Stitch radiography in detail add every point you know search various research papers , books , articles and give me notes on it in detail , like definition, principle, history, techniques , process , components etc u want to add , and also give me diagram to add in my notes
Checking Date & Time
Reading File
Finding Sources
Searching PubMed
stitch radiography full-length lower limb imaging
Searching the Web
stitch radiography definition principle technique components detailed
Finding Sources
Reading Article
Searching PubMed
panoramic radiography long cassette whole leg alignment
Finding Sources
Searching PubMed
image stitching digital radiography lower extremity alignment
Searching Images
stitch radiography full length lower limb x-ray
Finding Sources
Searching PubMed
full length lower limb radiograph mechanical axis HKA angle measurement
Loading Image
Finding Sources
Reading Article
Loading Image
Reading File
Reading File
Searching Images
stitch radiography technique multiple exposures panoramic digital radiograph stitching process
Loading Image
Loading Image
Finding Sources
Loading Image
Loading Image
📋 STITCH RADIOGRAPHY — Comprehensive Notes
1. DEFINITION
Stitch radiography (also called full-length radiography, long-leg radiography, whole-leg radiography, panoramic radiography of the extremities, or scanography) is a specialized radiographic imaging technique in which multiple overlapping X-ray exposures are taken sequentially along the length of a body region (most commonly the entire lower limb or the full spine), and then digitally or manually joined (stitched) together into a single, seamless, full-length composite image.
The term "stitching" refers to the post-processing step of merging these individual image frames into one continuous panoramic radiograph that cannot be obtained in a single standard X-ray exposure because of the size limitations of digital radiography (DR) detectors.
"Full-length lower limb x-rays are used to diagnose and plan surgical procedures such as Total Knee Arthroplasty (TKA) and High Tibial Osteotomy (HTO). Due to the size limitation of digital radiography, panoramic x-ray images cannot be obtained in a single exposure, necessitating multiple exposures and image stitching." — Alkhatatbeh et al., Frontiers in Surgery, 2022 [PMID: 36311950]
2. SYNONYMS & RELATED TERMS
| Term | Context |
|---|---|
| Full-length radiograph | General clinical usage |
| Long-leg radiograph | Lower limb orthopaedics |
| Scanogram / Orthoroentgenogram | Limb-length measurement |
| Teleroentgenogram | Historical film-based term |
| Goniometry (radiographic) | Lower limb axis assessment |
| EOS imaging | Modern low-dose biplanar stitched system |
| Panoramic radiography | Spine and extremity variants |
3. HISTORY & EVOLUTION
3.1 Film Era (Pre-digital)
- Early 20th century: Initial attempts using long cassettes (≥ 91 cm) placed along the full length of the limb, with a single exposure from a distant focus. Called teleroentgenography (tele = distant, to reduce magnification).
- Clinicians used 14 × 17 inch (35 × 43 cm) film cassettes butted end-to-end. The resulting films were physically overlapped and taped together.
- Scanography emerged as a technique where the X-ray tube moved along a slit-collimated beam past a stationary long cassette — reducing parallax and geometric distortion.
- Problems: parallax error, patient movement between exposures, magnification differences, and physical film misalignment at the stitching line.
3.2 Computed Radiography (CR) Era (1980s–2000s)
- Phosphor imaging plates replaced film but remained physically limited in size (~35 × 43 cm max).
- Manual stitching was performed in dedicated PACS/workstation software by overlapping landmark structures (e.g., joint outlines).
- Introduction of dedicated long-cassette CR systems (e.g., 35 × 91 cm plates) partially reduced the need for stitching.
3.3 Digital Radiography (DR) / Flat-Panel Detector Era (2000s–present)
- Flat-panel detectors (FPDs) are typically 43 × 43 cm (17 × 17 inch) — too short for full lower limb coverage.
- Software-based automated stitching algorithms were developed, using feature-detection methods to merge multiple overlapping images.
- EOS® system (EOS Imaging, France) introduced simultaneous biplanar (AP + lateral) full-body imaging in a single upright pass using slot-scanning technology — the gold standard by the 2010s.
- 2022: Canny-edge-detection-based automated stitching using bone edge detection + Wavelet fusion achieved 100% accuracy and 3-second stitching time (Alkhatatbeh et al., 2022).
4. PRINCIPLE
4.1 Fundamental Radiographic Principle
Stitch radiography is grounded in the basic principle of X-ray attenuation: X-ray photons pass through body tissues and are attenuated differentially according to tissue density (bone > muscle > fat > air), producing a projection image on a receptor.
4.2 The Stitching Principle
Since a standard DR detector cannot capture the entire length of the lower limb (avg. 80–100 cm) in one frame:
- Multiple overlapping exposures are made — each capturing a segment of the limb (e.g., hip-to-knee frame, knee-to-ankle frame).
- Each frame is acquired sequentially — the X-ray tube/detector shifts along the limb axis between exposures.
- The individual images are aligned using common anatomical landmarks present in the overlapping region (e.g., tibial plateau, femoral condyles) as registration points.
- The aligned images are blended (alpha blending, wavelet fusion, or feathering) to eliminate visible seam artifacts at the junction.
- The resulting composite image simulates what a single large-format exposure would have produced.
4.3 Weight-Bearing Principle
Full-length radiographs are performed in the standing (weight-bearing) position so that:
- Physiological joint loading is reproduced.
- True mechanical axis deviation (varus/valgus) is visible under load.
- Soft tissue compression across joints mimics functional anatomy.
- Non-weight-bearing images underestimate deformity severity.
5. INDICATIONS (CLINICAL USES)
Lower Limb
| Indication | Purpose |
|---|---|
| Osteoarthritis assessment | Evaluate joint space narrowing, varus/valgus |
| Pre-operative planning for Total Knee Arthroplasty (TKA) | Measure HKA angle, plan implant alignment |
| High Tibial Osteotomy (HTO) planning | Determine angle of correction, osteotomy site |
| Distal Femoral Osteotomy | Valgus correction planning |
| Limb Length Discrepancy (LLD) | Measure true leg length differences |
| Paediatric deformity (genu varum/valgum) | Follow physiological correction with age |
| Post-operative TKA/THA follow-up | Assess restoration of neutral axis |
| Limb-salvage oncology | Monitor expandable prosthesis, LLD |
| Fracture planning | Long bone deformity/malunion assessment |
Spine
| Indication | Purpose |
|---|---|
| Scoliosis (adolescent/adult) | Cobb angle measurement, curve classification |
| Sagittal balance assessment | Measure SVA, PI, LL, TK |
| Spinal fusion pre/post-op | Full instrumentation view |
| Degenerative spinal deformity | Global alignment measurement |
Upper Limb (less common)
- Full-length humerus/forearm in specific deformity/fracture contexts.
6. ANATOMY ASSESSED ON STITCH RADIOGRAPHY (LOWER LIMB)
A standard full-length lower limb stitch radiograph covers:
- Pelvis (both hip joints, femoral heads)
- Femoral shafts (bilateral)
- Knee joints (distal femur, proximal tibia, fibula head)
- Tibial and fibular shafts
- Ankle joints
- Optionally: foot
7. KEY MEASUREMENTS & ANGLES
7.1 Hip-Knee-Ankle (HKA) Angle
- A line drawn from the centre of the femoral head to the centre of the ankle (specifically the centre of the talus).
- The mechanical axis of the lower limb.
- Normal: 0° ± 3° (slight valgus in females is physiological).
- Varus = HKA < 0° (medial deviation)
- Valgus = HKA > 0° (lateral deviation)
- Gold-standard measurement from standing full-length radiograph.
7.2 Mechanical Axis Deviation (MAD)
- Horizontal distance (mm) between the mechanical axis line and the centre of the knee joint.
- Normal: passes 8–10 mm medial to the knee centre (within medial compartment).
7.3 Weight-Bearing Line Ratio (WBL)
- Position of the mechanical axis on the tibial plateau expressed as a percentage of plateau width.
- Normal: ~43–50% (near centre).
- Used for HTO correction planning; target point = 62.5% for lateral shift in varus correction.
7.4 Joint Line Convergence Angle (JLCA)
- Angle between the distal femoral joint line and proximal tibial joint line.
- Reflects medial/lateral soft-tissue laxity component vs bony deformity.
7.5 Femoral and Tibial Mechanical/Anatomical Angles
- mLDFA (mechanical Lateral Distal Femoral Angle): 85°–90° normal
- mMPTA (mechanical Medial Proximal Tibial Angle): 85°–90° normal
- Identify whether deformity is femoral or tibial in origin
7.6 Limb Length (LLD)
- True length from femoral head centre to ankle mortise.
- Bilateral comparison.
8. TECHNIQUE / PROCEDURE
8.1 Patient Preparation
- Patient changes to gown; remove metallic objects, jewellery.
- Ensure full lower limb is exposed from hip to ankle.
- Gonadal shielding where feasible (balanced against diagnostic field requirements).
8.2 Patient Positioning (Weight-Bearing)
- Patient stands erect on the platform in front of the detector.
- Feet positioned: shoulder-width apart OR in standardised position (feet together, first metatarsals and heels touching, toes pointing forward).
- Patellae facing forward (critical — ensures correct rotational alignment).
- Knees in full extension (no flexion).
- Hands placed on shoulders or holding side handles to avoid superimposition over pelvic/hip region.
- Both lower limbs imaged simultaneously on bilateral studies.
8.3 X-ray Parameters (Typical)
| Parameter | Value |
|---|---|
| Tube voltage (kVp) | 70–90 kVp (lower limb); 90–110 kVp (pelvis) |
| mAs | 10–25 mAs per exposure |
| Focus-to-detector distance (FDD) | 300–400 cm (long FFD reduces magnification) |
| Collimation | Tight — to body width |
| Projection | Anteroposterior (AP) standing |
8.4 Number of Exposures
- 2-frame stitch: Hip-to-knee + Knee-to-ankle (most common)
- 3-frame stitch: Hip / Knee / Ankle (for tall patients or large field)
- Each frame overlaps the previous by 10–20 cm to provide registration landmarks
8.5 Overlap Region (Critical)
- The overlapping zone between adjacent frames must include a bony landmark (e.g., tibial plateau/condyles).
- Without adequate overlap, stitching algorithms fail or produce gross misregistration.
9. IMAGE STITCHING PROCESS
Step-by-Step Stitching (Manual & Automated)
Frame 1 (Hip region) + Frame 2 (Knee region) + Frame 3 (Ankle region)
↓ ↓ ↓
Overlap zone A Overlap zone B
↓
STEP 1: Pre-processing
→ Normalise brightness/contrast across frames
→ Apply flat-field correction
↓
STEP 2: Feature Detection / Registration
→ Identify matching anatomical landmarks in overlap zones
→ Methods: SIFT, SURF, ORB, or Canny edge detection
→ Bone edges detected as registration features
↓
STEP 3: Image Alignment (Transformation)
→ Rigid or affine transformation applied
→ Frames shifted/rotated to align bone contours
↓
STEP 4: Image Fusion (Blending)
→ Alpha blending (weighted pixel average in overlap zone)
→ OR Wavelet domain fusion (frequency-based)
→ OR Gradient blending
↓
STEP 5: Output
→ Single composite full-length radiograph
→ DICOM format stored in PACS
9.1 Manual Stitching (Traditional)
- Performed on dedicated PACS workstations or dedicated software (e.g., Sectra, Horos, OsiriX).
- Operator manually aligns landmarks in overlapping zones.
- Time: 3–10 minutes per case.
- Subject to inter-observer variability.
9.2 Automated Stitching (Modern)
- Feature-based: Detects anatomical features (bone edges, joint contours) using computer vision algorithms.
- Canny algorithm (Alkhatatbeh et al., 2022): Detects bone edges → aligns them → fuses using Wavelet form domain. P-value 0.974 vs. manual; stitching time = 3 seconds.
- Intensity-based: Maximises normalised cross-correlation in the overlap zone.
- AI/Deep learning: Emerging convolutional neural networks (CNNs) for automated landmark detection and registration.
9.3 Common Stitching Artefacts
| Artefact | Cause | Effect |
|---|---|---|
| Step artefact / Mismatch | Bone misalignment at junction | False axis measurement |
| Ghost/double contour | Poor registration | Cortical duplication |
| Brightness banding | Exposure difference between frames | Density discontinuity |
| Magnification mismatch | Different FFDs per frame | Scale discrepancy |
| Patient movement artefact | Motion between frames | Anatomy shift |
10. COMPONENTS / EQUIPMENT
10.1 X-ray Generator and Tube
- High-frequency generator.
- Tube with rotating anode (for heat loading across multiple exposures).
- Collimator with tight field restriction.
10.2 Detector System
- Flat-panel detector (FPD): Amorphous selenium or cesium iodide scintillator, typically 43 × 43 cm.
- Long cassette CR systems: Up to 35 × 91 cm imaging plates (reduces frames needed).
- Motorised bucky/column: Moves the detector vertically between exposures under programmable control.
10.3 Patient Stand / Platform
- Elevated non-radio-opaque platform with foot markings.
- Alignment arrows for foot placement standardisation.
- Side handles for patient stability.
- Some systems incorporate a calibration marker (radio-opaque ruler at known distance) for magnification correction.
10.4 Stitching Software
- Integrated into DR system (manufacturer proprietary).
- OR workstation-based PACS tools.
- Modern AI platforms (e.g., TraumaCad, Sectra Orthopaedic, mediCAD).
10.5 EOS® System (Advanced Dedicated System)
- Slot-scanning X-ray system using linear detectors.
- Patient stands in the EOS cabin; simultaneous frontal + lateral low-dose images acquired.
- No "stitching" needed — single continuous image.
- Dose ~50–80% lower than conventional standing radiography.
- Generates 3D skeletal models from biplanar images.
11. RADIATION DOSE CONSIDERATIONS
| Method | Approximate Effective Dose |
|---|---|
| Single standard AP knee | 0.005–0.01 mSv |
| 2-frame stitch lower limb | 0.05–0.2 mSv |
| 3-frame stitch (hip to ankle) | 0.1–0.3 mSv |
| EOS full-body | 0.05–0.1 mSv (ultra-low) |
| Full-spine stitch (scoliosis) | 0.5–1.5 mSv conventional |
ALARA principle (As Low As Reasonably Achievable) applies — minimise frames and optimise exposure parameters. EOS is now preferred for paediatric scoliosis surveillance to reduce cumulative dose.
12. QUALITY ASSURANCE (QA)
Geometric Accuracy
- Magnification must be uniform or corrected using a calibration sphere/ruler at the level of the anatomy.
- Each frame should have the same FFD.
- A 25 mm calibration ball at hip level is common — used to calculate true scale.
Rotational Accuracy
- Patellae must face directly forward.
- Rotational malalignment (foot external rotation) will falsely alter HKA measurements.
- A 2° rotation error can produce a ~1° change in the apparent HKA angle.
Patient Positioning Reproducibility
- Standardised foot templates/markings ensure reproducibility on serial studies.
- Studies show that full body weight axial pressure during supine CT scanograms is comparable to standing stitch radiographs for HKA/WBL/JLCA (Liu et al., Skeletal Radiology, 2024, PMID: 38443696).
Stitching Accuracy Verification
- Compare measured bone lengths on stitched image vs. expected anatomical values.
- On automated systems, accuracy is validated by comparing HKA angles to manually stitched gold-standard (Alkhatatbeh et al., 2022 — 100% accuracy rate).
13. INTERPRETATION — WHAT IS READ ON THE RADIOGRAPH
13.1 Mechanical Axis
- Draw a straight line from the centre of the femoral head → centre of the tibial spines → centre of the ankle mortise (talus).
- Normal: this line passes through or just medial to the knee centre.
13.2 Varus Deformity (Genu Varum)
- Mechanical axis passes medial to the knee.
- Associated with medial compartment OA.
- Indication for HTO or medialising tibial osteotomy.
13.3 Valgus Deformity (Genu Valgum)
- Mechanical axis passes lateral to the knee.
- Associated with lateral compartment OA.
- Indication for distal femoral osteotomy (DFO).
13.4 Limb Length Discrepancy
- Measured from femoral head centre to ankle mortise bilaterally.
- True (bone) LLD vs. apparent LLD (from pelvic tilt).
13.5 Site of Deformity
- Using mLDFA and mMPTA angles, deformity localised to:
- Femoral (distal femur valgus/varus)
- Tibial (proximal or mid-shaft)
- Combined (double-level osteotomy required)
14. APPLICATIONS IN SURGERY
14.1 Total Knee Arthroplasty (TKA)
- Pre-op: Measure HKA, plan implant size, coronal alignment target.
- Post-op: Verify restoration of neutral mechanical axis (ideal: HKA = 0° ± 3°).
14.2 High Tibial Osteotomy (HTO)
- Plan angle of correction using Fujisawa point method.
- Target WBL ratio = 62.5% for varus correction.
- Osteotomy line length and wedge width calculated from the full-length radiograph.
14.3 Distal Femoral Varus Osteotomy
- Indicated for valgus malalignment + lateral compartment OA.
- Mechanical axis drawn; angle alpha determined at the femoral correction site.
14.4 Scoliosis Surgery
- Pre-op Cobb angle, curve flexibility.
- Intra-operative stitched fluoroscopy for long-segment instrumentation.
- Post-op implant position and correction assessment.
14.5 Limb Reconstruction
- Malunion correction (femoral/tibial).
- Expandable prosthesis monitoring in oncology.
15. COMPARISON WITH OTHER MODALITIES
| Modality | Advantages | Disadvantages |
|---|---|---|
| Stitch radiography (standing) | Weight-bearing, accurate HKA, low cost, widely available | 2D only, radiation, stitching artefacts possible |
| MRI (upright) | No radiation, soft tissue detail | Expensive, limited availability, longer exam time |
| CT scanogram | High resolution, no stitching needed | No weight-bearing (conventional), higher radiation |
| Supine weight-bearing CT | Mimics standing mechanically | Newer technique, needs specialised equipment |
| EOS biplanar | Ultra-low dose, 3D modelling, simultaneous AP + lateral | Cost, availability, bulky system |
Liu et al. (2024, Skeletal Radiology, PMID: 38443696) demonstrated no significant difference between standing stitch radiography and supine weight-bearing CT scanograms (with full body weight applied) for WBL, HKA, and JLCA measurements.
16. LIMITATIONS & PITFALLS
- Patient movement between frames — most common source of error.
- Rotational malalignment — feet externally rotated alters HKA.
- Stitching artefacts — step artefact, double contour at junction.
- Magnification variation — if FFD differs per frame.
- Pelvic obliquity / scoliosis — alters apparent limb alignment.
- 2D limitation — cannot assess axial/sagittal plane simultaneously.
- Radiation dose — significant for serial paediatric studies.
- Weight-bearing ability — patients with pain/instability may not stand correctly.
- No soft tissue information — cartilage, ligaments not visible.
17. RECENT ADVANCES
| Advance | Description |
|---|---|
| Automated AI stitching | Canny edge + Wavelet fusion (3 sec, 100% accuracy — 2022) |
| AI landmark detection | Deep learning auto-identifies hip/knee/ankle centres |
| AI angle measurement | Automated HKA, WBL, mLDFA from stitched image |
| Weight-bearing CT | Supine CT with axial load as alternative |
| EOS 3D modelling | 3D bone models from biplanar stitch-free images |
| Robotic TKA navigation | Intraoperative HKA verification using fluoroscopic stitching |
| AR/VR overlay | Stitched radiograph integrated with surgical navigation |
Archer et al. (Skeletal Radiology, 2025, PMID: 40295351) evaluated AI-generated lower extremity radiographic measurements in patients with implants — showing high accuracy of automated systems.
18. DIAGRAMS
Diagram 1 — Full-Length Lower Limb Stitch Radiograph (Bilateral Standing)
Shows both lower limbs from pelvis to ankles with HKA mechanical axis lines drawn, demonstrating bilateral varus alignment with measurement annotations:
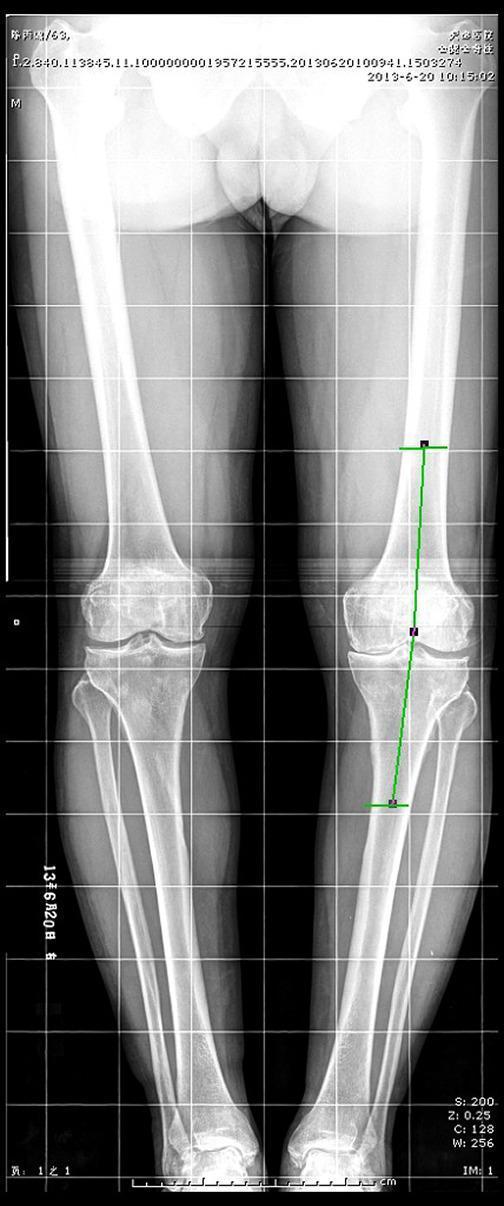
Diagram 2 — Full-Length Stitch Radiograph with HKA Axis Lines (Clinical)
Bilateral full-length standing radiograph with mechanical axis lines drawn from femoral head to ankle, showing genu valgum — includes bilateral limb length measurements (853.6 mm and 853.9 mm):
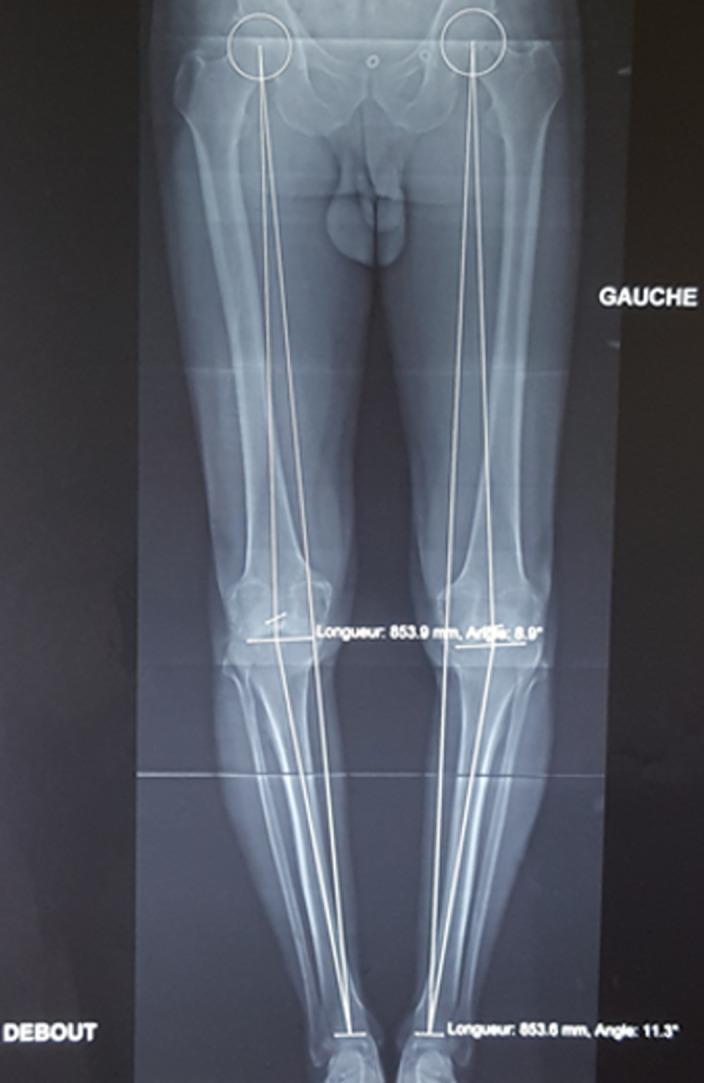
Diagram 3 — Patient Positioning for Stitch Radiography
Standardised patient positioning from multiple angles (anterior, posterior, lateral, oblique) showing the correct standing posture on the X-ray platform:
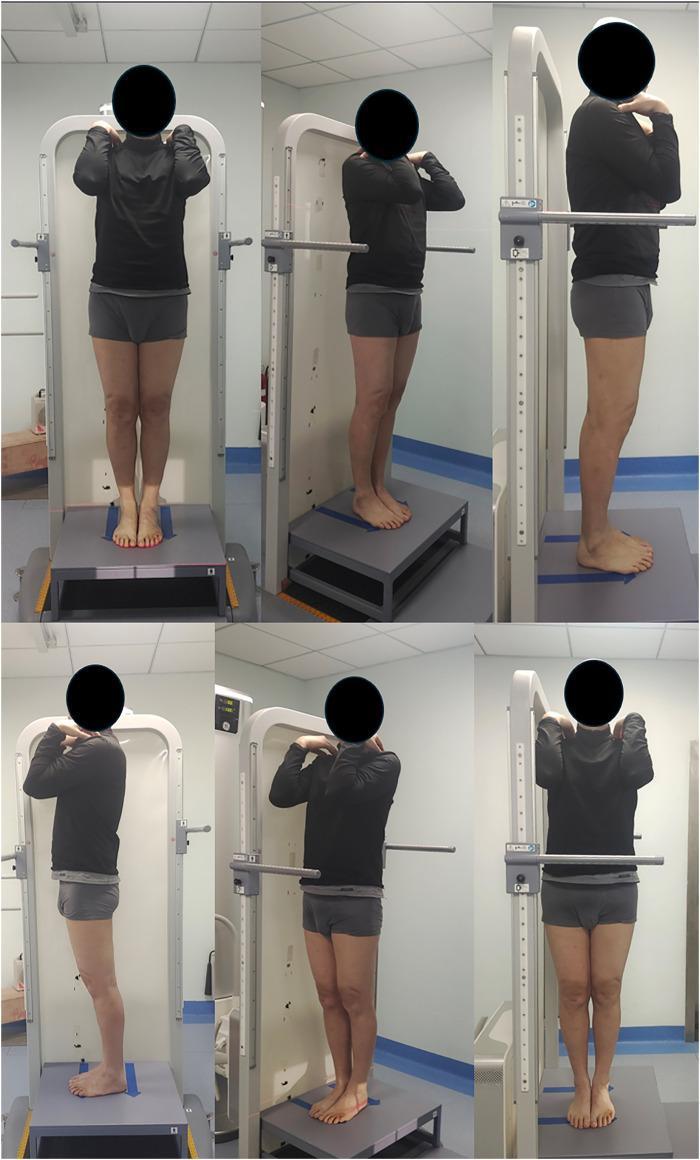
Diagram 4 — Mechanical Axis Measurement & Osteotomy Planning
Long-leg weight-bearing radiograph section showing mechanical axis lines (from hip centre to ankle centre), point of correction X on tibial plateau, and angle α for distal femoral varus osteotomy planning:
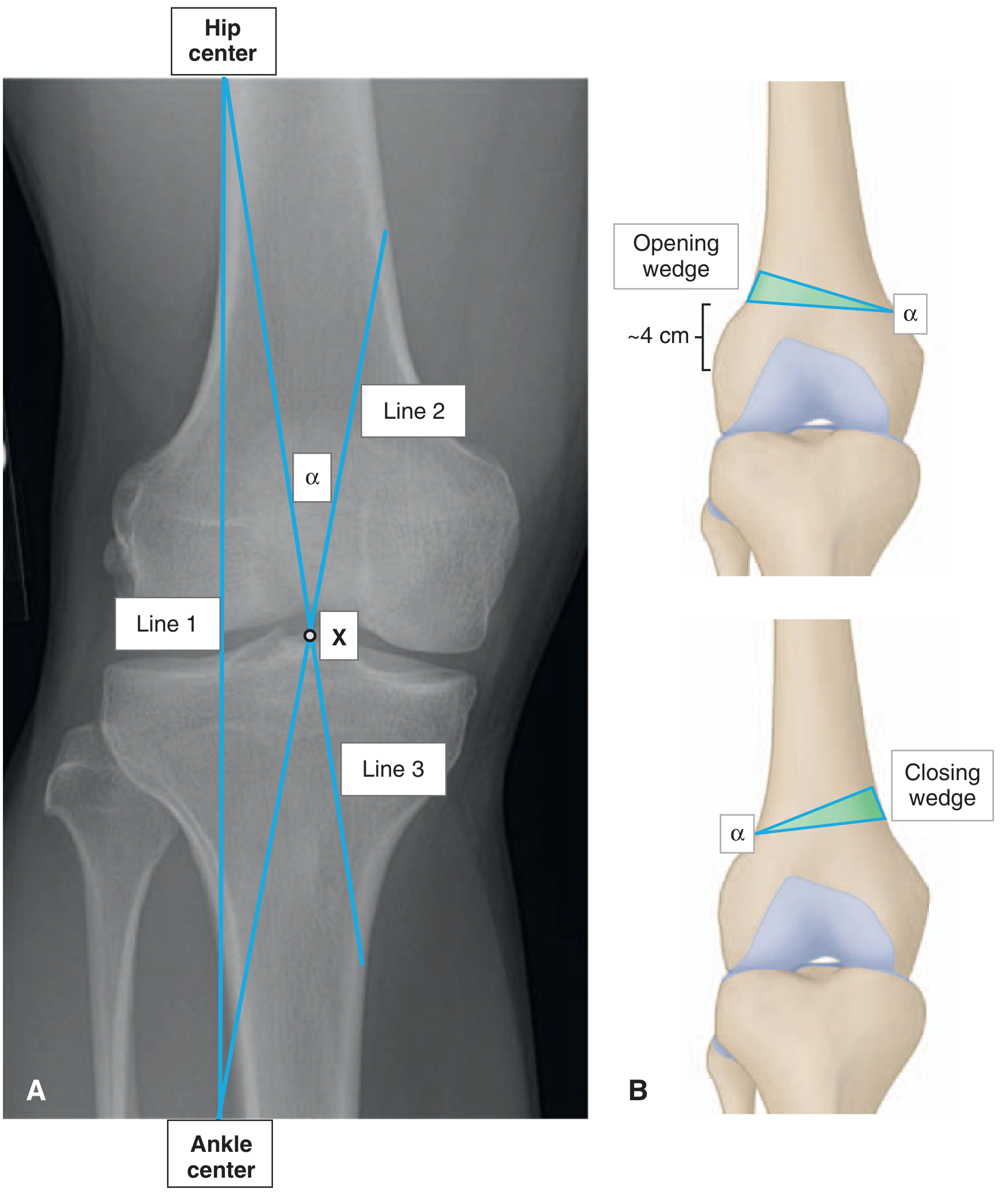
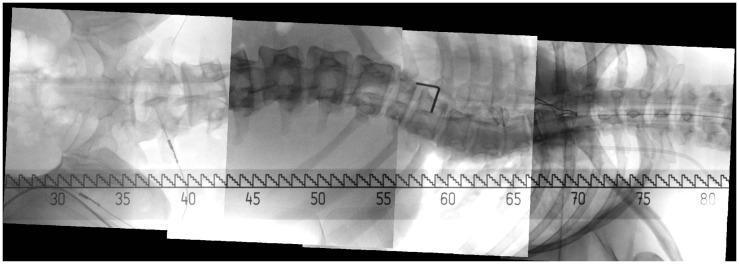
Diagram 5 — Intraoperative Spine Stitching (Panoramic C-arm)
Stitched intraoperative fluoroscopic image of thoracolumbar spine assembled from multiple C-arm frames, showing vertebral column alignment, implants, and calibration ruler:
19. SUMMARY TABLE
| Feature | Details |
|---|---|
| Definition | Multiple X-ray exposures stitched into one full-length composite image |
| Primary regions | Lower limb (hip to ankle), Spine (cervical to sacrum) |
| Position | Standing, weight-bearing (bilateral AP) |
| Frames | 2–3 overlapping exposures |
| Key measurement | HKA angle, WBL, MAD, limb length, mLDFA, mMPTA |
| Clinical use | TKA planning, HTO, DFO, scoliosis, LLD, deformity |
| Stitching | Manual (PACS workstation) or automated (AI/Canny/Wavelet) |
| Gold standard | Full-length standing AP radiograph |
| Modern alternative | EOS biplanar (simultaneous, ultra-low dose) |
| Key pitfalls | Rotation, patient movement, stitching artefact |
| Radiation dose | 0.05–0.3 mSv (2–3 frame lower limb) |
20. REFERENCES
- Alkhatatbeh T, Wang JL, Zhang WJ et al. "A new automatic stitching method for full-length lower limb radiography." Frontiers in Surgery, 2022. [PMID: 36311950] — DOI: 10.3389/fsurg.2022.1000074
- Liu X, Zhang B, Zhao C et al. "Assessment of lower limb alignment: supine weight-bearing CT scanograms compared with a standing full-length radiograph." Skeletal Radiology, 2024. [PMID: 38443696]
- Archer H, Xia S, Reine S et al. "Are artificial intelligence generated lower extremity radiographic measurements accurate in a cohort with implants?" Skeletal Radiology, 2025. [PMID: 40295351]
- Liodakis E, Kenawey M et al. "Upright MRI measurement of mechanical axis and frontal plane alignment: comparative study with weight bearing full length radiographs." Skeletal Radiology, 2011. [PMID: 21170524]
- Miller's Review of Orthopaedics, 9th Edition — Chapter on Imaging Studies (Knee) & Osteotomy Planning. — Miller's Review of Orthopaedics 9e, pp. 362, 466
- Rockwood and Green's Fractures in Adults, 10th Edition — Limb alignment and long-leg casting reference.
Key Exam Points:
- Stitch radiography = weight-bearing + multiple exposures + digital stitching
- HKA angle: measured from femoral head centre → talus centre; normal ≈ 0° ± 3°
- WBL ratio target for HTO varus correction = 62.5% of tibial plateau width
- EOS = slot-scan, biplanar, no stitching needed, ultra-low dose
- Main stitching artefact = step/mismatch artefact from patient movement
- Patellae must face directly forward for valid axis measurement
This is a shared conversation. Sign in to Orris to start your own chat.