Parathyroid adenoma in detail
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching PubMed
"parathyroid adenoma" AND "primary hyperparathyroidism"
Reading File
Reading File
Reading File
Loading Image
Parathyroid adenoma: detailed overview
A parathyroid adenoma is a benign neoplasm of parathyroid tissue, usually from chief cells, that autonomously secretes parathyroid hormone (PTH) and causes primary hyperparathyroidism (PHPT). It is the commonest cause of PHPT.
1) Epidemiology and importance
- PHPT is a common endocrine disorder and a major cause of hypercalcemia.
- Underlying lesion frequencies in PHPT:
- Adenoma: 85 to 95%
- Hyperplasia: 5 to 10%
- Carcinoma: around 1%
- Typical patient profile: adults, often over 50, female predominance.
(From Robbins pathology texts and related endocrine chapters.)
2) Pathophysiology
Normal feedback: rising calcium suppresses PTH via calcium-sensing receptor (CaSR).
In adenoma: this feedback set point is shifted, so PTH remains inappropriately elevated (or “normal but unsuppressed”) despite hypercalcemia.
In adenoma: this feedback set point is shifted, so PTH remains inappropriately elevated (or “normal but unsuppressed”) despite hypercalcemia.
PTH excess causes:
- Increased bone resorption
- Increased distal tubular calcium reabsorption
- Increased phosphaturia
- Increased 1,25-dihydroxyvitamin D production
Net biochemical pattern in classic PHPT:
- High calcium
- Low/low-normal phosphate
- Elevated or inappropriately normal PTH
3) Molecular biology and genetics
Commonly implicated pathways:
- Cyclin D1 (CCND1) dysregulation (gene rearrangement/overexpression)
- MEN1 mutations in a subset of sporadic tumors
- CDC73 alterations are more linked to carcinoma/atypical neoplasms, but can occasionally occur in adenoma contexts
Familial syndromic associations to remember:
- MEN1, MEN2A, MEN4
- Hyperparathyroidism-jaw tumor syndrome (CDC73 related)
4) Pathology (gross and microscopic)
Typical adenoma features:
- Solitary, well-circumscribed, encapsulated tan to reddish-brown nodule
- Usually about 0.5 to 5 g
- Remaining glands often normal or shrunken (feedback suppression)
Microscopy:
- Predominantly chief cells in sheets/nests
- Reduced stromal fat compared with normal gland
- Can show endocrine atypia (nuclear pleomorphism) without malignancy
- Mitotic figures uncommon
Histology image example
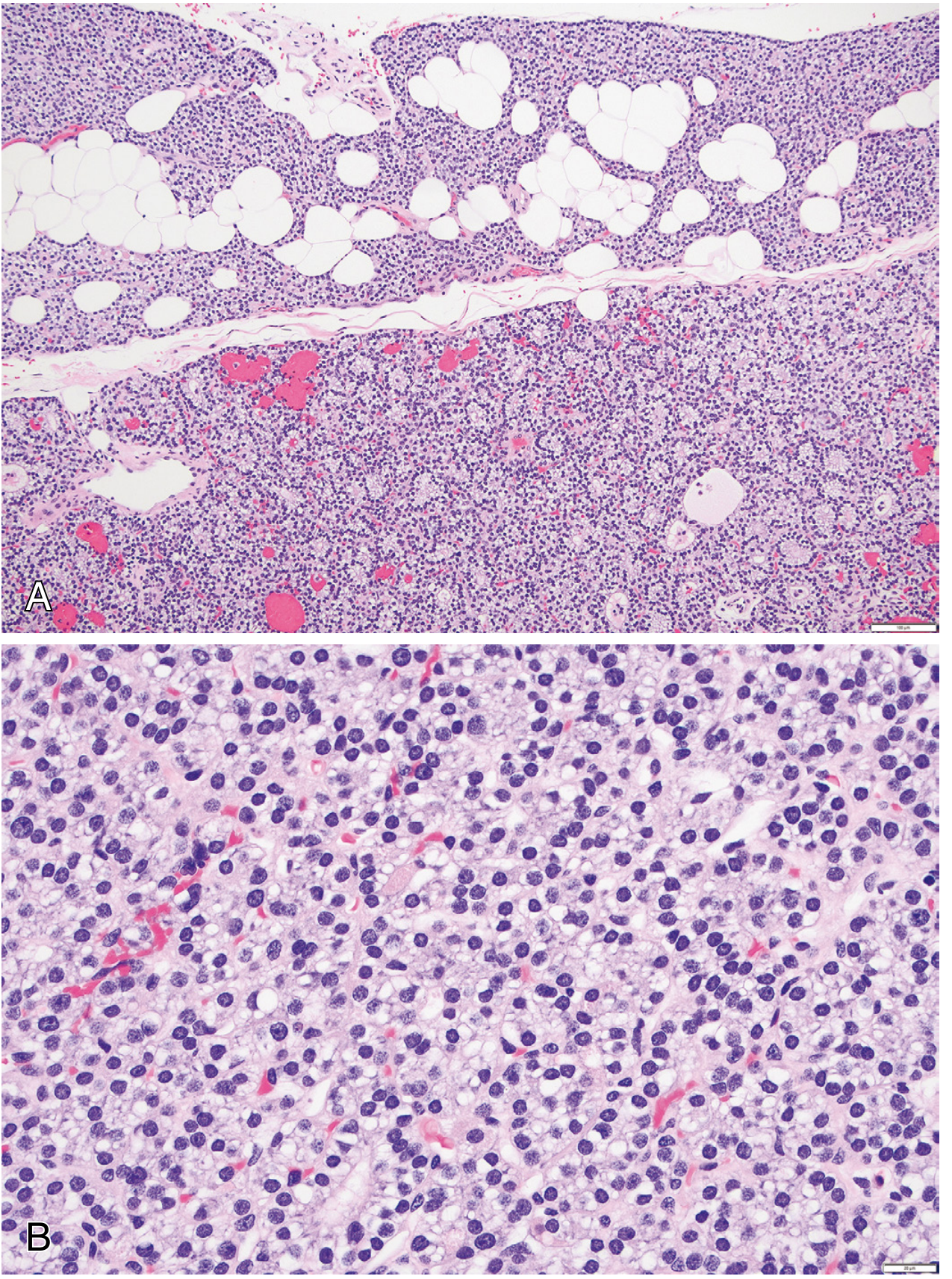
- Panel A shows adenoma tissue demarcated from residual fat-containing non-neoplastic parathyroid.
- Panel B shows monotonous chief-cell proliferation at higher power.
5) Clinical presentation
Many patients are now diagnosed incidentally during routine labs (asymptomatic hypercalcemia).
Classic symptomatic pattern, when present:
Classic symptomatic pattern, when present:
- “Bones”: bone pain, osteoporosis, osteitis fibrosa cystica, brown tumors
- “Stones”: nephrolithiasis, nephrocalcinosis
- “Groans”: GI symptoms (constipation, nausea, abdominal complaints, pancreatitis in some cases)
- “Psychic moans”: fatigue, mood/cognitive symptoms, depression, lethargy
Severe longstanding disease can produce significant skeletal and renal complications.
6) Diagnosis
Diagnosis is biochemical first; imaging is for localization before surgery, not for making PHPT diagnosis.
Typical workup:
- Serum total and/or ionized calcium
- Intact PTH
- Phosphate, creatinine/eGFR
- 25-hydroxyvitamin D
- 24-hour urinary calcium (important to distinguish from familial hypocalciuric hypercalcemia)
- Bone mineral density (DXA), renal imaging in selected cases
Biochemical phenotypes include:
- Hypercalcemic PHPT (most common)
- Normohormonal PHPT (high Ca with unsuppressed PTH)
- Normocalcemic PHPT (selected cases, after secondary causes excluded)
7) Imaging/localization modalities
Used after biochemical confirmation, especially when minimally invasive surgery is planned:
- High-resolution neck ultrasound
- Tc-99m sestamibi scintigraphy (often with SPECT/CT)
- 4D-CT (useful in discordant/negative first-line imaging, ectopic/small lesions)
- MRI or PET/CT for difficult/reoperative cases
Key point: localization sensitivity varies; if noninvasive localization fails, bilateral four-gland exploration may still be done.
8) Treatment
Definitive treatment for eligible patients: parathyroidectomy.
Approaches:
- Focused/minimally invasive parathyroidectomy when localization is concordant
- Bilateral neck exploration when localization unclear, concern for multigland disease, or reoperative complexity
Medical/nonoperative management (if not surgical candidate or defers surgery):
- Avoid unnecessary calcium restriction
- Replete vitamin D as appropriate
- Antiresorptives for bone protection in selected patients
- Calcimimetic therapy (cinacalcet) for calcium lowering in selected cases
9) Complications and postoperative issues
- Untreated disease: fracture risk, kidney stones, renal calcification, chronic hypercalcemia effects
- Post-op:
- Hypocalcemia (including hungry bone syndrome in severe bone disease)
- Persistent/recurrent hyperparathyroidism if multigland disease missed or ectopic tissue remains
- Intraoperative PTH monitoring is often used to confirm adequate excision (rapid PTH half-life supports this strategy)
10) Differential diagnosis
- Primary multigland hyperplasia
- Parathyroid carcinoma
- Familial hypocalciuric hypercalcemia
- Secondary/tertiary hyperparathyroidism (especially CKD context)
- Non-PTH hypercalcemia (malignancy, vitamin D excess, others)
Recent evidence check (last 2 years)
Recent meta-analyses/systematic reviews were identified:
- PMID: 38739762 (skeletal effects of parathyroidectomy in PHPT)
- PMID: 41721481 (anesthesia approach in minimally invasive parathyroidectomy)
- PMID: 37929814 (4D-CT in discordant adenoma scans)
No major contradiction to standard textbook framework, but they reinforce current trends:
- surgery improves bone outcomes
- 4D-CT has an important role when first-line localization is discordant
Textbook sources
- Robbins, Cotran & Kumar Pathologic Basis of Disease, endocrine/parathyroid sections, histology and clinical features (pp. around 1010-1013 in extracted block context)
- Robbins & Kumar Basic Pathology, hyperparathyroidism morphology/clinical sections (pp. around 741-743 in extracted block context)
- Sabiston Textbook of Surgery, parathyroid surgery/localization/management chapter (pp. around 1541-1545 in extracted block context)
If you want, I can next give:
- a concise exam-oriented table (adenoma vs hyperplasia vs carcinoma), or
- a practical clinical algorithm for evaluating hypercalcemia and confirming parathyroid adenoma.
Yes and in a creative manner
Great. Here is a creative, high-yield way to remember parathyroid adenoma.
1) Story mnemonic: “The One Rebel Gland”
In the Kingdom of Calcium, four parathyroid guards keep balance.
One day, one guard turns rogue (solitary adenoma, most common) and keeps shouting:
“More PTH! More PTH!”
Even when calcium is already high, the rebel does not listen.
What happens in the kingdom?
- Bones: walls are mined for calcium → osteopenia/osteoporosis, bone pain, brown tumors in severe disease
- Kidneys: calcium stones clog river channels → nephrolithiasis/nephrocalcinosis
- Belly: villagers complain of constipation, nausea, abdominal discomfort
- Brain/Mood: fatigue, low mood, cognitive fog
The three loyal glands shrink quietly from suppression, while the rebel keeps growing.
Villain signature (lab pattern)
- Calcium: high
- PTH: high or “inappropriately normal”
- Phosphate: often low
- Urinary calcium: usually not low (helps separate from FHH)
2) Creative comparison table: “The 3 suspects in hyperparathyroidism court”
| Feature | Adenoma (The Lone Rebel) | Hyperplasia (The Four Cousins) | Carcinoma (The Invader) |
|---|---|---|---|
| Gland involvement | Usually single gland | Usually multigland | Usually single, invasive |
| Frequency in PHPT | Most common (85 to 95%) | 5 to 10% | Around 1% |
| Gross pattern | Well-circumscribed nodule | Diffuse/nodular enlargement of multiple glands | Hard/infiltrative mass |
| Histology clue | Chief-cell proliferation, low stromal fat | Hypercellularity in multiple glands, low fat | Diagnosis by invasion/metastasis, not cytology alone |
| Typical context | Sporadic most often | Sporadic or MEN syndromes | Rare, severe hypercalcemia more likely |
| Treatment | Focused excision if localized | Often broader exploration | En bloc oncologic approach |
3) Creative diagnostic algorithm: “Calcium Detective Map”
Step A: Confirm the crime
- High calcium found
- Check intact PTH
- If PTH high or not suppressed → PTH-dependent hypercalcemia (suspect PHPT)
Step B: Identify impostors
- Check 24-hour urinary calcium (or calcium/creatinine clearance ratio)
- Low urinary calcium suggests FHH rather than adenoma
Step C: Check damage report
- Bone: DXA ± fracture risk
- Kidney: creatinine/eGFR, stone screen (US/CT as needed)
Step D: Locate the rebel (only after biochemical diagnosis)
- Ultrasound ± sestamibi/SPECT
- If discordant or negative, consider 4D-CT
- Difficult/reoperative cases: MRI/PET options
Step E: Restore order
- Parathyroidectomy when indicated/suitable
- If not surgical candidate: medical monitoring, bone protection, calcium/vitamin D optimization, selective cinacalcet use
4) Ultra-short viva style memory hooks
- “Single gland, single culprit” = adenoma
- “PTH not suppressed despite high calcium” = primary hyperparathyroidism pattern
- “Diagnosis is biochemical, imaging is localization”
- “Adenoma first, hyperplasia second, carcinoma rare”
If you want, I can turn this into:
- a one-page colorful revision sheet, or
- 15 rapid-fire MCQs with explanations.
Yes
One-page revision sheet: Parathyroid Adenoma
Snapshot
- Definition: Benign neoplasm of parathyroid tissue causing autonomous PTH secretion
- Most common cause of PHPT: 85 to 95%
- Typical pattern: Single-gland disease
Core physiology in one line
Parathyroid adenoma resets calcium sensing so PTH stays inappropriately high despite hypercalcemia.
Biochemical signature
- Serum calcium: high
- PTH: high or inappropriately normal
- Serum phosphate: often low
- Urinary calcium: usually normal/high (not low like many FHH cases)
Classic clinical picture
“Bones, stones, abdominal groans, psychic moans”
- Bones: osteopenia/osteoporosis, bone pain, severe cases with osteitis fibrosa cystica/brown tumors
- Stones: nephrolithiasis, nephrocalcinosis
- GI: constipation, nausea, abdominal discomfort
- Neuropsych: fatigue, mood/cognitive symptoms
Pathology pearls
- Usually solitary, well-circumscribed, soft tan nodule
- Chief-cell predominant, reduced stromal fat
- Endocrine atypia can occur and is not equal to carcinoma
- Other glands are often suppressed/shrunken
Adenoma vs hyperplasia vs carcinoma
- Adenoma: single gland, most common
- Hyperplasia: usually multigland
- Carcinoma: rare, diagnosis hinges on invasion/metastasis
Diagnostic algorithm (exam-safe)
- Confirm hypercalcemia
- Measure intact PTH
- If PTH-dependent pattern, exclude FHH (24-hour urinary calcium or Ca/Cr clearance ratio)
- Assess end-organ effects: bone density, renal status/stones
- Localize only after biochemical diagnosis: US + sestamibi/SPECT, then 4D-CT if needed
Management
- Definitive: parathyroidectomy
- Focused minimally invasive surgery when localization is concordant
- If non-surgical: monitoring, bone-directed therapy as needed, vitamin D optimization, selected cinacalcet use
High-yield pitfalls
- Imaging does not diagnose PHPT; labs do
- “Normal PTH” is abnormal if calcium is high
- Do not miss FHH before surgery decisions
15 rapid-fire MCQs (with answers)
1) Most common cause of primary hyperparathyroidism?
A. Parathyroid carcinoma
B. Parathyroid adenoma
C. Secondary hyperplasia
D. Vitamin D deficiency
Answer: B
B. Parathyroid adenoma
C. Secondary hyperplasia
D. Vitamin D deficiency
Answer: B
2) Typical gland involvement in parathyroid adenoma?
A. All four glands enlarged
B. Two glands always involved
C. Single gland in most cases
D. No gland enlargement
Answer: C
B. Two glands always involved
C. Single gland in most cases
D. No gland enlargement
Answer: C
3) Typical biochemical pattern in adenoma-related PHPT:
A. Low Ca, high PTH
B. High Ca, suppressed PTH
C. High Ca, high or inappropriately normal PTH
D. Low Ca, low PTH
Answer: C
B. High Ca, suppressed PTH
C. High Ca, high or inappropriately normal PTH
D. Low Ca, low PTH
Answer: C
4) Which is usually lower in PHPT?
A. Sodium
B. Phosphate
C. Potassium
D. Chloride
Answer: B
B. Phosphate
C. Potassium
D. Chloride
Answer: B
5) Before localizing scans, the most important first step is:
A. MRI neck
B. 4D-CT
C. Biochemical confirmation of PHPT
D. PET-CT
Answer: C
B. 4D-CT
C. Biochemical confirmation of PHPT
D. PET-CT
Answer: C
6) Which test helps distinguish PHPT from FHH?
A. ESR
B. 24-hour urinary calcium
C. Serum amylase
D. Troponin
Answer: B
B. 24-hour urinary calcium
C. Serum amylase
D. Troponin
Answer: B
7) Histology most commonly seen in adenoma:
A. Chief-cell proliferation with reduced stromal fat
B. Squamous nests
C. Medullary thyroid pattern
D. Granulomatous inflammation
Answer: A
B. Squamous nests
C. Medullary thyroid pattern
D. Granulomatous inflammation
Answer: A
8) A key criterion for parathyroid carcinoma diagnosis:
A. Pleomorphic nuclei alone
B. Large size alone
C. Invasion/metastasis
D. High calcium alone
Answer: C
B. Large size alone
C. Invasion/metastasis
D. High calcium alone
Answer: C
9) Classic symptom cluster includes all except:
A. Renal stones
B. Bone pain
C. Severe jaundice
D. Neuropsychiatric complaints
Answer: C
B. Bone pain
C. Severe jaundice
D. Neuropsychiatric complaints
Answer: C
10) Definitive treatment for fit patient with symptomatic adenoma:
A. Long-term antibiotics
B. Thyroxine
C. Parathyroidectomy
D. Steroids
Answer: C
B. Thyroxine
C. Parathyroidectomy
D. Steroids
Answer: C
11) Which statement is correct?
A. Imaging replaces lab diagnosis
B. Imaging is for localization after lab diagnosis
C. PTH must be very high in all cases
D. PHPT always causes symptoms
Answer: B
B. Imaging is for localization after lab diagnosis
C. PTH must be very high in all cases
D. PHPT always causes symptoms
Answer: B
12) Common genetic alteration in sporadic adenomas:
A. BCR-ABL
B. CCND1 dysregulation
C. CFTR mutation
D. APC germline only
Answer: B
B. CCND1 dysregulation
C. CFTR mutation
D. APC germline only
Answer: B
13) In many modern cases, PHPT is first found by:
A. Bone biopsy
B. Incidentally elevated calcium on routine labs
C. Emergency seizure only
D. Thyroid storm
Answer: B
B. Incidentally elevated calcium on routine labs
C. Emergency seizure only
D. Thyroid storm
Answer: B
14) Hyperplasia differs from adenoma because hyperplasia is usually:
A. Unifocal single-gland disease
B. Multigland process
C. Always malignant
D. Never associated with MEN syndromes
Answer: B
B. Multigland process
C. Always malignant
D. Never associated with MEN syndromes
Answer: B
15) True regarding PTH in hypercalcemia due to adenoma:
A. It should be fully suppressed
B. It may be inappropriately normal
C. It is always zero
D. It is irrelevant diagnostically
Answer: B
B. It may be inappropriately normal
C. It is always zero
D. It is irrelevant diagnostically
Answer: B
If you want, I can next give you a mnemonic-only cram card (30 seconds review) and a case-based viva script (examiner asks, you answer).
Hyper parathyroidism in detail
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.