Pulmonary embolism with latest guidelines
Reading File
Checking Date & Time
Finding Sources
Searching PubMed
"pulmonary embolism"[MeSH Terms] AND "diagnosis" AND "treatment"
Searching PubMed
"pulmonary embolism"[MeSH Terms] AND "anticoagulation"
Reading File
Reading File
Searching PubMed
"pulmonary embolism"[MeSH Terms] AND "guidelines"
Reading Article
Reading Article
Reading File
Reading File
Reading File
Searching the Web
2026 AHA ACC pulmonary embolism guidelines key recommendations clinical categories
Loading Image
Reading File
Searching the Web
2026 AHA ACC PE guideline clinical categories 1A 1B 2A 2B 3 anticoagulation DOAC recommendations
Searching the Web
2026 AHA ACC PE guideline five clinical categories A B C D E criteria hemodynamic RV dysfunction PERT
I now have all the information needed for a comprehensive, well-structured answer. Let me compile it.
Pulmonary Embolism: Comprehensive Clinical Overview with 2026 Guidelines
Guideline alert (April 2026): The 2026 AHA/ACC/ACCP/ACEP/CHEST/SCAI/SHM/SIR/SVM/SVN Guideline for the Evaluation and Management of Acute PE in Adults was published February 19, 2026 — the first dedicated joint AHA/ACC clinical practice guideline for acute PE. It replaces the old "massive/submassive/low-risk" terminology entirely. Full guideline in Circulation [PMID: 41712677]
1. Definition and Epidemiology
Pulmonary embolism (PE) is obstruction of the pulmonary arterial circulation, most commonly by thrombus originating from deep venous thrombosis (DVT) of the lower extremities. It is a leading cause of cardiovascular mortality, accounting for approximately 25% of sudden cardiac deaths. — Rosen's Emergency Medicine, p. 1202
Risk factors (Virchow's triad):
- Stasis: Immobility, prolonged travel, surgery
- Hypercoagulability: Cancer, thrombophilia (Factor V Leiden, prothrombin G20210A, protein C/S deficiency, antithrombin deficiency), oral contraceptives/HRT, antiphospholipid syndrome, pregnancy
- Endothelial injury: Trauma, surgery, indwelling catheters
2. Clinical Presentation
Symptoms range from asymptomatic (incidental) to sudden cardiovascular collapse. — Rosen's Emergency Medicine, p. 1202
| Symptom | Frequency |
|---|---|
| Dyspnea | 75–80% |
| Chest pain (pleuritic or non-pleuritic) | ~67% |
| Cough | variable |
| Hemoptysis | ~13% |
| Leg swelling (unilateral) | <30% |
| Syncope | <5% but significant |
- Fever from PE is typically low grade (<38.6°C); higher fever suggests infection
- Pleuritic pain occurs with peripheral PE causing pulmonary infarction
- PEA arrest (>20 depolarizations/min without palpable pulses) is the most common ECG finding in PE-related cardiac arrest
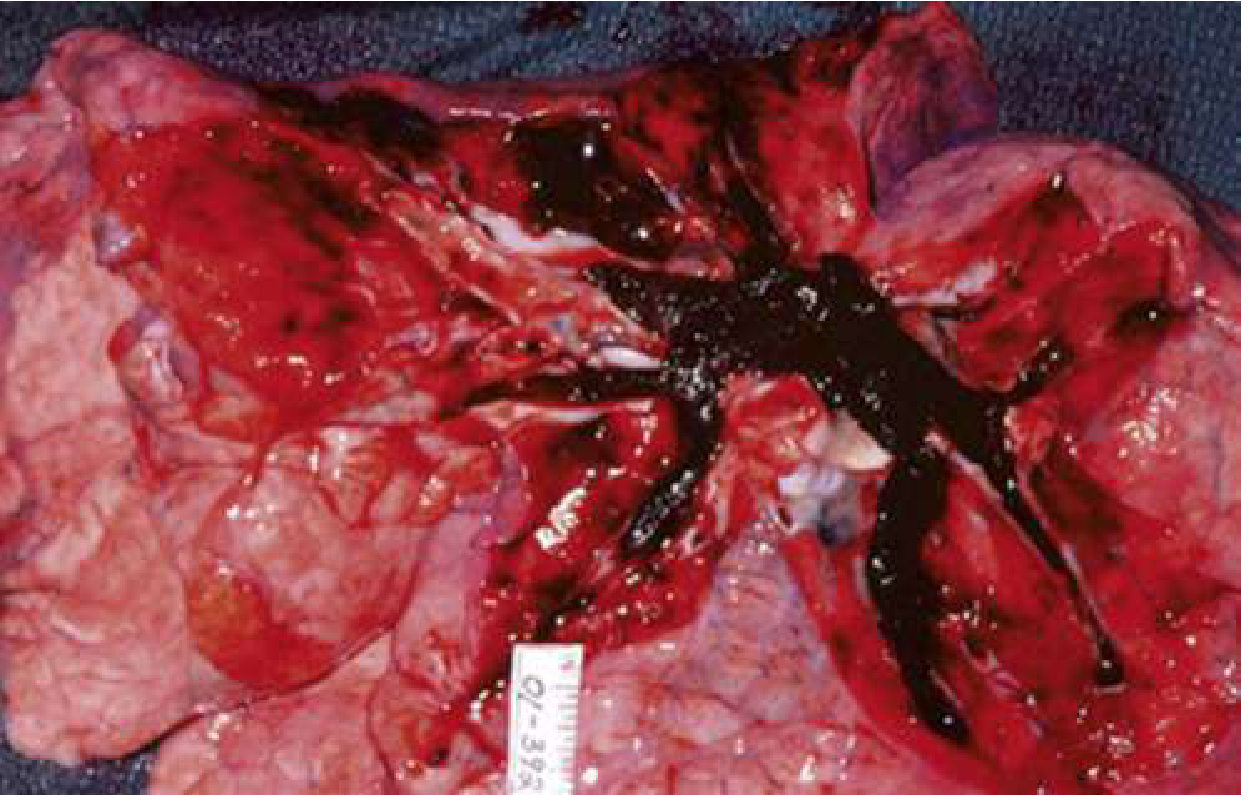
3. Diagnosis
Step 1: Pre-test Probability (PTP)
Wells Score for PE:
| Criterion | Points |
|---|---|
| Clinical signs of DVT | 3 |
| PE most likely diagnosis | 3 |
| HR > 100 | 1.5 |
| Immobilization/surgery in prior 4 weeks | 1.5 |
| Previous DVT/PE | 1.5 |
| Hemoptysis | 1 |
| Malignancy | 1 |
- ≤4 = Low/moderate probability; >4 = High probability; >6 = PE likely
Revised Geneva Score (fully objective, preferred in some systems):
- <4 points = low; 4–10 = intermediate; >10 = high
Step 2: PERC Rule (rule out without testing)
When clinical gestalt PTP is low, if all 8 criteria are met, no further testing is needed:
Age <50 | Pulse <100 | SaO₂ >94% | No unilateral leg swelling | No hemoptysis | No recent trauma/surgery | No prior PE/DVT | No hormone use — Rosen's Emergency Medicine, p. 1205
Step 3: D-Dimer
- Sensitivity: 95–98%; Specificity: 40–55%
- Use in non-high PTP patients only
- Age-adjusted cutoff: age × 10 μg/L for patients >50 years (reduces unnecessary CTPAs)
- A false-positive CTPA is more likely than a false-negative D-dimer; do not order imaging to "be safe" if D-dimer is negative
Step 4: Imaging
| Modality | Role |
|---|---|
| CT Pulmonary Angiography (CTPA) | Gold standard for PE diagnosis; first-line in most patients |
| V/Q scan | Preferred in contrast allergy, renal failure, pregnancy (reduced perfusion dose) |
| Echocardiography | Bedside; detects RV dysfunction, McConnell's sign, mobile clot; not primarily diagnostic |
| Lower limb compression ultrasound | Detects DVT; positive result may guide treatment without CTPA |
Biomarkers:
- Troponin (I or T): elevated = RV myocyte injury → higher short-term mortality
- BNP/NT-proBNP: elevated = RV strain, adverse outcomes
- D-dimer: rule-out tool, not diagnostic
4. 🆕 2026 AHA/ACC PE Clinical Category System
The landmark 2026 guideline abolishes the old "massive/submassive/low-risk" terminology, replacing it with a five-tier A–E system (with subcategories) based on hemodynamics, clinical severity scores, biomarkers, and imaging:
| Category | Description | Key Criteria |
|---|---|---|
| A | Subclinical | Incidental, asymptomatic PE |
| B | Symptomatic – low severity | Low clinical severity score (PESI class I–II, sPESI=0, Hestia=0); no RV dysfunction, no elevated biomarkers |
| C | Symptomatic – elevated severity score | PESI class III–V, sPESI ≥1, Hestia ≥1; may include low-risk biomarker/imaging profiles |
| D | Incipient cardiopulmonary failure | Elevated risk score + positive troponin and RV dysfunction on imaging; hemodynamically stable but deteriorating |
| E | Overt cardiopulmonary failure | Hemodynamic instability (hypotension, shock, cardiac arrest) |
A respiratory modifier (R) can be added to any category to denote significant hypoxemia requiring supplemental oxygen.
This replaces the ESC 2019 "low/intermediate-low/intermediate-high/high" system previously widely used.
5. Management
Hemodynamic Resuscitation (Category D–E)
- Oxygen targeting SpO₂ >90%; avoid intubation if possible (↑ intrathoracic pressure → ↓ RV preload → hemodynamic collapse)
- Cautious IV fluids: 250–500 mL boluses (excessive fluids worsen RV distension and septal bowing into LV)
- Vasopressors: Norepinephrine first-line; dobutamine as adjunct (may worsen hypotension if used alone)
- ECMO: Bridge to thrombolysis or thromboembolectomy in refractory arrest
Anticoagulation
2026 AHA/ACC: DOACs are now the preferred first-line anticoagulant (Class I, Level B-R) — over vitamin K antagonists (warfarin), unless contraindicated.
| Agent | Regimen |
|---|---|
| Rivaroxaban | 15 mg BID × 21 days, then 20 mg daily |
| Apixaban | 10 mg BID × 7 days, then 5 mg BID |
| Edoxaban | Requires 5–10 days parenteral lead-in, then 60 mg daily |
| Dabigatran | Requires 5–10 days parenteral lead-in, then 150 mg BID |
| LMWH → Warfarin | Alternative; preferred in cancer, pregnancy (LMWH only), severe renal failure |
Duration:
- Provoked by transient reversible factor: 3 months
- Unprovoked or chronic risk: ≥3–6 months; consider indefinite anticoagulation based on bleeding vs. recurrence risk
Special populations:
- Pregnancy: DOACs are contraindicated (teratogenic); use LMWH throughout — Murray & Nadel, p. 3029
- Cancer-associated VTE: LMWH (enoxaparin) or DOACs (rivaroxaban, apixaban preferred for low bleeding-risk cancers) — systematic review support [PMID: 38065753]
Reperfusion Therapy (Category D–E)
Systemic thrombolysis:
- Alteplase 100 mg IV over 2 hours (or 0.6 mg/kg over 15 min in arrest)
- Indicated for high-risk PE (overt hemodynamic instability) without contraindications
- Contraindications: recent surgery/stroke, active bleeding
Catheter-directed thrombolysis (CDT):
- A 2023 network meta-analysis (44 studies, 20,006 patients) found CDT was associated with lower in-hospital death vs. systemic thrombolysis (OR 0.43) and lower ICH (OR 0.44) and major bleeding (OR 0.61) [PMID: 37336568]
- The 2026 guideline upgrades the recommendation for PE Response Teams (PERT) to Class I, Level B-NR for intermediate-high and high-risk PE — PERT should be activated for all Category C–E patients
- CDT is now considered a reasonable first-line option for appropriate candidates at PERT-capable centers
Surgical embolectomy:
- For massive PE when thrombolysis is contraindicated or has failed
- Also for clot-in-transit with impending hemodynamic compromise
Outpatient Management
Eligible patients (low-risk PE, PESI class I–II, sPESI=0, Hestia criteria negative) can be safely discharged on a DOAC:
- No RV dysfunction, no elevated troponin/BNP, hemodynamically stable, adequate support at home, no bleeding concerns
6. Risk Stratification Summary (2026 Framework)
| Category | Old Term | Treatment Approach |
|---|---|---|
| A (subclinical) | — | Individualized; DOAC if treating |
| B (low severity) | Low-risk | DOAC, consider outpatient discharge |
| C (elevated score) | Intermediate-low | Anticoagulation, inpatient vs. obs unit; activate PERT |
| D (incipient failure) | Intermediate-high | Anticoagulation + PERT; advanced therapy if deteriorating |
| E (overt failure) | Massive/high-risk | Heparin + thrombolysis/embolectomy/ECMO; ICU |
7. Post-PE Care
- Follow-up imaging at 3–6 months to assess clot resolution
- Monitor for chronic thromboembolic pulmonary hypertension (CTEPH) — occurs in ~3–5%; investigate with V/Q scan if persistent dyspnea
- Post-PE syndrome: persistent dyspnea, exercise intolerance, functional limitation — even without CTEPH
- Evaluate for underlying hypercoagulable state (thrombophilia workup) in unprovoked PE, especially in young patients
Key 2026 Guideline Highlights at a Glance
| Recommendation | Class / Level |
|---|---|
| DOACs over VKA for eligible patients | Class I / B-R |
| PERT activation for Category C–E | Class I / B-NR |
| CDT as alternative to systemic thrombolysis in intermediate-high/high-risk PE | Class IIa |
| Systemic thrombolysis for Category E (overt failure) | Class I |
| Outpatient treatment for Category B | Class I / B-NR |
| Age-adjusted D-dimer cutoff | Class I |
Sources:
- Rosen's Emergency Medicine, Chapter 74 (Pulmonary Embolism)
- Murray & Nadel's Textbook of Respiratory Medicine, Chapter on PE
- 2026 AHA/ACC Acute PE Guideline — Circulation (PMID: 41712677)
- Catheter-directed vs. systemic thrombolysis — CMAJ 2023 network meta-analysis (PMID: 37336568)
- 2025 ESVM Interventional VTE Guidelines (PMID: 40587333)
Can you simplify this and simplify abbreviations
Pulmonary Embolism (PE) — Simplified Overview
Latest guidelines (2026): The American Heart Association (AHA) and American College of Cardiology (ACC) published the first-ever dedicated PE guideline in February 2026. The biggest change: the old terms "massive," "submassive," and "low-risk" are gone, replaced by a clearer A–E category system.
What Is It?
A pulmonary embolism is a blood clot that travels to and blocks the arteries in the lungs. Most clots start as a deep vein thrombosis (DVT) — a clot in the leg veins — that breaks off and travels to the lungs.
It is life-threatening and causes roughly 1 in 4 sudden cardiac deaths.
Risk Factors
- Prolonged immobility (bed rest, long flights, surgery)
- Cancer
- Inherited clotting disorders (e.g., Factor V Leiden)
- Oral contraceptives or hormone therapy
- Pregnancy
- Previous DVT or PE
- Obesity, smoking
Symptoms
| Symptom | How Common |
|---|---|
| Shortness of breath | 75–80% of patients |
| Chest pain | ~67% |
| Leg swelling (one side) | <30% |
| Coughing up blood | ~13% |
| Fainting | <5% |
- A quarter of patients have no shortness of breath — so PE should never be ruled out on symptoms alone
- Fever from PE is usually mild; high fever (>38.6°C / 101.5°F) suggests infection instead
- In severe cases: collapse, cardiac arrest

Diagnosis
Step 1 — Estimate the likelihood (Pre-test probability)
Use a clinical scoring tool like the Wells Score to estimate how likely PE is before ordering tests. This prevents overtesting.
Step 2 — PERC Rule (can you skip testing entirely?)
If PE seems unlikely to the clinician, and the patient meets all 8 of these criteria, no testing is needed:
Age under 50 | Heart rate under 100 | Blood oxygen above 94% | No one-sided leg swelling | No coughing blood | No recent surgery or trauma | No previous clots | No hormone use
Step 3 — D-Dimer Blood Test
- Very sensitive (95–98%) but not specific — a negative result rules PE out; a positive result does not confirm it
- Age-adjusted cutoff: in patients over 50, use (age × 10) as the threshold instead of the standard 500 — this reduces unnecessary CT scans
- Only useful in lower-probability patients
Step 4 — Imaging
| Test | When Used |
|---|---|
| CT pulmonary angiography (CT scan of lung vessels) | Gold standard; first choice in most patients |
| V/Q scan (ventilation-perfusion scan) | Preferred in pregnancy, kidney problems, or contrast allergy |
| Echocardiogram (heart ultrasound) | Bedside test; shows if the right side of the heart is under strain — not used to confirm PE |
| Leg ultrasound | Detects DVT; if positive, may be enough to start treatment |
Biomarkers (blood tests showing heart strain)
- Troponin — elevated = heart muscle damage from clot → higher risk of dying
- BNP (brain natriuretic peptide) — elevated = right heart strain → worse prognosis
🆕 2026 New Severity Classification (A–E Categories)
The new guideline replaces old confusing terms with five clear categories:
| Category | What It Means | Old Equivalent |
|---|---|---|
| A | Clot found by accident — patient has no symptoms | — |
| B | Symptoms present, but low risk (low severity scores, no heart strain) | Low-risk |
| C | Symptoms present with elevated risk scores | Intermediate-low risk |
| D | Signs of early heart strain — heart is struggling but blood pressure still normal | Intermediate-high risk |
| E | Overt cardiovascular collapse — low blood pressure, shock, or cardiac arrest | Massive / high-risk |
A letter "R" can be added to any category if the patient also needs supplemental oxygen.
Treatment
1. Stabilize the Patient (Category D–E)
- Supplemental oxygen to keep blood oxygen above 90%
- Avoid mechanical ventilation if possible — putting a patient on a ventilator increases chest pressure, reduces blood returning to the heart, and can worsen collapse
- IV fluids: small amounts only (250–500 mL at a time) — too much fluid over-stretches the right heart
- Vasopressors (medications to raise blood pressure): norepinephrine is first choice; dobutamine can be added but not used alone
- ECMO (heart-lung bypass machine): used as a bridge in patients in cardiac arrest while preparing for clot removal
2. Blood Thinners (Anticoagulation) — the cornerstone of treatment
2026 guideline: Direct oral anticoagulants (DOACs) are now the #1 recommended treatment — preferred over warfarin because they are safer, easier to use, and cause less major bleeding.
| Drug | Dosing Schedule |
|---|---|
| Rivaroxaban (Xarelto) | 15 mg twice daily × 3 weeks, then 20 mg once daily |
| Apixaban (Eliquis) | 10 mg twice daily × 1 week, then 5 mg twice daily |
| Edoxaban (Savaysa) | Needs 5–10 days of injectable blood thinner first, then 60 mg once daily |
| Dabigatran (Pradaxa) | Needs 5–10 days of injectable blood thinner first, then 150 mg twice daily |
| Warfarin | Second choice; still used if DOACs are contraindicated |
| Low molecular weight heparin (injection) | Preferred in cancer, and the only safe option in pregnancy |
How long to treat?
- Clot caused by a temporary trigger (surgery, travel): 3 months
- Unprovoked clot or ongoing risk: at least 6 months, often lifelong
3. Clot-Busting Drugs (Thrombolysis)
Used when the patient's life is immediately at risk (Category E):
- Systemic thrombolysis: alteplase (clot-dissolving drug) given into a vein — fast but higher bleeding risk
- Catheter-directed thrombolysis (CDT): a thin tube is guided directly to the clot in the lung, delivering a lower dose of drug — lower bleeding risk, lower death rate than systemic thrombolysis in recent large studies (2023 meta-analysis, 20,006 patients)
4. Surgery (Surgical Embolectomy)
- Physical removal of the clot during open-heart surgery
- Reserved for when clot-busting drugs are contraindicated or have failed
5. PE Response Team (PERT)
- A rapid multidisciplinary team (emergency, cardiology, pulmonology, hematology, vascular) that convenes for complex PE cases
- 2026 guideline upgrades PERT activation to a top-level (Class I) recommendation for all Category C–E patients
Treatment Decision by Category
| Category | Where to Treat | Main Treatment |
|---|---|---|
| A (incidental) | Outpatient possible | Anticoagulation, individualized |
| B (low risk) | Often discharged home | DOAC, outpatient |
| C (elevated score) | Hospital ward or observation | DOAC, activate PERT |
| D (early strain) | Monitored hospital bed | Heparin + PERT; consider CDT if worsening |
| E (collapse/shock) | ICU | Heparin → thrombolysis or surgery; ECMO if needed |
After Treatment (Long-Term)
- Follow-up scan at 3–6 months to check clot resolution
- Watch for chronic thromboembolic pulmonary hypertension (CTEPH) — clot scars that permanently raise lung pressures (~3–5% of patients); diagnosed with a V/Q scan if breathlessness persists
- Post-PE syndrome: some patients have ongoing fatigue and breathlessness even after the clot is gone
- Consider testing for inherited clotting disorders in young patients or those with unprovoked clots
Sources:
- Rosen's Emergency Medicine, Chapter 74
- Murray & Nadel's Textbook of Respiratory Medicine
- 2026 AHA/ACC PE Guideline — Circulation [PMID: 41712677]
- Catheter-directed vs. systemic thrombolysis — CMAJ 2023 meta-analysis [PMID: 37336568]
This is a shared conversation. Sign in to Orris to start your own chat.