bell s pasy in deatil
Reading File
search_medical_text
Bell's palsy etiology pathophysiology clinical features diagnosis
search_medical_text
Bell's palsy treatment management prognosis complications
search_medical_image
Bell's palsy facial nerve palsy clinical presentation
GradeResponse
GradeResponse
GradeResponse
Bell's Palsy — Detailed Overview
Definition
Bell's palsy is an acute, idiopathic, unilateral peripheral facial nerve (CN VII) palsy. It is the most common cause of acute facial nerve paralysis, affecting roughly 20–30 per 100,000 people per year.
Anatomy Recap
The facial nerve (CN VII) exits the brainstem, passes through the internal auditory canal, through the geniculate ganglion, through the stylomastoid foramen, and then fans out to supply all ipsilateral muscles of facial expression, the stapedius muscle, the anterior 2/3 tongue (taste via chorda tympani), and the lacrimal/salivary glands.
Etiology & Pathophysiology
(Harrison's, p. 12502)
- The nerve undergoes inflammation with mononuclear cell infiltration, consistent with infectious or immune-mediated injury.
- Herpes simplex virus type 1 (HSV-1) is the most commonly implicated pathogen — its DNA has been detected in endoneurial fluid and posterior auricular muscle, suggesting reactivation in the geniculate ganglion.
- Varicella-zoster virus (VZV) accounts for up to 1/3 of cases and is the second most frequent cause (when VZV is found with vesicles, the entity is called Ramsay Hunt Syndrome).
- Other viruses (EBV, CMV, adenovirus) and HIV seroconversion can also cause Bell's palsy.
- Inflammation causes edema within the bony facial canal, leading to nerve compression and ischemia.
Risk Factors
| Factor | Detail |
|---|---|
| Age | Peak incidence 15–45 years |
| Pregnancy | 3× increased risk (especially 3rd trimester) |
| Diabetes mellitus | Increased risk |
| Immunocompromised state | HIV, chemotherapy |
| Prior episode | Recurrence in ~10% |
Clinical Features
Key Presenting Symptoms
- Acute-onset unilateral facial weakness/paralysis — develops over hours to a few days
- Inability to close the eye on the affected side (lagophthalmos)
- Flattening of the nasolabial fold
- Drooping of the mouth corner, with deviation of mouth to unaffected side
- Loss or reduction of taste on anterior 2/3 of tongue (chorda tympani involvement)
- Hyperacusis (sensitivity to sound) due to stapedius muscle paralysis
- Post-auricular pain or numbness (often precedes the palsy by 1–2 days)
- Decreased lacrimation or, paradoxically, excessive tearing (crocodile tears — from aberrant regeneration)
Critical Distinguishing Feature: Upper vs. Lower Motor Neuron Lesion
| Feature | Bell's Palsy (LMN / Peripheral) | Central Lesion (UMN / Stroke) |
|---|---|---|
| Forehead involvement | Yes — forehead paralyzed | No — forehead spared (bilateral cortical input) |
| Entire face affected | Yes | Lower face mainly |
| Other neuro signs | None | Often present (limb weakness, etc.) |
Forehead sparing = central cause until proven otherwise. Bell's palsy always involves the forehead.
Clinical Image
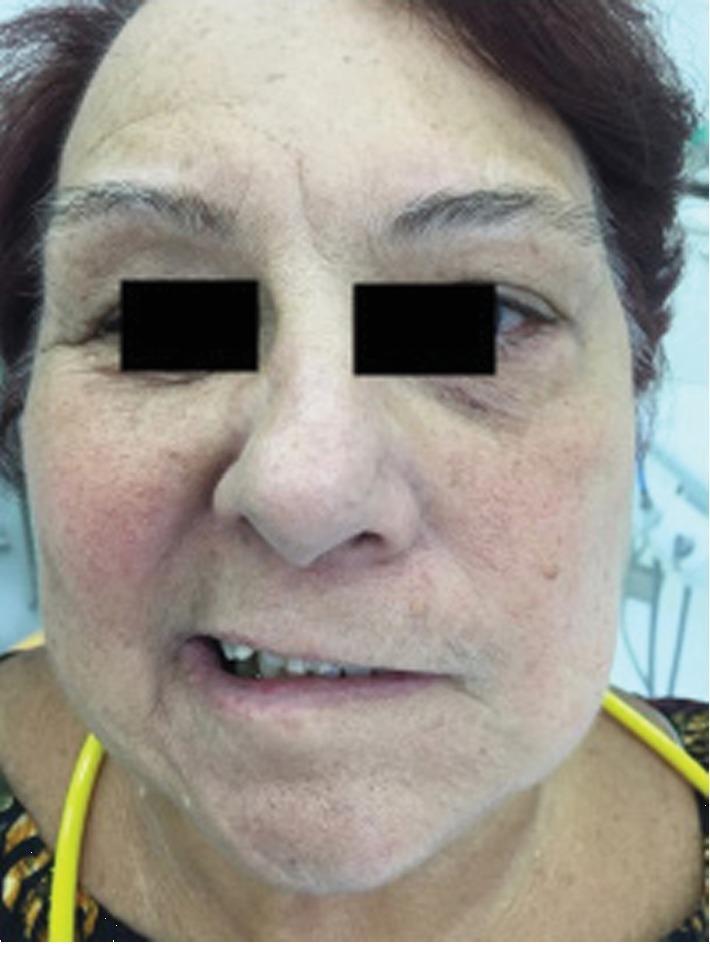
A 71-year-old female with Grade V Bell's palsy showing severe unilateral asymmetry — flattened left nasolabial fold, drooping left labial commissure, and mouth deviated to the unaffected right side.
Grading — House-Brackmann Scale
| Grade | Description |
|---|---|
| I | Normal |
| II | Mild dysfunction — slight weakness |
| III | Moderate dysfunction — obvious asymmetry, can close eye with effort |
| IV | Moderately severe — can barely close eye, obvious asymmetry |
| V | Severe — only slight movement, incomplete eye closure |
| VI | Total paralysis |
Diagnosis
Bell's palsy is a diagnosis of exclusion. No specific test confirms it; the focus is on ruling out dangerous causes.
Workup
- History & physical: Look for vesicles (Ramsay Hunt), otitis media, parotid mass, tick bite (Lyme), or systemic features (sarcoidosis, lymphoma).
- Blood tests: Consider Lyme serology in endemic areas, blood glucose, CBC.
- MRI with gadolinium: Indicated if:
- Atypical features or slow progression (>3 weeks)
- No improvement by 4 months
- Recurrent ipsilateral palsy
- Other cranial nerve deficits
- EMG/Nerve conduction studies: Used to assess severity and prognosis after 2–3 weeks.
Differential Diagnosis
| Condition | Clues |
|---|---|
| Ramsay Hunt syndrome | VZV, vesicles in ear/palate, severe pain |
| Lyme disease (neuroborreliosis) | Endemic area, rash, bilateral palsy possible |
| Stroke | Forehead sparing, other neuro signs |
| Parotid tumor | Gradual onset, palpable mass |
| Sarcoidosis | Bilateral palsy, systemic features |
| Otitis media/cholesteatoma | Ear pain, discharge |
| Guillain-Barré syndrome | Bilateral, ascending weakness |
Treatment
(Harrison's, p. 12504)
1. Corticosteroids (First-line)
- Prednisone 60–80 mg/day for the first 5 days, then tapered over the next 5 days.
- Modestly shortens recovery and improves functional outcome.
- Most effective when started within 72 hours of symptom onset.
2. Antivirals
- Large, well-controlled RCTs found no added benefit of valacyclovir (1000 mg/day × 5–7 days) or acyclovir (400 mg 5× daily × 10 days) over steroids alone in typical Bell's palsy.
- Use antivirals if vesicular lesions are present in the palate or external auditory canal (suggesting VZV/Ramsay Hunt) — in that setting, combination therapy is standard.
3. Eye Care (Critical)
- Paper tape over the eyelid at night to prevent corneal exposure.
- Artificial tears during the day.
- Consider a moisture chamber or eye patch.
- Ophthalmology referral if corneal exposure develops.
4. Physiotherapy
- Gentle massage of weakened muscles helps prevent contracture.
- Facial exercises during recovery.
5. Surgical Options
- For permanent paralysis: cosmetic procedures (e.g., facial reanimation surgery, gold weight implant in upper eyelid, brow lift).
- Surgical decompression of the facial nerve is controversial and rarely performed.
Prognosis
- ~70–80% of patients recover completely without treatment.
- With steroid treatment, recovery rates improve further.
- Recovery usually begins within 3–4 weeks and is complete by 3–6 months in most.
- Poor prognostic indicators:
- Complete paralysis at onset
- Age > 60 years
- Severe pain
- No recovery within 3 weeks
- Diabetes mellitus
Complications
| Complication | Description |
|---|---|
| Corneal ulceration/keratitis | From incomplete eye closure — can be vision-threatening |
| Synkinesis | Aberrant nerve regeneration (e.g., eye closes when smiling) |
| Crocodile tears (gustatory lacrimation) | Tearing while eating due to aberrant regeneration |
| Contracture | Permanent muscle stiffening from prolonged denervation |
| Psychological impact | Depression, social withdrawal, body image issues |
Special Populations
- Pregnancy: Steroids are used cautiously; most cases recover well.
- Children: Better prognosis than adults; generally recover fully.
- Bilateral palsy: Should prompt workup for Lyme disease, sarcoidosis, Guillain-Barré, or HIV — bilateral Bell's palsy is rare and demands investigation.
Summary: Bell's palsy is an acute peripheral facial nerve palsy caused primarily by HSV-1 reactivation. The hallmark is complete unilateral facial weakness including the forehead. Management is early steroids + eye protection; most patients recover fully.
This is a shared conversation. Sign in to Orris to start your own chat.