Dengu Fever PFL
Reading File
Finding Sources
Finding Sources
Searching PubMed
"dengue fever"[MeSH Terms] AND management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive content from multiple authoritative sources. Let me compile the full Problem Feature List (PFL) for Dengue Fever.
Dengue Fever — Problem Feature List (PFL)
1. Definition
Dengue fever is an acute febrile illness caused by dengue virus (DENV), a flavivirus transmitted primarily by Aedes aegypti (and less commonly Aedes albopictus and Aedes polynesiensis) mosquitoes. Four antigenically distinct serotypes exist: DENV-1, DENV-2, DENV-3, DENV-4. — Jawetz Medical Microbiology 28E; Red Book 2021
2. Epidemiology
| Feature | Detail |
|---|---|
| Global burden | ~400 million infections/year; ~100 million symptomatic; ~40,000 deaths from severe dengue |
| Distribution | Endemic in >100 countries; Southeast Asia, Western Pacific, Central/South America, India, Cuba |
| Vector | Day-biting Aedes aegypti mosquito; adapts to urban peridomestic environments |
| Transmission | Human → mosquito → human (no direct human-to-human); rare vertical, blood transfusion, organ transplant, breastfeeding routes |
| Risk factors | Tropical regions (>20°C), uncontrolled urbanization, lack of sanitation, crowding, water storage |
| Secondary infection risk | Prior infection with one serotype → cross-protection lasts 1–3 years, then reinfection with different serotype → severe disease |
— Robbins Pathology 2024; Andrews' Diseases of the Skin; Harrison's 22E
3. Pathogenesis
| Mechanism | Detail |
|---|---|
| Antibody-dependent enhancement (ADE) | Key mechanism of severe dengue: subneutralizing cross-reactive antibodies from a prior infection enhance DENV entry into macrophages via Fc receptors → amplified viral replication → cytokine storm |
| Cytokine cascade | Release of vasoactive mediators, procoagulants, IL, TNF-α, ET-1 → increased vascular permeability |
| Plasma leakage | Endothelial injury → extravasation into interstitial spaces (pleural effusion, ascites, hemoconcentration) |
| Thrombocytopenia | Bone marrow suppression + platelet destruction + consumptive coagulopathy |
| DHF serotype predilection | DENV-2 reinfection most likely to cause severe disease |
— Robbins Pathology 2024; Jawetz 28E; Comprehensive Clinical Nephrology 7E
4. Clinical Classification (WHO 2009)
Group A — Dengue Without Warning Signs
- Fever + ≥2 of: nausea/vomiting, rash, aches/pains (myalgia, arthralgia, retro-orbital pain, headache), leukopenia, positive tourniquet test
Group B — Dengue With Warning Signs
Any of the following during or after defervescence:
- Abdominal pain or tenderness
- Persistent vomiting
- Clinical fluid accumulation (ascites, pleural effusion)
- Mucosal bleeding
- Lethargy or restlessness
- Liver enlargement >2 cm
- Rapid decline in platelet count + rising hematocrit
Group C — Severe Dengue (previously DHF/DSS)
At least one of:
- Severe plasma leakage → shock (DSS) or fluid accumulation with respiratory distress
- Severe bleeding
- Severe organ involvement: AST/ALT ≥1000 IU/L, impaired consciousness, heart/organ failure
— Red Book 2021; Rosen's Emergency Medicine
5. Clinical Phases
| Phase | Timing | Features |
|---|---|---|
| Febrile phase | Days 1–3 (up to 7) | Abrupt high fever, severe myalgia/arthralgia (breakbone fever), headache, retro-orbital pain, facial flushing, injected oropharynx, macular/morbilliform rash, leukopenia, petechiae |
| Critical phase | Days 3–7 | Defervescence; ↑ vascular permeability → plasma leakage; hemoconcentration; thrombocytopenia nadir; warning signs appear; duration ~24–48 hrs |
| Recovery/Convalescent phase | Days 7–10 | Hemodynamic stabilization, reabsorption of leaked fluids, risk of fluid overload, bradycardia, fine convalescent rash |
6. Symptoms & Signs
Constitutional
- Abrupt onset high fever (38–40°C); may follow "saddleback" biphasic pattern (fever defervesces ~day 3, returns days 5–8)
- Severe myalgia, arthralgia, deep bone pain ("breakbone fever")
- Retro-orbital pain (characteristic)
- Headache, anorexia, nausea, vomiting
- Facial flushing, facial erythema
Skin (Andrews' Diseases of the Skin)
- ~50% develop rash; eruption most commonly begins days 3–5 as fever defervesces
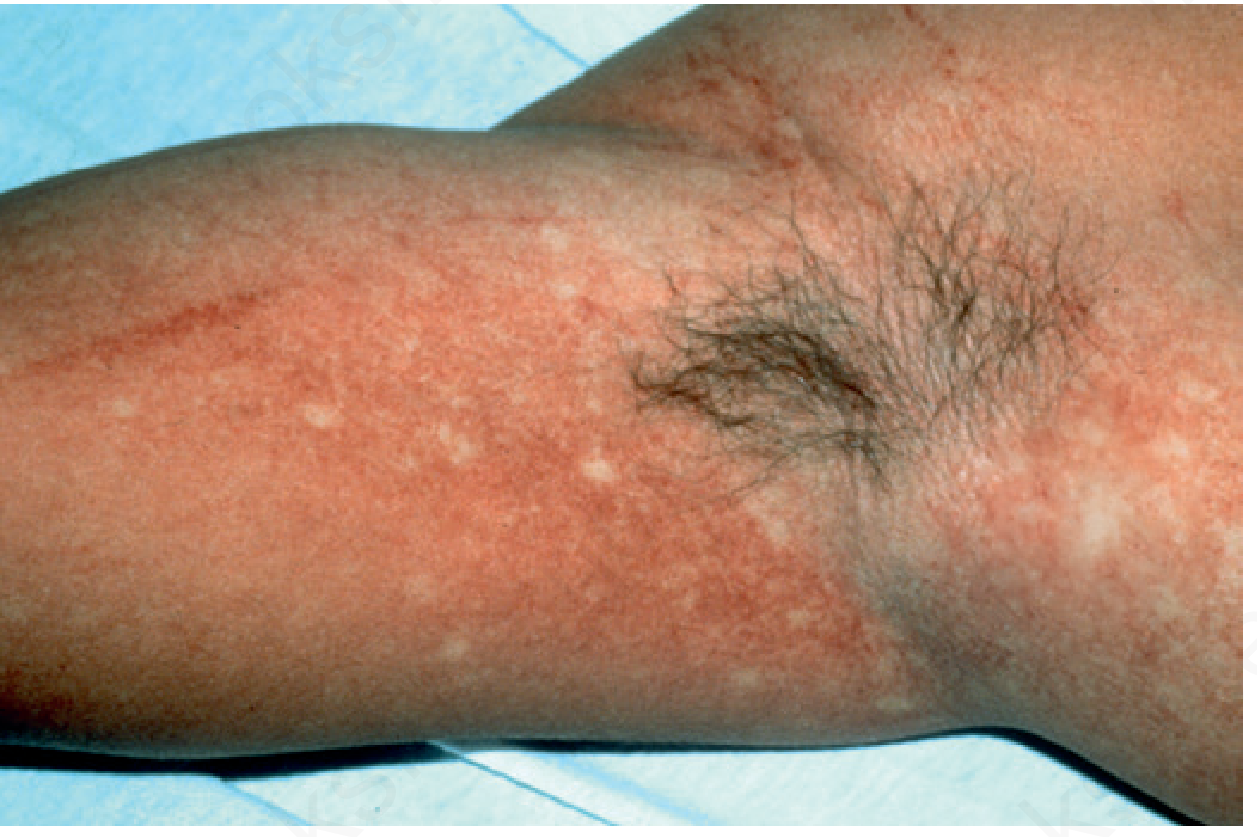
- Macular or morbilliform rash, typically generalized; characteristic "islands of white in a sea of red" — confluent erythema sparing small islands of normal skin
- Distribution: generalized (50%), extremities only (30%), trunk (20%)
- Asymptomatic or mildly pruritic
- Petechiae present; linear petechiae after BP cuff application (Fig. 19.42)
- Tourniquet test (Hess test): BP cuff inflated 5 min → ≥10 petechiae/square inch = positive (suggests dengue)
Hemorrhagic Features (Severe Dengue)
- Epistaxis, purpura, petechiae, ecchymosis
- Gingival bleeding, mucosal hemorrhage
- Pleural effusions, ascites
- Marked thrombocytopenia
Less Common Manifestations
- Myocarditis, pancreatitis, hepatitis
- Hemophagocytic lymphohistiocytosis (HLH)
- Neurologic: acute meningoencephalitis, post-dengue ADEM
- AKI (1–30% of cases): via endothelial injury, rhabdomyolysis, hemolysis (especially in G6PD deficiency), acute tubular necrosis, glomerulonephritis with immune complex deposition
7. Laboratory Findings
| Test | Finding |
|---|---|
| CBC | Leukopenia (characteristic); thrombocytopenia (platelets <100,000 in 50%); elevated hematocrit (hemoconcentration in DHF) |
| LFTs | Elevated AST/ALT (avg ~3× normal); severe dengue: AST/ALT ≥1000 IU/L |
| Coagulation | Prolonged PT/PTT in DHF (DIC picture) |
| Urinalysis | Proteinuria (sometimes nephrotic range), hematuria in AKI |
8. Diagnosis
| Method | Timing | Notes |
|---|---|---|
| NS1 antigen test | Days 1–5 (febrile phase) | Detects viral nonstructural protein 1; rapid bedside test |
| RT-PCR | Days 1–5 | Rapid identification + serotyping; most sensitive early |
| IgM ELISA | From day 5–6 | Often negative early; confirmatory by day 6 |
| IgG ELISA | From day 7 | Useful for secondary infection (elevated IgG even early) |
| Paired serology | Acute + convalescent (2–3 weeks apart) | 4× rise in titer = definitive confirmation |
| Virus isolation | Difficult; mosquito cell line inoculation + nucleic acid assay | Research/reference labs |
⚠️ Cross-reactivity of IgG with other flaviviruses (Zika, yellow fever, West Nile) complicates serology.
9. Differential Diagnosis
| Condition | Distinguishing Feature |
|---|---|
| Malaria | Must exclude first; has periodicity, splenomegaly, parasitemia on smear |
| Chikungunya | Similar rash + fever, but more persistent arthritis |
| Zika | Milder, teratogenic; similar vector |
| Influenza | No rash, no tourniquet positivity |
| Measles | Koplik spots, prodromal cough/coryza/conjunctivitis |
| Rubella | Lymphadenopathy + rash, milder |
| West Nile fever | Lymphadenopathy (absent in dengue) |
| Leptospirosis | Weil's disease; conjunctival suffusion, jaundice, renal failure |
| Rickettsial infections | Eschar, respond to doxycycline |
| Meningococcemia | Petechial rash indistinguishable; check CSF if meningism |
10. Management
Dengue Without Warning Signs (Group A)
- Outpatient management
- Rest, oral fluids, antipyretics
- Acetaminophen (paracetamol) ONLY for pain/fever
- ⛔ NSAIDs and aspirin are contraindicated — worsen bleeding tendency
- Monitor for warning signs; return precautions
Dengue With Warning Signs (Group B)
- Hospital admission for monitoring
- IV fluid replacement (isotonic crystalloid)
- Serial CBC, hematocrit, vital signs
- Watch for clinical deterioration during critical phase (days 3–7)
Severe Dengue (Group C — DHF/DSS)
- ICU admission
- Aggressive IV fluid resuscitation (guided by hematocrit/clinical response)
- Blood product transfusions for hemorrhagic sequelae (packed RBCs, platelets, FFP as indicated)
- Organ support as indicated
- ⚠️ Corticosteroids: evaluated in low-quality studies — evidence inconclusive; not currently recommended
- No specific antiviral agents approved
— Rosen's Emergency Medicine; Tintinalli's Emergency Medicine; Red Book 2021
11. Complications
| Complication | Notes |
|---|---|
| Dengue Shock Syndrome (DSS) | DHF + circulatory collapse; mortality >10% if untreated |
| Dengue Hemorrhagic Fever (DHF) | Plasma leakage, hemorrhage, thrombocytopenia, fever 2–7 days |
| Acute Kidney Injury | 1–30% incidence; via endothelial injury, rhabdomyolysis, hemolysis (G6PD), ATN, GN |
| Hepatic failure | ALT/AST >1000 IU/L; rare fulminant hepatitis |
| Neurologic | Encephalitis, ADEM |
| Myocarditis | Rare |
| Fluid overload | Risk during recovery phase from IV fluid given during critical phase |
12. Immunity & Vaccine
| Concept | Detail |
|---|---|
| Serotype-specific immunity | Lifelong protection against the infecting serotype; cross-protection against other serotypes lasts 1–3 years only |
| Secondary infection risk | Reinfection with a different serotype → ADE → higher risk of severe dengue |
| Vaccines | Available (e.g., Dengvaxia/CYD-TDV) — only recommended for seropositive individuals (prior dengue exposure); vaccinating seronegatives risks ADE and more severe disease upon natural infection |
13. Prevention
- Vector control: eliminate standing water breeding sites (peridomestic water storage)
- Mosquito nets, repellents (DEET), protective clothing
- Aedes biting peak: daytime (dawn and dusk)
- Novel biocontrol: Wolbachia-infected mosquitoes reduce dengue transmission by 95–97% (Colombia trial) — Robbins Pathology 2024
- Screen travelers returning from endemic regions presenting with fever within 2 weeks
Key Sources: Harrison's Principles of Internal Medicine 22E (2025) | Tintinalli's Emergency Medicine | Rosen's Emergency Medicine | Jawetz Medical Microbiology 28E | Robbins & Cotran Pathologic Basis of Disease | Andrews' Diseases of the Skin | Red Book 2021 | Comprehensive Clinical Nephrology 7E
This is a shared conversation. Sign in to Orris to start your own chat.