Atrophic rhinitis
Reading File
Finding Sources
Finding Sources
Searching PubMed
atrophic rhinitis
Reading File
Reading File
Searching Images
atrophic rhinitis nasal mucosa ozena
Loading Image
Here is a comprehensive overview of atrophic rhinitis.
Atrophic Rhinitis
Definition
Atrophic rhinitis is a chronic condition characterized by progressive atrophy of the nasal mucosa, submucosal glands, turbinate bones, and nasal nerves, resulting in a paradoxically widened but functionally impaired nasal cavity. It is also known as rhinitis sicca or, in its severe primary form with foul-smelling discharge, ozena (from the Greek word for stench). — K.J. Lee's Essential Otolaryngology, p. 579; Cummings Otolaryngology Head and Neck Surgery
Classification
Primary Atrophic Rhinitis
- Most prevalent in developing countries in subtropical and temperate climate zones
- Etiology is incompletely understood, but bacterial colonization is strongly implicated
- Causative organisms: Klebsiella ozaenae, Staphylococcus aureus, Proteus mirabilis, Escherichia coli
- More severe and progressive course
Secondary Atrophic Rhinitis
- More prevalent in developed countries; less severe and less progressive
- Caused by identifiable precipitants:
- Iatrogenic: excessive turbinate resection (→ Empty Nose Syndrome), sinonasal surgery
- Trauma
- Radiation therapy
- Granulomatous diseases (e.g., granulomatosis with polyangiitis, sarcoidosis, leprosy)
- Rhinitis medicamentosa (prolonged use of topical decongestants)
Pathology / Histology
The hallmark histological findings are:
- Squamous metaplasia of the respiratory epithelium
- Glandular atrophy — loss of seromucinous glands
- Diffuse endarteritis obliterans — progressive vascular occlusion reducing mucosal blood flow
- Loss of mucociliary function
- Atrophy and fibrosis of nasal mucosa, submucosa, turbinate bone, and nerves
— K.J. Lee's Essential Otolaryngology, p. 579
Clinical Features
| Feature | Detail |
|---|---|
| Nasal obstruction/congestion | Paradoxical — cavity is wide but patient feels blocked |
| Crusting | Yellow-green, thick, extensive crusts |
| Fetor (ozena) | Foul odor from crusts; characteristic of primary form |
| Anosmia | Loss of smell, partly due to mucosal destruction |
| Nasal dryness | From loss of glandular secretions |
| Wide nasal cavity | Visible on endoscopy/imaging |
| Epistaxis | From friable mucosa |
Endoscopic Appearance
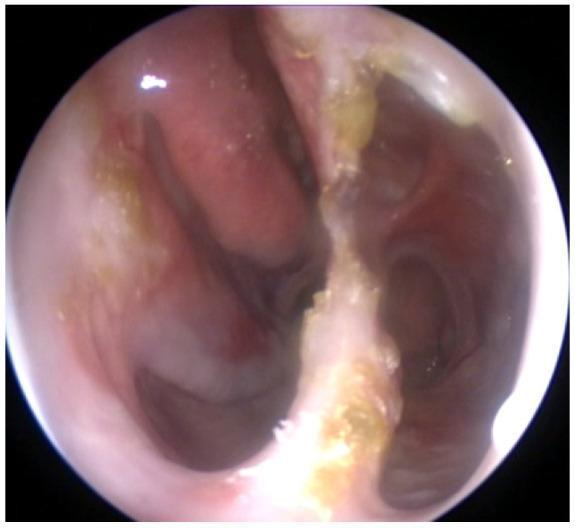
The image below shows an endoscopic view of nasal atrophy: atrophic, thin, pale mucosa with near-absent turbinates, yellow-gold crusting adherent to the septum and posterior nasal cavity, and a widened nasal space — findings characteristic of advanced secondary atrophic rhinitis (in this case from granulomatous disease with septal perforation):
Diagnosis
Diagnosis is primarily clinical:
- History and examination findings (wide nasal cavity, crusting, fetor, anosmia)
- Nasal endoscopy showing atrophic mucosa and turbinate reduction
- Culture of nasal secretions (may identify K. ozaenae)
- CT sinuses: widened nasal cavity, turbinate atrophy, mucosal thickening
Management
Medical (first-line)
| Treatment | Purpose |
|---|---|
| Nasal saline irrigation | Softens and removes crusts; cornerstone of therapy |
| Nasal lubricants/emollients | Reduce mucosal dryness |
| Antibiotics | Target causative organisms (e.g., ciprofloxacin for K. ozaenae, rifampicin, streptomycin in some regimens) |
| Estrogen nasal drops | Historically used to promote mucosal vascularization |
| Glucose in glycerin drops | Inhibit proteolytic bacteria |
Surgical (for refractory cases)
- Nasal cavity narrowing procedures — reduce the dead space to improve air humidification and prevent crust formation
- Submucosal injection of Teflon, fat, or cartilage
- Young's operation: surgical closure of one or both nostrils (allows mucosal recovery)
- Modified Young's procedure (partial closure)
- Autologous fat/platelet-rich plasma (PRP) injection — emerging regenerative approach (see PubMed below)
— K.J. Lee's Essential Otolaryngology, p. 579; Cummings Otolaryngology
Atrophic Rhinitis vs. Empty Nose Syndrome
These are distinct entities:
- Atrophic rhinitis: mucosal and glandular atrophy ± infection; can be primary or secondary
- Empty nose syndrome (ENS): paradoxical nasal obstruction specifically attributed to excessive turbinate removal surgically; may represent the most severe form of iatrogenic secondary atrophic rhinitis but is classified separately
— K.J. Lee's Essential Otolaryngology, p. 579
Recent Evidence (PubMed, 2023–2026)
- A 2025 systematic review (PMID: 40820344) examined platelet-rich plasma (PRP) injection in atrophic rhinitis, reflecting growing interest in regenerative approaches.
- Two 2025 systematic reviews (PMIDs: 39126290, 40617870) addressed Empty Nose Syndrome management and its psychological burden (depression/anxiety), relevant to the iatrogenic secondary subtype.
No high-level evidence currently contradicts the standard management approach; saline irrigation and surgical cavity reduction remain the mainstay.
Summary: Atrophic rhinitis is a chronic, progressive nasal condition causing mucosal and turbinate atrophy, paradoxical nasal obstruction, fetor, and crusting. Primary disease is driven by bacterial infection (especially K. ozaenae) in tropical regions; secondary disease follows surgery, radiation, or granulomatous processes. Management centers on saline irrigation, antibiotics for bacterial forms, and surgical cavity narrowing in refractory cases. — Cummings Otolaryngology; K.J. Lee's Essential Otolaryngology
This is a shared conversation. Sign in to Orris to start your own chat.