What is galeazzi fracture left
Galeazzi fracture definition classification mechanism treatment
Galeazzi fracture X-ray radiograph
Galeazzi Fracture
Mechanism of Injury
- Most commonly caused by a fall on an outstretched hand (FOOSH) with the forearm in forced pronation
- Can also result from direct trauma to the dorsolateral wrist/forearm
- The distal radial fragment typically displaces dorsally and proximally, while the ulnar head dislocates dorsally relative to the radius
Classification (Mansat / Rettig & Raskin)
| Type | Description |
|---|---|
| Type I | Fracture at the junction of the middle and distal thirds of the radius |
| Type II | Fracture within 7.5 cm of the radiocarpal joint; higher risk of DRUJ instability |
Radiographic Findings
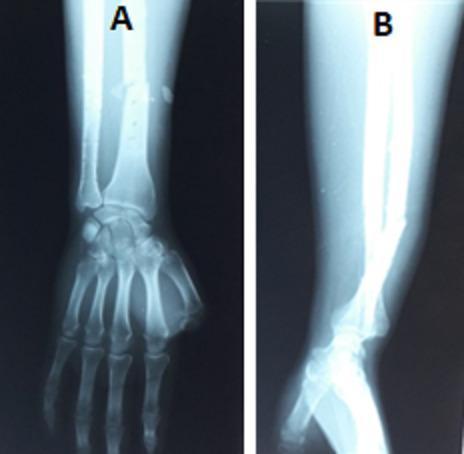
- Radial shaft fracture, typically at the distal third
- Widened DRUJ on AP view (>2 mm gap between radius and ulna at the wrist)
- Dorsal dislocation of the ulnar head on lateral view
- Radial shortening
- Possible avulsion of the ulnar styloid
Clinical Presentation
- Pain, swelling, and deformity of the distal forearm and wrist
- Prominent ulnar head on the dorsum of the wrist (piano key sign)
- Limited and painful forearm rotation
- Tenderness over the DRUJ
Management
- Open reduction and internal fixation (ORIF) of the radial shaft with a 3.5 mm dynamic compression plate (DCP)
- Assess DRUJ stability intraoperatively after radius fixation:
- Stable DRUJ → long-arm cast in supination for 4–6 weeks
- Unstable DRUJ → repair of the triangular fibrocartilage complex (TFCC) ± percutaneous Kirschner wire (K-wire) across the DRUJ in supination
- Closed reduction + long-arm cast (due to remodeling potential)
- Surgical fixation if reduction is unsatisfactory
Complications
| Complication | Notes |
|---|---|
| DRUJ instability (chronic) | Most common if DRUJ disruption is missed |
| Malunion / radial shortening | Leads to wrist pain and restricted rotation |
| Nerve injury | Posterior interosseous nerve (PIN) at risk |
| Compartment syndrome | Rare but possible |
| Re-fracture (children) | If cast removed too early |
Key Teaching Point
- Galeazzi = Genitalia (distal — DRUJ disruption)
- Monteggia = Mouth (proximal — radial head dislocation)
Please explain this CT scan ... Is there any abnormalities?
brain CT scan hemorrhage abnormality interpretation
brain CT scan interpretation hemorrhage infarct mass effect midline shift
CT Brain Analysis — Patient: Azizul Islam, 70 years
⚠️ Disclaimer: This is an AI-assisted educational interpretation only. It does not replace formal radiologist reporting or clinical decision-making by a qualified physician.
Patient Details (from film header)
- Patient: Azizul Islam
- Age: 70 years
- Institution: Dhaka Medical College
- Scan type: Non-contrast CT Brain (NCCT), axial cuts from skull base to vertex
Systematic Review
- Continued presence of the posterior fossa hyperdensity
- The ventricular system appears enlarged — the temporal horns and lateral ventricles look dilated, raising concern for obstructive hydrocephalus (likely secondary to the posterior fossa lesion compressing the 4th ventricle/aqueduct)
- There may be periventricular hypodensity suggesting transependymal CSF flow (a sign of raised intracranial pressure)
- Bilateral lateral ventricles are dilated
- Small hyperdense foci are visible near the choroid plexus / thalamic region — could represent calcifications or intraventricular hemorrhage
- Brain parenchyma appears relatively symmetric at this level
- Diffuse cortical atrophy consistent with age (70 years) — widened sulci, prominent CSF spaces
- No obvious focal infarct or large parenchymal bleed at these levels
- White matter appears somewhat hypodense diffusely — may suggest leukoaraiosis (small vessel disease)
Summary of Abnormalities
| Finding | Location | Significance |
|---|---|---|
| Large hyperdense lesion | Posterior fossa / cerebellum | Likely cerebellar hemorrhage or mass — critical finding |
| Hydrocephalus | Lateral ventricles bilaterally enlarged | Likely obstructive — secondary to posterior fossa lesion |
| Leukoaraiosis | Periventricular white matter | Chronic small vessel cerebrovascular disease |
| Cerebral atrophy | Diffuse | Age-related (70 years), likely chronic |
| Possible intraventricular blood / calcification | Near choroid plexus | Needs correlation |
Clinical Impression
- Cerebellar hemorrhage (most likely) — a neurosurgical emergency
- Hemorrhagic cerebellar infarct
- Posterior fossa tumor with hemorrhage (less acute)
Urgent Recommendations
- Immediate neurosurgical consultation — posterior fossa hemorrhage with hydrocephalus can rapidly cause brainstem compression and herniation
- Urgent repeat imaging or MRI brain with contrast for better characterization
- Monitor for signs of raised ICP: deteriorating GCS, Cushing's triad (bradycardia, hypertension, irregular breathing)
- Consider external ventricular drain (EVD) if hydrocephalus is symptomatic
Could I hold Ecosprin or not ?
Ecosprin aspirin hold withhold intracranial hemorrhage cerebellar hemorrhage management
antiplatelet therapy aspirin discontinuation intracerebral hemorrhage guidelines
Should Ecosprin (Aspirin) Be Held?
Why Hold It?
- Inhibits platelet aggregation irreversibly (for the platelet's lifetime, ~7–10 days)
- Continuing it risks hematoma expansion — the single most important determinant of poor outcome in intracerebral hemorrhage
- Can make any surgical intervention (evacuation, EVD placement) more dangerous by increasing bleeding risk
Immediate Actions Regarding Ecosprin
| Action | Detail |
|---|---|
| Hold Ecosprin now | Do not give the next dose |
| Note indication | Was it for secondary stroke prevention, cardiac, or other? |
| Platelet transfusion | Generally NOT recommended routinely for aspirin-related ICH (AHA/ASA 2022 guidelines) unless patient is going to surgery |
| Reversal | No specific reversal agent for aspirin — supportive management |
When Can Aspirin Be Restarted?
- If hemorrhage was spontaneous (hypertensive): restart is typically considered at 4–8 weeks only if there is a compelling indication (e.g., recent coronary stent, high-risk cardiac condition)
- If no strong indication existed: may not need to restart at all
- Decision must weigh: risk of hematoma re-expansion vs. thromboembolic risk (e.g., cardiac stent, prior MI, AF)
Bottom line: In the context of this CT showing active intracranial hemorrhage, Ecosprin must be held. Resumption should only be decided by the treating neurosurgeon/neurologist based on clinical course and underlying indication.
In row 1 is it hyperdense due to haemorrhage or bone ?
CT brain posterior fossa skull base hyperdensity bone artifact petrous bone cerebellum interpretation
Row 1 Hyperdensity — Bone or Hemorrhage?
The honest answer: Likely predominantly bone at the skull base level, BUT with a superimposed suspicious hyperdense lesion in the cerebellar region.
How to Distinguish
| Feature | Bone / Artifact | True Hemorrhage |
|---|---|---|
| Location | Follows skull contour, petrous ridges, clivus | Within brain parenchyma, away from bone |
| Shape | Linear, symmetric, follows skull base anatomy | Rounded, irregular, asymmetric |
| Density (HU) | Very bright white — >300–400 HU (cortical bone) | Moderately bright — 50–80 HU (acute blood) |
| Symmetry | Bilateral and symmetric (petrous bones) | Usually unilateral or asymmetric |
| Edges | Sharp, geometric | Less defined, may have surrounding hypodensity (edema) |
Specifically in This CT (Row 1)
- The outer bright white rim = calvarium/skull bone — this is normal
- The petrous ridges bilaterally appearing bright = normal bone
- However, the central posterior fossa region (cerebellum) has a hyperdense area that does NOT follow the symmetric bone pattern — this is what raises concern for true hemorrhage
"CT may fail to show small ischemic strokes in the posterior fossa because of bone artifact" — Harrison's (p. 12118)
Conclusion
- The symmetric bright areas along the periphery and skull base in Row 1 = bone (normal)
- The central/asymmetric hyperdensity within the cerebellar parenchyma = hemorrhage until proven otherwise
- The fact that this hyperdensity persists on higher cuts (Row 2) where bone artifact is less prominent strongly supports it being true cerebellar hemorrhage, not just artifact
In row 3 3rd picture is there any signs of haemorrhage
basal ganglia thalamic hemorrhage CT hyperdensity signs internal capsule
Row 3, 3rd Image — Hemorrhage Analysis
What Is Visible
Is It Hemorrhage?
| Possibility | Features Supporting It |
|---|---|
| Choroid plexus calcification | Bilateral, symmetric, very small, well-defined — extremely common incidental finding, especially in a 70-year-old |
| Intraventricular hemorrhage (IVH) | If hyperdensity is within the ventricular lumen rather than the parenchyma, blood can settle in the ventricles secondary to the posterior fossa bleed |
Key Distinguishing Points
- If symmetric and pinpoint → most likely normal choroid plexus calcification (benign, age-related)
- If filling the ventricular space / asymmetric / irregular → suggests intraventricular extension of hemorrhage
- The dilated ventricles seen in this row further support that the posterior fossa bleed may be causing obstructive hydrocephalus with possible IVH
Clinical Significance
- It can block CSF drainage further at multiple levels
- Indicates more severe hemorrhage with ventricular rupture
- May require external ventricular drain (EVD) urgently
Bottom Line
The small hyperdense foci in Row 3, image 3 are likely choroid plexus calcifications, but intraventricular hemorrhage cannot be excluded given the overall clinical picture. A thin-cut posterior fossa CT or MRI is needed to differentiate with certainty.