45 year female with swelling on face and hand and feet’s intermittent episodes decease by it self non pitting swelling normal kFT normal thyroid function negative Anti ccp
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Searching PubMed
hereditary angioedema diagnosis management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
I now have comprehensive information to provide a thorough clinical answer.
Clinical Assessment: 45-Year-Old Female with Intermittent Non-Pitting Swelling of Face, Hands, and Feet
Key Features Driving the Differential:
- Non-pitting (not dependent) edema
- Episodic/intermittent — resolves spontaneously
- Face + acral (hands/feet) distribution
- Normal KFT → renal cause excluded
- Normal thyroid → myxedema excluded
- Negative Anti-CCP → Rheumatoid arthritis excluded
Most Likely Diagnosis: Angioedema (Bradykinin-mediated)
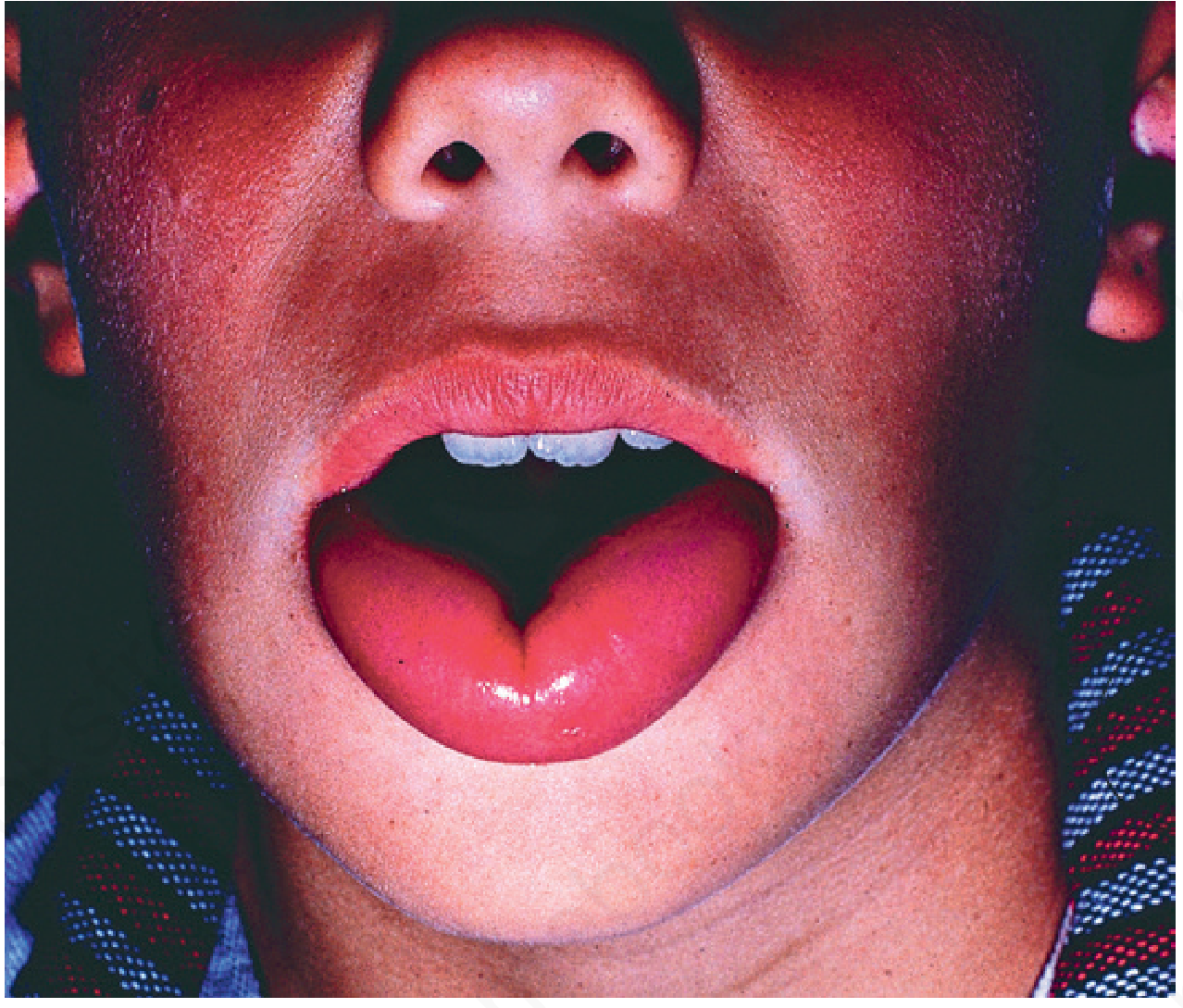
Angioedema is an acute, evanescent, circumscribed edema affecting distensible tissues — eyelids, lips, earlobes, and genitalia — occurring in the deep dermis or subcutaneous tissues. The swelling is only slightly tender, with overlying skin unaltered. Diffuse swelling on the hands, feet, and ankles is characteristic. — Andrews' Diseases of the Skin, p. 179
Differential Diagnosis
| Condition | Favors | Against |
|---|---|---|
| Hereditary Angioedema (HAE) | Non-pitting, episodic, self-resolving, face/extremities, no urticaria | Usually onset <20 yrs; BUT Type III predominates in women |
| Acquired Angioedema (AAE) | Onset after 4th decade, no family history | Need low C1q |
| ACE inhibitor-induced | Bradykinin-mediated, face/tongue | Ask about ACEI use |
| Idiopathic Histaminergic Angioedema | Responds to antihistamines | Typically urticaria co-exists |
| Chronic Spontaneous Urticaria with angioedema | Common in women | Usually pruritic |
This patient is 45 years old with onset likely in adulthood — this raises the important distinction between HAE Type III (normal C1-EI, predominantly females) and Acquired Angioedema (onset >40 yrs, associated with lymphoproliferative disease).
HAE Classification (Critical for Workup)
| Type | C4 | C1-EI Antigen | C1-EI Function | C1q | Notes |
|---|---|---|---|---|---|
| Type I | ↓ | ↓ | ↓ | Normal | Most common (85%) |
| Type II | ↓ | Normal/↑ | ↓ | Normal | Dysfunctional protein |
| Type III | Normal | Normal | Normal | Normal | Women predominant; FXII mutation |
| Acquired | ↓ | ↓ | ↓ | ↓ | Onset >40, lymphoma |
— Andrews' Diseases of the Skin, p. 180; Goldman-Cecil Medicine, p. 2694
Recommended Workup
First-Line (Screen for Types I & II)
- Serum C4 level — best screening test; persistently low even between attacks
- C1 esterase inhibitor antigen level
- C1 esterase inhibitor functional assay
- C1q level — low only in acquired angioedema (not HAE)
If all above normal (suspect Type III or idiopathic)
- FXII gene mutation (Factor XII — associated with estrogen-dependent HAE Type III)
- Tryptase level — rule out systemic mastocytosis
- ANA, anti-dsDNA — rule out lupus-associated angioedema
- Serum immunoglobulins + SPEP — exclude plasma cell dyscrasia
- CBC + LDH — screen for lymphoproliferative disease (especially if C1q is low)
- Ask about ACE inhibitor use — even past use; this is a common trigger
Also Ask:
- Family history of angioedema (HAE is autosomal dominant)
- Trigger factors: trauma, stress, infections, hormonal changes, dental procedures
- History of abdominal pain episodes (GI angioedema mimics appendicitis)
- Any laryngeal/throat tightness (life-threatening feature)
- Oral contraceptive use (estrogens precipitate HAE attacks)
Why Not Urticaria?
"The second subgroup, angioedema associated with C1 esterase inhibitor deficiency, or that related to ACE inhibitors, is not associated with hives or pruritus. Symptoms of pain predominate, and this is mediated by bradykinin." — Andrews' Diseases of the Skin, p. 179
The absence of pruritus/urticaria in this patient strongly points to bradykinin-mediated rather than histamine-mediated angioedema.
Acquired Angioedema — Important Consideration at Age 45
"Some patients present with symptoms indistinguishable from HAE, but with onset after the fourth decade of life and lacking a family history... Acquired angioedema I is associated with lymphoproliferative disease including B-cell lymphoma, CLL, monoclonal gammopathy." — Andrews' Diseases of the Skin, p. 180
Since this patient is 45 and has no stated family history — acquired angioedema must be ruled out, requiring:
- C1q level
- Serum immunoglobulins / SPEP
- CBC with differential
Management
Acute Attack Treatment
| Agent | Mechanism | Dose |
|---|---|---|
| Icatibant (Firazyr) | Bradykinin-2 receptor antagonist | 30 mg SC |
| Ecallantide (Kalbitor) | Kallikrein inhibitor | 30 mg SC |
| C1 esterase inhibitor concentrate (Berinert) | Replacement therapy | 20 U/kg IV |
| Fresh frozen plasma | If above unavailable | 2 units IV |
⚠️ Antihistamines, epinephrine, and corticosteroids have minimal benefit in bradykinin-mediated angioedema.
Long-term Prophylaxis
- Lanadelumab (anti-kallikrein monoclonal antibody) 300 mg SC every 2–4 weeks
- Berotralstat (oral kallikrein inhibitor) 150 mg daily
- SC C1 esterase inhibitor (60 IU/kg twice weekly)
- Danazol 50–200 mg twice daily (attenuated androgen; second-line; avoid in pregnancy)
Avoid
- ACE inhibitors (precipitate/worsen attacks)
- Estrogens / oral contraceptives (precipitate attacks)
— Goldman-Cecil Medicine, p. 2694; Tintinalli's Emergency Medicine, p. 113
Airway Warning
Laryngeal edema is the main cause of mortality in HAE. If this patient ever reports throat tightness, voice change, or difficulty breathing, this is a medical emergency requiring immediate treatment and airway management (intubation/tracheostomy readiness).
Summary Recommendation
| Step | Action |
|---|---|
| 1 | Order C4, C1-EI antigen, C1-EI function, C1q |
| 2 | Ask full drug history (ACEI?), family history |
| 3 | If C4 low → confirm HAE Type I or II |
| 4 | If C4 normal → suspect HAE Type III, ACE inhibitor-induced, or idiopathic |
| 5 | If C1q low → workup for acquired angioedema (CBC, SPEP, LDH) |
| 6 | Prescribe icatibant for on-demand acute use |
| 7 | Counsel on triggers and airway risk |
Recent Evidence: A 2024 systematic review (PMID: 39666085) confirms efficacy and safety of donidalorsen (a new oral plasma kallikrein inhibitor) for HAE with C1 inhibitor deficiency — a promising emerging option for long-term prophylaxis.
This is a shared conversation. Sign in to Orris to start your own chat.