Adult still disease
Reading File
Finding Sources
Finding Sources
Searching PubMed
"adult-onset Still disease"[MeSH Terms]
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Loading Image
Finding Sources
I now have comprehensive information to deliver a thorough answer on Adult-onset Still's Disease (AOSD).
Adult-Onset Still's Disease (AOSD)
Adult-onset Still's disease is a rare systemic autoinflammatory disorder characterized by the classic triad of quotidian spiking fevers, polyarthritis, and an evanescent salmon-pink rash. It is the adult counterpart of systemic juvenile idiopathic arthritis (sJIA).
Epidemiology
- Predominantly affects young adults (mean age at onset ~42 years in large series); onset before age 30 is most common, rarely over 60
- Women > men (61% female in largest combined series)
- Incidence: ~0.16–0.34 per 100,000 (France/Japan data)
- Average diagnostic delay: ~2.3 months
— Fitzpatrick's Dermatology, Vol. 1–2
Pathogenesis
The etiology is unknown, but the disease behaves as a reactive autoinflammatory syndrome in a genetically susceptible host, likely triggered by infectious agents (enteroviruses, herpesviruses, organisms causing pneumonia/enterocolitis — none implicated consistently).
Key cytokines driving inflammation:
- IL-1β, IL-6, IL-18, TNF-α, IFN-γ — all markedly elevated
- HLA associations suggest a genetic predisposition
- Overlap with sJIA pathogenesis is significant
— Dermatology 2-Volume Set 5e (Bolognija)
Clinical Features
Frequency of signs/symptoms (cumulative series of 731 patients):
| Feature | Frequency |
|---|---|
| Fever ≥39°C | 93% |
| Arthralgia/arthritis | 90% |
| Skin rash | 70% |
| Sore throat | 64% |
| Lymphadenopathy/splenomegaly | 53% |
| Hepatomegaly | 39% |
| Pericarditis | 13% |
| Myalgia | 35–44% |
Fever: 1–2 daily spikes > 39°C (102.2°F), classically in the late afternoon or evening, resolving within hours (quotidian pattern).
Rash: Asymptomatic, salmon-pink macules/slightly edematous papules (5–10 mm), favoring the trunk and extensor surfaces. Crucially, it appears with fever spikes and disappears as fever resolves. It may show the Koebner phenomenon. Atypical persistent lesions (violaceous scaly plaques, flagellate erythema, eyelid edema) are associated with worse prognosis and can mimic dermatomyositis.
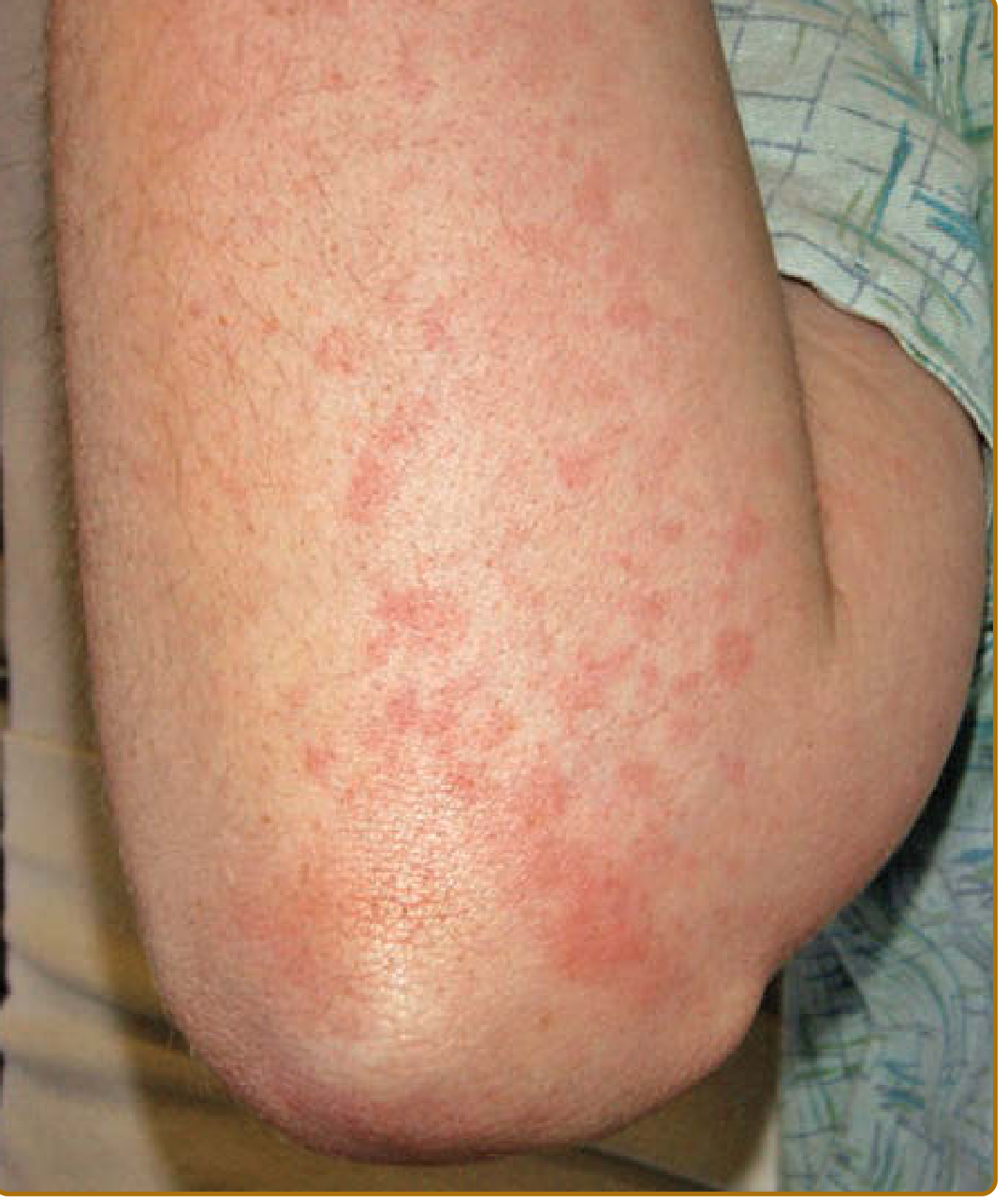
Arthritis: Symmetric, affecting knees, wrists, and ankles most often. A distinctive feature is carpal ankylosis (limited range of motion with minimal pain). The MCP joints are typically spared. Similar ankylosis can occur in PIP/DIP joints and the cervical spine.
Disease course:
- Monocyclic: 24–30%
- Polycyclic (intermittent): 41–44%
- Chronic articular: 26–36%
Laboratory Findings
| Test | Finding |
|---|---|
| Serum ferritin | Markedly elevated; often >4,000 ng/mL, can be >50,000 |
| Glycosylated ferritin fraction | <20% (normally 50–80%) — highly characteristic |
| Leukocytosis | 85% of patients; ≥80% PMNs in 69% |
| CRP | Elevated in 93% |
| ESR | Elevated in 85% |
| Liver enzymes | Elevated in 62% |
| Thrombocytosis | 46% |
| Anemia (<10 g/dL) | 50–75% |
| ANA, RF, anti-CCP | Negative or low-titer (characteristic) |
Pearl: The combination of very high ferritin + glycosylated ferritin fraction <20% is the most diagnostically useful lab finding, though not pathognomonic.
— Fitzpatrick's Dermatology
Classification Criteria
Two validated systems are used clinically:
Yamaguchi Criteria (1992)
Requires ≥5 criteria, ≥2 major + exclusion of infections/malignancy/other inflammatory disease:
Major:
- Fever ≥39°C lasting ≥1 week
- Arthralgia ≥2 weeks
- Typical salmon-pink maculopapular rash with concomitant fever
- Leukocytosis ≥10,000/mm³ with ≥80% PMNs
Minor:
- Pharyngitis/sore throat
- Lymphadenopathy and/or splenomegaly
- Elevated liver enzymes
- Negative RF and ANA
Fautrel Criteria (2002)
4 major OR 3 major + 2 minor (no exclusion criteria required):
Major: Spiking fever ≥39°C, arthralgia, transient erythema, pharyngitis, PMNs ≥80%, glycosylated ferritin ≤20%
Minor: Typical rash, leukocytosis >10,000/mm³
— Fitzpatrick's Dermatology
Complications
Macrophage Activation Syndrome (MAS) / Hemophagocytic Lymphohistiocytosis (HLH)
The most feared and potentially life-threatening complication. MAS (secondary HLH) occurs most commonly with sJIA and AOSD. It presents with worsening cytopenias, hyperferritinemia, coagulopathy, and multiorgan failure.
Cardiac: Pericarditis in up to 50% of patients; rare cardiac tamponade and myocarditis.
Other systemic: Pleuritis, pleural effusions, pulmonary fibrosis, pulmonary arterial hypertension, nephritis.
Malignancy association: Atypical cutaneous presentations have been associated with delayed or concurrent malignancy.
— Dermatology 2-Volume Set 5e; Fuster and Hurst's The Heart, 15e; Fitzpatrick's Dermatology
Histopathology
The classical evanescent rash shows:
- Mild mixed perivascular and interstitial infiltrate (lymphocytic, neutrophilic, occasionally eosinophilic) in the upper dermis
- Basal vacuolization and keratinocyte necrosis
- Mucin in the dermis
Persistent (atypical) lesions show epidermal changes: acanthosis, spongiosis, necrotic keratinocytes in the spinous layer — findings that can overlap with dermatomyositis.
Differential Diagnosis
| Condition | Distinguishing features |
|---|---|
| Sepsis / infection (EBV, enteroviral) | Must exclude first (Yamaguchi exclusion criterion) |
| Lymphoma | Paraneoplastic AOSD-like syndromes documented |
| Schnitzler syndrome | Non-pruritic urticaria + monoclonal IgM + bone pain (hyperostosis) |
| Dermatomyositis | Myositis, dermatomyositis-specific autoantibodies, interface dermatitis on biopsy |
| SLE | ANA/anti-dsDNA positive; lupus-specific features |
| Reactive arthritis | Asymmetric, post-infectious |
Treatment
Step-up approach:
- NSAIDs / high-dose aspirin — effective in ~20% (mild systemic disease or predominant arthritis)
- Oral corticosteroids — prednisone 40–60 mg/day for acute systemic features; mainstay of initial therapy
- Methotrexate — first steroid-sparing agent when corticosteroids cannot be tapered (predominant arthritis)
- Biologic agents (moderate–severe systemic disease):
- IL-1 inhibitors: Anakinra (IL-1 receptor antagonist), canakinumab (anti-IL-1β monoclonal antibody) — increasingly used as first-line for severe systemic-predominant disease
- IL-6 receptor inhibitors: Tocilizumab — effective especially in refractory cases
- TNF inhibitors: Some evidence of response in refractory cases
- JAK inhibitors — emerging evidence in refractory AOSD
Current trend: IL-1 and IL-6 pathway inhibitors are being moved earlier in treatment, particularly when systemic inflammation predominates without joint-dominant disease.
— Dermatology 2-Volume Set 5e; Fuster and Hurst's The Heart, 15e
Key Takeaways
| Feature | Hallmark |
|---|---|
| Fever | Quotidian spikes ≥39°C, late afternoon/evening |
| Rash | Salmon-pink, evanescent, coincides with fever |
| Arthritis | Symmetric; carpal ankylosis is distinctive |
| Lab | Markedly elevated ferritin; glycosylated ferritin <20%; seronegative |
| Complication | MAS/HLH — potentially fatal |
| Treatment | NSAIDs → corticosteroids → MTX → IL-1/IL-6 biologics |
This is a shared conversation. Sign in to Orris to start your own chat.