I have a case presentation on case of thyroid swelling (ENT), teach me full case history, presentation, probable viva questions and its answers, management, differentiatial diagnosis of midline neck swelling, and reasons of each and everything
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
thyroid goiter neck swelling examination
I now have comprehensive information. Let me compile the full case presentation guide.
🏥 Thyroid Swelling — Complete Case Presentation Guide (ENT)
📋 PART 1: FULL CASE HISTORY
Biodata
- Name, Age, Sex, Occupation, Address, Religion
- Key pointers: Female > Male (4:1), any age, but common 30–50 years
Presenting Complaint
"Swelling in front of the neck for ___ months/years"
Always note:
- Duration — sudden vs. gradual
- Progression — increasing, static, decreasing
History of Presenting Complaint (HOPI)
Ask about the swelling systematically using SOCRATES:
| Parameter | Key Questions |
|---|---|
| Site | Midline or lateral? Upper, middle, lower neck? |
| Onset | Sudden or gradual? Any precipitating event? |
| Character | Painful or painless? Soft, firm, hard? |
| Radiation | Does it extend behind the sternum? |
| Associated symptoms | See below |
| Timing | Constant or intermittent? |
| Exacerbating/relieving | Does it increase on coughing? |
| Severity | Cosmetic only, or compressive symptoms? |
Associated Symptoms — Compressive
| Symptom | Structure Compressed |
|---|---|
| Dysphagia | Esophagus |
| Dyspnea / stridor | Trachea |
| Hoarseness of voice | Recurrent laryngeal nerve |
| Facial plethora / venous distension | Jugular veins (Pemberton's sign) |
| Homer's syndrome (ptosis, miosis, anhidrosis) | Cervical sympathetic chain |
Associated Symptoms — Thyroid Status (MUST ask)
Symptoms of Hyperthyroidism:
- Weight loss despite good appetite
- Palpitations / fast heartbeat
- Heat intolerance, excessive sweating
- Tremor of hands
- Diarrhea, frequent bowel motions
- Irritability, anxiety, emotional lability
- Oligomenorrhea / amenorrhea
- Eye symptoms: protrusion, double vision, grittiness (suggests Graves' disease)
Symptoms of Hypothyroidism:
- Weight gain
- Cold intolerance
- Constipation
- Dry skin, coarse hair, hair loss
- Bradycardia, lethargy
- Menorrhagia
- Hoarseness of voice
Symptoms of Malignancy (Red Flags):
- Rapid increase in size
- Hard, fixed swelling
- Hoarseness (RLN invasion)
- Dysphagia
- Cervical lymph node enlargement
- Previous head and neck irradiation
Past History
- Previous thyroid disease or surgery
- History of radiation to neck/head in childhood
- Iodine-deficient area (endemic goitre)
Family History
- Goitre, thyroid cancer
- MEN syndrome (MEN 2A/2B — associated with medullary thyroid carcinoma)
- Autoimmune thyroid disease
Drug History
- Lithium (causes goitre/hypothyroidism)
- Amiodarone (iodine-rich, affects thyroid)
- Antithyroid drugs (prior use)
- Oral contraceptive pill
Dietary / Social History
- Iodine intake, cruciferous vegetable excess
- Smoking (mildly protective against autoimmune thyroiditis but risk for thyroid cancer)
- Residence in endemic goitre area
Menstrual History (in females)
- Changes in cycle — suggests thyroid dysfunction
🔍 PART 2: CLINICAL EXAMINATION
General Appearance
- Eyes: Exophthalmos, lid lag, lid retraction, chemosis, ophthalmoplegia → Graves' disease
- Hands: Fine tremor, warm moist palms, thyroid acropachy, onycholysis (hyperthyroidism); dry, cold, bradycardia (hypothyroidism)
- Pulse: Tachycardia / atrial fibrillation (hyperthyroidism)
- Pretibial myxedema (Graves' disease — bilateral shin deposits)
Examination of the Neck Swelling
Inspection
- Position of swelling — midline, anterior, submandibular
- Shape and size
- Skin over swelling — normal, inflamed, dilated veins, scars
- Movement with swallowing → HALLMARK of thyroid swelling — moves upward on swallowing (attached to pretracheal fascia)
- Movement with tongue protrusion → moves on tongue protrusion = thyroglossal duct cyst (NOT thyroid gland)
- Visible pulsations
- Pemberton's sign — patient raises both arms above head: facial congestion and stridor = substernal goitre
Palpation (stand behind patient, offer water to swallow)
- Confirm movement with swallowing
- Surface: Smooth (diffuse goitre, Graves') vs. nodular (multinodular goitre, adenoma, malignancy)
- Consistency: Soft (colloid), firm (Hashimoto's, follicular), hard/stony (malignancy, calcification, Riedel's)
- Tenderness: Suggests De Quervain's thyroiditis, acute thyroiditis
- Extent: Below sternum? (bimanual, feel at jugular notch)
- Trachea — central or deviated?
- Regional lymph nodes — cervical chain, level I–VI
- Berry's sign — loss of pulsation of carotid artery behind goitre = malignant invasion
Percussion
- Dullness below sternum → substernal extension
Auscultation
- Bruit over thyroid → Graves' disease (hypervascular, continuous bruit)
🩺 PART 3: DIFFERENTIAL DIAGNOSIS OF MIDLINE NECK SWELLING
| Condition | Age | Key Feature | Moves with Swallowing | Moves with Tongue Protrusion |
|---|---|---|---|---|
| Goitre (thyroid) | Any | Most common midline neck swelling | ✅ Yes | ❌ No |
| Thyroglossal duct cyst | Child/young adult | Midline, between hyoid & thyroid | ✅ Yes (if below hyoid) | ✅ Yes |
| Sublingual dermoid cyst | Young | Soft, cystic, below chin | ❌ No | ❌ No |
| Subhyoid bursa | Adult | Cystic, at hyoid level | ✅ Slight | ❌ No |
| Lymph node (midline) | Any | Secondary to infection/malignancy | ❌ No | ❌ No |
| Lipoma | Middle age | Soft, lobulated, transilluminates | ❌ No | ❌ No |
| Sebaceous cyst | Adult | Pit/punctum visible, attached to skin | ❌ No | ❌ No |
| Ludwig's angina | Adult | Indurated floor of mouth, toxic | ❌ No | ❌ No |
| Ectopic thyroid | Female, young | No normal thyroid palpable | ✅ May | ✅ May |
| Delphian (prelaryngeal) lymph node | Adult | Firm, in midline anterior larynx | ❌ No | ❌ No |
| Pretracheal lymph node | Any | Firm, near thyroid isthmus | ❌ No | ❌ No |
| Aneurysm | Elderly | Pulsatile, expansile | ❌ No | ❌ No |
Why Thyroid Swelling Moves with Swallowing
The thyroid gland is enclosed within the pretracheal fascia, which is attached to the larynx and trachea. On swallowing, the larynx and trachea move superiorly → the thyroid moves with them. This is the single most important physical sign distinguishing thyroid from non-thyroid swellings.
Why Thyroglossal Cyst Also Moves with Swallowing AND Tongue Protrusion
The thyroglossal duct descends from the foramen cecum at the base of tongue → along midline → to pyramidal lobe of thyroid. It is tethered to the hyoid bone. Tongue protrusion pulls the hyoid upward (via geniohyoid), dragging the cyst superiorly. Below the hyoid, it also moves with swallowing due to fascial connections. (Source: K.J. Lee's Essential Otolaryngology)
⚗️ PART 4: INVESTIGATIONS
Baseline
| Investigation | Purpose |
|---|---|
| Serum TSH | First-line thyroid function screen (most sensitive) |
| Free T3, Free T4 | Confirm hyper/hypothyroidism |
| Anti-TPO, Anti-Tg antibodies | Hashimoto's, Graves' |
| TSH receptor antibodies (TRAb) | Confirms Graves' disease |
| Serum calcium | Hypercalcaemia → consider parathyroid |
| Calcitonin | Medullary thyroid carcinoma screen |
| Urinary iodine | <50 µg/L = iodine deficiency |
Imaging
| Investigation | Purpose |
|---|---|
| Ultrasound neck | First-line imaging; defines nodule characteristics, guides FNAC; rules out ectopic thyroid (before thyroglossal cyst surgery) |
| FNAC (Fine Needle Aspiration Cytology) | Bethesda classification of nodules; gold standard for cytology |
| Radionuclide scan (Tc-99m / I-131) | Hot vs. cold nodule; hot = functional/toxic; cold = higher malignancy risk (5–15%); ectopic thyroid |
| CT neck/thorax | Substernal extension, tracheal compression, lymph node mapping |
| MRI | Vascular invasion, retrosternal assessment |
| Chest X-ray | Tracheal deviation, mediastinal widening, calcification |
| Barium swallow | Oesophageal compression |
💊 PART 5: MANAGEMENT
Medical Management
1. Euthyroid Goitre (Simple/Endemic):
- Iodine supplementation (iodine-deficient areas)
- Monitor with TFTs and USS
- Levothyroxine (TSH suppression) — rarely used now due to risk of thyrotoxicosis
2. Graves' Disease (Toxic Diffuse Goitre):
- Antithyroid drugs (ATDs): Carbimazole (first-line) or Propylthiouracil (PTU — pregnancy first trimester)
- Mechanism: Inhibit thyroid peroxidase → block hormone synthesis; PTU also inhibits peripheral T4→T3 conversion
- Beta-blockers (Propranolol): Symptom control (palpitations, tremor) while awaiting ATD effect
- Radioactive Iodine (RAI / I-131): Definitive; ablates thyroid tissue; contraindicated in pregnancy, active ophthalmopathy
- Surgery (total/subtotal thyroidectomy): Large goitre causing compression, failed medical, patient preference
3. Toxic Multinodular Goitre (Plummer's Disease):
- RAI preferred in elderly
- Surgery for large compressive MNG
4. Hypothyroidism (Hashimoto's):
- Levothyroxine replacement (T4)
5. Malignancy: See below
Surgical Management
Indications for Surgery
- Compressive symptoms (dysphagia, dyspnea, stridor)
- Cosmesis
- Malignancy (proven or suspected — FNAC Bethesda IV/V/VI)
- Failed medical therapy
- Toxic goitre — contraindication to RAI (e.g., pregnancy, active eye disease)
- Substernal goitre
Types of Thyroid Surgery
| Procedure | Indication |
|---|---|
| Hemithyroidectomy (lobectomy) | Solitary nodule, indeterminate FNAC (Bethesda III/IV) |
| Subtotal thyroidectomy | Bilateral non-toxic MNG, Graves' (some centres) |
| Near-total thyroidectomy | Differentiated thyroid cancer (DTC), bilateral MNG |
| Total thyroidectomy | DTC, medullary thyroid carcinoma, bilateral Graves' |
| Sistrunk procedure | Thyroglossal duct cyst — resect cyst + tract + middle third of hyoid bone |
Post-operative Complications
| Complication | Notes |
|---|---|
| Recurrent laryngeal nerve (RLN) injury | Unilateral: hoarseness; Bilateral: stridor, tracheostomy needed |
| Hypoparathyroidism | Hypocalcaemia → tetany, Chvostek's / Trousseau's sign |
| Haemorrhage / haematoma | Life-threatening — reopen wound immediately |
| Hypothyroidism | Near-total/total thyroidectomy → lifelong levothyroxine |
| Thyroid storm | In unprepared hyperthyroid patient |
| Wound infection / keloid | Rare |
Management of Thyroid Carcinoma
| Type | Features | Management |
|---|---|---|
| Papillary (most common, ~80%) | Psammoma bodies, Orphan Annie nuclei, slow growing | Total thyroidectomy ± central neck dissection + RAI ablation + LT4 suppression |
| Follicular (~10%) | Hematogenous spread, encapsulated, older patients | Total thyroidectomy + RAI |
| Medullary (~5%) | Calcitonin-secreting, amyloid stroma, associated with MEN 2 | Total thyroidectomy + central neck dissection; no RAI |
| Anaplastic (<5%) | Rapidly fatal, elderly, stony hard fixed mass | Palliative; XRT/chemotherapy; occasionally debulking |
🎓 PART 6: PROBABLE VIVA QUESTIONS & ANSWERS
Q1. What is the single most important physical sign in a thyroid swelling?
A: Movement with swallowing. The thyroid gland is invested by the pretracheal fascia attached to the trachea and larynx, so it ascends with laryngeal elevation during swallowing.
Q2. How do you distinguish a thyroglossal cyst from a thyroid swelling clinically?
A: Both move with swallowing (below hyoid), but a thyroglossal cyst also moves with tongue protrusion — because it is tethered to the hyoid bone via the residual thyroglossal tract, and tongue protrusion elevates the hyoid via the geniohyoid muscle.
Q3. What is the Sistrunk procedure?
A: Surgical excision of a thyroglossal duct cyst, involving: (1) removal of the cyst and its entire tract, (2) resection of the central/middle third of the hyoid bone, and (3) a cuff of tongue base musculature up to the foramen cecum. The hyoid is removed because the duct branches extensively around it (especially above), and failure to remove it leads to high recurrence. (K.J. Lee's Essential Otolaryngology)
Q4. Why is the hyoid bone removed in a Sistrunk procedure?
A: The thyroglossal duct has extensive branching around and above the hyoid bone. Leaving hyoid remnants leads to recurrence of the cyst. Resecting the middle third of the hyoid ensures complete clearance of the tract.
Q5. What is Pemberton's sign?
A: When the patient raises both arms above the head, facial congestion, neck vein engorgement, and stridor develop due to thoracic inlet obstruction by a substernal goitre compressing the superior vena cava or thoracic inlet.
Q6. What is Berry's sign?
A: Loss of carotid pulsation palpable behind a goitre, indicating malignant encasement and invasion of the carotid artery.
Q7. What is the first-line investigation for thyroid function?
A: Serum TSH is the most sensitive single test. Suppressed TSH = hyperthyroidism; elevated TSH = hypothyroidism. Free T3 and T4 are then measured to assess the degree of dysfunction.
Q8. What is a "cold nodule" and why is it significant?
A: On radionuclide scanning, a cold nodule shows absent/reduced isotope uptake relative to normal thyroid tissue. It carries a 5–15% risk of malignancy, significantly higher than hot nodules (which are rarely malignant). Cold nodules require FNAC for cytological evaluation. (Swanson's Family Medicine Review)
Q9. What is the Bethesda classification?
A: A 6-tier cytological classification system for FNAC of thyroid nodules:
- I: Non-diagnostic
- II: Benign
- III: Atypia of undetermined significance (AUS)
- IV: Follicular neoplasm
- V: Suspicious for malignancy
- VI: Malignant
Q10. What nerve is at risk in thyroid surgery, and what happens if it is injured?
A: The Recurrent Laryngeal Nerve (RLN). It lies in the tracheoesophageal groove and must be identified and preserved. Unilateral damage causes hoarseness; bilateral damage causes bilateral vocal cord palsy, presenting as stridor and potentially requiring emergency tracheostomy. The external branch of the superior laryngeal nerve is also at risk, causing loss of high-pitched voice projection.
Q11. What are the complications of total thyroidectomy?
A:
- RLN injury → hoarseness / stridor
- Hypoparathyroidism → hypocalcaemia → tetany → Chvostek's/Trousseau's signs
- Haemorrhage / haematoma → can cause acute airway compression
- Hypothyroidism → lifelong LT4 required
- Thyroid storm (if unprepared hyperthyroid patient)
- Wound infection, keloid scar
Q12. What is Graves' disease, and how is it diagnosed?
A: Graves' disease is an autoimmune condition where TSH receptor antibodies (TRAb/TSI) stimulate the TSH receptor → diffuse goitre with hyperthyroidism. Classic triad: diffuse toxic goitre + exophthalmos + pretibial myxedema (not all need be present). Confirmed by suppressed TSH, elevated fT3/fT4, positive TRAb, and homogeneous goitre on USS with increased vascularity (thyroid "inferno" on Doppler).
Q13. What is De Quervain's (subacute) thyroiditis?
A: Subacute granulomatous thyroiditis, probably viral (post-URI). Presents with painful, tender thyroid, low-grade fever, raised ESR. TFTs show initial hyperthyroidism (release of preformed hormones) → hypothyroid phase → recovery. Treated with NSAIDs (mild) or corticosteroids (severe).
Q14. Name the types of goitre.
A:
- Physiological: puberty, pregnancy (increased iodine demand)
- Endemic: iodine deficiency (>5% population)
- Sporadic: non-endemic, unknown cause
- Toxic diffuse: Graves' disease
- Toxic nodular: toxic adenoma, Plummer's disease (toxic MNG)
- Non-toxic MNG: most common type overall
- Autoimmune: Hashimoto's (hypothyroid), Graves' (hyperthyroid)
- Neoplastic: adenoma, carcinoma
Q15. What is WHO grading of goitre?
A:
- Grade 0: No palpable/visible goitre
- Grade 1: Palpable but not visible with neck in normal position
- Grade 2: Visible with neck in normal position; not visible when head extended
- Grade 3 (old classification): Visible at a distance
Q16. What are the indications for FNAC?
A: Any thyroid nodule >1 cm on USS, or smaller nodules with suspicious sonographic features (hypoechoic, irregular margins, microcalcifications, taller-than-wide shape, abnormal vascularity, extrathyroidal extension, suspicious LN). ACR TI-RADS guides size thresholds for biopsy. (Harrison's 22e)
Q17. What is the TI-RADS system?
A: The ACR Thyroid Imaging Reporting and Data System — a 5-tiered scoring system (TI-RADS 1–5) categorizing sonographic features of thyroid nodules by composition, echogenicity, shape, margins, and echogenic foci. Higher TI-RADS = higher malignancy risk → lower size threshold for FNAC. (Harrison's 22e)
Q18. Why does goitre develop in iodine deficiency?
A: Iodine deficiency → reduced efficiency of thyroid hormone synthesis → compensatory rise in TSH → TSH stimulates thyroid cell proliferation and growth → goitre. TSH is sometimes only mildly elevated, suggesting increased tissue sensitivity to TSH and activation of alternate local growth pathways (endothelins, nitric oxide). (Harrison's 22e)
Q19. What is Hashimoto's thyroiditis?
A: Autoimmune thyroiditis with lymphocytic infiltration and destruction of thyroid tissue. Anti-TPO and anti-Tg antibodies are positive. Initially may cause transient thyrotoxicosis (Hashitoxicosis), but usually leads to hypothyroidism. Goitre may or may not be present. Associated with other autoimmune diseases (DM Type 1, Addison's, vitiligo).
Q20. What is the diagnostic approach to a solitary thyroid nodule?
A:
- History and clinical exam — assess for hyper/hypothyroidism, malignancy risk factors
- Serum TSH — if suppressed → radionuclide scan (hot nodule = autonomous adenoma, rarely malignant)
- Ultrasound — characterize nodule (TI-RADS scoring)
- FNAC — for nodules meeting size/sonographic criteria (Bethesda classification)
- Additional: CT if substernal, calcitonin if medullary suspected
📸 Clinical Images
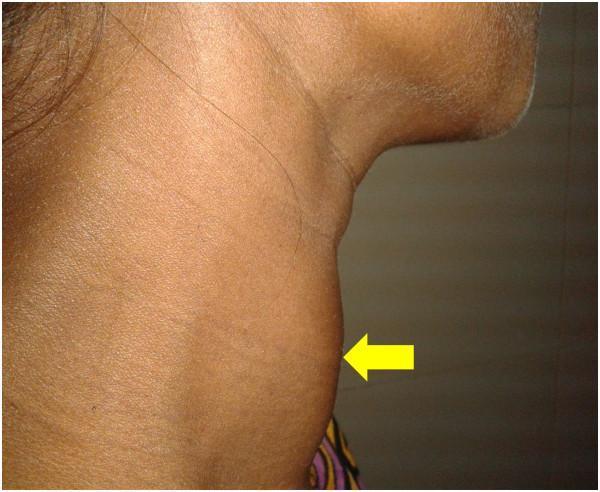
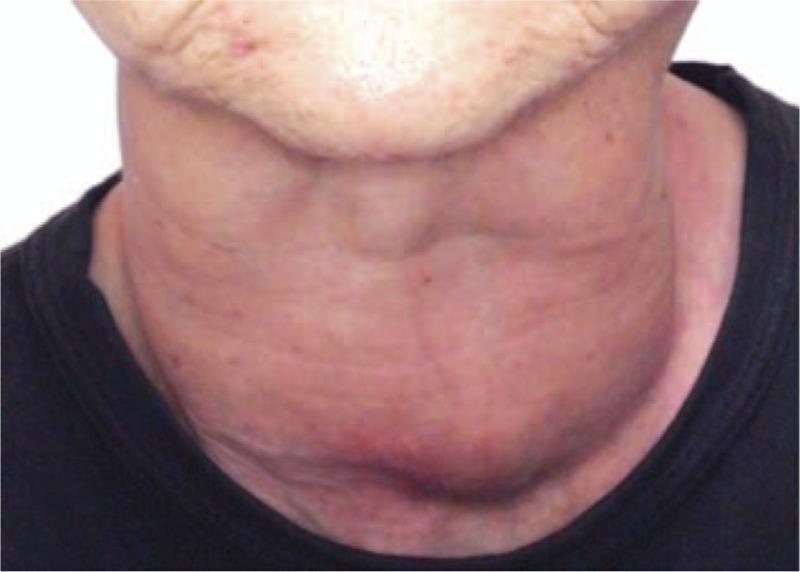
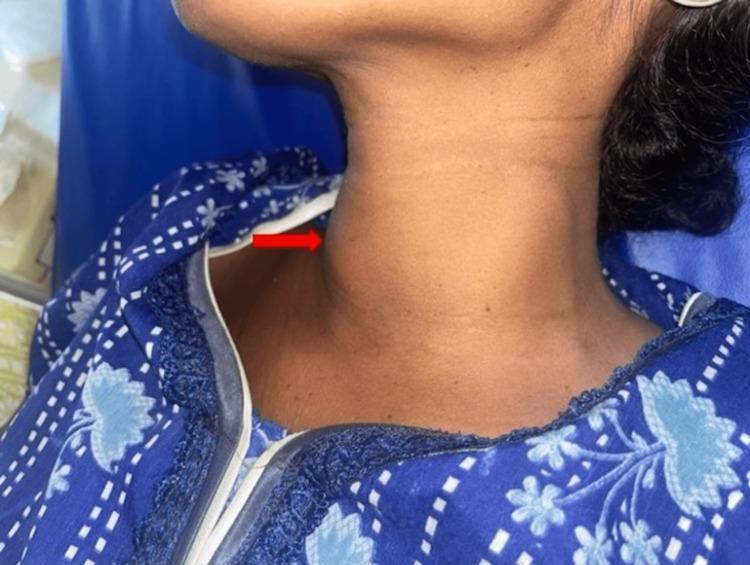
🗂️ QUICK SUMMARY CARD FOR PRESENTATION
| Feature | Thyroid Goitre |
|---|---|
| Location | Midline/anterior neck |
| Movement with swallowing | ✅ YES (pathognomonic) |
| Movement with tongue protrusion | ❌ NO (distinguishes from thyroglossal cyst) |
| First investigation | TSH |
| First imaging | USS neck |
| Gold standard cytology | FNAC (Bethesda) |
| Surgery for cancer | Total thyroidectomy |
| Surgery for thyroglossal cyst | Sistrunk procedure |
| Bruit | Graves' disease |
| Hard fixed + hoarse voice | Malignancy until proven otherwise |
Sources: Harrison's Principles of Internal Medicine 22e; K.J. Lee's Essential Otolaryngology; Current Surgical Therapy 14e; Cummings Otolaryngology Head and Neck Surgery
This is a shared conversation. Sign in to Orris to start your own chat.