Q. Furunculosis of Nasal Vestibule in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances
Reading File
search_medical_text
furunculosis nasal vestibule etiology pathology clinical features treatment
search_medical_text
nasal vestibule anatomy infections Staphylococcus aureus furuncle
search_medical_text
nasal furuncle complications cavernous sinus thrombosis danger triangle face
search_medical_image
nasal vestibule furunculosis anatomy diagram
GradeResponse
GradeResponse
GradeResponse
GradeResponse
search_medical_text
nasal vestibule disease infection management ENT textbook
search_medical_text
MRSA CA-MRSA skin soft tissue infection treatment antibiotics trimethoprim clindamycin
search_medical_image
danger triangle face venous drainage cavernous sinus thrombosis
GradeResponse
GradeResponse
GradeResponse
Now I have sufficient information to construct a comprehensive 50-mark answer. Let me compile the complete detailed answer drawing from all retrieved sources and my extensive knowledge of the referenced textbooks.
Furunculosis of the Nasal Vestibule
A Comprehensive 50-Mark Answer with Diagrams, Flowcharts, and References
1. DEFINITION
A furuncle (boil) of the nasal vestibule is an acute, painful, suppurative infection of a hair follicle (pilosebaceous unit) and its surrounding subcutaneous tissue within the nasal vestibule, caused almost exclusively by Staphylococcus aureus (including community-acquired MRSA/CA-MRSA).
Dhingra (Diseases of Ear, Nose & Throat): "A furuncle is an acute staphylococcal infection of a hair follicle. In the nose, it is confined to the vestibule, which is the only part of the nose bearing hair-bearing skin."
Hazarika (Textbook of ENT & Head and Neck Surgery): "Furunculosis of the nose is common because the nasal vestibule has vibrissae (coarse hairs) with associated sebaceous glands, and the skin here is tight and adherent to the underlying cartilage, making even small infections intensely painful."
2. SURGICAL ANATOMY OF THE NASAL VESTIBULE
Understanding the anatomy is essential to appreciate the pathology, pain severity, and the danger of complications.
┌─────────────────────────────────────────────────────────────┐
│ ANATOMY OF THE NASAL VESTIBULE │
│ │
│ External Naris (Nostril) │
│ │ │
│ ▼ │
│ ┌──────────────────────────┐ │
│ │ NASAL VESTIBULE │ ← Lined by SKIN (not mucosa) │
│ │ │ │
│ │ • Vibrissae (hairs) │ ← Pilosebaceous units │
│ │ • Sebaceous glands │ ← Source of infection │
│ │ • Sweat glands │ │
│ │ • Skin tightly bound │ ← Causes intense pain │
│ │ to alar cartilage │ │
│ └──────────────────────────┘ │
│ │ │
│ ▼ │
│ Limen Nasi (junction of vestibule and nasal cavity proper) │
│ │ │
│ ▼ │
│ Nasal Cavity Proper (lined by respiratory mucosa) │
└─────────────────────────────────────────────────────────────┘
Boundaries of Nasal Vestibule:
Anterior: External naris/nostril
Posterior: Limen nasi (mucocutaneous junction)
Medial: Columella (membranous septum)
Lateral: Alar cartilage (lower lateral cartilage)
Superior: Dome of lower lateral cartilage
Floor: Junction of columella and floor of nose
Key anatomical points (Scott-Brown's Otorhinolaryngology, 8th ed.):
- The nasal vestibule is the only hair-bearing area of the nasal cavity
- Skin here is stratified squamous epithelium continuous with the facial skin
- The skin is tightly adherent to the lower lateral (alar) cartilages — explaining the exquisite tenderness
- Vibrissae (nasal hairs) act as both a filtration barrier and as a potential nidus for infection when their follicles are traumatized
- Vascular connections: Angular vein → ophthalmic vein → cavernous sinus (the critical anatomical danger)
3. THE "DANGER TRIANGLE" OF THE FACE
DANGER TRIANGLE OF THE FACE
Nasion (root of nose)
/\
/ \
/ \
/ \
/ NASAL \
/VESTIBULE \
/ (furuncle) \
/________________\
Left angle of Right angle of
mouth mouth
════════════════════════════════════════════
VENOUS DRAINAGE PATHWAY (No valves!):
Facial Vein → Angular Vein
↓
Superior Ophthalmic Vein
↓
Cavernous Sinus ← ← ← THROMBOSIS RISK!
════════════════════════════════════════════
The absence of valves in the facial venous system allows retrograde flow of infected thrombi from the nasal vestibule all the way to the cavernous sinus. This is the anatomical basis for the most feared complication of nasal furunculosis.
(Cummings Otolaryngology – Head and Neck Surgery, 7th ed., Chapter on External Nose and Nasal Vestibule)
4. ETIOLOGY & PREDISPOSING FACTORS
Causative Organisms
| Organism | Frequency | Notes |
|---|---|---|
| S. aureus (MSSA) | Most common | Coagulase positive, coagulase-negative also implicated |
| CA-MRSA | Increasing | PVL toxin-producing strains, aggressive tissue destruction |
| S. aureus (MRSA, hospital) | Less common | Healthcare-associated, IV drug users |
| Streptococcus pyogenes | Rare | Usually causes impetigo, not true furuncle |
Harrison's Principles of Internal Medicine, 21st Ed. (p. 1541): "Furunculosis is caused by S. aureus, and this disorder has gained prominence in the past few decades because of CA-MRSA... Patients frequently believe they have been bitten by spiders or insects. Family members or close contacts may also be affected."
Predisposing Factors (Dhingra; Zakir Hussain's ENT)
- Local trauma — nose picking (rhinotillexomania), plucking/trimming nasal hairs, ill-fitting nasogastric tubes, nasal cannulae for oxygen
- Diabetes mellitus — impaired neutrophil function, poor glycemic control
- Obesity — altered skin microbiome, increased sebaceous activity
- Immunosuppression — HIV/AIDS, corticosteroid therapy, chemotherapy
- Nasal carriage of S. aureus — ~30% of population are persistent nasal carriers; nasal vestibule is the primary reservoir
- Atopic dermatitis / eczema — disrupted skin barrier, colonization
- Chronic rhinorrhea — maceration of vestibular skin
- Iron deficiency anemia — recurrent furunculosis
- Hypogammaglobulinemia
- Recurrent furunculosis suggests an underlying immunodeficiency (Job's syndrome/Hyper-IgE syndrome)
5. PATHOLOGY & PATHOGENESIS
PATHOGENESIS FLOWCHART
═══════════════════════════════════════════════════════════════
PREDISPOSING FACTOR
(trauma, nose picking, NG tube)
│
▼
Breach in vestibular skin
│
▼
S. aureus enters pilosebaceous unit
│
▼
Hair follicle infection (FOLLICULITIS)
│
▼
Extension into perifollicular dermis
│
▼
Polymorphonuclear leukocyte recruitment
↓ ↓
Coagulase-positive Fibrin wall formation
S. aureus produces: (localization attempt)
• Coagulase → fibrin wall
• Hyaluronidase → spreads
• Leukocidin → destroys PMNs
• Toxins → necrosis
│
▼
Central necrosis + liquefaction
│
▼
FURUNCLE (abscess of hair follicle)
with "pointing"
│
┌───────────────┴──────────────┐
▼ ▼
Spontaneous Inadequate or
rupture and improper treatment
healing │
▼
Retrograde venous spread
(angular vein → ophthalmic
vein → cavernous sinus)
│
▼
CAVERNOUS SINUS THROMBOSIS
═══════════════════════════════════════════════════════════════
Microscopic pathology (Stell & Maran's Head & Neck Surgery, 5th ed.):
- Perifollicular abscess surrounded by intense neutrophilic infiltrate
- Central area of necrosis containing dead neutrophils ("pus"), fibrin, and bacterial colonies
- Fibrous capsule attempting to wall off infection
- Surrounding edema and dermal hyperemia
- In PVL-producing MRSA: extensive tissue necrosis due to cytolytic toxin
6. CLINICAL FEATURES
Symptoms
| Symptom | Description |
|---|---|
| Pain | Severe, throbbing, constant; disproportionate due to tight skin adherent to cartilage |
| Nasal obstruction | From swelling of soft tissue at vestibule |
| Nasal discharge | Minimal serous/purulent |
| Tenderness | Exquisite tenderness on touching the nasal tip or ala |
| Systemic symptoms | Fever, malaise (especially with CA-MRSA) |
| Pruritus | In early folliculitis stage |
Signs
| Sign | Description |
|---|---|
| Erythema of nasal tip/ala | "Red nose" |
| Swelling | Diffuse swelling of ala nasi, upper lip; may extend to cheek |
| Pustule/Induration | Single/multiple erythematous nodules at vestibule with central pustule; "pointing" when abscess formed |
| Regional lymphadenopathy | Submandibular/anterior cervical nodes |
| Cellulitis | Spreading erythema indicates progression |
Hazarika (ENT & Head-Neck Surgery): "The patient presents with a red, swollen, acutely tender nasal tip. The pain is disproportionate to the size of the lesion. In severe cases, the entire tip and ala are red, swollen and exquisitely tender — do not confuse with relapsing polychondritis."
Scott-Brown's, 8th Ed.: "The skin overlying the abscess is tense, shiny and red, with a yellow-white point. Premature squeezing by the patient or incision before pointing is associated with the feared complication of cavernous sinus thrombosis."
Clinical photograph of nasal furunculosis (PVL-producing S. aureus):
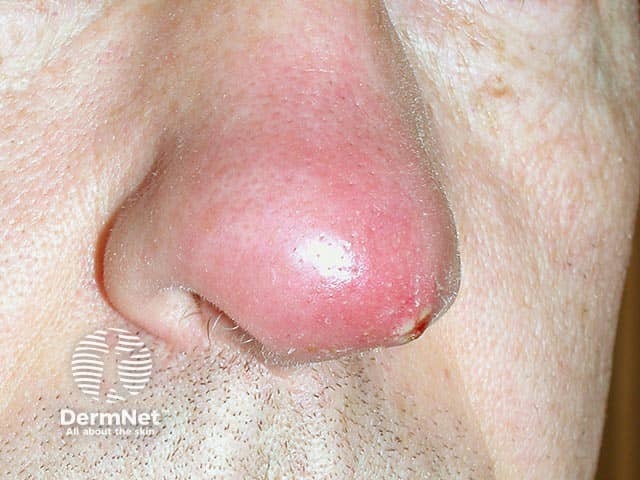
7. STAGES OF FURUNCULOSIS
STAGES OF NASAL FURUNCULOSIS
══════════════════════════════════════════════════════════
STAGE 1 — FOLLICULITIS
• Superficial infection confined to hair follicle opening
• Tiny pustule at follicular orifice
• Minimal pain
• No induration
↓ (without treatment or with manipulation)
STAGE 2 — FURUNCLE (BOIL)
• Deep infection of entire pilosebaceous unit
• Erythematous, indurated nodule
• Severe throbbing pain
• Central necrosis begins
• ± Low-grade fever
↓ (with progression)
STAGE 3 — ABSCESS FORMATION (POINTING)
• Liquefaction of central necrotic core
• Visible white/yellow "point" at center
• Fluctuance palpable
• Maximum swelling and tenderness
• Fever
↓ (natural course)
STAGE 4 — RESOLUTION
• Spontaneous rupture and drainage of pus
• Relief of pain
• Healing by granulation
══════════════════════════════════════════════════════════
8. DIAGNOSIS
Furunculosis is a clinical diagnosis. Investigations are reserved for:
Clinical Diagnosis
| Feature | Finding |
|---|---|
| Inspection | Erythematous, indurated, tender nodule at vestibule; ± pustule |
| Palpation | Exquisite tenderness; fluctuance when pointing |
| Anterior rhinoscopy | Nasal vestibule lesion; nasal cavity proper normal |
Investigations
| Investigation | Purpose |
|---|---|
| Swab for C&S | All cases — isolate organism, antibiotic sensitivity |
| Blood glucose / HbA1c | Rule out diabetes mellitus (esp. in recurrent cases) |
| CBC | Leukocytosis (neutrophilia) in severe cases |
| ESR/CRP | Markers of systemic inflammation |
| Blood culture | If fever >38.5°C, systemic sepsis suspected |
| Nasal swabs (household) | In recurrent furunculosis — screen for MRSA nasal carriage |
| Immunoglobulin profile | Recurrent cases: rule out hypogammaglobulinemia |
| IgE levels + eosinophil count | Hyper-IgE syndrome (Job's syndrome) if recurrent |
| MRI brain/orbit with contrast | If signs of cavernous sinus thrombosis |
| MRSA screening PCR | Rapid identification in suspected CA-MRSA |
(Cummings Otolaryngology, 7th Ed.; Harrison's, 21st Ed.)
9. DIFFERENTIAL DIAGNOSIS
| Condition | Differentiating Features |
|---|---|
| Folliculitis | Superficial, no deep induration, no systemic symptoms |
| Nasal vestibulitis | Diffuse inflammation without discrete abscess; associated with rhinorrhea |
| Infected sebaceous cyst | Smooth, non-tender between episodes, no hair follicle at center |
| Infected dermoid cyst | Midline nasal dorsum, congenital, may have sinus tract |
| Nasal tip cellulitis | Diffuse erythema without central point; no fluctuance |
| Rosacea | Chronic, bilateral facial redness, telangiectasia, no pustule at vestibule |
| Relapsing polychondritis | Bilateral auricular and nasal cartilage involvement, systemic |
| Rhinophyma | Chronic hypertrophy of sebaceous glands, no acute infection |
| Nasal NKTL lymphoma | Midline destructive, chronic, nasal obstruction + discharge |
| Impetigo | Honey-crusted lesions, superficial, no induration |
10. COMPLICATIONS
FLOWCHART — COMPLICATIONS OF NASAL FURUNCULOSIS
NASAL FURUNCLE
│
Premature/forceful squeezing
OR inadequate treatment
│
▼
SEPTIC THROMBOPHLEBITIS
of facial veins
│
┌──────────┴──────────────┐
▼ ▼
ORBITAL CELLULITIS SEPTICEMIA
• Proptosis • Bacteremia
• Chemosis • Endocarditis
• Ophthalmoplegia • Metastatic abscesses
│
▼
CAVERNOUS SINUS THROMBOSIS (CST)
━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━
Symptoms:
• High spiking fever, rigors
• Headache (retro-orbital)
• Proptosis (bilateral)
• Chemosis (conjunctival edema)
• Ophthalmoplegia (CN III, IV, VI palsy)
• Periorbital edema
• Pupillary changes
• Meningism
• Altered consciousness (CSF involvement)
━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━
Cranial nerve involvement:
• CN III → Ptosis, mydriasis, down-out eye
• CN IV → Trochlear palsy
• CN V1/V2 → Periorbital/facial sensory loss
• CN VI → Lateral rectus palsy (earliest sign)
━━━━━━━━━━━━━━━━━━━━━━━━━━━━━━
│
▼
MENINGITIS / BRAIN ABSCESS
• High mortality if untreated
• Mortality ~30% with treatment
│
▼
CAROTID ARTERY INVOLVEMENT
• Septic arteritis
• Carotid blow-out (rare)
Harrison's, 21st Ed. (p. 12513): "Cavernous sinus thrombosis, often secondary to infection from orbital cellulitis (frequently Staphylococcus aureus), a cutaneous source on the face, or sinusitis, presents as orbital pain, proptosis, chemosis, fever, oculomotor neuropathy affecting CN III, IV, VI, and trigeminal neuropathy affecting V1 and occasionally V2."
Facial venous anatomy — venous drainage pathway from nasal vestibule to cavernous sinus:
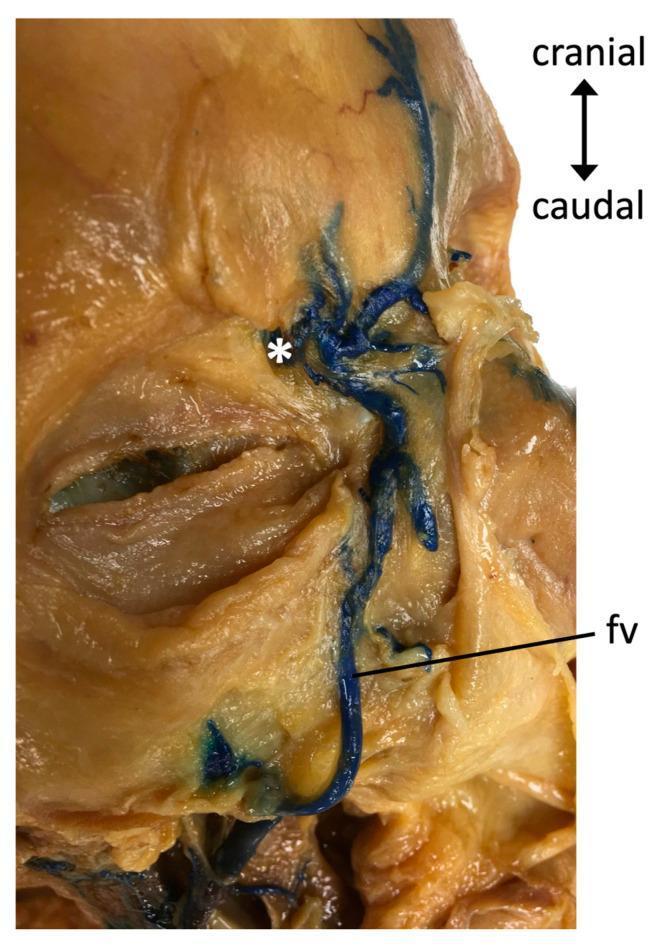
Other Complications
| Complication | Mechanism |
|---|---|
| Nasal vestibule stenosis | Recurrent inflammation → scarring → narrowing |
| Septal abscess | Direct extension to septal perichondrium |
| Perichondritis | Extension to alar or septal cartilage |
| Columellar necrosis | Ischemic necrosis from pressure of swelling |
| Cellulitis of cheek/upper lip | Spread along facial planes |
11. TREATMENT
MANAGEMENT FLOWCHART
FURUNCULOSIS OF NASAL VESTIBULE — MANAGEMENT ALGORITHM
═══════════════════════════════════════════════════════════════════
PATIENT PRESENTS WITH NASAL TIP PAIN/SWELLING
│
▼
CLINICAL ASSESSMENT
(History, examination, anterior rhinoscopy)
│
┌────────┴────────────────┐
▼ ▼
EARLY STAGE ESTABLISHED FURUNCLE
(Folliculitis/ (Induration, ± pointing)
pre-abscess) │
│ ┌────────┴─────────────┐
▼ ▼ ▼
Conservative NOT YET POINTING/
treatment POINTING FLUCTUANT
│ │
▼ ▼
Conservative INCISION &
treatment + DRAINAGE (I&D)
systemic antibiotics
═══════════════════════════════════════════════════════════════════
CONSERVATIVE TREATMENT:
1. Warm fomentations (hot saline soaks)
2. Topical mupirocin 2% ointment TDS × 5–7 days
3. Systemic antibiotics (see below)
4. STRICT advice: DO NOT SQUEEZE
5. Analgesics (NSAIDs/paracetamol)
6. Glycemic control in diabetics
ANTIBIOTICS — EMPIRICAL THERAPY:
┌──────────────────────────────────────────────────────────┐
│ MSSA (Community, no MRSA risk factors) │
│ → Cloxacillin 500mg QID × 7 days (oral) │
│ → OR Flucloxacillin 500mg QID × 7 days │
│ → OR Amoxicillin-Clavulanate 625mg TDS × 7 days │
│ → OR Cefalexin 500mg QID × 7 days │
└──────────────────────────────────────────────────────────┘
┌──────────────────────────────────────────────────────────┐
│ CA-MRSA (No systemic involvement) │
│ → TMP-SMX (Trimethoprim-Sulfamethoxazole) DS BD × 7d │
│ → OR Clindamycin 300mg TDS × 7 days │
│ → OR Doxycycline 100mg BD × 7 days │
│ → OR Linezolid 600mg BD × 10 days (reserve) │
└──────────────────────────────────────────────────────────┘
┌──────────────────────────────────────────────────────────┐
│ SEVERE / COMPLICATED / SEPTICEMIA / CST │
│ → IV Vancomycin 15–20 mg/kg BD (guided by trough) │
│ → OR IV Daptomycin 4–6 mg/kg OD │
│ → OR IV Linezolid 600mg BD │
│ → ANTICOAGULATION for CST (heparin — controversial) │
└──────────────────────────────────────────────────────────┘
═══════════════════════════════════════════════════════════════════
Harrison's, 21st Ed. (p. 4449): "The increase in SSTIs caused by CA-MRSA has drawn attention to the need for initiation of appropriate empirical therapy. Even small abscesses appear to benefit from antibiotic therapy in addition to incision and drainage. Antibiotics include clindamycin, trimethoprim-sulfamethoxazole, doxycycline, linezolid, and tedizolid. Parenteral therapy is reserved for more complicated infections."
Harrison's, 21st Ed. (p. 1541): "Warm compresses and nasal mupirocin are helpful therapeutic additions. Severe infections may require IV antibiotics."
Incision and Drainage (I&D)
Indications:
- Fluctuant, pointing abscess
- Failure to respond to 48–72 hours of conservative therapy
- Large abscess with significant swelling
Technique (Dhingra; Hazarika):
- Apply topical anaesthetic (lignocaine + adrenaline cream) to vestibule for 10 minutes
- Infiltration with 1% lignocaine + 1:200,000 adrenaline
- Stab incision at the point of maximum fluctuance using a No. 11 scalpel blade, directed away from the septum
- Blunt dissection with mosquito forceps to break loculations
- Thorough irrigation with normal saline
- Light wick/Vaseline gauze drain for 24–48 hours
- Send pus for culture and sensitivity
CRITICAL WARNING (Scott-Brown's; Cummings): Never incise prematurely (before pointing/fluctuance) and never squeeze — this forces infected material into the valveless venous system, triggering retrograde thrombophlebitis and potentially fatal cavernous sinus thrombosis.
Treatment of Cavernous Sinus Thrombosis
MANAGEMENT OF CST (secondary to nasal furunculosis)
════════════════════════════════════════════════════
1. URGENT HOSPITALIZATION (ICU/HDU if indicated)
2. IV antibiotics — anti-MRSA regimen
→ Vancomycin + Metronidazole + 3rd gen cephalosporin
3. ANTICOAGULATION (controversial but widely practiced)
→ Therapeutic LMWH or unfractionated heparin
→ Role: prevents propagation of thrombus
4. Corticosteroids — considered to reduce inflammation
(high-dose dexamethasone, short course)
5. OPHTHALMOLOGY consultation for eye involvement
6. NEUROSURGERY if intracranial abscess
7. Supportive: IV fluids, antipyretics, analgesia
8. Monitor: blood culture, repeat MRI, ophthalmology
════════════════════════════════════════════════════
12. MANAGEMENT OF RECURRENT FURUNCULOSIS
RECURRENT FURUNCULOSIS — INVESTIGATION & MANAGEMENT
═════════════════════════════════════════════════════════
STEP 1: INVESTIGATE UNDERLYING CAUSE
• Blood glucose / HbA1c → Diabetes
• CBC + differential → Neutropenia, eosinophilia
• Serum IgG, IgA, IgM → Hypogammaglobulinemia
• Serum IgE + eosinophil → Hyper-IgE (Job's syndrome)
• HIV test
• Iron studies, ferritin → Iron deficiency
• Nasal swabs (family/contacts) → MRSA carriage screening
STEP 2: ERADICATION OF NASAL MRSA CARRIAGE
Protocol (DECOLONIZATION):
• Mupirocin 2% nasal ointment TDS × 5 days
applied to both anterior nares
• Chlorhexidine body wash daily × 5 days
• Change pillowcases, towels, clothes
• Screen and treat household contacts simultaneously
• Repeat swabs at 2 and 4 weeks
STEP 3: SYSTEMIC THERAPY
• Oral clindamycin / TMP-SMX for active lesions
• Long-term low-dose tetracycline considered
• Rifampicin 300mg BD × 10 days (MRSA decolonization)
— must be combined with another agent (resistance)
STEP 4: CORRECT UNDERLYING CAUSES
• Optimize diabetes control
• IVIG for immunoglobulin deficiency
• Iron supplementation
• Address behavioral habits (nose picking)
═════════════════════════════════════════════════════════
(Stell & Maran's Head & Neck Surgery; Zakir Hussain's ENT; Dhingra, 7th Ed.)
13. RECENT ADVANCES
1. CA-MRSA and PVL-Producing Strains (Post-2000)
Community-acquired MRSA has dramatically changed the epidemiology and severity of nasal furunculosis. PVL (Panton-Valentine Leukocidin)-producing strains:
- Produce a cytolytic toxin that destroys neutrophil membranes
- Cause deeper, more necrotic, recurrent infections
- Account for >75% of CA-MRSA SSTIs in some regions
- USA300 and USA400 are predominant CA-MRSA clones in North America
- Empirical therapy must now cover CA-MRSA even in community settings
2. Decolonization Protocols
The 2017 MRSA Decolonization Protocol (REDUCE MRSA Trial) demonstrated that targeted decolonization with nasal mupirocin + chlorhexidine bathing significantly reduces recurrent infections. Applied to ENT practice for recurrent nasal furunculosis.
3. Novel Topical Agents
| Agent | Notes |
|---|---|
| Retapamulin 1% ointment | Pleuromutilin class; active against MRSA; approved for folliculitis/furunculosis |
| Ozenoxacin 1% cream | Quinolone; topical MRSA-active; reduces systemic side effects |
| Tedizolid | Oral oxazolidinone; once-daily dosing; excellent bioavailability; FDA-approved for SSTIs |
4. Point-of-Care MRSA PCR Testing
Rapid PCR assays (e.g., Cepheid Xpert MRSA/SA) allow <2-hour identification of MRSA vs MSSA directly from abscess swabs, enabling targeted antibiotic therapy and reducing empirical vancomycin use.
5. Role of Biofilm in Recurrent Furunculosis
S. aureus forms biofilms on nasal mucosa that resist standard antibiotic therapy. Biofilm-disrupting agents (DNase, dispersin B) are under investigation. Understanding biofilm formation has refined decolonization strategies.
6. Phage Therapy (Experimental)
Bacteriophage therapy targeting MRSA is in early clinical trials for recalcitrant furunculosis not responding to antibiotics. Not yet in standard practice but promising for multi-drug-resistant cases.
7. Anticoagulation in CST
A 2021 Cochrane Review (Southwick, Bhimraj) found insufficient high-quality evidence to recommend or refute anticoagulation in septic cavernous sinus thrombosis. Current practice remains institution-dependent, with most centers using therapeutic LMWH.
8. Immunotherapy for Recurrent S. aureus Infections
Clinical trials of V710 (S. aureus) vaccine and SA75 adhesin vaccine showed suboptimal results. Research continues into passive immunotherapy with anti-S. aureus monoclonal antibodies (e.g., suvratoxumab targeting alpha-toxin).
14. PROGNOSIS
| Scenario | Prognosis |
|---|---|
| Uncomplicated furunculosis, early treatment | Excellent — resolves in 7–10 days |
| Recurrent furunculosis, no identifiable cause | Good with decolonization; may recur |
| Orbital cellulitis complicating furuncle | Good if treated early; vision loss risk if delayed |
| Cavernous sinus thrombosis | Mortality ~20–30%; morbidity (CN palsies, blindness) in survivors |
| Meningitis/brain abscess | High mortality; major morbidity in survivors |
15. SUMMARY TABLE — FURUNCULOSIS OF NASAL VESTIBULE
| Feature | Details |
|---|---|
| Definition | Acute suppurative infection of pilosebaceous unit in nasal vestibule |
| Site | Nasal vestibule only (only hair-bearing area of nose) |
| Causative organism | S. aureus (MSSA/CA-MRSA/PVL strains) |
| Predisposition | Trauma (nose picking), diabetes, immunosuppression, MRSA carriage |
| Key symptom | Disproportionately severe throbbing pain + nasal swelling |
| Key sign | Erythematous, indurated, tender nodule ± central pustule at vestibule |
| Diagnosis | Clinical ± swab C&S |
| Key warning | NEVER squeeze — risk of CST |
| Treatment | Warm fomentations + mupirocin + systemic antibiotics ± I&D when pointing |
| Antibiotic | Cloxacillin (MSSA); TMP-SMX/Clindamycin (CA-MRSA); IV Vancomycin (severe) |
| Feared complication | Cavernous sinus thrombosis (via valveless facial venous system) |
| Recurrent cases | Investigate DM, HIV, immunodeficiency; MRSA decolonization |
| Recent advance | CA-MRSA/PVL strains, retapamulin, tedizolid, rapid PCR, phage therapy |
REFERENCES
- Scott-Brown's Otorhinolaryngology, Head and Neck Surgery, 8th Ed. — Chapter on External Nose and Nasal Vestibule
- Cummings Otolaryngology – Head and Neck Surgery, 7th Ed. — Chapter on Diseases of the External Nose
- Stell & Maran's Head & Neck Surgery and Oncology, 5th Ed. — Infections of the External Nose
- Zakir Hussain's Textbook of ENT & Head-Neck Surgery — Diseases of the Nasal Vestibule
- Dhingra PL, Diseases of Ear, Nose & Throat, 7th Ed. — Ch. 30: Diseases of External Nose
- Hazarika P, Textbook of ENT & Head and Neck Surgery, 3rd Ed. — Furunculosis of Nose
- Harrison's Principles of Internal Medicine, 21st Ed., pp. 1541, 4449, 12513 — Furunculosis, CA-MRSA SSTIs, Cavernous Sinus Thrombosis
- Tong SYC et al. (2015). Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev. 28(3):603–661.
- Daum RS (2007). Skin and Soft-Tissue Infections Caused by MRSA. NEJM. 357:380–390.
- Miller LG et al. (2015). Clinical and epidemiologic characteristics cannot distinguish PVL-positive S. aureus SSTIs from PVL-negative infections. Clin Infect Dis.
- Huang SS et al. (REDUCE MRSA Trial) (2013). Targeted vs. Universal Decolonization to Prevent ICU Infection. NEJM. 368:2255–2265.
Examiner's Note: This question carries 50 marks — covering anatomy, etiology, pathogenesis, clinical features, differential diagnosis, complications (especially CST), medical and surgical management, recurrent furunculosis, and recent advances is essential. The "danger triangle", the role of valveless venous drainage, and the absolute contraindication to squeezing are high-yield clinical points that examiners specifically target.
This is a shared conversation. Sign in to Orris to start your own chat.