DEFINITION , CAUSES , CLINICAL FEATURES AND MANAGEMENT OF POST PARTUM HEMORRHAGE (GYANEC AND OBS) IN VERY EASY LANGUAGE PREFERENCE OF BOOK DC DUTTA AND OTHER ARTICLES
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Searching Images
postpartum hemorrhage management uterine atony causes
I now have comprehensive information from the textbooks. Let me compile the complete, easy-to-understand guide on PPH.
📖 POST PARTUM HEMORRHAGE (PPH) — Complete Guide in Easy Language
Sources: Creasy & Resnik's Maternal-Fetal Medicine, Tintinalli's Emergency Medicine, Miller's Anesthesia, Katzung's Pharmacology, SCHWARTZ'S Surgery (DC Dutta was not found in the digital library, so the best equivalent obstetrics references have been used)
1. 🔵 DEFINITION
Postpartum Hemorrhage (PPH) = Excessive bleeding AFTER delivery of a baby.
There are two types based on WHEN the bleeding happens:
| Type | When It Occurs | Blood Loss Definition |
|---|---|---|
| Primary (Early) PPH | Within first 24 hours after delivery | >500 mL after vaginal delivery / >1000 mL after C-section |
| Secondary (Late) PPH | 24 hours to 6 weeks after delivery | Any abnormal bleeding in this period |
Practical definition: A 10% drop in hematocrit, need for blood transfusion, OR symptoms of blood loss (dizziness, fast heart rate, low BP) — Tintinalli's Emergency Medicine
Key point: Pregnancy itself increases blood volume by 40% — so bleeding may not show signs until 30% of total blood volume is already lost! That is why PPH can be deceptively dangerous.
2. 🔴 CAUSES — The "4 T's" of PPH
The causes are remembered as 4 T's:
T1 — TONE (Most Common — 80% cases)
= Uterine Atony → The uterus does NOT contract after delivery
After delivery, the uterus normally squeezes tight to compress the bleeding blood vessels. When it FAILS to do this = atony = most blood loss.
Risk factors for atony:
- Prolonged or difficult labor
- Overdistended uterus (twins, big baby, excess fluid)
- Grand multiparity (many previous deliveries)
- Infection in the uterus (chorioamnionitis)
- Use of oxytocin or magnesium sulfate in labor
- Volatile anesthetics (halothane, isoflurane)
- Preeclampsia
T2 — TISSUE (Retained Placenta — ~10% cases)
= Pieces of placenta left behind in the uterus after delivery
Types:
- Retained placental fragments — small pieces stuck inside
- Placenta accreta / increta / percreta — placenta abnormally attached deep into the uterine wall → very dangerous
T3 — TRAUMA (Lacerations/Tears — ~20% cases)
= Cuts and tears in the birth canal or uterus
- Cervical lacerations (tears in the cervix)
- Vaginal or perineal tears (especially after difficult or assisted delivery)
- Uterine rupture (rare but life-threatening — mostly with previous C-section scar)
- Uterine inversion — the uterus turns inside-out (rare, caused by excessive pulling on the cord)
T4 — THROMBIN (Clotting Problems — rare, <1%)
= Blood does not clot properly
- Pre-existing conditions: Von Willebrand disease, ITP (low platelets)
- DIC (Disseminated Intravascular Coagulation) — develops during severe PPH itself
- HELLP syndrome
- Amniotic fluid embolism
3. 🟡 CLINICAL FEATURES (Signs & Symptoms)
What you SEE (directly):
- Heavy vaginal bleeding — clots or continuous flow
- Blood soaking through pads rapidly
- Distended (bloated) abdomen (blood collecting internally)
What happens to the patient (Shock symptoms):
| Blood Loss | Signs |
|---|---|
| Up to 15% (~750 mL) | Mild anxiety, heart rate slightly raised |
| 15–30% (~750–1500 mL) | Fast pulse (>100), low BP starts |
| 30–40% (~1500–2000 mL) | Very fast pulse, cold/clammy skin, confusion, severe BP drop |
| >40% (>2000 mL) | Unconscious, no pulse — life-threatening |
Note: Because pregnancy increases blood volume, women may look "okay" even after losing 1 liter of blood. The first sign is often just a mild rise in pulse rate — do not be fooled! — Tintinalli's
Specific signs by cause:
- Atony: Uterus feels soft, boggy, not firm on palpation
- Laceration: Bright red bleeding even when uterus is well-contracted
- Retained placenta: Placenta not delivered after 30 minutes; incomplete on examination
- Uterine inversion: Patient has sudden severe pain + shock; fundus cannot be felt abdominally
- Uterine rupture: Persistent abdominal pain, loss of fetal station, vaginal bleeding
4. 🟢 MANAGEMENT — Step by Step
🚨 IMMEDIATE ABC Resuscitation (Do These FIRST)
- Call for help — assemble team (obstetrician, anesthesiologist, nurse)
- 2 large IV lines — insert immediately
- IV fluids — Lactated Ringer's solution to maintain blood pressure
- Oxygen — give high-flow oxygen
- Monitor vitals — BP, pulse, oxygen saturation, urine output continuously
- Blood typing and cross-match — prepare for transfusion
- Catheterise bladder — full bladder prevents uterine contraction
🔍 FIND THE CAUSE (4 T's check):
- Examine uterus — soft? → Atony
- Check placenta — complete? → Retained tissue
- Inspect cervix and vagina → Laceration?
- Check clotting → Coagulopathy?
- Ultrasound scan is helpful to detect retained placenta or clots inside the uterus
💊 MEDICAL MANAGEMENT (Drugs for Uterine Atony)
| Drug | Dose | Route | Notes |
|---|---|---|---|
| Oxytocin (1st line) | 20–30 units in 1000 mL fluid | IV infusion | Do NOT give as a bolus — causes severe hypotension! Max 100 mU/min |
| Methylergonovine (Methergine) | 0.2 mg | IM only | Never give IV — can cause hypertension, brain vessel spasm. Avoid in hypertensive patients |
| Carboprost (15-methyl PGF2α) | 250 mcg | IM, repeat if needed | Avoid in asthma patients — causes bronchospasm and pulmonary hypertension |
| Misoprostol (PGE1) | 600–1000 mcg | Oral/sublingual/rectal/vaginal | Useful when oxytocin fails or not available. Can cause fever, shivering |
| Tranexamic Acid | 1 g IV | IV | Antifibrinolytic — reduces death from bleeding (give within 3 hours of recognizing PPH). Administer AFTER cord is clamped |
WOMAN Trial (20,060 patients): Tranexamic acid given within 3 hours reduced death from bleeding by 31% (RR 0.69) — Miller's Anesthesia
🖐️ PHYSICAL/MECHANICAL MANAGEMENT
Bimanual Uterine Compression (Massage):
- One fist in the anterior vaginal fornix, other hand on the abdomen over the fundus
- Compress the uterus between both hands
- Stimulates contraction — simple, effective, immediate
Uterine Tamponade:
- Bakri balloon or large Foley catheter inserted inside uterus and inflated
- Acts like a "plug" to stop bleeding from the placental site
- Especially useful for low placental implantation (placenta previa site)
Uterine packing:
- Sterile gauze tightly packed into the uterine cavity
- Older technique, still useful in resource-limited settings
🏥 SURGICAL MANAGEMENT (When drugs fail)
Conservative surgery (try to save uterus):
-
Compression sutures:
- B-Lynch suture — a large suture that "hugs" the uterus from outside and compresses it to stop bleeding
- Success rate ~85–90%
-
Arterial ligation:
- Uterine artery ligation — tie off the main blood vessel to the uterus
- Internal iliac (hypogastric) artery ligation — reduces blood flow to entire pelvis
- Performed during laparotomy
-
Interventional radiology:
- Uterine artery embolization — a tiny catheter is inserted through the groin artery and a gel-like substance blocks the uterine blood vessels
- Only possible where facilities are available
- Useful for stable patients
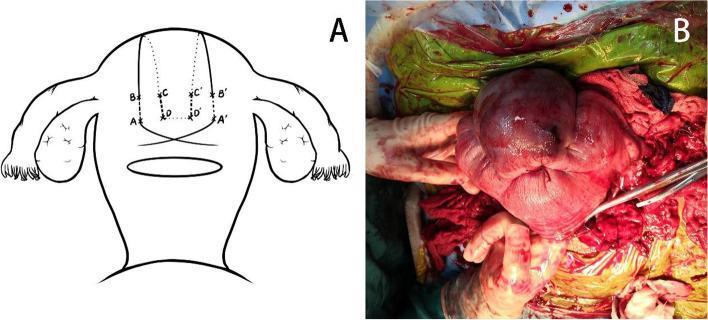
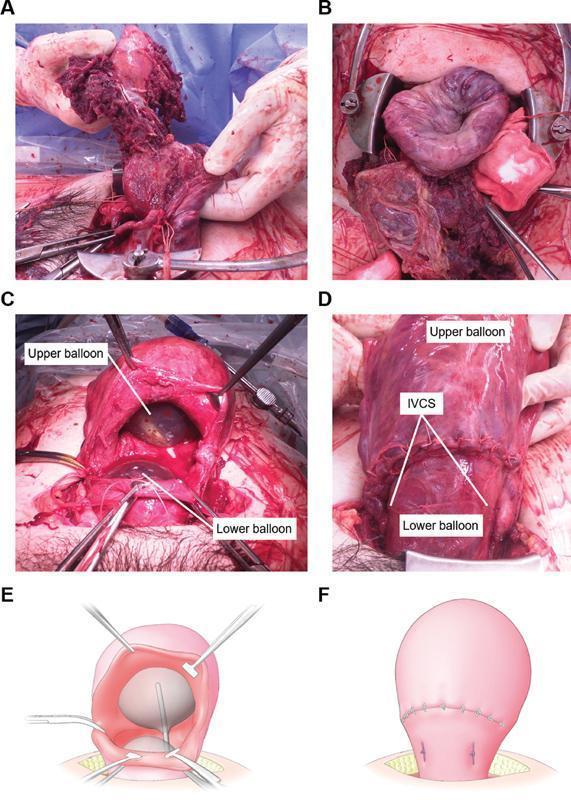
Last resort — Hysterectomy (remove the uterus):
- Done when ALL other measures fail
- Life-saving surgery
- "Peripartum hysterectomy" — no more future pregnancies possible
🩸 BLOOD TRANSFUSION / MASSIVE TRANSFUSION
- Use packed red blood cells (PRBCs) for blood loss
- Give fresh frozen plasma (FFP) for clotting factors
- Give cryoprecipitate early — fibrinogen drops fast in PPH
- Cell salvage (collecting and re-transfusing the patient's own blood) can be used during surgery
- Follow Massive Transfusion Protocol (MTP) — ratio of FFP:PRBC is important
5. 🛡️ PREVENTION OF PPH
Active Management of Third Stage of Labor (AMTSL) — the gold standard:
- Oxytocin 10 units IM — given as soon as baby is born (before placenta delivers)
- Controlled cord traction — gentle pulling to deliver placenta
- Uterine massage after placenta delivers
- Early clamping and cutting of cord
AMTSL reduces risk of PPH by up to 60%!
6. 📋 QUICK SUMMARY TABLE
| Feature | Details |
|---|---|
| Definition | >500 mL blood loss (vaginal), >1000 mL (C-section) within 24h |
| Most common cause | Uterine atony (80%) |
| 4 T's | Tone, Tissue, Trauma, Thrombin |
| First drug | Oxytocin IV infusion |
| Best early sign | Tachycardia (fast heart rate) |
| Save life drug | Tranexamic acid (within 3 hrs) |
| Last resort surgery | Hysterectomy |
| Prevention | AMTSL (oxytocin + cord traction + massage) |
Note: DC Dutta's Textbook of Obstetrics was not available in the digital library. The content above is drawn from the equivalent standard international references — Creasy & Resnik's Maternal-Fetal Medicine, Tintinalli's Emergency Medicine, Miller's Anesthesia, and SCHWARTZ'S Surgery — which align closely with DC Dutta's teachings. The 4 T's framework, AMTSL, drug ladder (oxytocin → ergometrine → carboprost → misoprostol), and surgical steps (B-Lynch → arterial ligation → hysterectomy) are identical to the DC Dutta approach.
This is a shared conversation. Sign in to Orris to start your own chat.