Varicose veins in detail with reference to standard textbooks
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Searching Images
varicose veins lower limb clinical photograph
Reading File
Reading File
Searching PubMed
varicose veins treatment management
Loading Image
Loading Image
Here is a comprehensive, textbook-referenced review of varicose veins:
Varicose Veins — A Detailed Review
1. Definition
Varicose veins are dilated, bulging, tortuous superficial veins measuring at least 3 mm in diameter. Smaller vessels are classified separately:
- Reticular veins: dilated intradermal veins, blue-green, 1–3 mm, do not protrude from the skin surface
- Telangiectasias (spider veins): <1 mm, forming blue, purple, or red linear, branching, or spider-web patterns near the skin surface
— Harrison's Principles of Internal Medicine, 22nd ed.
2. Epidemiology
Varicose veins are present in at least 10% of the general population (Schwartz's Principles of Surgery). Robbins Pathology (Cotran & Kumar) places the figure higher: up to 20% of males and one-third of females develop lower extremity varicose veins. By age 65, prevalence in Western populations exceeds 55% (Edinburgh Vein Study, cited in Current Surgical Therapy 14e).
Risk factors include:
- Female sex (elevated venous pressure from gravid uterus during pregnancy)
- Obesity
- Prolonged standing/sitting (occupational exposure)
- Family history — approximately half of patients with primary varicose veins have a positive family history, reflecting defective venous wall development
- Aging, hormonal therapy, inactivity
3. Relevant Anatomy
The superficial venous system of the lower limb includes:
- Great saphenous vein (GSV): the longest vein in the body; originates on the medial foot, ascends anterior to the medial malleolus, along the medial calf and thigh, draining into the common femoral vein at the saphenofemoral junction (SFJ)
- Small saphenous vein (SSV): originates on the dorsolateral foot, ascends posterior to the lateral malleolus, posterolateral calf, draining into the popliteal vein at the saphenopopliteal junction (SPJ)
- Perforating veins: connect the superficial and deep systems; normally direct blood from superficial → deep; their incompetence reverses this flow
Deep veins (femoral, popliteal, tibial) carry the majority of venous return. Bicuspid valves throughout the venous system direct flow centrally.
— Harrison's Principles of Internal Medicine, 22nd ed.
4. Pathophysiology
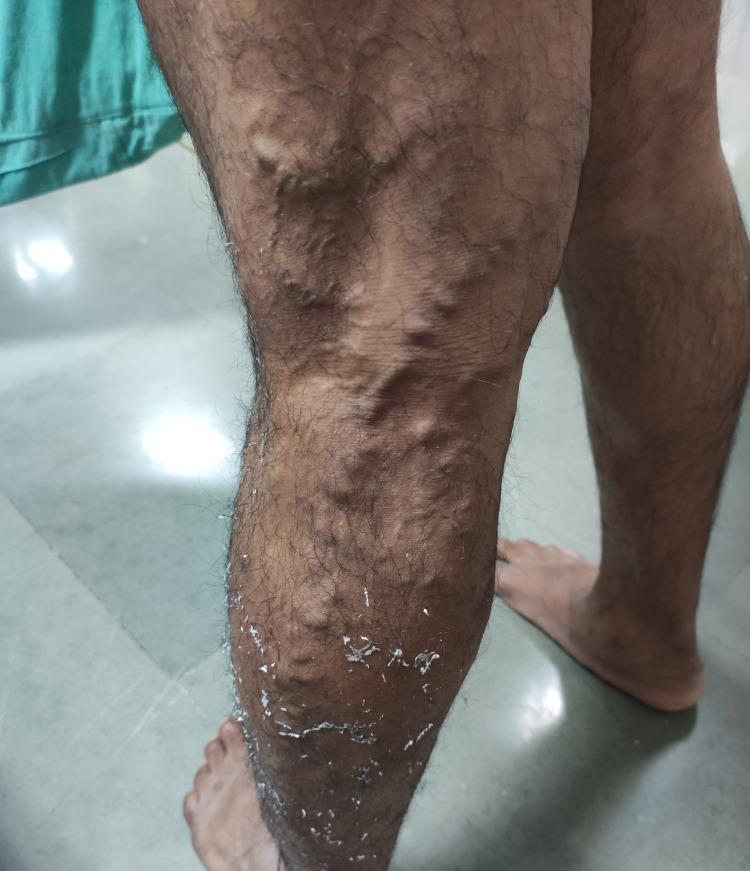
Clinical photograph: CEAP C2 varicose veins with secondary stasis dermatitis of the lower calf
Venous Pump Mechanism
When calf muscles contract, they compress the soleal sinuses and deep veins (pressure up to 300 cm H₂O), propelling blood centrally. During the resting phase, blood fills the superficial system from the skin and subcutaneous tissues, flowing through the perforators into the deep veins. The superficial venous system thus functions as an "atrium" and the deep calf veins as a "ventricle." In an upright individual at rest, foot venous pressure equals the hydrostatic column from foot to right heart (~70–80 cm H₂O).
— Pfenninger & Fowler's Procedures for Primary Care, 3rd ed.
Mechanism of Varicosity Formation
When venous walls dilate, the valve cusps fail to coapt, leading to valvular incompetence. Blood refluxes retrograde under gravity, increasing intraluminal pressure in more distal segments, propagating further dilatation and incompetence distally. This is produced by:
- Primary intrinsic weakness of the venous wall or valve structure
- Sustained elevated intraluminal pressure (prolonged standing, pregnancy, obesity)
Dysfunction of the superficial, deep, or perforating venous system can create widespread venous hypertension, leading to abnormal dilation, tortuosity, and dysfunction of superficial veins. — Fitzpatrick's Dermatology, 5th ed.
Varicose veins are abnormally dilated, tortuous veins produced by prolonged, increased intraluminal pressure resulting in vessel dilation and subsequent incompetence of the venous valves. Venous pressures in superficial sites can be markedly elevated — up to 10 times normal — by prolonged dependent posture. — Robbins, Cotran & Kumar: Pathologic Basis of Disease
5. Classification
Primary vs. Secondary
| Type | Mechanism |
|---|---|
| Primary | Intrinsic abnormalities of the venous wall or superficial valve structure; originate in the superficial system; ~50% have family history |
| Secondary | Venous hypertension from deep-venous insufficiency, deep-venous obstruction, or incompetent perforating veins; also from arteriovenous fistulas |
— Harrison's Principles of Internal Medicine, 22nd ed.; Schwartz's Principles of Surgery, 11th ed.
Vessel Size Classification (Pfenninger & Fowler, 3rd ed.)
| Type | Designation | Diameter | Color |
|---|---|---|---|
| I | Telangiectases ("spider veins") | 0.1–1 mm | Red |
| Ia | Telangiectatic matting | <0.2 mm | Red |
| II | Venulectasia | 1–2 mm | Violaceous |
| III | Reticular veins | 2–4 mm | Blue |
| IV | Nonsaphenous varicosities (2nd degree perforators) | 3–8 mm | Blue |
| V | Saphenous varicosities | 7–8 mm | Blue |
CEAP Classification (Revised 2020)
The CEAP (Clinical–Etiologic–Anatomic–Pathophysiologic) system is the international standard for grading chronic venous disease severity:
| Grade | Description |
|---|---|
| C0 | No visible or palpable venous disease |
| C1 | Telangiectasias or reticular veins |
| C2 | Varicose veins |
| C2r | Recurrent varicose veins |
| C3 | Edema |
| C4a | Pigmentation or eczema |
| C4b | Lipodermatosclerosis or atrophie blanche |
| C4c | Corona phlebectatica |
| C5 | Healed venous ulcer |
| C6 | Active venous ulcer |
| C6r | Recurrent active venous ulcer |
The etiologic modifier classifies as Primary (Ep), Secondary intravenous/extravenous (Esi/Ese), or Congenital (Ec). The ambulatory venous pressure (AVP) correlates with severity: skin manifestations are uncommon at AVP <35 mmHg but almost certain at AVP >90 mmHg. — Current Surgical Therapy, 14th ed.
6. Clinical Features and Presentation
Symptoms
Patients are often asymptomatic and present with cosmetic concerns. Symptoms, when present, include:
- Dull ache, throbbing, heaviness, or pressure sensation — worse after prolonged standing, relieved by leg elevation
- Cramping, burning, pruritus
- Ankle/leg swelling (pitting edema)
- Skin ulceration in advanced disease
— Harrison's Principles of Internal Medicine, 22nd ed.
Signs and Examination
Examination is performed in both supine and standing positions:
- Visual inspection and palpation in standing position confirm dilated, tortuous superficial veins
- Saphena varix: a bulge at the SFJ (saphenofemoral junction) in the groin, which may transmit a cough impulse
- Stasis dermatitis ("brawny induration"): brawny pigmentation from hemolysis of extravasated red cells
- Lipodermatosclerosis: induration + hemosiderin deposition + inflammation — typically just above the medial malleolus
- Atrophie blanche: white scar tissue with hyperpigmented border, near medial malleolus
- Phlebectasia corona: fan-shaped intradermal veins near ankle/foot
- Venous ulcer: shallow, irregular border, granulation tissue base, near medial or lateral malleoli
Notably, embolism from superficial varicosities is very rare, in contrast to deep vein thrombosis. — Robbins, Cotran & Kumar: Pathologic Basis of Disease
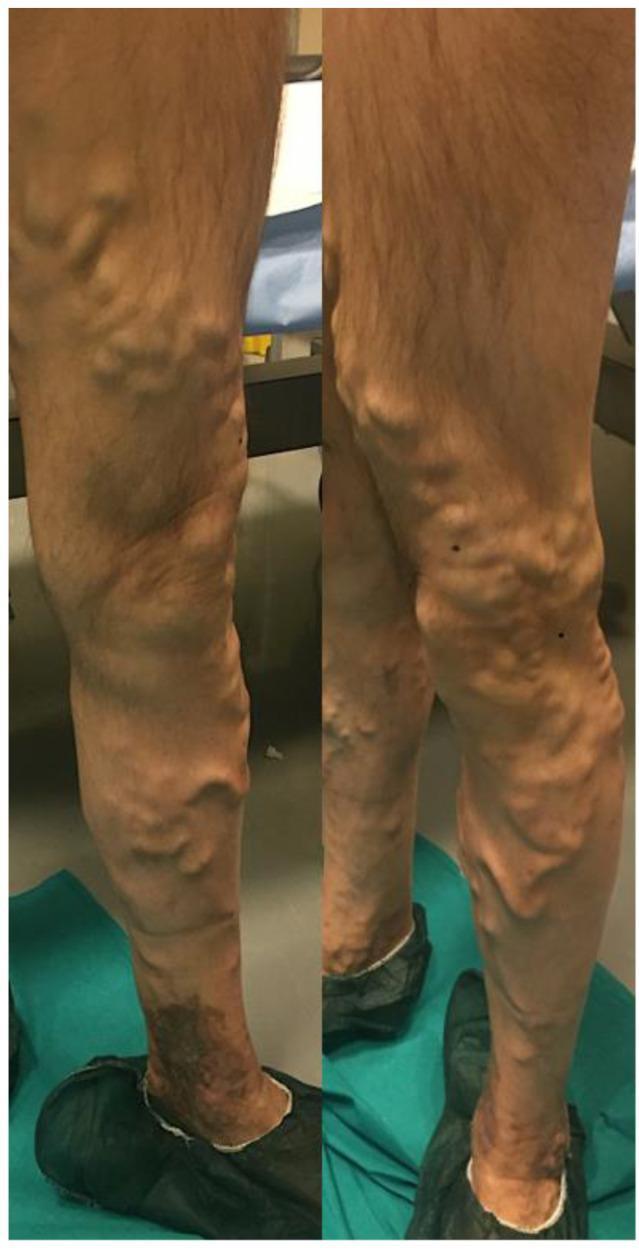
Anterior and posterior views of advanced varicose veins involving the GSV distribution with hyperpigmentation and lipodermatosclerosis at the ankle
7. Sites of Valvular Incompetence
The key anatomical sites where valvular incompetence typically produces marked varicosities are:
- Saphenofemoral junction (saphena varix) — GSV meets the femoral vein
- Mid-thigh perforating vein — GSV to femoral vein
- Three calf perforators — 5, 10, and 15 cm above the medial malleolus (GSV to deep calf veins)
- Saphenopopliteal junction — SSV meets the popliteal vein
— Gray's Anatomy for Students
8. Bedside Clinical Tests
Brodie–Trendelenburg Test
The leg is elevated supine to empty the veins; a tourniquet is placed on the proximal thigh; the patient stands. Prompt filling within 30 seconds indicates deep-venous insufficiency and incompetent perforators. If filling only occurs after tourniquet removal, primary superficial venous insufficiency is the diagnosis.
Perthes Test
A tourniquet is placed on the mid-thigh after standing (veins filled); patient walks for 5 minutes. If the deep system is patent with competent perforators, superficial veins below collapse. Further distension with walking indicates deep-venous obstruction.
— Harrison's Principles of Internal Medicine, 22nd ed.; Gray's Anatomy for Students
9. Investigations
Duplex Ultrasound
The principal diagnostic test. Combines B-mode imaging and spectral Doppler to detect:
- Venous obstruction (absent flow, echogenic thrombus, non-compressible vein)
- Venous reflux (prolonged reversal of flow during Valsalva or calf compression/release)
Venous reflux is detected when retrograde flow lasts >0.5 seconds in superficial veins and >1 second in deep veins during the release phase of a calf compression maneuver. — Harrison's Principles of Internal Medicine, 22nd ed.
10. Complications
| Complication | Notes |
|---|---|
| Superficial thrombophlebitis | Inflammation + thrombus in superficial veins; painful, indurated cord; rarely embolises |
| Stasis dermatitis | Eczematous, hyperpigmented skin from venous congestion and hemosiderin deposition |
| Lipodermatosclerosis | Fibrotic induration of subcutaneous fat, typically above the medial malleolus |
| Venous ulceration | Near medial/lateral malleolus; shallow, irregular border; notoriously slow healing |
| Bleeding | Spontaneous rupture of attenuated superficial varices; controlled by elevation and compression |
| Deep vein thrombosis | Rare from superficial disease alone; more often from deep venous pathology |
— Schwartz's Principles of Surgery, 11th ed.; Robbins, Cotran & Kumar: Pathologic Basis of Disease
11. Treatment
Conservative Management
Elastic compression stockings are the cornerstone of conservative therapy:
- Grades: 20–30, 30–40, or 40–50 mmHg
- Range from knee-high to waist-high
- Provide symptom relief in many patients
- Indicated as first-line before considering interventions
— Schwartz's Principles of Surgery, 11th ed.
Indications for Intervention
- Symptoms worsening despite compression therapy
- Lipodermatosclerosis or venous ulceration
- Cosmetic indication (patient preference)
- Superficial thrombophlebitis or bleeding varices
Sclerotherapy
Acts by destroying the venous endothelium, causing inflammatory apposition of vein walls and eventual fibrosis. A randomised trial demonstrated significant symptom relief and improved cosmetic appearance with foam sclerotherapy vs. placebo.
Common sclerosing agents and concentrations:
| Agent | For Telangiectasias | For Larger Varices |
|---|---|---|
| Hypertonic saline | 11.7–18.7% | 23.4% |
| Sodium tetradecyl sulfate (STS) | 0.125–0.25% | 0.5–1.0% |
| Polidocanol | 0.5% | 0.75–1.0% |
After injection, elastic bandages are worn continuously for 3–5 days (apposition of inflamed walls), followed by elastic stockings for a minimum of 2 weeks. Complications include allergic reaction, hyperpigmentation, thrombophlebitis, DVT, and skin necrosis.
— Schwartz's Principles of Surgery, 11th ed.; Pfenninger & Fowler's Procedures for Primary Care, 3rd ed.
Endovenous Thermal Ablation
Endovenous laser treatment (EVLT) and radiofrequency ablation (RFA) are the preferred modalities for symptomatic GSV or SSV reflux. Under ultrasound guidance:
- A 21-gauge needle punctures the distal thigh/proximal calf GSV
- A sheath is placed over a guidewire
- Laser fiber or RFA catheter is advanced to just below the SFJ
- Tumescent anaesthesia is injected around the GSV
- The vein is treated as the catheter is withdrawn
Results are comparable to open surgery, but with more rapid postprocedure recovery. Risks include DVT, ecchymosis, and saphenous nerve injury.
— Schwartz's Principles of Surgery, 11th ed.
Surgical Treatment
Saphenous vein ligation and stripping remains preferred for GSV diameter >2 cm:
- Small medial groin incision (SFJ) and incision just below the knee
- GSV removed with a blunt-tip catheter or invagination pin stripper
- Complications: ecchymosis, haematoma, lymphocele, DVT, infection, saphenous nerve injury
- Lower recurrence rate than SFJ ligation alone
Stab avulsion phlebectomy: for large branch varicosities — 2 mm incisions directly over the vein; varicosity is avulsed without formal ligation. Haemostasis achieved with leg elevation and compression.
— Schwartz's Principles of Surgery, 11th ed.
Nonthermal Techniques
- Mechanochemical ablation (MOCA): catheter-based mechanical endoluminal injury combined with sclerotherapy; no tumescent anaesthesia required
- Cyanoacrylate adhesive (VenaSeal): proprietary adhesive seals the vein lumen; no thermal energy or tumescent; promising early results
12. Special Sites of Varicosities
Beyond the lower extremity, clinically important varicosities include:
Esophageal varices — Portal hypertension (most commonly from liver cirrhosis) opens portosystemic shunts into the gastroesophageal junction veins. Rupture causes massive, potentially fatal upper GI haemorrhage.
Hemorrhoids — Varicose dilation of the anorectal venous plexus from chronic pelvic venous congestion (pregnancy, chronic straining). Source of bleeding and prone to thrombosis and painful ulceration.
— Robbins, Cotran & Kumar: Pathologic Basis of Disease
13. Differential Diagnosis of Leg Swelling
Varicose veins with oedema must be distinguished from:
- Acute DVT: acute onset vs. chronic course
- Lymphoedema: non-pitting, progressive; may coexist (phlebo-lymphoedema)
- CCF, nephrotic syndrome, hypothyroidism: bilateral pitting oedema with systemic features
- Calcium channel blockers / thiazolidinediones: drug-induced oedema
- Cellulitis: erythema, warmth, fever
- Venous ulcers vs. arterial/neuropathic ulcers: location, wound bed characteristics
— Harrison's Principles of Internal Medicine, 22nd ed.
Recent Evidence
Recent systematic reviews (2024–2025) confirm the established evidence base:
- Anatomical reflux patterns in primary chronic venous disease are reviewed in a 2024 systematic review and meta-analysis [PMID: 39025298]
- Physiotherapy (calf muscle exercises, compression, elevation) has a role in managing venous ulcers as adjunct therapy [PMID: 40504402]
- Platelet-rich plasma shows emerging utility for chronic venous ulcer healing [PMID: 41643347]
Sources cited:
- Harrison's Principles of Internal Medicine, 22nd ed. (2025)
- Schwartz's Principles of Surgery, 11th ed.
- Robbins, Cotran & Kumar: Pathologic Basis of Disease
- Robbins & Kumar Basic Pathology
- Gray's Anatomy for Students
- Current Surgical Therapy, 14th ed.
- Pfenninger & Fowler's Procedures for Primary Care, 3rd ed.
- Fitzpatrick's Dermatology, 5th ed.
Arterial vs venos ulcer
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching Images
arterial ulcer versus venous ulcer leg comparison
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
!
Image processing blocked due to content policy violation.
We encountered an error while processing your request. Please try again or reach out to us for help.
This is a shared conversation. Sign in to Orris to start your own chat.