Hey tell me about herpes zoster
Reading Document
Medical Text Search
herpes zoster etiology pathophysiology clinical presentation diagnosis
Medical Text Search
herpes zoster treatment antiviral management complications postherpetic neuralgia
Medical Image Search
herpes zoster rash dermatomal distribution
GradeResponse
GradeResponse
GradeResponse
Herpes Zoster (Shingles)
Etiology & Pathophysiology
Herpes zoster is caused by the reactivation of varicella-zoster virus (VZV) — the same virus responsible for chickenpox (varicella). After primary varicella infection, VZV establishes latency in the dorsal root ganglia (sensory nerve ganglia). Decades later, when cell-mediated immunity wanes (due to aging, immunosuppression, or stress), the virus reactivates, travels down the sensory nerve, and erupts along the corresponding dermatome.
Restriction endonuclease analysis has confirmed the molecular identity of VZV in both varicella and herpes zoster presentations (Harrison's, p. 5567).
Clinical Presentation
Prodrome (2–4 days before rash)
- Dermatomal pain, burning, or tingling
- Allodynia (sensitivity to touch)
- Mild fever, malaise, headache
- Pain can precede the rash and mimic other conditions (pleurisy, MI, appendicitis)
Acute Phase
- Unilateral, dermatomal vesicular rash — the hallmark finding
- Grouped vesicles on an erythematous base, appearing in crops
- Vesicles progress: clear → hemorrhagic → crusted (over 7–10 days)
- Lesions do not cross the midline
Thoracic dermatomes (T3–L2) are most commonly involved (~50% of cases), followed by the face (cranial nerve V, especially ophthalmic branch — V1)
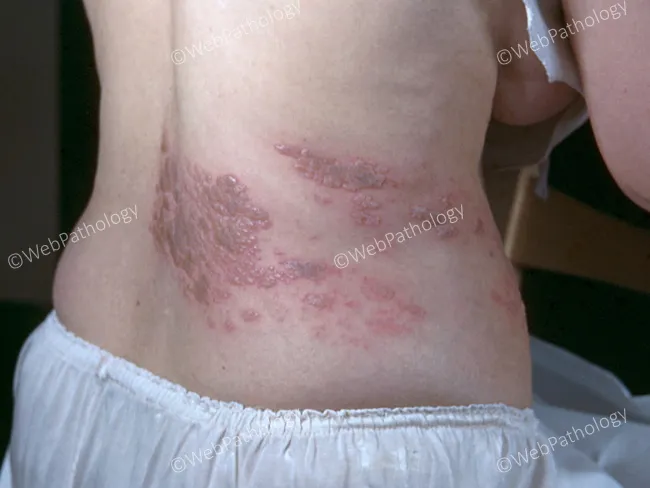
Special Clinical Variants
| Variant | Features |
|---|---|
| Herpes zoster ophthalmicus | V1 involvement; risk of keratitis, uveitis, vision loss |
| Ramsay Hunt syndrome | Geniculate ganglion; ear pain, facial palsy, ear vesicles |
| Zoster sine herpete | Dermatomal pain without rash |
| Disseminated zoster | >20 lesions outside primary dermatome; seen in immunocompromised |
Diagnosis
Usually clinical based on the characteristic dermatomal vesicular rash. When confirmation is needed:
- PCR of vesicular fluid — gold standard
- Tzanck smear — shows multinucleated giant cells (does not distinguish VZV from HSV)
- Direct fluorescent antibody (DFA) testing
- Serology (less useful acutely)
Management
Antiviral Therapy
Start within 72 hours of rash onset for maximum benefit (can still help if new lesions are appearing):
| Drug | Dose | Duration |
|---|---|---|
| Valacyclovir | 1000 mg TID | 7 days |
| Famciclovir | 500 mg TID | 7 days |
| Acyclovir | 800 mg 5x/day | 7–10 days |
Antivirals reduce duration, severity, and risk of postherpetic neuralgia (PHN).
Pain Management
- Mild-moderate: NSAIDs, acetaminophen
- Severe: opioids (short-term)
- Neuropathic adjuncts: gabapentin, pregabalin, amitriptyline, lidocaine patches
Glucocorticoids
Oral prednisone (60 mg/d × 7d → 30 mg/d × 7d → 15 mg/d × 7d) may accelerate return to activity and reduce analgesic use when given early — but only with concomitant antiviral therapy. Not appropriate in patients with diabetes, osteoporosis, hypertension, or glycosuria (Harrison's, p. 5578).
Complications
| Complication | Notes |
|---|---|
| Postherpetic neuralgia (PHN) | Most common; pain persisting >90 days after rash; risk ↑ with age |
| Ocular complications | Keratitis, uveitis, blindness (zoster ophthalmicus) |
| Bacterial superinfection | Secondary skin infection |
| Neurologic | Encephalitis, myelitis, cranial nerve palsies, stroke (VZV vasculopathy) |
| Visceral dissemination | Rare; seen in immunocompromised (pneumonitis, hepatitis) |
Prevention — Vaccination
| Vaccine | Type | Details |
|---|---|---|
| Shingrix (RZV) | Recombinant subunit | Preferred; 2 doses 2–6 months apart; ~97% efficacy in adults ≥50 |
| Zostavax (ZVL) | Live attenuated | Older vaccine; largely replaced by Shingrix; contraindicated in immunocompromised |
Shingrix is recommended for all immunocompetent adults ≥50 years and immunocompromised adults ≥19 years.
Risk Factors for Reactivation
- Advanced age (>50 years)
- HIV/AIDS, malignancy (especially hematologic)
- Immunosuppressive therapy (steroids, chemotherapy, biologics)
- Organ transplant recipients
- Physical/emotional stress