Accidental ingestion of petrol
Reading File
Finding Sources
Finding Sources
Searching PubMed
hydrocarbon ingestion children management
Finding Sources
Finding Sources
Searching the Web
accidental petrol ingestion management clinical guidelines
Reading File
Reading File
Reading File
I now have comprehensive content from multiple emergency medicine textbooks. Let me compile the full answer.
Accidental Petrol (Hydrocarbon) Ingestion
Petrol (gasoline) is a petroleum distillate — a low-viscosity, high-volatility, low-surface-tension hydrocarbon. These three physical properties make aspiration into the lungs, not GI absorption, the primary danger.
Epidemiology
- Accidental pediatric ingestion is the most common exposure scenario, typically in children under 6 years old
- U.S. poison centers reported >28,500 hydrocarbon exposures in 2018 alone, with ~4,000 pediatric cases/year; ~10% were hospitalised
- Most accidental small-volume ingestions in children have a favourable outcome
Pathophysiology
Why aspiration is the key danger
Petrol has low viscosity (<60 Saybolt universal seconds), high volatility, and low surface tension — these properties cause it to:
- Spread rapidly across the oral mucosa and tracheobronchial tree
- Vaporize at body temperature
- Be aspirated easily during swallowing, gagging, or vomiting
Pulmonary injury mechanism
Aspiration causes chemical pneumonitis through:
- Direct toxicity to pulmonary parenchyma
- Alteration/destruction of surfactant function
- Destruction of alveolar and capillary membranes → increased vascular permeability → pulmonary oedema
- Can progress to necrotising pneumonitis and haemorrhagic pulmonary oedema in severe cases
GI absorption
Petrol is poorly absorbed from the GI tract; most ingested petrol passes through with only local mucosal irritation.
Systemic toxicity
Simple aliphatic petroleum distillates (plain petrol) cause minimal systemic effects unless large volumes are ingested. Exceptions with greater systemic risk:
- Aromatic hydrocarbons (benzene, toluene, xylene) — CNS, hepatic, renal, haematologic toxicity
- Halogenated hydrocarbons — ventricular arrhythmias ("sudden sniffing death"), hepatotoxicity
- Petrol containing additives (lead, pesticides) — heavy metal or insecticide toxicity on top
Clinical Features
| System | Manifestations |
|---|---|
| Pulmonary | Coughing, choking, gagging, burning in mouth/throat, tachypnoea, grunting respirations, wheezing, retractions, hypoxia — appear soon after exposure |
| GI | Nausea, vomiting, abdominal pain, diarrhoea |
| CNS | Slurred speech, ataxia, lethargy, coma (mostly with aromatic/halogenated types or large volumes) |
| Cardiovascular | Ventricular arrhythmias — mainly with aromatic or halogenated hydrocarbons |
| Fever | ≥39°C (≥102.2°F) — inflammatory response; may appear 6–8 hours post-aspiration |
Key clinical rule: Any patient with coughing, choking, gagging, or dyspnoea after ingestion should be assumed to have aspirated.
Diagnosis
- History is usually straightforward — characteristic petrol odour on breath or clothing
- Chest X-ray at 6 hours after ingestion (bilateral infiltrates; right-sided predominance; multilobar involvement common)
- Note: CXR findings do not reliably correlate with clinical severity
- Investigations for symptomatic or significant ingestions:
- Pulse oximetry / ABG
- Chest X-ray
- ECG (arrhythmia screening, especially for aromatic/halogenated hydrocarbons)
- LFTs, renal function if systemic toxicity suspected
- Screening for co-ingestants in intentional cases
Management
1. Immediate priorities
- Remove contaminated clothing
- Skin: copious irrigation with warm water
- Airway, Breathing, Circulation — assess and support
- Do NOT induce vomiting — this increases aspiration risk
- Do NOT perform gastric lavage or give activated charcoal — not indicated; risks outweigh benefits
- Contact Poison Control Centre / Toxicologist for guidance
2. Respiratory support (if aspiration has occurred)
- Supplemental oxygen for hypoxia
- Inhaled β₂-agonists (e.g., salbutamol) for bronchospasm
- Endotracheal intubation and mechanical ventilation (± PEEP) for severe hypoxia or respiratory failure
3. What NOT to do
| Intervention | Rationale for avoidance |
|---|---|
| Induce emesis | Increases aspiration risk |
| Gastric lavage | Risk of aspiration outweighs benefit; petrol poorly absorbed from GI tract |
| Activated charcoal | Not effective for hydrocarbons; aspiration risk |
| Routine corticosteroids | Not indicated; may be useful only if aspiration triggers acute asthma exacerbation in a known asthmatic |
| Prophylactic antibiotics | Not indicated; may use later if bacterial superinfection develops (typically Staphylococcus aureus or gram-negative organisms) |
4. Monitoring period
- Asymptomatic patients: observe for a minimum of 6 hours
- If still asymptomatic at 6 hours with normal SpO₂ and normal chest exam → can consider discharge with safety-net advice
Discharge Criteria
All of the following must be met:
- Normal GCS
- Normal ECG
- No respiratory symptoms (cough, dyspnoea, wheeze)
- Normal observations including pulse oximetry
- Completed observation period
When to Escalate / Admit
| Indication | Level of care |
|---|---|
| Symptomatic respiratory distress | Admit for monitoring and O₂ |
| Progressive hypoxia or respiratory failure | ICU / PICU; may need intubation |
| CNS depression / seizures | PICU |
| Arrhythmia | Monitored PICU bed |
| Suspected aromatic/halogenated hydrocarbon or toxic additive | Toxicology consult + admission |
Lethality Reference
- In adults: ~20–50 g can cause severe intoxication; ~350 g may be fatal in a 70 kg adult
- In children: as little as 10–15 g (<0.5 oz) may be fatal — lower threshold for aggressive management in paediatric cases
Sources: Rosen's Emergency Medicine (9th ed.), pp. 850–851 | Tintinalli's Emergency Medicine (9th ed.), pp. 1334–1339 | Murray & Nadel's Respiratory Medicine | ATSDR Medical Management Guidelines for Gasoline
Clinical bottom line: Do not induce vomiting. The danger is aspiration pneumonitis, not GI absorption. Supportive care, airway monitoring, β-agonists for bronchospasm, and observation for 6 hours are the cornerstones of management. Most small accidental ingestions in children resolve without complication.
Accidental ingestion of petrol 26 years male
Reading File
Finding Sources
Finding Sources
Searching PubMed
hydrocarbon petroleum ingestion adult toxicity management
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
Excellent — comprehensive data gathered. Here is the full, adult-specific clinical guide:
Accidental Petrol Ingestion — 26-Year-Old Male
Petrol (gasoline) is an aliphatic petroleum distillate with low viscosity, high volatility, and low surface tension — properties that make aspiration into the lungs the primary threat, not GI absorption.
Immediate Priorities on Presentation
- Call Poison Control immediately (1800 222 1222 USA / National Poisons Information in your region)
- Do NOT induce vomiting — this is the single most dangerous mistake; it massively increases aspiration risk
- Remove any petrol-soaked clothing; wash skin with soap and water
- Assess — is he symptomatic or asymptomatic?
Pathophysiology
Petrol enters the tracheobronchial tree during swallowing or vomiting and causes:
- Direct toxicity to pulmonary parenchyma
- Destruction of surfactant
- Breakdown of alveolar-capillary membranes → increased permeability → oedema
- Chemical pneumonitis, potentially progressing to haemorrhagic pulmonary oedema
GI absorption of plain petrol is poor — most passes through with only mucosal irritation.
Risk Stratification for This Patient
Key questions that change management:
| Question | Why it matters |
|---|---|
| How much was swallowed? | >20–50 g = severe intoxication risk in adults |
| Is he symptomatic (coughing, choking, dyspnoea)? | Any of these = assume aspiration has occurred |
| What type of petrol? | Plain pump petrol vs. leaded, aromatic-enriched, or additive-containing |
| Was it accidental or deliberate? | Changes psychiatric risk assessment |
| Any vomiting since ingestion? | Each vomiting episode = re-aspiration risk |
Clinical Features to Assess
Early / Immediate
- Burning in mouth and throat
- Coughing, choking, gagging
- Nausea and vomiting
- Petrol odour on breath
Pulmonary (Aspiration)
- Tachypnoea, grunting respirations, wheezing, retractions
- Hypoxia (SpO₂ ↓)
- Fever ≥39°C — may appear 6–8 hours post-exposure (inflammatory pneumonitis)
- Can progress to necrotising pneumonitis, ARDS
Systemic (Large-Volume Ingestion / Aromatic Components)
| System | Features |
|---|---|
| CNS | Headache, dizziness, slurred speech, ataxia, lethargy, coma |
| Cardiac | Ventricular arrhythmias (especially with aromatic/halogenated hydrocarbons — "sudden sniffing death" syndrome) |
| GI | Abdominal pain, vomiting, diarrhoea |
| Haematologic | Haemolysis (rare with gasoline), methemoglobinaemia (amine-containing additives) |
Any cough, choking, dyspnoea, or gagging = assume aspiration — treat as pulmonary emergency
Emergency Department Management
Step 1 — Decontamination
- Remove contaminated clothing (protect staff from vapour exposure)
- Copious skin washing with soap and water
- Eye irrigation with saline if ocular exposure
Step 2 — Airway and Breathing
- Supplemental oxygen for any hypoxia
- Inhaled β₂-agonists (salbutamol) for bronchospasm/wheeze
- CPAP/BiPAP if oxygenation inadequate on O₂ alone
- Endotracheal intubation + mechanical ventilation (with PEEP) for severe hypoxia, respiratory failure, or CNS depression
- In refractory cases: high-frequency jet ventilation or ECMO (case reports)
- Surfactant therapy — consider for severe pneumonitis
Step 3 — Cardiac Monitoring
- Continuous cardiac monitoring + 12-lead ECG
- Treat ventricular arrhythmias with propranolol, esmolol, or lidocaine
- AVOID catecholamines (adrenaline/epinephrine, dopamine, noradrenaline) — these sensitise the myocardium and can precipitate fatal arrhythmias
- Avoid class IA (procainamide) and class III (amiodarone, sotalol) antiarrhythmics — risk of QT prolongation
Step 4 — IV Access & Fluids
- IV access in symptomatic patients
- IV crystalloid for hypotension
Step 5 — What NOT to Do
| Intervention | Reason to Avoid |
|---|---|
| Induce vomiting | Causes aspiration |
| Gastric lavage | Aspiration risk >> benefit; petrol poorly GI-absorbed |
| Activated charcoal | Does not adsorb hydrocarbons; aspiration risk |
| Routine corticosteroids | No evidence of benefit; may worsen outcome |
| Prophylactic antibiotics | Not indicated acutely; reserve for bacterial superinfection (typically >24 h) |
| Catecholamines for hypotension | Arrhythmia risk — use fluids first |
Investigations
| Test | When to Order |
|---|---|
| Pulse oximetry | All patients |
| Chest X-ray | At 6 hours (even if asymptomatic) — bilateral infiltrates, right-sided predominance |
| ABG | If hypoxic or tachypnoeic |
| 12-lead ECG | All symptomatic patients |
| U&E, creatinine | If systemic toxicity suspected |
| LFTs | If aromatic/halogenated hydrocarbon suspected |
| FBC | If haemolysis or haematologic toxicity suspected |
| Carboxyhaemoglobin | If methylene chloride exposure possible |
| Methaemoglobin | If amine-containing compounds |
CXR findings do not reliably predict clinical severity — manage based on symptoms.
CXR appearance in hydrocarbon pneumonitis:
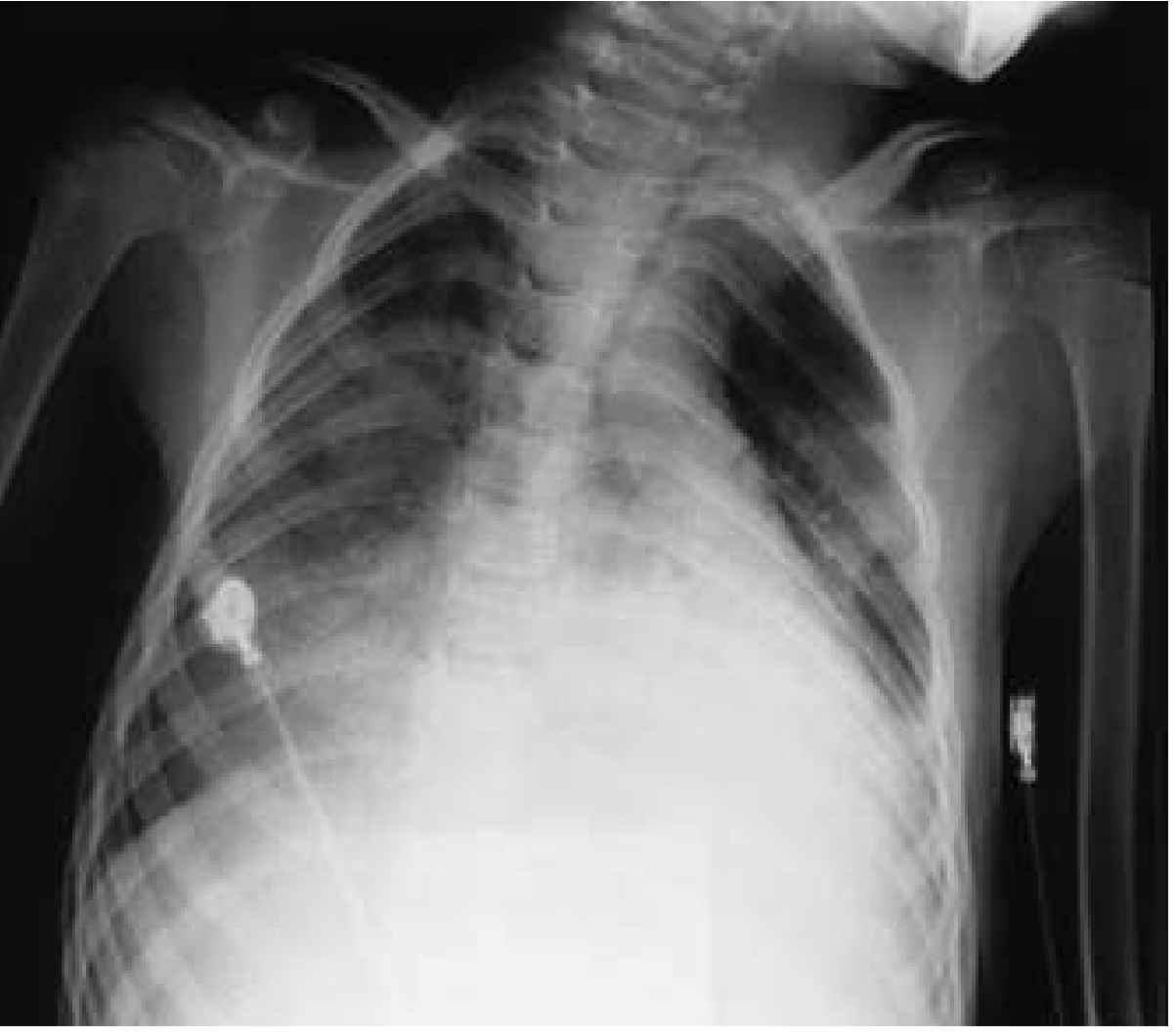
Observation Period & Disposition
| Clinical Status | Action |
|---|---|
| Asymptomatic at 6 hours, normal SpO₂, clear CXR | Can discharge with safety-net advice; poison control follow-up |
| Mild symptoms (cough, minimal work of breathing, low O₂ requirement) | Admit to inpatient ward for monitoring |
| Moderate-severe respiratory distress, significant hypoxia, tachyarrhythmia | ICU admission |
| Mechanical ventilation required | ICU, consider pulmonology consult |
| CNS depression / seizures | ICU |
Discharge Criteria (all must be met)
- Normal GCS and orientation
- Normal ECG
- No respiratory symptoms (no cough, dyspnoea, wheeze)
- Normal SpO₂ on room air
- Normal observations throughout 6-hour period
- Asymptomatic without CXR findings
Prognosis
- Most accidental small-volume petrol ingestions in adults — if no aspiration occurs — have a favourable outcome
- Aspiration pneumonitis is the main cause of morbidity and mortality
- If symptomatic, most patients improve within 2–5 days with supportive care
- Severe cases can progress to ARDS with significant mortality
- A 26-year-old otherwise healthy male has favourable reserve, but prompt assessment is essential
Sources: Rosen's Emergency Medicine (9th ed.), pp. 850–851 | Tintinalli's Emergency Medicine (9th ed.), pp. 1334–1339 | ATSDR Medical Management Guidelines for Gasoline
Bottom line for this patient: Transport to ED. Do not induce vomiting. Monitor for 6 hours minimum. Respiratory symptoms = aspiration until proven otherwise — treat aggressively with O₂ and bronchodilators. Avoid all catecholamines if arrhythmia develops.
This is a shared conversation. Sign in to Orris to start your own chat.