typhoid fever
Reading File
Finding Sources
Searching PubMed
"typhoid fever"[MeSH Terms] AND "treatment"[MeSH Terms]
Searching the Web
typhoid fever pathophysiology clinical features management 2024 2025
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
typhoid fever rose spots rash
Loading Image
Loading Image
I now have comprehensive data from multiple authoritative sources. Here is a complete clinical overview of typhoid fever:
Typhoid Fever (Enteric Fever)
Definition & Etiology
Typhoid fever (enteric fever) is a systemic illness caused by Salmonella enterica serotype Typhi and, less commonly, S. Paratyphi A, B, and C. The name "typhoid" was coined because of clinical similarity to typhus; "enteric fever" was later proposed to reflect the anatomic site of infection. Both terms remain in use.
S. Typhi and S. Paratyphi have no animal reservoir — humans are the sole host. Transmission is fecal-oral via contaminated food or water, or from chronic carriers (often with gallstones).
Epidemiology
- Estimated 9.2–21 million cases of typhoid fever and ~110,000–280,000 deaths per year globally
- Highest burden: Indian subcontinent (India, Pakistan, Bangladesh, Nepal), Eastern Mediterranean, and sub-Saharan Africa; can exceed 1,000 cases/100,000 children in some urban areas
- In the US, ~5,700 cases/year; 78% travel-associated, predominantly from South Asia
- Most affected: young children, adolescents, and travelers to endemic areas
- Risk factors: contaminated drinking water, street food, raw produce fertilized with sewage, prior H. pylori infection (associated with reduced gastric acidity)
Drug resistance is a major and growing concern:
- MDR strains (resistant to chloramphenicol, ampicillin, TMP-SMX) emerged in the 1980s
- Decreased susceptibility to ciprofloxacin (DSC) / fluoroquinolone resistance — especially from South/Southeast Asia (clone H58)
- XDR (extensively drug-resistant) S. Typhi emerged in Pakistan in 2016, also resistant to third-generation cephalosporins and fluoroquinolones
— Harrison's Principles of Internal Medicine 22E, p. 1359
Pathogenesis
- Ingestion of contaminated food/water → organisms reach the distal ileum
- Entry via M cells overlying Peyer's patches → phagocytosed by mononuclear cells in lymphoid tissue
- Peyer's patches enlarge (plateau-like elevations up to 8 cm diameter) in the terminal ileum; mucosal shedding creates oval ulcers oriented along the long axis of the ileum
- Unlike non-typhoidal Salmonella, S. Typhi disseminates via lymphatics and bloodstream → bacteremia
- Hematogenous seeding of liver, spleen, bone marrow, gallbladder, and other organs
- Typhoid nodules (small foci of parenchymal necrosis with macrophage aggregates) may appear in liver, spleen, bone marrow, and lymph nodes
- Red pulp of the spleen expands due to prominent phagocyte hyperplasia
- Gallbladder colonization → chronic carrier state (associated with gallstones)
— Robbins Basic Pathology, Robbins Cotran Pathologic Basis of Disease
Clinical Course
Incubation Period
10–14 days (range 5–21 days), depending on inoculum size and host immunity.
Classic Weekly Progression
| Week | Features |
|---|---|
| Week 1 | Fever rises in stepwise fashion; headache (80%), malaise, chills (35–45%), myalgia, cough (30%), relative bradycardia |
| Week 2 | High plateau fever (38.8–40.5°C); rose spots; splenomegaly; anorexia (55%); abdominal pain (30–40%); possible diarrhea or constipation |
| Week 3 | Complications: intestinal hemorrhage, perforation, encephalopathy; "typhoid state" (apathy, confusion) |
| Week 4 | Gradual defervescence if untreated and uncomplicated; may relapse |
Key Clinical Features
- Fever — present at initial evaluation in >75%; prolonged, sustained, up to 4 weeks untreated
- Relative bradycardia — pulse-temperature dissociation (classic but present in <50%)
- Rose spots — faint, salmon-colored, blanching maculopapular rash on trunk/chest; appear at end of week 1 in ~30% of patients; 2–5 day duration; difficult to see in darker skin
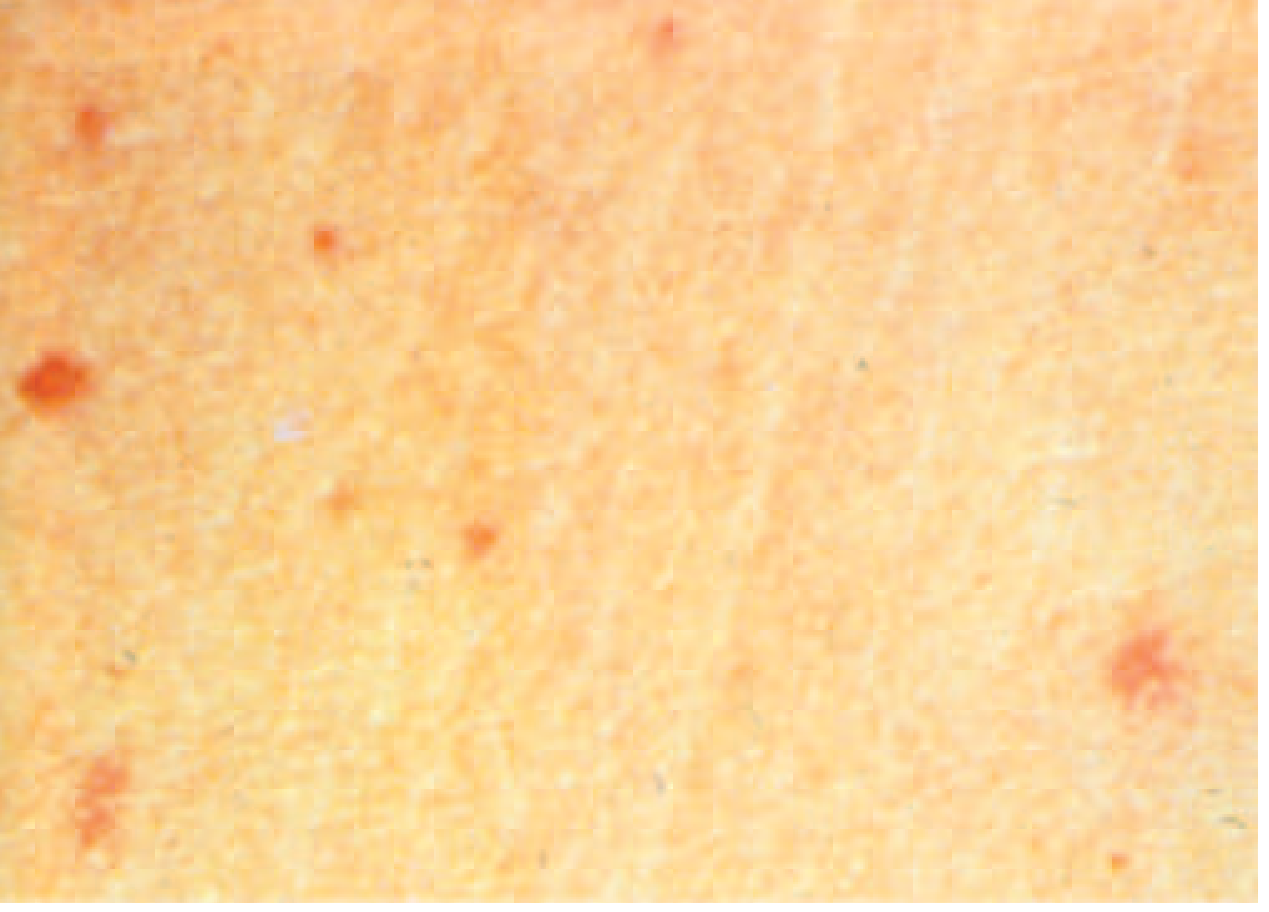
- Hepatosplenomegaly (3–6%), coated tongue (51–56%)
- Leukopenia or normal WBC (not leukocytosis — key distinguishing feature from bacterial sepsis)
- GI: anorexia, nausea, vomiting; diarrhea (22–28%) or constipation (13–16%)
Diagnosis
| Test | Notes |
|---|---|
| Blood culture | Gold standard — positive in ~90% during febrile phase (weeks 1–2); should be done before antibiotics |
| Bone marrow culture | Most sensitive; remains positive even after antibiotic therapy |
| Stool culture | Positive from week 2 onward; less reliable in week 1 |
| Urine culture | Useful adjunct |
| Widal test | Serologic (agglutination); widely used in endemic areas but low specificity — cross-reactions common; not reliable for diagnosis |
| Rapid antigen tests | Available; sensitivity variable |
Stool is negative early; blood culture is the test of choice in the first week. Bone marrow culture can diagnose even in antibiotic-treated patients.
— Jawetz Melnick & Adelberg's Medical Microbiology 28E; Tintinalli's Emergency Medicine
Complications
- Intestinal perforation — most feared; typically in the distal ileum at necrotic Peyer's patches; occurs in ~3% (up to 10% in some series); presents as acute abdomen
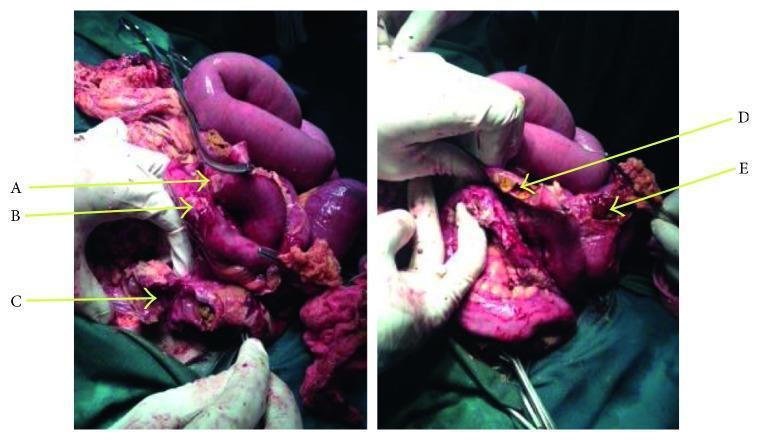
- Intestinal hemorrhage — from ulcerated Peyer's patches
- Hepatitis with focal necrosis
- Cholecystitis, gallbladder colonization → chronic carrier state
- Neuropsychiatric: encephalopathy, meningitis, psychosis, ataxia, seizures (typhoid encephalopathy)
- Myocarditis, endocarditis, pneumonia
- Septic arthritis, osteomyelitis (especially in sickle cell disease)
- DIC, renal failure
- Deafness (sequela)
Treatment
Antibiotic Selection (Based on Susceptibility)
| Susceptibility Pattern | Drug of Choice | Alternative |
|---|---|---|
| Fully susceptible | Fluoroquinolone (ciprofloxacin 500 mg BID × 5–7 days) | Chloramphenicol, ampicillin, TMP-SMX |
| MDR (resistant to chloramphenicol, ampicillin, TMP-SMX) | Fluoroquinolone OR ceftriaxone | Azithromycin |
| Decreased fluoroquinolone susceptibility (DSC) / fluoroquinolone-resistant | Ceftriaxone IV (2 g/day × 10–14 days) or azithromycin (1 g/day × 5 days) | Cefixime |
| XDR (resistant to above + 3rd-gen cephalosporins) | Azithromycin or carbapenems |
- Fluoroquinolone resistance is now predominant in travelers returning from South/Southeast Asia — empiric fluoroquinolone monotherapy is unreliable for these patients
- For severe disease (typhoid encephalopathy/meningitis, shock): add dexamethasone (3 mg/kg IV loading dose, then 1 mg/kg q6h × 48 hours) alongside antibiotics
- Supportive: IV fluid rehydration, blood transfusion if significant GI blood loss
- Relapse occurs in 5–10%, usually milder; re-treat with same antibiotic
Mortality
- Pre-antibiotic era: 10–20%
- With appropriate treatment: <1%
— Harrison's 22E, Tintinalli's Emergency Medicine, CDC
Chronic Carrier State
~1–4% of patients become chronic fecal carriers (excretion >1 year). Chronic carriage is strongly associated with gallstones and gallbladder colonization. Treat with prolonged fluoroquinolones or ampicillin; consider cholecystectomy for refractory cases. Carriers are a source of ongoing community transmission.
Prevention & Vaccination
Two vaccines available (neither 100% effective; food/water precautions still essential):
| Vaccine | Type | Route | Efficacy | Schedule |
|---|---|---|---|---|
| Ty21a (Vivotif) | Live oral attenuated | Oral | ~70% | 4 capsules on alternate days |
| Vi polysaccharide (Typhim Vi) | Conjugated subunit | IM | ~70% | Single dose; booster q2–3 years |
| Typhoid conjugate vaccine (TCV) | Vi-TT conjugate | IM | ~80% | Single dose; now WHO-recommended for children |
- Vaccines do not cover S. Paratyphi — important limitation given rising paratyphoid incidence
- Revaccination required as protection wanes
Key Differentials
- Malaria (exclude first in febrile traveler)
- Dengue fever
- Leptospirosis
- Brucellosis
- Viral hepatitis
- Rickettsial infections
Clinical Pearl: In any traveler returning from South Asia or Africa with fever lasting >10 days, typhoid should be high on the differential. Blood culture is the diagnostic cornerstone. Fluoroquinolone resistance is now so prevalent from the Indian subcontinent that empiric ceftriaxone or azithromycin is preferred pending susceptibility results.
Sources: Harrison's Principles of Internal Medicine 22E (2025) | Tintinalli's Emergency Medicine | Robbins Basic Pathology | Robbins Cotran Pathologic Basis of Disease | Jawetz Melnick & Adelberg's Medical Microbiology 28E | Sleisenger & Fordtran's Gastrointestinal and Liver Disease | CDC Clinical Guidance 2024 | The Lancet Infectious Diseases (2025)
This is a shared conversation. Sign in to Orris to start your own chat.