B lymphocytes
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
B lymphocyte development maturation activation
Loading Image
Loading Image
Finding Sources
Reading File
Reading File
Now I have comprehensive information to write a thorough answer on B lymphocytes. Let me compile it.
B Lymphocytes (B Cells)
Origin and Nomenclature
B lymphocytes are named for the bursa of Fabricius in birds, the organ where they were first discovered to mature. In mammals, no bursal equivalent exists — instead, early B cell maturation occurs in the bone marrow, so "B" now stands for bone marrow-derived. Before birth, B cells develop from committed precursors in the fetal liver; after birth, the bone marrow takes over as the primary site.
— Cellular and Molecular Immunology, p. 80; Robbins & Kumar Basic Pathology, p. 160
Role in Immunity
B cells are the principal effector cells of humoral (antibody-mediated) immunity. They:
- Recognize antigens via membrane-bound antibody (IgM class) expressed as the B-cell receptor (BCR) complex
- Unlike T cells, can recognize soluble or cell-associated proteins, lipids, polysaccharides, nucleic acids, and small chemicals — without MHC presentation
- After activation, differentiate into plasma cells that secrete large quantities of antibodies
- Make up 10–20% of circulating lymphocytes
— Robbins & Kumar Basic Pathology, p. 160
Development Stages
Development takes approximately 2–3 days from lymphoid progenitor to mature B cell (in humans). The process involves sequential Ig gene rearrangement and stringent selection:
| Stage | Key Events |
|---|---|
| Pro-B cell | Earliest committed B lineage cell; expresses CD19, CD10; RAG1/RAG2 expressed; D-J recombination of IgH locus begins |
| Pre-B cell | V-to-DJ recombination completes; pre-BCR expressed (μ heavy chain + surrogate light chain); pre-antigen receptor checkpoint passed |
| Immature B cell | First IgM-expressing cell; complete BCR (IgM + Igα/Igβ) on surface; tonic BCR signals suppress further Ig gene rearrangement; self-reactive cells eliminated by receptor editing or apoptosis (central tolerance) |
| Transitional B cell | Leave bone marrow into peripheral blood in 3 stages; self-reactive cells further inactivated in spleen |
| Mature follicular B cell | Express both IgM and IgD; populate secondary lymphoid organs; ready to respond to antigen |
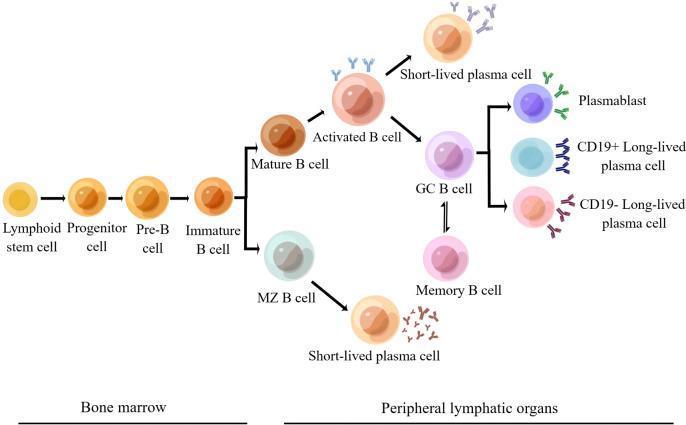
— Cellular and Molecular Immunology, pp. 584–594
B Cell Subsets
Three major subsets exist, each in distinct anatomic locations:
| Subset | Location | Key Features |
|---|---|---|
| Follicular B cells | Lymphoid tissues, blood | Most numerous; express highly diverse BCRs; T cell–dependent activation; produce high-affinity antibodies and memory B cells; undergo class switching (IgM → IgG, IgA, IgE) |
| Marginal zone B cells | Spleen marginal zone (circulating in humans) | T cell–independent; rapid IgM production against blood-borne pathogens; express IgM and CD27 |
| B-1 cells | Mucosal tissues, peritoneal/pleural cavities | Fetal liver–derived; limited antibody diversity; produce "natural antibodies" |
— Cellular and Molecular Immunology, p. 81; Sabiston Textbook of Surgery, p. 545
The B-Cell Receptor (BCR) Complex
- Surface receptor is a monomer of IgM or IgD (~150,000 copies per B cell)
- Each BCR has a unique amino acid sequence in its antigen-binding site (variable region)
- BCR is non-covalently associated with signaling heterodimer Igα (CD79a) and Igβ (CD79b), responsible for intracellular signal transduction upon antigen recognition
- Antigen binding → endocytosis → peptide presentation on MHC class II → helper T cell activation of the B cell
— Janeway's Immunobiology, p. 37; Junqueira's Basic Histology, p. 683
Activation and Germinal Center Reaction
Follicular B cell activation is T cell–dependent:
- BCR binds antigen → endocytosis and MHC II presentation
- CD4⁺ T follicular helper (Tfh) cell recognizes peptide–MHC II complex and provides co-stimulation + IL-4
- B cells enter lymphoid follicles and form germinal centers (GC)
- In germinal centers, B cell DNA undergoes:
- Somatic hypermutation (variable region genes) → affinity maturation
- Class switch recombination (IgM → IgG, IgA, or IgE)
- B cells that acquire high-affinity receptors survive; others undergo apoptosis (cleared by macrophages)
- Post-GC B cells differentiate into:
- Long-lived plasma cells → secrete antibodies (persist in bone marrow)
- Memory B cells → long-lived; enable rapid secondary responses on re-exposure
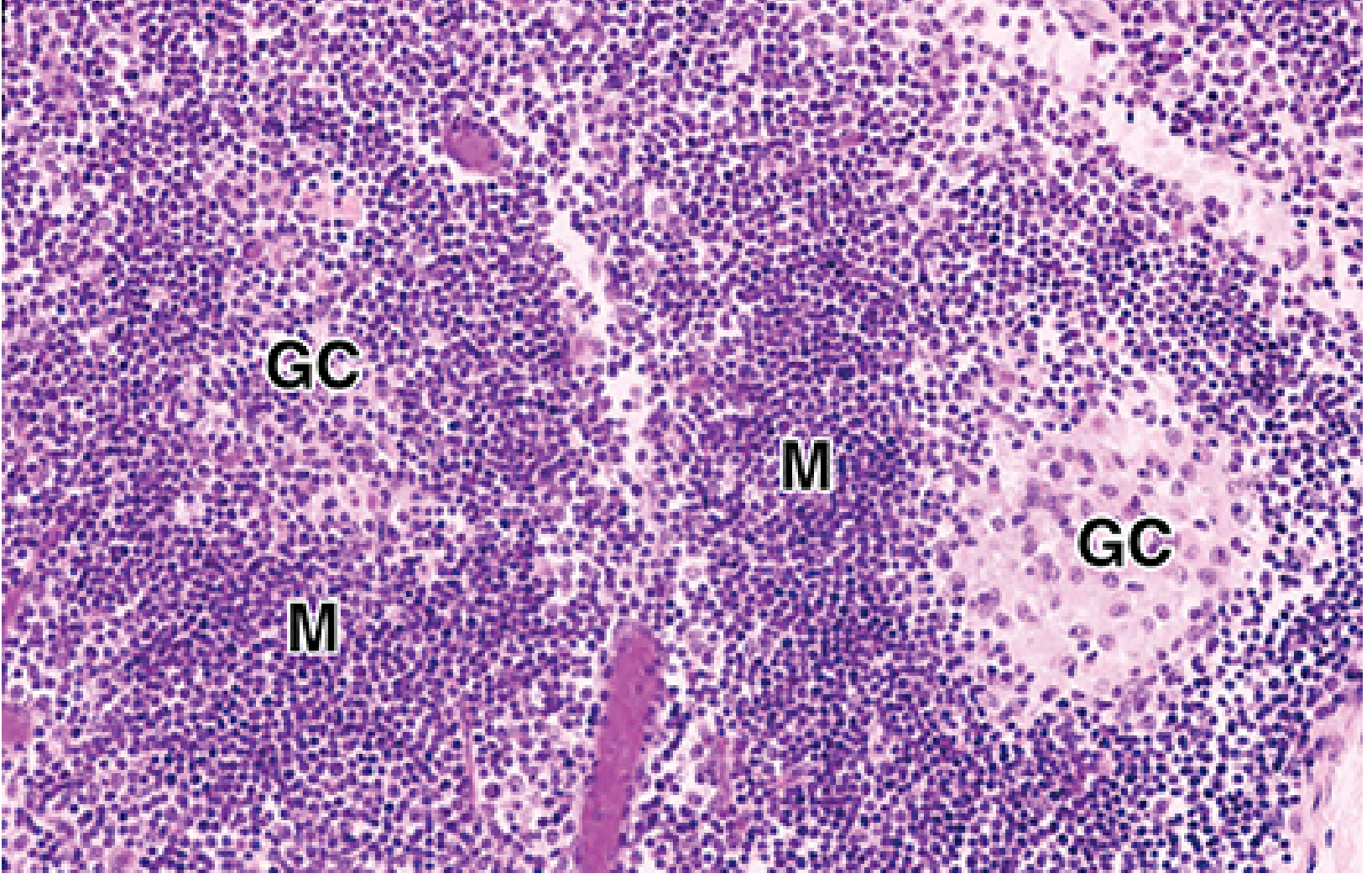
Secondary lymphoid nodules with germinal centers (GC) and follicular mantle (M). Rapid B cell proliferation in the GC pushes naïve lymphocytes to the periphery. — Junqueira's Basic Histology, p. 684
— Junqueira's Basic Histology, pp. 683–685; Cellular and Molecular Immunology, pp. 584–594
Immunoglobulin Classes (Isotypes)
After class switching, B cells/plasma cells produce five isotypes:
| Isotype | Key Role |
|---|---|
| IgG | Highest circulating concentration; long-term protection; crosses placenta |
| IgM | First antibody produced in primary response; efficient complement activation |
| IgA | Predominant in mucosal secretions (gut, respiratory, breast milk) |
| IgE | Very low circulating levels; bound to mast cell surfaces; mediates allergic responses |
| IgD | Expressed on B cell surface; virtually undetectable in blood |
IgG + IgM + IgA together account for >95% of circulating antibodies.
— Robbins & Kumar Basic Pathology, p. 160
Key Surface Markers
- CD19 — expressed throughout B cell lineage; essential for BCR signaling
- CD20 — expressed on mature B cells (target of rituximab)
- CD21 — complement receptor 2; also the EBV receptor
- CD23 — low-affinity IgE receptor (follicular B cells)
- CD27 — memory B cell marker
- MHC class II — required for antigen presentation to T cells
- Fc receptors — modulate B cell activation
Clinical Relevance
- Primary antibody deficiencies (e.g., X-linked agammaglobulinemia / Bruton's disease): failure of B cell maturation due to BTK mutation
- B cell lymphomas/leukemias: malignant transformation at various maturation stages (CLL, follicular lymphoma, diffuse large B cell lymphoma, multiple myeloma from plasma cells)
- Autoimmune disease: autoreactive B cells escaping tolerance → autoantibody production (SLE, rheumatoid arthritis)
- Therapeutic targets: rituximab (anti-CD20), belimumab (anti-BAFF), CAR-T therapies targeting B cell antigens
This is a shared conversation. Sign in to Orris to start your own chat.