Alcoholic liver disease examination findings in inspection, palpation, percussion and auscultation.
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Loading Image
Searching Images
spider naevi alcoholic liver disease
I now have comprehensive material from Goldman-Cecil Medicine and Harrison's to construct a detailed, well-structured answer. Let me compile it.
Alcoholic Liver Disease — Physical Examination Findings
Alcoholic liver disease (ALD) encompasses a spectrum from hepatic steatosis → alcoholic hepatitis → cirrhosis. The examination findings vary by stage but overlap significantly. The structured approach below covers all four components of examination.
INSPECTION
General Appearance
- Muscle wasting — temporal wasting and generalised sarcopenia from poor nutrition and alcohol's catabolic effect
- Jaundice — best detected by examining the sclera (scleral icterus) or under the tongue where elastin retains bilirubin; present in alcoholic hepatitis and decompensated cirrhosis
- Fetor hepaticus — a musty, sweet-smelling breath caused by portosystemic shunting of mercaptans; indicates advanced disease
- Abdominal distension — visible with significant ascites; the flanks bulge outward and the umbilicus may evert
- Peripheral oedema — ankle and leg oedema from hypoalbuminaemia and portal hypertension
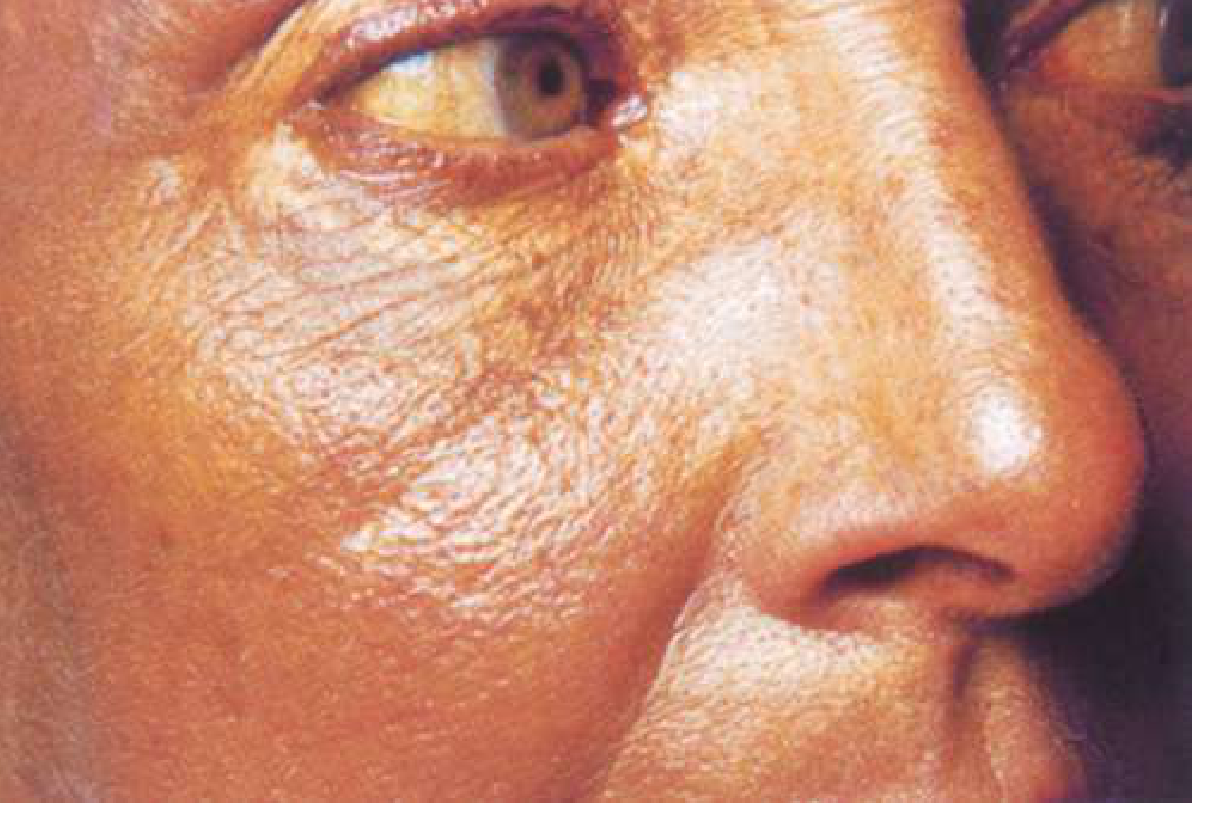
Skin & Mucocutaneous Signs
- Spider naevi — vascular lesions with a central arteriole and radiating capillaries on the face, neck, and thorax; >5 are significant; caused by elevated oestrogen from impaired hepatic metabolism
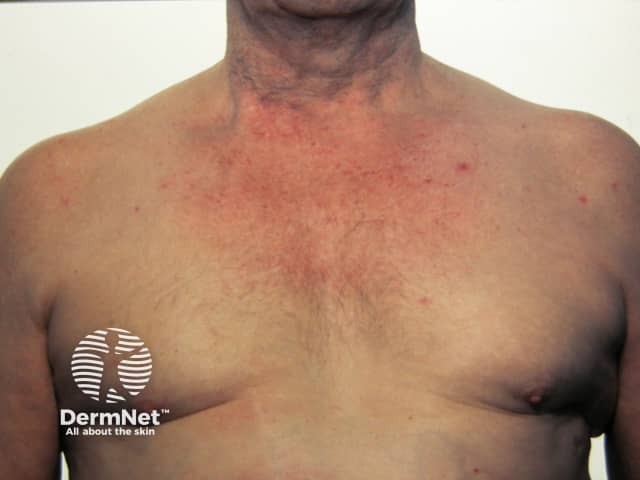
- Palmar erythema — bilateral erythema of the thenar and hypothenar eminences; suggests liver disease in men (can be normal in women)
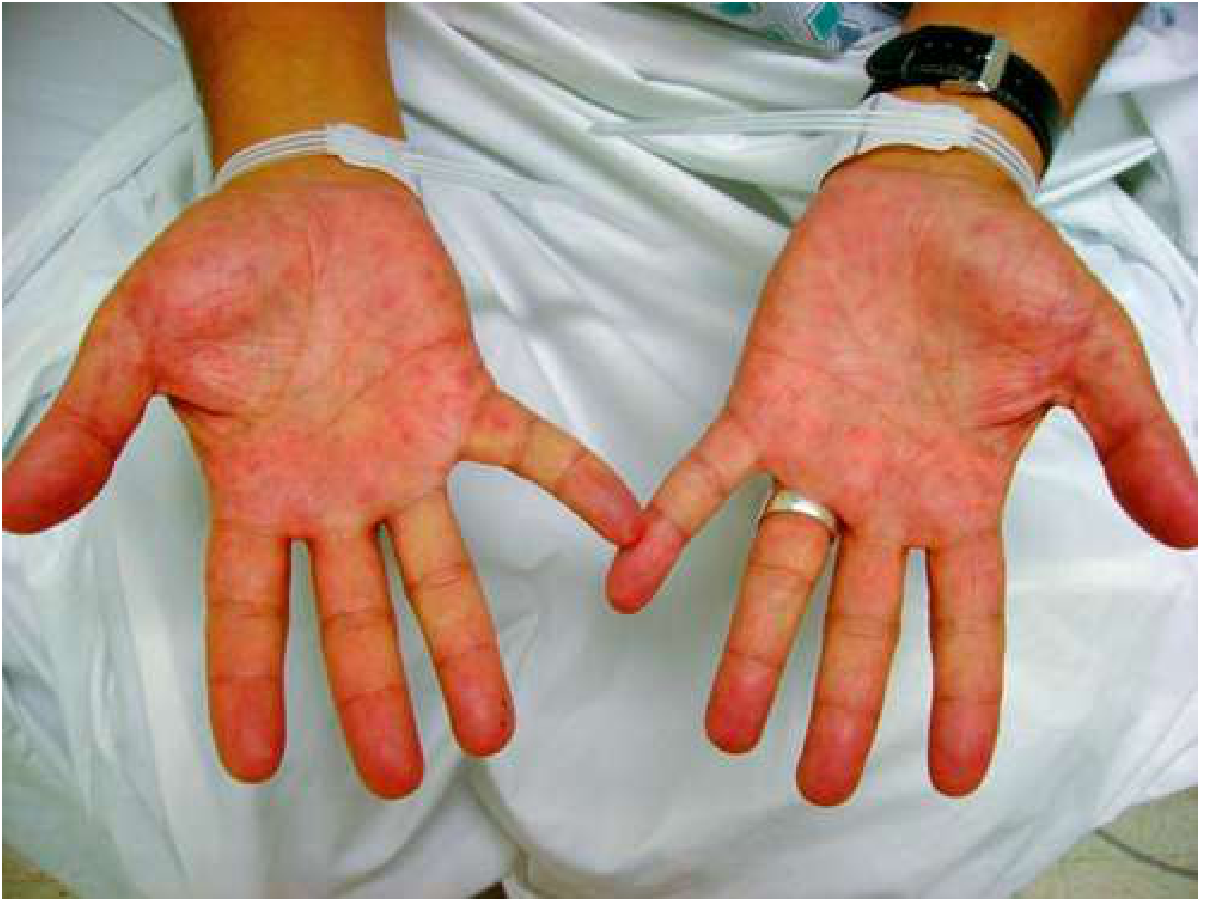
- Dupuytren's contracture — retraction of the palmar fascia with finger contracture; a sign specifically associated with alcoholic liver disease (also seen in epilepsy and diabetes)
- Leuconychia (white nails / Terry's nails) — patches of white discolouration on the nails in advanced liver disease
- Petechiae and ecchymoses — from impaired clotting factor synthesis and hypersplenism
- "Paper money" skin — atrophic facial skin with fine telangiectasiae; a sign of advanced liver disease
- Parotid gland swelling — bilateral parotid enlargement characteristic of alcoholic patients
- Poor dentition — common in alcoholics; excessive caries suggest alcohol-related neglect
Signs of Feminisation / Hormonal Changes (cirrhosis)
- Gynaecomastia — breast tissue enlargement in men (elevated oestrogen:androgen ratio)
- Loss of axillary and pubic hair
- Testicular atrophy
- Caput medusae — dilated periumbilical veins from recanalization of the umbilical vein due to portal hypertension; seen on abdominal inspection
Neurological (visible on inspection)
- Asterixis ("liver flap") — ask the patient to dorsiflex both wrists with arms extended for 15 seconds; a coarse flapping tremor indicates hepatic encephalopathy
- Constructional apraxia — inability to draw a five-pointed star; found in encephalopathy without altered consciousness
PALPATION
Liver
- In alcoholic fatty liver and alcoholic hepatitis: the liver is enlarged (hepatomegaly), smooth, and tender — similar to acute viral hepatitis or hepatic congestion
- In cirrhosis: the liver may be small and shrunken (late cirrhosis) or feel hard and irregular with a nodular edge — due to fibrosis and regenerative nodules
- The liver edge is best felt starting from the right lower quadrant, moving upward; normally smooth and up to 2 cm below the costal margin
- A liver edge that is unusually firm or nodular is a reliable sign of cirrhosis
- In ascites, a dipping/balloting technique (quick pressure with fingertips below the rib cage) may be needed to detect the liver edge
- The scratch test (stethoscope over right upper quadrant, scratch from mid-abdomen toward liver): sound is amplified overlying the liver — useful when ascites obscures the edge
Spleen
- Splenomegaly — a palpable spleen tip is a reliable sign of portal hypertension in chronic liver disease; also present in acute alcoholic hepatitis and infiltrative diseases
- In decompensated cirrhosis the spleen may be massively enlarged
Ascites
- Fluid thrill (fluid wave) — place the medial border of one hand on the abdomen; an assistant presses the midline to prevent fat transmission; tapping one flank transmits a wave felt by the other hand — indicates significant (>1–2 L) ascites
- Shifting dullness (see percussion below)
- Abdominal wall hernias — umbilical or inguinal hernias may develop with chronic ascites
- Scrotal oedema — in long-standing ascites
Tenderness
- Right upper quadrant tenderness — characteristic of alcoholic hepatitis (tender hepatomegaly)
- Abdominal tenderness with ascites — raises suspicion for spontaneous bacterial peritonitis (SBP), although SBP may be painless
Other
- Palpable gallbladder — suggests biliary obstruction; should be distinguished from the liver edge
- Murphy sign (pain on palpation during inspiration) — suggests cholecystitis, not ALD per se, but may be a coexisting problem
PERCUSSION
Liver Span
- Normal liver span: 6–12 cm in the midclavicular line
- Reduced liver span: suggests cirrhotic shrinkage
- Increased liver span (hepatomegaly): found in alcoholic fatty liver, alcoholic hepatitis, hepatic congestion, or early cirrhosis with inflammation
- The liver is dull to percussion over the right upper quadrant; loss of dullness (tympany) below the right costal margin = small or absent liver
Ascites
- Flank dullness — percussion from midline toward the flank; a change from tympany (gas-filled bowel) to dullness at the flanks indicates fluid
- Shifting dullness — the definitive percussion sign: identify the tympany-to-dullness transition, then ask the patient to roll toward the examiner; if the point becomes tympanic, fluid has shifted — confirms ascites. Repeat on both sides for confirmation. This indicates the fluid pool moves to the most dependent part of the abdomen.
Splenomegaly
- Dullness to percussion between the 9th and 11th ribs in the left midaxillary line suggests splenomegaly; normally this area is tympanic (resonant due to bowel)
AUSCULTATION
Hepatic Bruit
- A hepatic arterial bruit over the right upper quadrant can be heard in hepatocellular carcinoma (a complication of cirrhosis) or, occasionally, in severe acute alcoholic hepatitis
- Also heard in hepatic haemangioma or arteriovenous fistulae
Venous Hum
- A venous hum (Cruveilhier-Baumgarten murmur) — a continuous humming sound heard at the epigastrium/umbilicus — indicates recanalization of the paraumbilical veins due to portal hypertension; correlates with caput medusae on inspection
Hepatic Friction Rub
- A friction rub over the liver indicates hepatic infarction, tumour, or perihepatitis; uncommon in pure ALD but possible in hepatocellular carcinoma complicating cirrhosis
Cardiorespiratory Findings
- Tachycardia and wide pulse pressure — hyperdynamic circulation from peripheral vasodilation in cirrhosis
- Crepitations (rales) and raised JVP — if hepatic congestion is due to concomitant cardiac disease
- Absent breath sounds at the base — hepatic hydrothorax (transdiaphragmatic passage of ascitic fluid, more commonly right-sided)
Summary Table
| Examination | Finding | Significance |
|---|---|---|
| Inspection | Jaundice, scleral icterus | Hyperbilirubinaemia |
| Spider naevi (>5) | Hyperoestrogenaemia, cirrhosis | |
| Palmar erythema | Chronic liver disease | |
| Dupuytren's contracture | Specific to alcohol | |
| Parotid enlargement | Alcohol use | |
| Caput medusae | Portal hypertension | |
| Gynaecomastia, testicular atrophy | Cirrhosis (hormonal) | |
| Asterixis | Hepatic encephalopathy | |
| Muscle wasting, leuconychia | Advanced disease | |
| Fetor hepaticus | Portosystemic shunting | |
| Palpation | Tender, smooth hepatomegaly | Alcoholic hepatitis / fatty liver |
| Hard, nodular liver | Cirrhosis | |
| Splenomegaly | Portal hypertension | |
| Fluid thrill, ascites | Cirrhosis / decompensation | |
| RUQ tenderness | Alcoholic hepatitis | |
| Percussion | Reduced liver span | Cirrhotic shrinkage |
| Flank dullness, shifting dullness | Ascites | |
| Splenic dullness (L midaxillary, 9–11th ribs) | Splenomegaly | |
| Auscultation | Venous hum (epigastrium) | Portal hypertension (caput medusae) |
| Hepatic bruit | HCC complicating cirrhosis | |
| Absent breath sounds (base R) | Hepatic hydrothorax | |
| Tachycardia, wide pulse pressure | Hyperdynamic circulation |
Sources: Goldman-Cecil Medicine (International Edition), Chapter 132 — Approach to the Patient with Liver Disease; Harrison's Principles of Internal Medicine, 22nd ed., Chapter 347 — Approach to the Patient with Liver Disease
This is a shared conversation. Sign in to Orris to start your own chat.