how to remebr autonomic nervius sytem assessment
Reading File
search_medical_text
autonomic nervous system assessment clinical evaluation mnemonics
search_medical_text
sympathetic parasympathetic nervous system clinical signs symptoms memory
GradeResponse
GradeResponse
Here is a structured, memorable breakdown of the autonomic nervous system (ANS) assessment:
Remembering the ANS Assessment
Step 1 — Know the Two Divisions First
Use the classic mnemonics:
| Division | Mnemonic | Key Effects |
|---|---|---|
| Sympathetic | "Fight or Flight" | ↑HR, ↑BP, dilated pupils, dry mouth, sweating, bronchodilation, ↓GI motility |
| Parasympathetic | "Rest and Digest" | ↓HR, ↓BP, constricted pupils (miosis), salivation, lacrimation, urination, defecation, GI motility |
SLUDGE = Parasympathetic (cholinergic) excess:
Salivation, Lacrimation, Urination, Defecation, GI cramps, Emesis
DUMBELS = Same (used in toxicology for organophosphate poisoning):
Defecation, Urination, Miosis, Bradycardia, Emesis, Lacrimation, Salivation
Step 2 — Know What to Assess (Use "HOPS")
| Letter | Domain | What to Check |
|---|---|---|
| H | Heart rate/BP | Resting HR, postural BP changes |
| O | Orthostasis | BP drop ≥20 mmHg systolic or ≥10 mmHg diastolic on standing |
| P | Pupils | Symmetry, light reflex, response to accommodation |
| S | Sweat/Skin/Secretions | Anhidrosis, dry mouth, dry eyes |
Step 3 — Clinical Tests (Remember "HSVT")
| Test | What It Assesses |
|---|---|
| Heart Rate Variability (HRV) | Parasympathetic integrity (best done with deep breathing) |
| Skin conductance / Sweat test | Sympathetic sudomotor function |
| Valsalva maneuver | Both sympathetic and parasympathetic responses |
| Tilt table test | Cardiovagal and adrenergic function; detects POTS, orthostatic hypotension |
Step 4 — Anatomy Anchor (Spine Levels)
A simple anchor for anatomy:
- Sympathetic: T1–L2 ("ThoracoLumbar" = Think Loud = Fight or Flight)
- Parasympathetic: Cranial nerves (III, VII, IX, X) + S2–S4 ("CraniaSacral")
Memory trick: "Craniosacral is calm" (parasympathetic = rest and digest)
Step 5 — Dysautonomia Red Flags (Remember "DROP")
Dizziness on standing (orthostatic hypotension) Resting tachycardia or bradycardia Office BP variability (hypertension or hypotension) Pupil abnormalities (Horner's, Adie's)
Quick Summary Card
ANS Assessment = HOPS + HSVT + SLUDGE
Sympathetic → Fight or Flight → T1–L2
Parasympathetic → Rest & Digest → Craniosacral (CN III,VII,IX,X + S2-S4)
Orthostatic drop: ≥20 systolic / ≥10 diastolic mmHg
These frameworks are grounded in standard autonomic testing consensus (American Autonomic Society / AAN guidelines) and Harrison's Principles of Internal Medicine (pp. 717, 12459).
now assemnet of autonimc nervoud sytem
search_medical_text
autonomic nervous system clinical assessment tests orthostatic hypotension heart rate variability
search_medical_text
Valsalva maneuver tilt table test autonomic function testing
GradeResponse
GradeResponse
search_medical_text
autonomic neuropathy examination findings pupil sweat skin cardiovascular reflex
search_medical_image
autonomic nervous system assessment diagram tests
GradeResponse
Here is a complete, structured clinical assessment of the autonomic nervous system:
Autonomic Nervous System (ANS) Assessment
The ANS assessment is divided into History, Physical Examination, and Formal Autonomic Tests.
1. History
Ask about symptoms across each organ system:
| System | Sympathetic Dysfunction | Parasympathetic Dysfunction |
|---|---|---|
| Cardiovascular | Orthostatic dizziness, fainting | Resting tachycardia |
| GI | Constipation | Nausea, vomiting, diarrhea |
| Urinary | Urinary retention | Overflow incontinence |
| Sexual | Erectile dysfunction | — |
| Sweat/Skin | Anhidrosis, heat intolerance | Hyperhidrosis |
| Eyes | Ptosis, miosis (Horner's) | Blurred near vision |
2. Physical Examination
A. Cardiovascular
- Resting HR & BP — both lying and standing
- Orthostatic Hypotension Test:
- Measure BP supine → then at 1 min and 3 min after standing
- Positive = systolic drop ≥20 mmHg or diastolic drop ≥10 mmHg
- Indicates sympathetic adrenergic failure
B. Pupils
| Finding | Meaning |
|---|---|
| Miosis + ptosis + anhidrosis | Horner's syndrome (sympathetic loss) |
| Dilated, unreactive pupil | Parasympathetic loss (CN III lesion) |
| Light-near dissociation | Adie's tonic pupil (postganglionic parasympathetic) |
| Small, irregular, react to accommodation | Argyll Robertson pupil (syphilis) |
C. Skin & Sweating
- Check for anhidrosis (dry, warm skin) vs. hyperhidrosis
- Loss of sweating = sympathetic cholinergic failure
D. Eyes, Mouth, Bladder
- Dry eyes, dry mouth = parasympathetic failure
- Bladder palpation for retention
3. Formal Autonomic Tests
(Harrison's Principles, p. 715)
A. Parasympathetic Tests
| Test | How | Normal Response |
|---|---|---|
| Heart Rate Variability (HRV) to Deep Breathing | Patient breathes 6 cycles/min; measure R-R interval variation on ECG | HR varies ≥15 bpm (E:I ratio ≥1.2) |
| Valsalva Ratio | Forceful expiration against closed glottis for 15 sec | HR speeds up in phase II, then bradycardia in phase IV; ratio ≥1.5 |
| 30:15 Ratio | HR at beat 30 vs beat 15 after standing | Ratio ≥1.04 |
B. Sympathetic Cholinergic Tests (Sudomotor)
| Test | What It Does |
|---|---|
| Thermoregulatory Sweat Test (TST) | Patient heated; sweating pattern mapped with indicator powder |
| QSART (Quantitative Sudomotor Axon Reflex Test) | Acetylcholine applied via iontophoresis; measures axon reflex sweating — postganglionic |
C. Sympathetic Adrenergic Tests
| Test | What It Assesses |
|---|---|
| BP response to Valsalva | Phase II late BP fall + Phase IV overshoot = intact sympathetic adrenergic function |
| Tilt-Table Test (Head-up 60–70°, 20–45 min) | Distinguishes autonomic failure (gradual BP fall, no compensatory HR rise) from POTS (HR rise ≥30 bpm) from vasovagal syncope (sudden BP+HR drop) |
4. Tilt Table Test — Key Patterns
| Pattern | Finding | Diagnosis |
|---|---|---|
| Progressive BP fall, no HR rise | Sympathetic adrenergic failure | Neurogenic orthostatic hypotension |
| HR rise ≥30 bpm, minimal BP fall | Sympathetic preserved, venous pooling | POTS |
| Sudden BP + HR drop (late) | Vasovagal reflex | Neurally mediated syncope |
5. Summary Table — What Tests What
| Domain | Test |
|---|---|
| Parasympathetic (cardiovagal) | HRV to deep breathing, Valsalva ratio, 30:15 ratio |
| Sympathetic cholinergic (sudomotor) | TST, QSART |
| Sympathetic adrenergic (vasomotor) | BP response to Valsalva, tilt-table test |
Quick Clinical Rule
If the patient is dizzy on standing → Orthostatic BP test first If sweating abnormally → Sudomotor testing If unexplained syncope → Tilt-table test If small pupils + ptosis → Examine for Horner's (sympathetic) If dry eyes/mouth + urinary retention → Parasympathetic failure
expain in detail glassopharngeal neuragia
Reading File
search_medical_text
glossopharyngeal neuralgia clinical features diagnosis treatment
search_medical_text
glossopharyngeal neuralgia pathophysiology etiology triggers carbamazepine surgery
search_medical_image
glossopharyngeal nerve CN IX anatomy diagram
GradeResponse
GradeResponse
GradeResponse
Here is a detailed explanation of Glossopharyngeal Neuralgia (GPN):
Glossopharyngeal Neuralgia
1. Definition
Glossopharyngeal neuralgia is a rare but severe paroxysmal pain syndrome involving the 9th cranial nerve (CN IX — glossopharyngeal nerve), sometimes with co-involvement of the vagus nerve (CN X). It is analogous to trigeminal neuralgia but far less common.
(Harrison's Principles of Internal Medicine, 21st Ed., p. 12505–12506)
2. Anatomy of CN IX (Essential to Understanding the Pain)
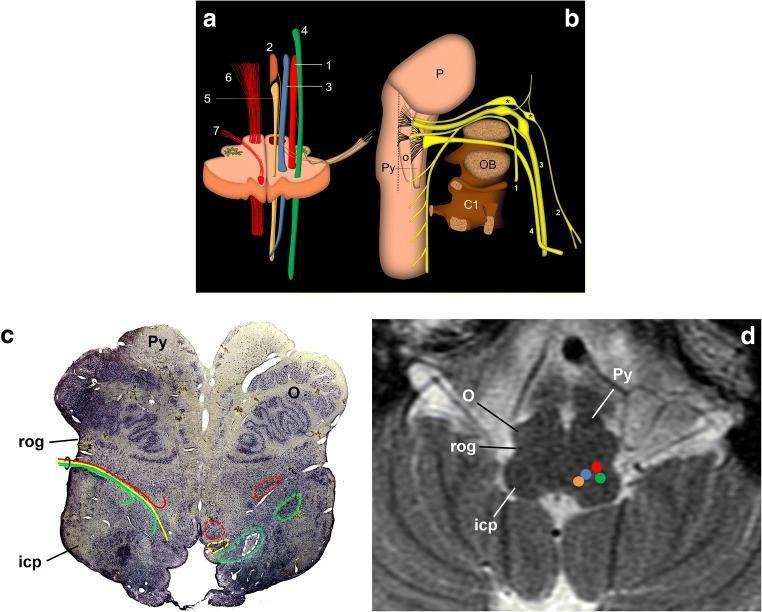
The glossopharyngeal nerve carries multiple functions:
| Function | Detail |
|---|---|
| General somatic sensation | Pharynx, middle ear, tympanic membrane, eustachian tube, posterior 1/3 of tongue → spinal trigeminal nucleus |
| Taste | Posterior 1/3 of tongue → nucleus solitarius |
| Baroreception | Carotid sinus → nucleus solitarius (blood pressure regulation) |
| Motor | Nucleus ambiguus → stylopharyngeus muscle only |
| Parasympathetic | Inferior salivatory nucleus → otic ganglion → parotid gland |
This wide sensory distribution explains why GPN pain can radiate from throat to ear, and why cardiac effects (via baroreceptor connections) can occur.
3. Epidemiology
- Much rarer than trigeminal neuralgia (roughly 100x less common)
- Incidence: ~0.5–0.8 per 100,000 per year
- Affects adults, typically >40 years
- Slightly more common in females
- Usually unilateral
4. Etiology & Pathophysiology
Causes
| Type | Examples |
|---|---|
| Idiopathic (most common) | No identifiable structural cause |
| Vascular compression | Posterior inferior cerebellar artery (PICA) or vertebral artery compressing CN IX at the root entry zone |
| Demyelinating disease | Multiple sclerosis (MS) |
| Tumors | Cerebellopontine angle tumors, parapharyngeal tumors, nasopharyngeal carcinoma |
| Elongated styloid process | Eagle syndrome — styloid or calcified stylohyoid ligament irritating CN IX |
| Infections/inflammation | Peritonsillar abscess, otitis media |
Pathophysiology
The underlying mechanism mirrors that of trigeminal neuralgia:
- Focal demyelination of CN IX (from compression or disease) leads to ephaptic transmission — abnormal cross-firing between pain fibers and non-pain fibers
- This produces ectopic discharge — brief, intense, electric-shock-like pain bursts
- Vascular pulsation against the nerve root continuously re-triggers this cycle
5. Clinical Features
Pain Characteristics
| Feature | Description |
|---|---|
| Quality | Severe, sharp, electric shock-like, stabbing, lancinating |
| Duration | Seconds to 2 minutes per episode |
| Onset | Paroxysmal (sudden onset and offset) |
| Frequency | Multiple attacks per day, or clustered |
| Location | Unilateral — originates in the tonsillar fossa |
| Radiation | Throat → ear (via tympanic branch), sometimes jaw/neck |
| Refractory period | Brief pain-free interval after attack |
Trigger Factors (highly characteristic)
- Swallowing (most common — even liquids)
- Talking
- Coughing / yawning
- Laughing
- Chewing
- Touching the throat or ear
Associated Cardiac Features (important — life-threatening)
In some patients, CN IX irritation also affects the carotid sinus baroreceptor fibers, leading to:
- Bradycardia
- Asystole
- Hypotension
- Syncope / sudden collapse
This cardiac variant is called "vagoglossopharyngeal syncope" and can be misdiagnosed as epilepsy or cardiogenic syncope.
Neurological Examination
- No motor or sensory deficit on examination (pain is functional/paroxysmal, not structural loss)
- This is an important distinguishing feature
6. Diagnosis
Clinical Diagnosis
Diagnosis is primarily clinical based on:
- Characteristic paroxysmal pain in the throat/tonsillar fossa
- Radiation to the ear
- Triggered by swallowing or coughing
- No neurological deficit
Confirmatory Test
- Topical anesthesia test: Applying lidocaine/cocaine spray to the oropharynx/tonsillar fossa temporarily abolishes the pain — strongly confirms diagnosis
Investigations to Identify Secondary Causes
| Investigation | Purpose |
|---|---|
| MRI brain with contrast (with FIESTA/CISS sequences) | Detect vascular compression of CN IX, MS plaques, tumors |
| MRA (MR Angiography) | Identify offending vessel (PICA, vertebral artery) |
| CT neck/skull base | Assess elongated styloid process (Eagle syndrome) |
| ECG / Holter monitor | Document bradycardia/asystole during attacks |
| Nasopharyngoscopy | Exclude pharyngeal or tonsillar tumor |
7. Differential Diagnosis
| Condition | Key Distinguishing Feature |
|---|---|
| Trigeminal neuralgia | Pain in face (V2/V3), triggered by touch to face, not by swallowing |
| Eagle syndrome | Styloid process palpable; pain on turning head or swallowing |
| Geniculate neuralgia (CN VII) | Deep ear pain, triggered by touch in ear canal |
| Otitis media / mastoiditis | Constant dull ear pain, fever, signs of infection |
| Peritonsillar abscess | Constant pain, trismus, uvular deviation, fever |
| Nasopharyngeal carcinoma | Constant pain, cranial nerve deficits, mass on imaging |
| SUNCT syndrome | Short-lasting unilateral neuralgiform headache around eye |
8. Management
A. Medical (First-line)
| Drug | Mechanism | Dose | Notes |
|---|---|---|---|
| Carbamazepine (first choice) | Na+ channel blocker | 200–1200 mg/day | Monitor CBC, LFTs, hyponatremia |
| Oxcarbazepine | Na+ channel blocker | 300–1800 mg/day | Better tolerated than carbamazepine |
| Gabapentin | Ca²+ channel α2δ subunit | 300–3600 mg/day | Useful adjunct |
| Phenytoin | Na+ channel blocker | 300–400 mg/day | Second-line |
| Baclofen | GABA-B agonist | 30–80 mg/day | Can combine with carbamazepine |
| Lamotrigine | Na+ channel blocker | 100–400 mg/day | Third-line |
For cardiac syncope variant: a temporary pacemaker may be needed before surgical intervention to prevent asystole.
B. Interventional / Surgical (for refractory cases)
| Procedure | Indication | Detail |
|---|---|---|
| Microvascular Decompression (MVD) | Vascular compression on MRI | Teflon pad placed between vessel and CN IX at posterior fossa — highest long-term cure rate |
| CN IX Rhizotomy | No vascular compression identified | Surgical sectioning of CN IX root — definitive but causes permanent sensory loss |
| Percutaneous ganglion block | Temporary relief/diagnostic | Local anesthetic injected near jugular foramen |
| Stereotactic radiosurgery (Gamma Knife) | Poor surgical candidates | Radiation targeted to CN IX root entry zone |
| Styloidectomy | Eagle syndrome confirmed | Surgical shortening of elongated styloid process |
9. Prognosis
- Medical therapy controls pain in ~50–70% of patients initially
- Over time, many patients develop drug resistance or side effects
- MVD has the best long-term outcome when vascular compression is identified — remission rates >85%
- The cardiac syncope variant carries risk of sudden death if untreated
10. Summary
GPN = Paroxysmal electric-shock pain in tonsillar fossa
→ triggered by SWALLOWING
→ radiates to EAR
→ +/- CARDIAC SYNCOPE (bradycardia/asystole)
→ NO neurological deficit
Diagnose: Clinical + lidocaine spray test + MRI
Treat: Carbamazepine → MVD if refractory
This is a shared conversation. Sign in to Orris to start your own chat.