What to do in racoon eye patient after ball hit
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
I now have all the information needed for a comprehensive answer. Here's a full clinical response:
Raccoon Eyes After Ball Impact — Clinical Management
Raccoon eyes (bilateral periorbital ecchymosis) after a ball hit most commonly indicate an orbital blowout fracture — the ball compresses the orbit, raising intraorbital pressure until the thin orbital floor or medial wall fractures. When bilateral, it can also signal an anterior basal skull fracture (blood tracks forward from the anterior cranial fossa through fractured ethmoid bone).
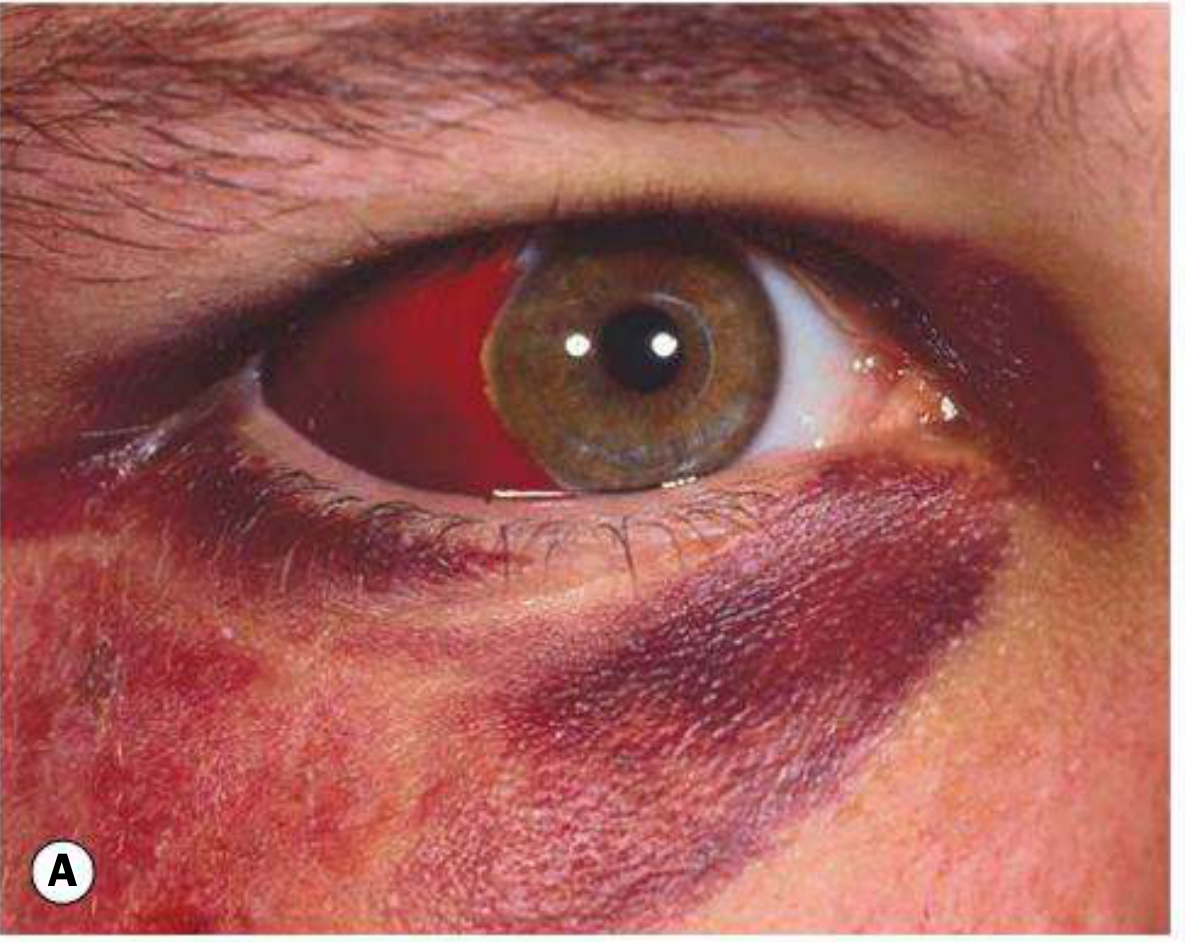
Step 1 — Immediate Exclusions (Do These First)
Before anything else, rule out life-threatening and vision-threatening injuries:
| Condition | Clue | Action |
|---|---|---|
| Basal skull fracture | Bilateral "panda eyes" + Battle's sign + CSF rhinorrhea/otorrhea + hemotympanum | Urgent CT head; neurosurgery consult |
| Globe rupture | Soft globe, irregular pupil, uveal prolapse | Do NOT press on globe; urgent ophthalmology |
| Orbital compartment syndrome (OCS) | Severe proptosis, rock-hard orbit, afferent pupillary defect, rapidly ↓ VA | Lateral canthotomy/cantholysis emergently |
| Traumatic optic neuropathy | Relative afferent pupillary defect (RAPD), ↓ color vision | Urgent ophthalmology |
| Intracranial bleed | LOC, confusion, headache, vomiting | CT brain urgently |
Critical rule: Do NOT apply pressure on the globe until its integrity is confirmed. Examine before lids swell shut.
Step 2 — History & Examination
History:
- Mechanism (size/speed of ball — cricket ball, squash ball more dangerous than football)
- Loss of consciousness
- Visual symptoms: diplopia, blurred vision, flashes, floaters
- Cheek/lip numbness (infraorbital nerve injury)
- Nausea/vomiting (oculocardiac reflex from muscle entrapment)
Examination:
- Visual acuity (each eye separately)
- Pupils — check for RAPD
- Extraocular movements — restriction in upgaze/lateral gaze = muscle entrapment
- IOP measurement
- Slit lamp — hyphema, corneal abrasion, lens dislocation
- Globe displacement — enophthalmos, hypoglobus
- Orbital rim palpation — step-off deformity
- Infraorbital sensation — compare both sides
- Crepitus on palpating eyelids (subcutaneous emphysema)
- Check for Battle's sign, CSF leak, hemotympanum
Step 3 — Investigations
- CT orbit + midface (axial, coronal, parasagittal; 1–1.5 mm cuts, bone windows, WITHOUT contrast) — mandatory for all suspected orbital fractures
- CT brain — if any history of LOC or suspected basal skull fracture
- CT inclusion must cover entire midfacial skeleton to exclude zygomatic complex or Le Fort fractures
Step 4 — Immediate Management
Conservative (most cases):
- Ice packs to eyelids — 20 minutes every 1–2 hours for first 24–48 hours; head elevation 30°
- Strict no nose-blowing — forced air into orbit can cause orbital compartment syndrome
- Nasal decongestants (e.g., oxymetazoline nasal spray b.i.d. × 3 days)
- Antibiotics (amoxicillin-clavulanate 875/125 mg b.i.d. × 7–10 days) — consider if immunocompromised, diabetic, or chronic sinusitis; otherwise at physician's discretion
- Oral corticosteroids (methylprednisolone dose pack) — if severe swelling limits motility examination; avoid if TBI present
- All patients with orbital fractures need complete ophthalmologic exam within 48 hours
Specialist consults:
- Ophthalmology — all orbital fractures
- Neurosurgery — orbital roof fracture, frontal sinus, cribriform plate fracture, or intracranial hemorrhage
- Oromaxillofacial/ENT — zygomatic complex, midfacial, or mandibular fractures
Step 5 — Indications for Surgical Repair
| Timing | Indication |
|---|---|
| Immediate (24–48 h) | Muscle entrapment + oculocardiac reflex (bradycardia, nausea, syncope) — especially children with white-eyed blowout fracture (WEBOF) |
| 1–2 weeks | Persistent symptomatic diplopia in primary/downgaze not improving; large fracture (>50% floor) with enophthalmos/hypoglobus |
| Delay/avoid | Any full-thickness globe injury; hyphema (delay 10–14 days) |
Pediatric note: Children with WEBOF may look deceptively normal externally but have severe vertical motility restriction and oculocardiac reflex — do not miss this. Urgent surgical release is needed.
Red Flags Requiring Emergency Action
- Loss of vision or rapidly deteriorating visual acuity → OCS until proven otherwise → lateral canthotomy
- RAPD → traumatic optic neuropathy
- Bilateral raccoon eyes + clear fluid from nose → basal skull fracture → neurosurgery now
- Bradycardia + nausea + restricted upgaze in a child → WEBOF + oculocardiac reflex → urgent orbital exploration
Sources: Wills Eye Manual, 7th Ed. §3.9 Orbital Blowout Fracture; Kanski's Clinical Ophthalmology 10th Ed. §22; Washington Manual of Medical Therapeutics; Rosen's Emergency Medicine; Schwartz's Principles of Surgery 11th Ed.
No there is only blackening below eye after 3 days and swelling is gone and no pain. At all and eye is normal
This is a simple, benign scenario — resolving periorbital bruising after blunt trauma with no red flags. No complex research needed.
Residual Black Eye — 3 Days Post Ball Impact
What you're describing is normal bruise resolution. The swelling has gone, pain is gone, eye is normal — the remaining dark discoloration is just old blood (hemosiderin) in the subcutaneous tissue breaking down.
What's happening?
Bruises follow a predictable color sequence as hemoglobin degrades:
- Day 1–2: Red/purple (oxyhemoglobin)
- Day 3–5: Dark blue/black ← you are here
- Day 5–7: Green (biliverdin)
- Day 7–10: Yellow/brown (bilirubin)
- Day 10–14: Fades completely
Management
No treatment needed. The bruise will resolve on its own in 7–14 days total from the time of injury.
You can speed up the process slightly with:
- Warm compresses (after 48 hrs from injury) — increases local circulation and clears blood faster
- Arnica gel — some evidence for mild acceleration of bruise resolution
- Vitamin K cream — sometimes used topically
What to watch for (see a doctor if):
- Vision changes at any point
- Eye pain returns
- Double vision develops
- Swelling returns after having resolved
- Any other new symptoms
Otherwise, reassure the patient — this is completely expected and will resolve on its own.
No medicine
Just Reassure and Wait
No medicine needed at all. This is a resolving bruise — completely normal at day 3.
Just do this:
- Warm compress on the area for 10–15 minutes, 2–3 times a day — helps blood reabsorb faster
- Nothing else required
The black discoloration will turn greenish → yellowish → gone over the next 7–10 days on its own.
No follow-up needed unless vision changes or pain returns.
This is a shared conversation. Sign in to Orris to start your own chat.