Varicose vein examination
Reading File
search_medical_text
varicose vein clinical examination assessment
search_medical_image
varicose vein examination clinical findings
GradeResponse
GradeResponse
search_medical_text
Trendelenburg test Perthes test varicose veins special tests saphenofemoral junction
GradeResponse
Varicose vein examination (clinical approach)
1) History first
Ask for:
- Leg heaviness, aching, swelling, itching, night cramps, worse on standing
- Visible tortuous veins, skin discoloration, eczema, ulcer history, bleeding episodes
- Prior DVT, thrombophlebitis, trauma, surgery, pregnancy, family history
- Occupation with prolonged standing
Complications to screen: superficial thrombophlebitis, bleeding, venous ulceration.
(Bailey & Love, p. 1051)
(Bailey & Love, p. 1051)
2) Inspection (standing position is essential)
Examine both limbs from groin to ankle, front and back:
- Dilated, tortuous superficial veins along GSV/SSV territories
- Edema (ankle/calf)
- Skin changes of chronic venous hypertension:
- Hyperpigmentation
- Venous eczema
- Lipodermatosclerosis
- Atrophie blanche
- Healed or active ulcer (usually gaiter area)
Advanced disease can show marked varicosity with stasis skin changes, similar to the example image below.
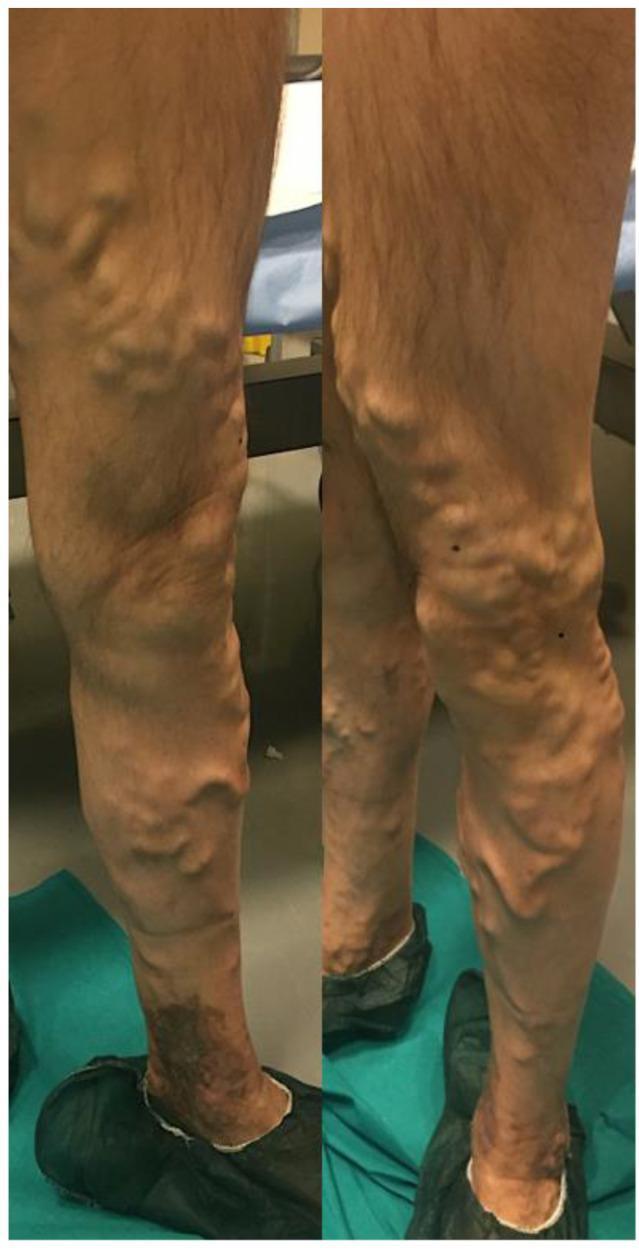
3) Palpation
- Temperature and tenderness over veins (suggests thrombophlebitis)
- Compressibility of varicosities
- Saphenous trunk tenderness or cord-like segments
- Pitting edema
- Peripheral pulses (to exclude mixed arterial disease before compression therapy)
4) Bedside special tests (classical; now less used)
Historically used, but largely replaced by duplex ultrasound:
-
Brodie-Trendelenburg test
- Supine, elevate leg to empty veins, apply proximal thigh tourniquet, then stand.
- Rapid filling may indicate perforator/deep system incompetence; delayed filling after release suggests superficial reflux patterns.
(Harrison, p. 7796)
-
Perthes test
- Tourniquet to occlude superficial flow, then patient walks.
- Pain/increased distension suggests deep venous obstruction or poor deep outflow.
Clinical note: these tests are examiner-dependent and less reliable than duplex mapping.
5) Confirmatory investigation (current standard)
- Duplex venous ultrasound is the key test for:
- Reflux location (SFJ, SPJ, GSV, SSV, perforators)
- Reflux duration/severity
- Deep venous patency and prior DVT changes
- Pre-procedure planning
Harrison notes bedside maneuvers are used infrequently in contemporary practice because of venous ultrasound. (Harrison, p. 7796)
6) Document severity (exam output)
Use CEAP during examination documentation:
- C0-C6 clinical class (from no visible disease to active ulcer)
- Etiology, anatomy, pathophysiology (reflux/obstruction)
If you want, I can give you an OSCE-style varicose vein examination script (exact wording + sequence + presentation summary).
Yes please
search_medical_text
varicose vein OSCE examination sequence steps presentation
search_medical_text
CEAP classification varicose veins grading chronic venous insufficiency
GradeResponse
GradeResponse
Varicose veins OSCE examination script
1) Opening
“Hello, I’m [Name], a medical student/doctor. I’ve been asked to examine your legs, specifically your veins.
This will involve looking and feeling your legs, first lying down and then standing.
It should not be painful, but tell me if you are uncomfortable.
Can I confirm your name and get your consent?”
This will involve looking and feeling your legs, first lying down and then standing.
It should not be painful, but tell me if you are uncomfortable.
Can I confirm your name and get your consent?”
- Wash hands, PPE as needed
- Adequate exposure: from groin to feet (with dignity/chaperone)
- Ensure good lighting
2) Initial overview
From end of bed:
- Is patient comfortable?
- Any walking aid/compression stockings/dressings?
- Visible varicosities, ulcers, edema, skin changes
3) Examination in standing position (most important)
“Could you please stand for me?”
Inspection
Compare both legs, anterior/medial/posterior:
- Dilated tortuous superficial veins (GSV/SSV distribution)
- Edema (ankle/calf)
- Skin changes of chronic venous disease:
- Hyperpigmentation
- Venous eczema
- Lipodermatosclerosis
- Atrophie blanche
- Ulcers/healed ulcers (gaiter area)
- Scars from prior venous procedures
- Signs of thrombophlebitis (localized erythema over vein)
Palpation
- Temperature, tenderness over varicosities
- Induration/cord-like tender superficial vein
- Pitting edema
- Peripheral pulses (DP/PT) to assess arterial status before compression decisions
4) Supine examination
“Please lie down now.”
- Reassess varicosities after elevation (emptying)
- Palpate long saphenous path if needed
- Check for calf tenderness/asymmetry if DVT concern
5) Special tests (mention and perform if required in exam)
(Used less now due to duplex ultrasound)
-
Brodie-Trendelenburg test
- Elevate leg to empty veins, apply upper-thigh tourniquet, ask patient to stand
- Observe filling before/after release
- Used to infer superficial vs perforator/deep incompetence
(Harrison’s, p. 7796)
-
Perthes test
- Tourniquet to occlude superficial veins, patient walks/heel-raises
- Pain/distension suggests poor deep venous outflow
6) Close examination
“Thank you, you can relax and get dressed. I will wash my hands.”
7) Presentation to examiner (concise)
“I examined this patient’s lower limbs for varicose veins.
There are [right/left/bilateral] tortuous superficial veins predominantly in the [GSV/SSV] territory, with [or without] chronic venous skin changes including [list].
There is [or is no] evidence of active ulceration, superficial thrombophlebitis, or bleeding.
Peripheral pulses are [present/absent].
Overall, this is consistent with chronic venous disease likely due to superficial venous reflux.
I would confirm and map reflux with duplex venous ultrasound and classify severity using CEAP.”
There are [right/left/bilateral] tortuous superficial veins predominantly in the [GSV/SSV] territory, with [or without] chronic venous skin changes including [list].
There is [or is no] evidence of active ulceration, superficial thrombophlebitis, or bleeding.
Peripheral pulses are [present/absent].
Overall, this is consistent with chronic venous disease likely due to superficial venous reflux.
I would confirm and map reflux with duplex venous ultrasound and classify severity using CEAP.”
8) What to say for CEAP (quick OSCE add-on)
- C0 no visible disease
- C1 telangiectasia/reticular
- C2 varicose veins
- C3 edema
- C4 skin changes
- C5 healed ulcer
- C6 active ulcer
Guideline recommendation supports using updated CEAP in practice/research.
(Management of Varicose Veins of the Lower Extremities, Part II, p. 9)
(Management of Varicose Veins of the Lower Extremities, Part II, p. 9)
9) Suggested “to complete exam” line
“I would also like to:
- Perform/arrange duplex venous ultrasound,
- Assess VTE risk and DVT history,
- Check ABPI if compression therapy is being considered,
- Do a focused cardiovascular and abdominal exam if secondary causes are suspected.”
If you want, I can give you a 1-minute viva version and a marking checklist.
Supraumbilical hernia
A supraumbilical hernia is a type of ventral (epigastric) hernia occurring in the midline above the umbilicus through a defect in the linea alba.
Key points
- Usually contains preperitoneal fat/omentum, less often bowel
- Presents as a midline swelling above the umbilicus, often more obvious on coughing/straining
- May be asymptomatic or cause pain/discomfort
Clinical features
- Visible/palpable lump above umbilicus
- Cough impulse may be present
- Reducible in many cases
- Pain can worsen with exertion
Red flags (urgent)
- Sudden severe pain
- Irreducible tender swelling
- Vomiting, abdominal distension, constipation
- Skin erythema over swelling
These suggest incarceration/strangulation and need urgent surgical assessment.
Management
- Definitive treatment is surgical repair (open or laparoscopic, often with mesh depending on defect size and patient factors)
- Watchful waiting may be considered in small minimally symptomatic hernias, but persistent symptoms generally favor repair
- Optimize risk factors: weight, smoking, chronic cough, constipation
If you want, I can give you an OSCE-style examination script for supraumbilical hernia and how to differentiate it from paraumbilical, umbilical, and incisional hernia.
Examination
search_medical_text
epigastric hernia supraumbilical hernia clinical examination
search_medical_text
abdominal hernia OSCE examination cough impulse reducibility
GradeResponse
GradeResponse
Supraumbilical (epigastric) hernia examination (OSCE style)
1) Introduction
“Hello, I’m [Name]. I’ve been asked to examine your abdomen, especially the swelling above your umbilicus.
I will inspect and feel your abdomen and may ask you to cough or raise your head.
Tell me if you feel pain. May I proceed?”
I will inspect and feel your abdomen and may ask you to cough or raise your head.
Tell me if you feel pain. May I proceed?”
- Hand hygiene, chaperone, adequate exposure (xiphisternum to pubis)
2) Inspection
- Examine from end of bed and then at abdominal level
- Look for:
- Midline swelling above umbilicus (linea alba)
- Size/shape, skin changes, scars
- Multiple swellings (can have more than one defect)
- Visible cough impulse
Ask patient to:
- Cough
- Raise head/shoulders (or do a mini crunch) to accentuate hernia
(Visible cough impulse helps identify abdominal wall hernia: Bailey & Love, p. 1076)
3) Palpation
- Check local temperature/tenderness
- Identify exact site in midline between xiphisternum and umbilicus
- Assess:
- Size of swelling
- Consistency
- Reducibility (gentle pressure)
- Cough impulse on palpation
- Try to feel fascial defect margins (often small, elliptical)
Epigastric/supraumbilical hernias arise through linea alba and are often small defects; commonly contain extraperitoneal fat rather than bowel.
(Bailey & Love, p. 1095)
(Bailey & Love, p. 1095)
4) Assess for complications
Look specifically for signs of incarceration/strangulation:
- Irreducible painful lump
- Marked tenderness
- Overlying erythema
- Features of obstruction (vomiting, distension) from history
5) Complete abdominal exam
- General abdominal palpation for other masses/tenderness
- Check for additional ventral hernias (umbilical, paraumbilical, incisional)
- Optional: examine hernial orifices if differential includes other hernias
6) Closing
“Thank you, that completes the examination. You can relax.”
7) Presentation summary to examiner
“I examined this patient’s abdomen and found a [size] midline swelling above the umbilicus, consistent with a supraumbilical (epigastric) hernia. It is [reducible/irreducible], with [present/absent] cough impulse, and [no/yes] signs of strangulation. I would confirm clinically and consider ultrasound if uncertainty exists, then refer for surgical management based on symptoms and risk.”
If you want, I can also give you a quick differential table (supraumbilical vs paraumbilical vs incisional vs rectus divarication) for viva answers.
This is a shared conversation. Sign in to Orris to start your own chat.