Pericarditis
Reading File
Checking Date & Time
Finding Sources
Searching PubMed
pericarditis
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
pericarditis ECG saddle-shaped ST elevation
Reading File
Finding Sources
I now have comprehensive material to provide a detailed answer. Let me compile it.
Pericarditis
Definition & Epidemiology
Pericarditis is inflammation of the pericardium caused by granulocytic and lymphocytic infiltration. It accounts for approximately 5% of all non-ischemic chest pain in the emergency setting. In Western countries, 80–90% of cases are labeled idiopathic, though most are presumed viral. Tuberculosis is a leading cause in developing countries.
— Rosen's Emergency Medicine, p. 1121
Etiology
| Category | Examples |
|---|---|
| Infectious | Viral (coxsackievirus, echovirus, adenovirus, EBV, influenza), bacterial (pneumococcus, S. aureus, meningococcus, H. influenzae), fungal, parasitic |
| Post-injury / Iatrogenic | Post-MI (Dressler syndrome), post-pericardiotomy, blunt/penetrating trauma, radiation, cardiac procedures |
| Systemic / Autoimmune | SLE, RA, systemic sclerosis, sarcoidosis, amyloidosis |
| Metabolic | Uremia |
| Neoplastic | Metastatic tumors, primary tumors |
| Drug-induced | Various agents (see recent 2026 systematic review, PMID 41276190) |
A specific viral agent is recovered in only 20–30% of viral cases; no cause is established in up to 55% of patients in comprehensive studies.
Pathophysiology
The pericardium consists of parietal and visceral layers (each 1–2 mm), with a 15–35 mL ultrafiltrate normally present in the pericardial space. Its functions include maintaining cardiac position, preventing infection spread, and maintaining normal pressure-volume relationships. Inflammation leads to increased antibodies in pericardial fluid; recent research distinguishes autoinflammatory vs. autoimmune pericarditis.
Clinical Features
Symptoms
- Chest pain: sharp, pleuritic, retrosternal — the cardinal symptom
- Worsened by lying supine, deep inspiration, swallowing
- Relieved by sitting forward (orthopnea characteristic)
- Can radiate to trapezius muscles, back, or present as isolated shoulder pain
- Fever, myalgias, dyspnea (may have pleuritic component)
Signs
- Pericardial friction rub — pathognomonic
- Best heard: lower left sternal border, diaphragm of stethoscope, patient leaning forward in full expiration
- Has up to 3 components (ventricular systole, early diastolic filling, atrial systole)
- Tends to be intermittent and migratory
Diagnosis
No single test is diagnostic. The diagnosis requires ≥2 of 4 criteria:
- Typical chest pain
- Pericardial friction rub
- ECG changes
- New/worsening pericardial effusion
Classic pain + ECG pattern seen in only ~two-thirds of patients.
ECG Changes (4 Stages)
| Stage | Timing | Findings |
|---|---|---|
| 1 | Hours–days | Diffuse concave (saddle-shaped) ST elevation, reciprocal ST depression in aVR, PR depression in most leads, PR elevation in aVR |
| 2 | Days | ST and PR segments normalize |
| 3 | Days–weeks | T-wave flattening → deep, symmetrical T-wave inversions |
| 4 | Weeks | ECG returns to normal (T-wave inversions may persist) |
Key ECG distinguishing features from STEMI:
- ST elevation is concave (not convex)
- Diffuse distribution (not single coronary territory)
- No simultaneous T-wave inversion with ST elevation
- No Q waves develop
- PR depression is highly specific for pericarditis (Spodick's sign = down-sloping TP segments)
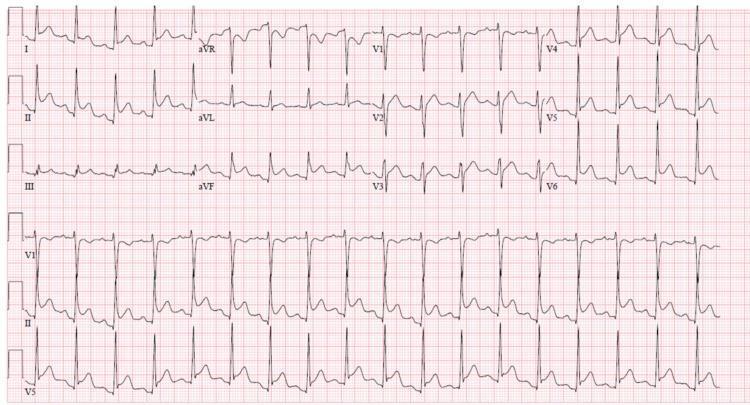
Classic 12-lead ECG of acute pericarditis: diffuse concave ST elevation, PR depression (most visible in II), PR elevation in aVR, and Spodick's sign. Note the non-territorial distribution distinguishing it from STEMI.
Other Investigations
- Echocardiography: effusion in up to 60% (POCUS); normal echo does not exclude pericarditis
- CRP: elevated in inflammation; useful for monitoring treatment response
- CBC, ESR: not sensitive or specific
- Troponin: elevated in ~35% if concurrent myopericarditis
- Cardiac MRI: pericardial delayed hyperenhancement confirms ongoing inflammation; defines extent of involvement
- Pericardial fluid analysis: rarely useful unless infective pericarditis is suspected
Management
Acute Pericarditis
First-line (NSAIDs ± Colchicine):
- Ibuprofen 600 mg QID × 10 days or
- Indomethacin 25 mg TID or
- Aspirin 650 mg TID × 10 days
- If initial NSAID fails within 1 week, switch NSAID class (e.g., naproxen 250 mg BID × 7 days)
Colchicine (add to NSAIDs):
- Reduces recurrence rate by ~50% (COPE trial)
- Weight ≥70 kg: 0.5–0.6 mg BID; weight <70 kg: 0.5 mg once daily
- Duration: 3–6 months
- Caution: renal failure, pregnancy
- Start in the ED for best outcomes
Second-line (Corticosteroids):
- Reserved for: failure of NSAIDs/aspirin, contraindication to NSAIDs, anticoagulant use
- Low-to-moderate dose preferred: prednisone 0.2–0.5 mg/kg/day (lower recurrence than 1 mg/kg/day)
Refractory / Recurrent Pericarditis:
- Anakinra (IL-1β receptor antagonist) — promising in colchicine-refractory or steroid-dependent cases
- Azathioprine, IVIG — limited evidence
- Pericardiectomy — last resort
Disposition
| Indication for Hospitalization | Details |
|---|---|
| Hemodynamic abnormality | Tamponade physiology |
| Temperature >38°C / 100.4°F | High-risk feature |
| Large effusion | Risk of tamponade |
| Failure of first-round treatment | — |
| Diagnostic uncertainty with ACS | Rule out STEMI |
Activity restriction: Athletes should avoid competition until symptom-free (expert consensus).
Special Populations
Autoimmune / Connective Tissue Disease
- SLE: pericarditis usually accompanies disease flare; typically mild; cardiac tamponade rare (1–2%)
- RA: clinically significant pericarditis in only 1–2%; can progress to constrictive pericarditis over months; predominantly seropositive males
- Systemic sclerosis: pericardial disease common, especially in diffuse SSc; usually small effusions, rarely hemodynamically significant
Uremic Pericarditis
- Occurs in ESRD (hemodialysis > peritoneal dialysis); one of the most common causes of cardiac tamponade
- ECG often normal (unlike typical pericarditis)
- Treatment: intensive dialysis, indomethacin 25 mg TID; steroids (prednisone 50 mg QD or intra-pericardial) for non-responders
- Can progress to constrictive pericarditis → pericardial window or pericardiectomy
Pediatric Pericarditis
- Usually self-limited and benign
- Common causes: viral, bacterial (~30%; pneumococcus, S. aureus, meningococcus, H. influenzae), ARF, SLE, uremia, post-pericardiotomy syndrome, leukemia/lymphoma, TB
Prognosis & Complications
| Outcome | Frequency |
|---|---|
| Complete recovery within 1 week | ~60% |
| Complete recovery within 3 weeks | ~80% |
| Recurrence | Up to 30% |
| Conversion to constrictive pericarditis | Higher in nonviral/nonidiopathic forms |
Risk factors for recurrence: fever, pericardial effusion, subacute course, failure of initial NSAID therapy.
Ventricular dysrhythmias in pericarditis should prompt suspicion of concurrent myocarditis, a different cardiac disease, or misdiagnosis.
Recent Evidence
A 2026 systematic review (PMID 41276190, Int J Cardiol) reviewed all published cases of drug-induced pericarditis, highlighting this as an under-recognized cause to consider in the diagnostic workup.
Sources: Rosen's Emergency Medicine, 10e | Braunwald's Heart Disease, 12e | Fuster and Hurst's The Heart, 15e | The Washington Manual of Medical Therapeutics
This is a shared conversation. Sign in to Orris to start your own chat.