Diagnose and plan the management( Step by step) of Erythema Toxicum Neonatorum, Adenoma Sebaceum, Cutis Marmorata and Seborrheic Dermatitis.( Pediatrics)
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
I now have comprehensive information from authoritative textbooks to provide a thorough, well-structured answer on all four conditions.
Pediatric Skin Conditions: Diagnosis & Step-by-Step Management
1. Erythema Toxicum Neonatorum (ETN)
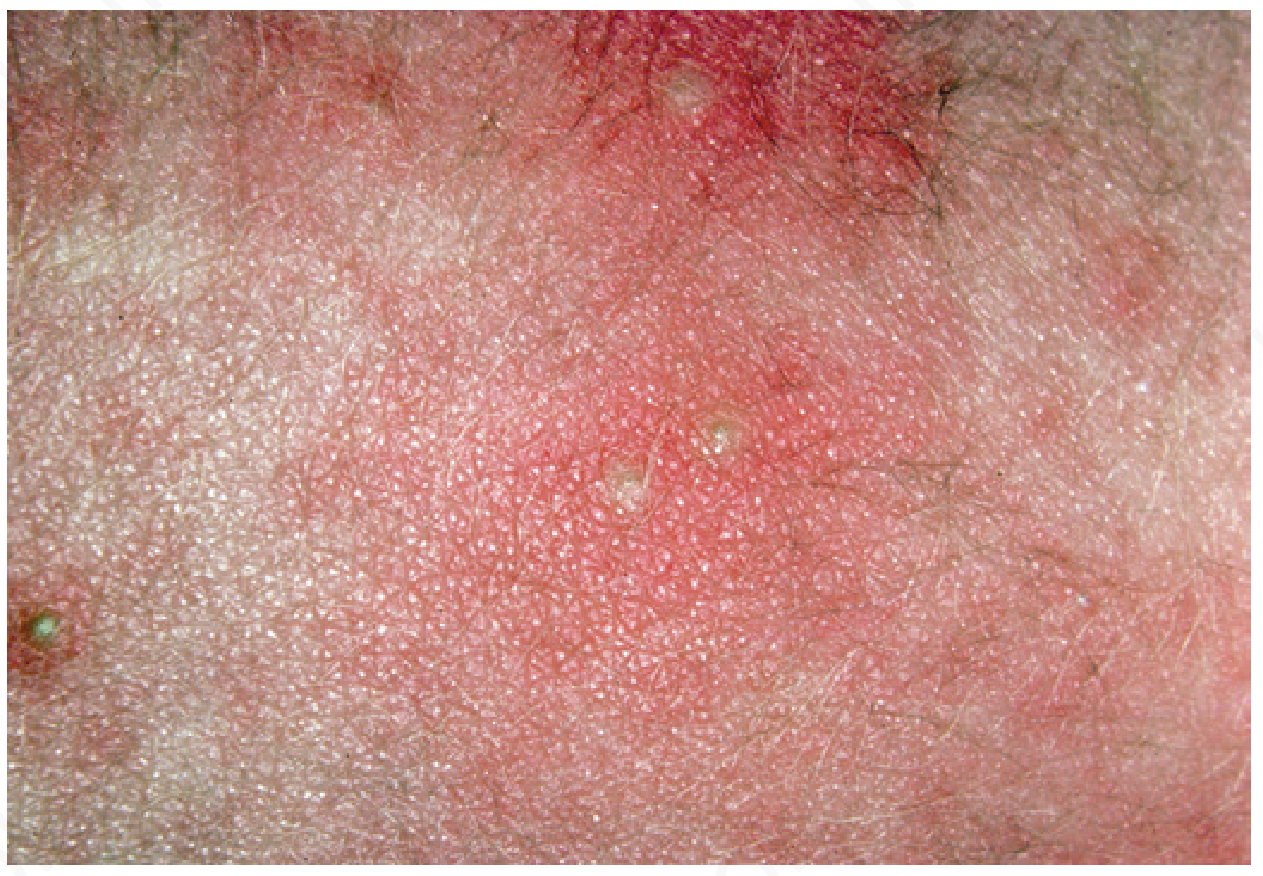
Diagnosis
| Feature | Details |
|---|---|
| Incidence | 25–50% of healthy full-term newborns; declines with prematurity and low birth weight |
| Onset | Typically day 2–3 of life; can appear at birth or up to 2–3 weeks |
| Morphology | Small erythematous macules and papules evolving into pustules on a broad erythematous base (the flare is disproportionately larger than the central lesion) |
| Distribution | Face, trunk, proximal extremities; spares palms and soles |
| Systemic signs | Fever is absent |
| Natural history | Self-limited; resolves within 5–10 days; recurrences possible |
Key diagnostic feature: The wide erythematous halo surrounding a tiny central follicular pustule is pathognomonic.
Differential diagnosis to exclude:
- Miliaria (heat rash)
- Bacterial folliculitis
- Neonatal herpes simplex
- Transient neonatal pustular melanosis (no erythematous base; collarette of scale)
- Scabies
Management (Step by Step)
Step 1 — Clinical diagnosis
Diagnose clinically based on the characteristic morphology and timing. No workup is needed in typical cases.
Step 2 — Laboratory confirmation (atypical cases only)
If the rash is atypical or diagnosis is uncertain: perform a smear of pustular contents stained with Wright or Giemsa — the finding of eosinophils confirms ETN. Rarely, biopsy shows folliculitis with eosinophils and neutrophils.
Step 3 — Reassurance and parental counseling
Inform parents this is a benign, self-resolving condition requiring no treatment. Resolution occurs by day 10.
Step 4 — No pharmacologic treatment required
No topical or systemic therapy is indicated. Avoid unnecessary antibiotic use.
Step 5 — Monitoring
Observe for any signs suggesting infection (fever, worsening, systemic symptoms) that would prompt further investigation.
2. Adenoma Sebaceum (Facial Angiofibromas of Tuberous Sclerosis Complex)
Important: "Adenoma sebaceum" is a misnomer — these are facial angiofibromas, a cutaneous hallmark of Tuberous Sclerosis Complex (TSC). They are not true adenomas of sebaceous glands.
Diagnosis
Classic triad of TSC (Bourneville's triad):
- Epilepsy (seizures — 80% of patients)
- Intellectual disability / developmental delay (60%)
- Adenoma sebaceum / facial angiofibromas (75%)
| Feature | Details |
|---|---|
| Lesion appearance | Multiple small, smooth, pink-to-red papules over the nasolabial folds, cheeks, and chin in a butterfly distribution |
| Age of onset | Appear between the 4th and 10th year of life; progressive thereafter |
| Earlier cutaneous sign | Hypomelanotic "ash-leaf" macules appear before angiofibromas in ~90% of patients; detected under Wood's lamp (UV light at 360 nm) |
| Other cutaneous signs | Shagreen patch (collagenous skin patch), subungual/periungual fibromas, café-au-lait–like spots |
Genetics: Autosomal dominant; TSC1 gene (9q34.3 — hamartin) or TSC2 gene (16p13.3 — tuberin). Sporadic mutations account for ~75% of cases. Either mutation causes upregulation of mTOR signaling, driving hamartoma formation throughout multiple organs.
Multi-organ involvement to evaluate:
| Organ | Manifestation |
|---|---|
| Brain | Cortical tubers, subependymal nodules ("brain stones"), subependymal giant cell astrocytomas (SEGAs) |
| Heart | Cardiac rhabdomyomas (may cause obstructive heart failure in neonates) |
| Kidney | Angiomyolipomas, renal cysts |
| Lung | Lymphangioleiomyomatosis (LAM) — particularly in women |
| Eye | Retinal hamartomas (phakomas) |
Management (Step by Step)
Step 1 — Clinical diagnosis + genetic testing
Diagnose clinically using the TSC diagnostic criteria. Genetic testing (TSC1/TSC2) is useful in atypical cases and for family genetic counseling.
Step 2 — Neuroimaging
- MRI brain — more sensitive for cortical tubers and subcortical lesions
- CT brain — better demonstrates calcified periventricular tubers ("brain stones")
- Serial MRI annually for patients <21 years; every 2–3 years thereafter to monitor SEGA growth
Step 3 — Systemic workup
- Echocardiography — especially in neonates/infants (cardiac rhabdomyomas)
- Renal ultrasound or MRI — screen for angiomyolipomas and cysts
- Pulmonary HRCT — in adolescent/adult females (LAM screening)
- Ophthalmology referral — retinal hamartoma evaluation
Step 4 — Seizure management
- Vigabatrin is first-line for infantile spasms (flexion spasms) in TSC
- ACTH suppresses flexor spasms in infancy and transiently normalizes EEG
- Standard antiepileptic drugs (AEDs) for other seizure types
- Everolimus (mTOR inhibitor): FDA-approved for intractable epilepsy due to TSC; evidence supports starting before clinical seizure onset to reduce severity
Step 5 — mTOR inhibitor therapy
- Everolimus (titrated to 5–15 ng/mL): reduces SEGA size by ≥50% in ~1/3 of patients; reduces angiomyolipoma size by ~40%
- Sirolimus (2 mg/day): approved for lymphangioleiomyomatosis; also shrinks bodily angiolipomas
- ⚠️ Lesions regrow upon discontinuation — therapy is ongoing
- Topical rapamycin (0.1%): shrinks facial angiofibromas; combination with 0.0003% calcitriol may be more effective
Step 6 — Cosmetic management of facial angiofibromas
- Dermabrasion — reduces facial lesions cosmetically; slow regrowth expected
- Laser therapy is an alternative option used at specialist centers
Step 7 — Surgical options
- Neurosurgical excision of single epileptogenic cortical tubers in otherwise-normal children with localized seizures
- Renal hamartoma resection only if impairing kidney function
Step 8 — Genetic counseling
Counsel family members; screen at-risk relatives with imaging and dermatologic exam. Refer to specialized TSC centers (e.g., Tuberous Sclerosis Alliance).
3. Cutis Marmorata
Diagnosis
Definition: A normal, transient mottled marbling pattern of the skin caused by vasospasm in response to cold (physiologic livedo reticularis).
| Feature | Details |
|---|---|
| Synonyms | Physiologic livedo reticularis, cutis marmorata |
| Mechanism | Cold → cutaneous vasospasm → irregular dilation of superficial capillaries and venules → reticulated violaceous/marbled network |
| Age group | Most prominent in neonates, infants, and young children |
| Distribution | Widespread; especially on lower extremities |
| Key feature | Disappears with warming — temperature-dependent |
| Prognosis | Benign and self-resolving |
Distinguish from Cutis Marmorata Telangiectatica Congenita (CMTC):
| Feature | Cutis Marmorata (Physiologic) | CMTC (Pathologic) |
|---|---|---|
| Cause | Cold/vasospasm | Congenital vascular malformation |
| Reversibility | Disappears with warming | Persistent — does not resolve with warming |
| Distribution | Generalized, symmetric | Often unilateral; lower extremity common |
| Associations | None | Limb asymmetry, telangiectasias, ulceration |
| Prognosis | Fully benign | 50% improve over first 2 years; may persist |
Secondary causes to rule out (especially if persistent or asymmetric):
- Systemic lupus erythematosus
- Raynaud phenomenon
- Polycythemia
- Hypothyroidism
- Down syndrome (common association)
Management (Step by Step)
Step 1 — Clinical recognition
Identify the mottled reticulated pattern on a cold-exposed or underdressed infant.
Step 2 — Warming test
Warm the infant — physiologic cutis marmorata should completely disappear. This is the essential diagnostic maneuver.
Step 3 — Reassure parents
Explain that this is a normal vasomotor response in infants and young children. No treatment is required.
Step 4 — Maintain warmth
Ensure the infant is kept adequately warm. Avoid unnecessary cold exposure.
Step 5 — Evaluate for persistence or associated features
If the mottling persists after warming, does not improve over time, or is associated with limb asymmetry, telangiectasias, or ulceration — consider CMTC and refer to a pediatric dermatologist.
Step 6 — Screen for secondary causes if atypical
If there are associated systemic signs (growth failure, dysmorphic features, etc.), evaluate for:
- Thyroid function tests (hypothyroidism)
- Complete blood count (polycythemia)
- ANA/complement (lupus)
- Chromosomal studies if dysmorphic features present
Step 7 — Follow-up
Physiologic cutis marmorata typically resolves as the child grows and thermoregulation matures. CMTC should be followed annually by dermatology.
4. Seborrheic Dermatitis (Infantile)
Diagnosis
| Feature | Details |
|---|---|
| Peak incidence | First 3 months of life; typically remits by 1–2 years |
| Common name | "Cradle cap" (when confined to scalp) |
| Morphology | Greasy, yellow-brown scales with mild underlying erythema |
| Scalp | Thick, waxy yellow scaling — most common presentation ("cradle cap") |
| Face | Eyebrows, nasolabial folds — erythema + greasy scale |
| Flexures/diaper area | Less scaling, more well-defined erythema; may overlap with infantile psoriasis ("sebopsoriasis") |
| Torso | Variable erythema and greasy scaling |
| Pruritus | Generally non-pruritic (key differentiator from atopic dermatitis) |
| Pathophysiology | Likely involves exaggerated immune response to Malassezia species colonization; hormonal and genetic factors also implicated; alterations in essential fatty acid patterns |
Complications:
- Impetiginization (secondary bacterial superinfection)
- Secondary Candida infection in intertriginous/diaper areas
Differential diagnosis:
- Atopic dermatitis — pruritic, starts after 2 months, cheeks and extensor surfaces, family history of atopy
- Infantile psoriasis — sharper borders, salmon-colored plaques, may have nail pits
- Langerhans cell histiocytosis — consider if rash is recalcitrant, associated with purpura, or systemic symptoms
- Tinea capitis — patchy hair loss, positive fungal culture
⚠️ Red flag: If seborrheic dermatitis is unusually severe, recalcitrant to treatment, or accompanied by failure to thrive, developmental delay, or recurrent infections — evaluate for immunodeficiency (e.g., HIV, Wiskott-Aldrich syndrome) and metabolic/nutritional disease.
Management (Step by Step)
Step 1 — Clinical diagnosis
Diagnose clinically from the characteristic greasy yellow scales, distribution, and non-pruritic nature.
Step 2 — Mild cases (cradle cap) — Mechanical removal
- Apply baby oil, mineral oil, or petroleum jelly to scalp; leave for 15–20 minutes
- Gently comb to loosen scales
- Shampoo hair to remove oil and scales
- Repeat 1–2 times per week
- Educate caregivers that shampooing is safe and important — scale buildup worsens if hair is not washed
Step 3 — Moderate scalp involvement — Antifungal shampoo
- Selenium sulfide 1–2.5% shampoo — used 2–3 times per week; leave on 5 minutes before rinsing
- Ketoconazole 2% shampoo — effective against Malassezia; current WHO guidelines recommend ketoconazole as first-line antifungal
Step 4 — Facial/body involvement or persistent scalp disease — Topical corticosteroids
- Apply low-potency topical corticosteroid (hydrocortisone 1% cream) to affected areas for short-term use
- Avoid high-potency steroids on infant skin; monitor for cutaneous atrophy
- Topical calcineurin inhibitors (pimecrolimus, tacrolimus) are not approved for infants <2 years; use with caution as second-line in older children
Step 5 — Secondary infection management
- Candidal superinfection: topical antifungal (nystatin or clotrimazole cream)
- Bacterial impetiginization: topical mupirocin; systemic antibiotics if extensive
Step 6 — Maintenance and caregiver education
- Regular gentle cleansing with mild, pH-neutral baby shampoo
- Avoid occlusive/greasy products that promote Malassezia growth
- Reassure that the condition typically resolves spontaneously by 1–2 years of age
Step 7 — Follow-up
If the rash persists beyond 2 years, recurs, or worsens despite treatment, reassess the diagnosis and screen for associated conditions (immunodeficiency, metabolic disorders).
Quick Reference Summary
| Condition | Key Diagnostic Feature | Treatment |
|---|---|---|
| Erythema Toxicum Neonatorum | Broad erythematous flare + central follicular pustule; day 2–3 of life; eosinophils on smear | Reassurance only; self-resolves by day 10 |
| Adenoma Sebaceum (TSC) | Facial angiofibromas + ash-leaf spots + seizures + developmental delay; mTOR mutation | mTOR inhibitors (everolimus/sirolimus); AEDs; topical rapamycin; multidisciplinary surveillance |
| Cutis Marmorata | Mottled reticulated pattern resolving with warming | Reassurance + warmth; rule out CMTC if persistent |
| Seborrheic Dermatitis | Greasy yellow scales ("cradle cap"); non-pruritic; first 3 months; Malassezia | Oil + combing; antifungal shampoo; low-potency topical steroids for moderate disease |
Sources: Andrews' Diseases of the Skin (9780323547536); Harriet Lane Handbook 23e (9780323876988); Fitzpatrick's Dermatology (9780071837781); Adams and Victor's Principles of Neurology 12e (9781264264520); Goldman-Cecil Medicine (9780323930345); Swanson's Family Medicine Review (9780323698115); Dermatology 2-Volume Set 5e (9780702082252)
This is a shared conversation. Sign in to Orris to start your own chat.