posterior to the orbital septum, usually from sinusitis (ethmoid sinus most common, via lamina papyracea).
Clinical features: Fever, proptosis, restricted extraocular movements, chemosis, pain with eye movement, decreased visual acuity
Organisms: Polymicrobial — S. aureus, S. pneumoniae, anaerobes (Bacteroides, Fusobacterium); mucormycosis in diabetics/immunocompromised
Complications if untreated: Subperiosteal abscess → orbital abscess → cavernous sinus thrombosis → meningitis, subdural empyema, brain abscess
C. Other Infectious Causes
| Condition | Key Features |
|---|---|
| Hordeolum (Stye) | Focal eyelid swelling at lash line (external) or inner tarsal surface (internal); Staphylococcus |
| Dacryocystitis | Swelling over lacrimal sac (medial canthal area), tearing, discharge |
| Dacryoadenitis | Swelling of lacrimal gland (temporal upper eyelid) |
| Herpes Zoster Ophthalmicus | Vesicular rash along V1 trigeminal dermatome |
| Herpes Simplex | Vesicular lid lesions |
| Infectious Mononucleosis | Bilateral periorbital edema early in illness |
| Mucormycosis | Diabetics/immunocompromised; tissue necrosis, rapid progression |
2. Allergic / Inflammatory Causes
- Allergic reaction / angioedema — bilateral, non-painful, pruritic; rapid onset; may involve lips/tongue (anaphylaxis risk)
- Contact dermatitis — pruritic, weeping eyelid skin; exposure history
- Atopic/chronic allergic conjunctivitis
- Insect bite — unilateral, history of bite
3. Systemic / Medical Causes
| Cause | Mechanism |
|---|---|
| Nephrotic syndrome | Hypoalbuminemia → fluid leaks; bilateral periorbital edema, often worse in mornings (classic in children) |
| Hypothyroidism | Myxedematous infiltration; bilateral non-pitting periorbital fullness |
| Graves' disease / Thyroid Eye Disease | Glycosaminoglycan deposition in orbital fat + muscles; proptosis + eyelid retraction |
| Superior vena cava syndrome | Bilateral periorbital + facial edema; venous distension of neck/chest |
| Congestive heart failure | Generalized fluid retention; bilateral |
| Hypoalbuminemia (liver disease, malnutrition) | Low oncotic pressure → generalized edema |
4. Traumatic Causes
- Blunt orbital trauma — periorbital ecchymosis ("black eye"), hematoma
- Retrobulbar hemorrhage — proptosis, raised intraocular pressure; surgical emergency
- Orbital fractures — may cause subcutaneous emphysema
5. Neoplastic Causes
- Orbital tumors (rhabdomyosarcoma in children, lymphoma, metastases) — gradual onset, no fever
- Orbital pseudotumor (idiopathic orbital inflammation) — painful proptosis
6. Other / Lifestyle Causes
- Chronic sleep deprivation, high-salt diet, excess alcohol
- Crying (transient)
- Aging (fat herniation, reduced lymphatic drainage)
🚩 Red Flags (Require Urgent Assessment)
| Finding | Concern |
|---|---|
| Pain with eye movement | Orbital cellulitis |
| Proptosis | Retrobulbar process (abscess, hemorrhage) |
| Decreased visual acuity | Optic nerve compromise |
| Restricted extraocular movements | Orbital cellulitis |
| Bilateral periorbital edema in a child | Nephrotic syndrome |
| Lip/tongue swelling + dyspnea | Anaphylaxis/angioedema |
| Fever + altered mental status | Cavernous sinus thrombosis |
Diagnosis
- Clinical exam: Check visual acuity, extraocular movements, proptosis, and skin findings
- CT orbits + sinuses (contrast-enhanced): Gold standard to differentiate preseptal from postseptal cellulitis; identifies subperiosteal abscess
- MRI: Better soft tissue detail, useful for cavernous sinus thrombosis
- Labs: CBC, CRP, blood cultures (for systemic illness); urinalysis/protein for nephrotic syndrome; TFTs for thyroid disease
Treatment
Preseptal Cellulitis
| Severity | Management |
|---|---|
| Mild, afebrile, well-appearing (usually outpatient) | Amoxicillin-clavulanate 20 mg/kg PO twice daily × 7–10 days |
| Moderate/severe or suspected hematogenous spread | Hospitalize + IV antibiotics: Cefuroxime 50 mg/kg IV q8h, or Ceftriaxone 50 mg/kg IV q12h, or Ampicillin-sulbactam 50 mg/kg IV q6h |
| MRSA suspected | Add Vancomycin IV |
Postseptal (Orbital) Cellulitis — Inpatient Emergency
- Ophthalmology consult immediately
- IV broad-spectrum antibiotics with aerobic + anaerobic coverage:
- Vancomycin + 3rd-generation cephalosporin (ceftriaxone)
- Alternatives: Piperacillin-tazobactam, imipenem, or meropenem
- Add metronidazole or clindamycin for anaerobic coverage
- Nasal decongestant (e.g., oxymetazoline) as adjuvant
- Emergent lateral canthotomy if elevated intraocular pressure or optic neuropathy
- Surgical drainage + debridement for subperiosteal/orbital abscess
Other Specific Treatments
| Cause | Treatment |
|---|---|
| Hordeolum/Chalazion | Warm compresses 4×/day; topical antibiotics; incision & drainage if persistent |
| Dacryocystitis | Warm compresses; systemic antibiotics; dacryocystorhinostomy (DCR) for recurrent cases |
| Allergic/Angioedema | Antihistamines (cetirizine, loratadine); oral corticosteroids; epinephrine 0.3–0.5 mg IM for anaphylaxis |
| Nephrotic syndrome | Treat underlying cause; diuretics (furosemide); corticosteroids (for minimal change disease) |
| Thyroid eye disease | Selenium; IV glucocorticoids; orbital decompression in severe cases |
| Herpes zoster ophthalmicus | Oral acyclovir/valacyclovir within 72h; topical steroids for keratitis |
| Retrobulbar hemorrhage | Emergent lateral canthotomy + cantholysis |
| Trauma/hematoma | Cold compresses; elevation; CT to rule out fracture/hemorrhage |
Summary Algorithm
Periorbital Swelling
│
├── Proptosis / restricted EOM / ↓vision?
│ YES → CT orbits → Orbital cellulitis / abscess → ADMIT + IV Abx
│ NO ↓
├── Infectious features (erythema, warmth, fever)?
│ YES → Preseptal cellulitis → Oral or IV Abx based on severity
├── Allergic features (pruritus, bilateral, rapid onset)?
│ YES → Antihistamines ± steroids; check for anaphylaxis
├── Bilateral, morning predominance, child?
│ YES → Rule out Nephrotic syndrome (urine protein)
└── Systemic features?
YES → TFTs (thyroid), echo (cardiac), albumin/LFTs
Sources: Tintinalli's Emergency Medicine, 9th Ed.; StatPearls — Periorbital Cellulitis; WikEM — Periorbital Swelling
This is a shared conversation. Sign in to Orris to start your own chat.