bone marrow reduced means
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
"Reduced bone marrow" means the bone marrow has decreased cellularity — fewer blood-forming (hematopoietic) cells than normal. This is described medically as bone marrow hypoplasia (partial reduction) or bone marrow aplasia (near-complete absence of cells). The clinical syndrome that results is called aplastic anemia.
What It Means
Normally, bone marrow is packed with hematopoietic stem cells that produce red blood cells, white blood cells, and platelets. When the marrow is "reduced," these stem cells are depleted and replaced by fat cells, leaving a hypocellular marrow.
The result is pancytopenia — simultaneous reduction in all three blood cell lines:
| Blood Cell | Effect of Reduction |
|---|---|
| Red blood cells | Anemia (fatigue, pallor) |
| White blood cells (neutrophils) | Neutropenia → increased infection risk |
| Platelets | Thrombocytopenia → bleeding tendency |
Causes of Reduced Bone Marrow
Acquired
- Idiopathic (most common — ~70%, immune-mediated T-cell destruction of stem cells)
- Drugs (dose-related): chemotherapy agents, benzene, chloramphenicol, phenylbutazone, gold salts, NSAIDs, anticonvulsants
- Radiation: whole-body irradiation destroys stem cells in a dose-dependent manner
- Viral infections: hepatitis (seronegative, ~5% of cases), CMV, EBV, parvovirus B19 (causes pure red cell aplasia)
- Immune diseases: graft-versus-host disease (GVHD), SLE, eosinophilic fasciitis, thymoma
- Paroxysmal nocturnal hemoglobinuria (PNH): PIG-A gene mutation causes a clone of cells deficient in GPI-linked proteins
Inherited
- Fanconi anemia: autosomal recessive; defective DNA repair complex; marrow failure appears early in life, often with thumb/radial anomalies, kidney/spleen hypoplasia
- Telomerase defects: found in 5–10% of adult-onset aplastic anemia; premature stem cell exhaustion due to abnormally short telomeres
Diagnosis
Bone marrow biopsy is essential — it shows:
- Hypocellular marrow (< 25% cellularity for severe aplastic anemia)
- Replacement of hematopoietic tissue by fat cells
- Absence or marked reduction of all cell lineages
Treatment
- Immunosuppressive therapy: anti-thymocyte globulin (ATG) + cyclosporine (for patients without a matched donor)
- Allogeneic bone marrow/stem cell transplantation: curative, preferred for younger patients with a matched sibling donor
- Supportive: transfusions, growth factors, infection prophylaxis
In short: "reduced bone marrow" = hypocellular/aplastic marrow → pancytopenia. The most common cause in adults is autoimmune destruction of hematopoietic stem cells (aplastic anemia).
— Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 616; Harrison's Principles of Internal Medicine 22E
milia
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Milia
Milia (singular: milium) are small, benign, superficial keratinous cysts — 1–4 mm in diameter — that appear as firm, white to yellowish, dome-shaped papules just beneath the skin surface.
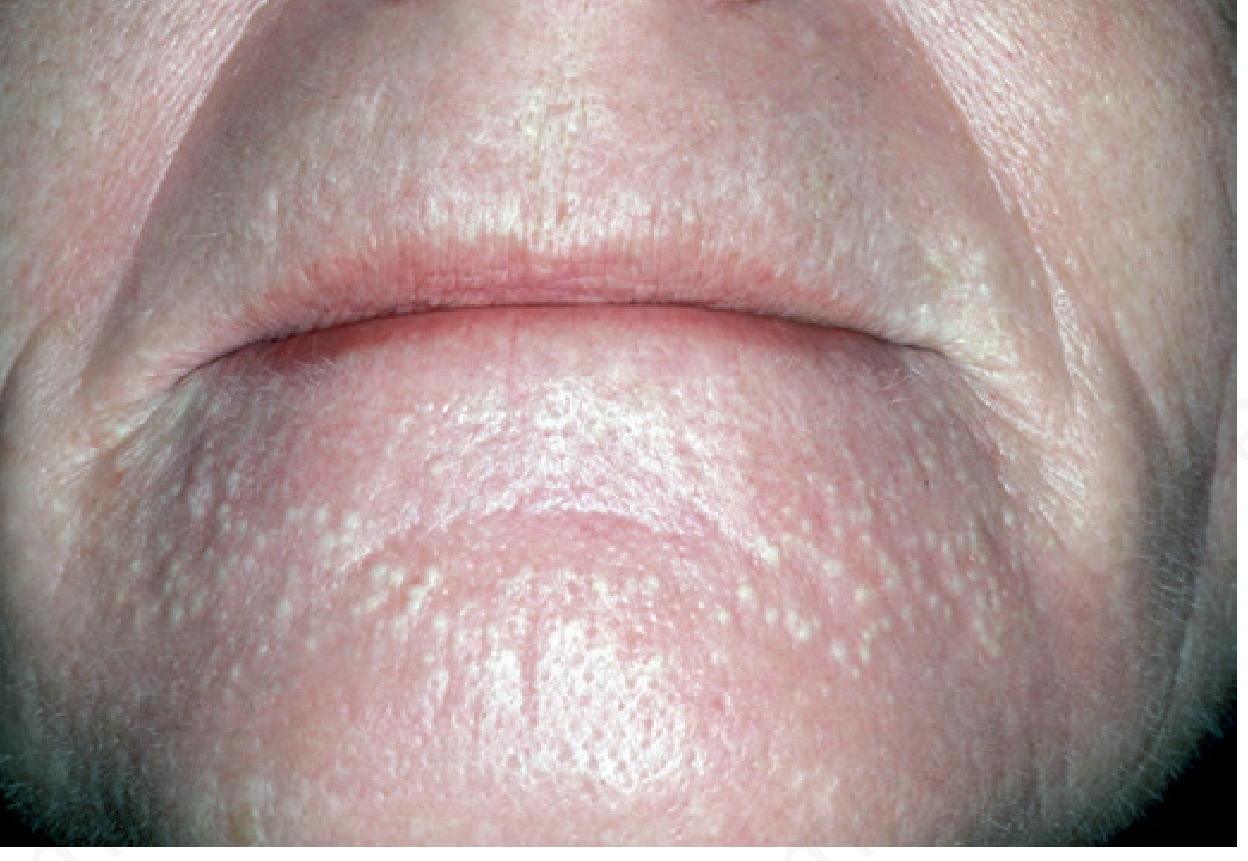
Origin
- Arise from the infundibulum (upper portion) of vellus hair follicles, or from eccrine ducts or minor salivary gland ducts (oral milia)
- The cyst wall is a stratified squamous epithelium with a granular layer; the cyst contents are laminated keratin
- Essentially small epidermoid cysts
Types
Primary Milia
Appear spontaneously, without an identifiable trigger.
| Setting | Details |
|---|---|
| Neonatal | 40–50% of newborns; mainly on the face (nose, cheeks); resolve spontaneously within 4 weeks |
| Epstein pearls | Milia on the hard palate of newborns; resolve on their own |
| Bohn nodules | On alveolar ridges of newborns; also self-resolving |
| Adults/children | Cheeks, eyelids, forehead, genitalia; tend to persist |
| Multiple eruptive milia | Large number erupt over weeks–months; can be idiopathic or familial |
| Milia en plaque | Multiple milia within an erythematous, edematous plaque; most common in the periauricular/periorbital region; mainly middle-aged women |
| Nasal crease milia | Horizontal row in the nasal crease; some congenital |
Secondary Milia
Arise after skin injury or disease — form as the epidermis attempts to reepithelialize.
Causes include:
- Blistering diseases: epidermolysis bullosa, bullous pemphigoid, pemphigus, porphyria cutanea tarda, herpes zoster, Stevens-Johnson syndrome, lupus erythematosus
- Trauma: dermabrasion, chemical peel, ablative laser, skin grafts, radiotherapy
- Drugs: long-term topical corticosteroids, occlusive moisturizers, cyclosporine, 5-FU, BRAF inhibitors
Associated Syndromes (Genetic)
Multiple milia can be a feature of:
- Oral-facial-digital syndrome type 1 (X-linked; lethal in males)
- Basal cell nevus syndrome (Gorlin syndrome)
- Rombo syndrome, Bazex-Dupré-Christol syndrome
- Atrichia with papular lesions
- Pachyonychia congenita type 2
- Loeys-Dietz syndrome, Brooke-Spiegler syndrome
- Naegeli-Franceschetti-Jadassohn syndrome
- Fanconi anemia-related syndromes
Histology
- Small epidermoid cyst with stratified squamous epithelial lining including a granular layer
- Cyst contents: laminated keratin
Differential Diagnosis
Comedonal acne, flat warts, syringomas, trichoepiteliomas, xanthelasma, milia-like calcinosis cutis, miliary osteomas
Treatment
- Neonatal milia: no treatment needed — spontaneous resolution
- Persistent milia: incise the overlying epidermis with a needle/lancet and express the cyst (comedo extractor can assist)
- Laser ablation and electrodesiccation are alternatives
- Multiple facial milia: topical retinoids reduce new lesion formation and facilitate removal
— Andrews' Diseases of the Skin, p. 782; Dermatology 2-Volume Set 5e, p. 2313; Fitzpatrick's Dermatology
This is a shared conversation. Sign in to Orris to start your own chat.