Give me laq answer on atropine pharmacology
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I have all the content needed for a comprehensive LAQ answer. Here it is:
Atropine — Long Answer Question (Pharmacology)
1. Introduction
Atropine is a naturally occurring tertiary amine belladonna alkaloid (from Atropa belladonna, Datura stramonium) and the prototypical competitive muscarinic receptor antagonist (anticholinergic). It is the racemic mixture of d- and l-hyoscyamine; the l-isomer (l-hyoscyamine) is pharmacologically active.
2. Classification
- Class: Anticholinergic / Antimuscarinic
- Sub-class: Non-selective muscarinic antagonist (blocks M1–M5 equally)
- Chemical nature: Tertiary amine → crosses the blood–brain barrier (CNS effects)
3. Mechanism of Action
Atropine competitively and reversibly blocks muscarinic (M) receptors, preventing acetylcholine (ACh) from binding. It has high affinity for all muscarinic receptor subtypes (M1–M5) without selectivity.
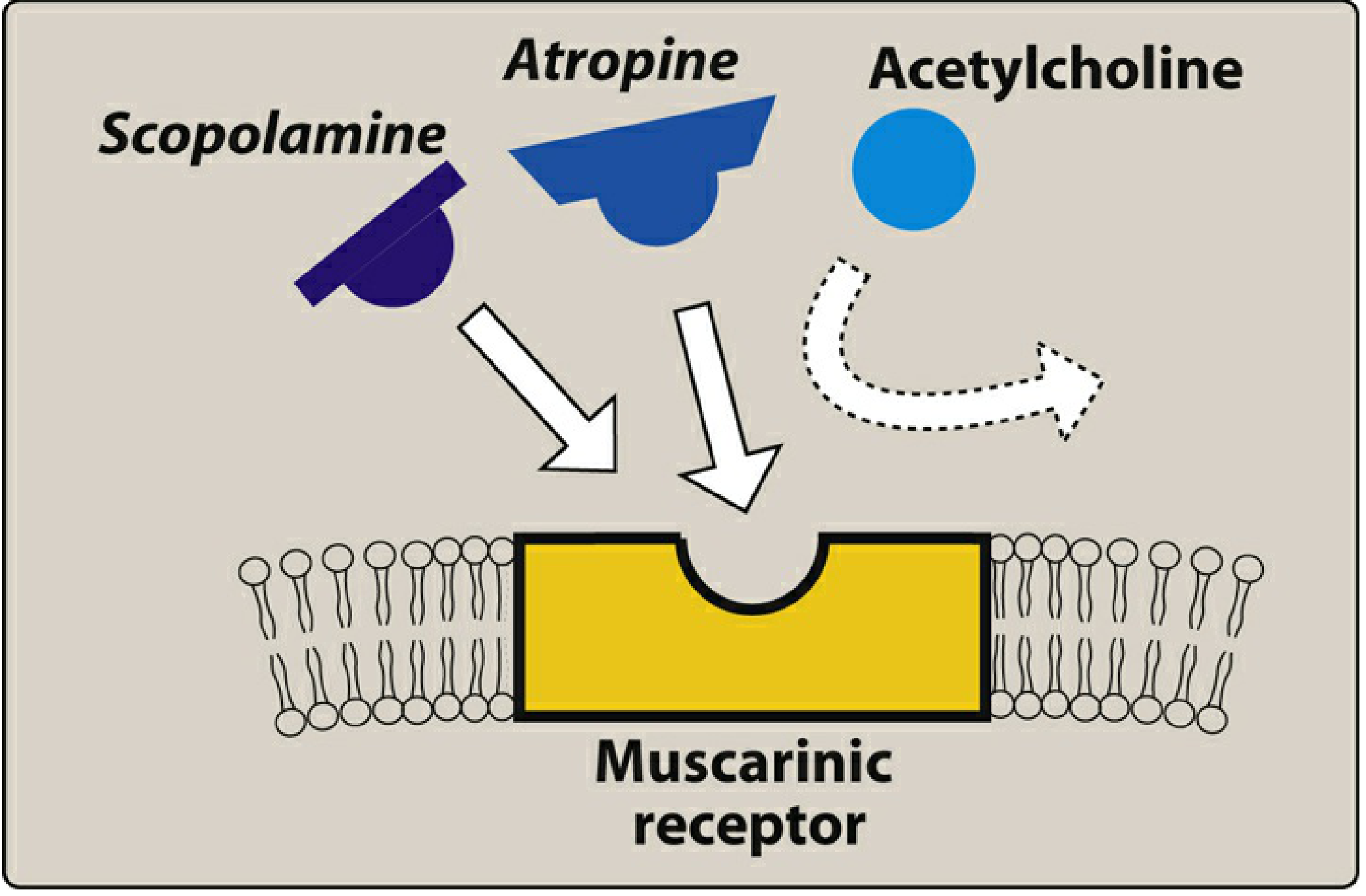
Fig. Competition of atropine and scopolamine with ACh for the muscarinic receptor — Lippincott Illustrated Reviews: Pharmacology
Key receptor subtypes and their locations:
| Receptor | Location | Effect when blocked |
|---|---|---|
| M1 | Nerves, gastric parietal cells | ↓ acid secretion (minimal), ↓ tremor |
| M2 | SA node, AV node, heart | ↑ Heart rate (tachycardia) |
| M3 | Smooth muscle, glands, endothelium | Bronchodilation, dry mouth, mydriasis, urinary retention |
Atropine does NOT block nicotinic receptors at therapeutic doses.
Tissue sensitivity (most → least sensitive to atropine):
Salivary > Bronchial > Sweat glands > Heart > Eye > GI > Bladder > Gastric acid (least)
4. Pharmacokinetics
| Parameter | Details |
|---|---|
| Absorption | Rapidly absorbed orally, IM, IV, or by inhalation |
| Distribution | Widely distributed; crosses BBB (tertiary amine) and placenta |
| Metabolism | Partial hepatic metabolism |
| Excretion | Primarily renal (unchanged + metabolites) |
| Half-life | ~4 hours |
| Duration | Systemic effects ~4 hours; topical ocular effects: 5–6 days |
5. Pharmacological Actions (Organ-by-Organ)
A. Eye (M3 receptors)
- Mydriasis — pupillary dilation (sphincter pupillae blocked)
- Cycloplegia — paralysis of accommodation (ciliary muscle blocked → loss of near vision)
- Unresponsiveness to light
- ⚠ Raises intraocular pressure in angle-closure glaucoma
B. Cardiovascular System (M2 receptors)
- Dose-dependent biphasic effect on heart rate (see diagram below):
- Low dose (0.5 mg): Paradoxical bradycardia (blocks presynaptic M1 on inhibitory neurons → increased ACh release → net slowing)
- Higher doses (≥1–2 mg): Progressive tachycardia (block of M2 at SA node)
- 5 mg: Marked tachycardia, palpitations
- AV conduction time shortened; useful in vagally-mediated bradycardia
C. Exocrine Glands (M3)
- Antisialagogue: Dry mouth (xerostomia) — salivary glands are most sensitive to atropine
- Inhibits lacrimal secretion ("sandy eyes")
- Anhidrosis: Blocks sweat glands → hyperthermia (dangerous in children and elderly)
D. Gastrointestinal Tract (M3)
- Reduces GI motility and peristalsis → antispasmodic
- Decreases intestinal secretions
- Does NOT significantly reduce HCl production (gastric parietal cells are least sensitive) → not useful for peptic ulcer disease
E. Pulmonary
- Bronchodilation by blocking M3 receptors in bronchial smooth muscle
- Reduces bronchial secretions
- Note: Ipratropium (quaternary, inhaled) preferred over systemic atropine for COPD/asthma due to fewer systemic side effects
F. Urinary Tract (M3)
- Relaxes bladder detrusor muscle → urinary retention
- Useful in overactive bladder / bladder spasm (though selective agents like oxybutynin preferred)
G. Central Nervous System
- Low–moderate doses: Mild sedation, antiemetic (vestibular suppression), antitremor
- High/toxic doses: Restlessness, confusion, hallucinations, delirium, coma
- Scopolamine has greater CNS effect; atropine's CNS effects are mainly seen at toxic doses
6. Dose-Dependent Effects
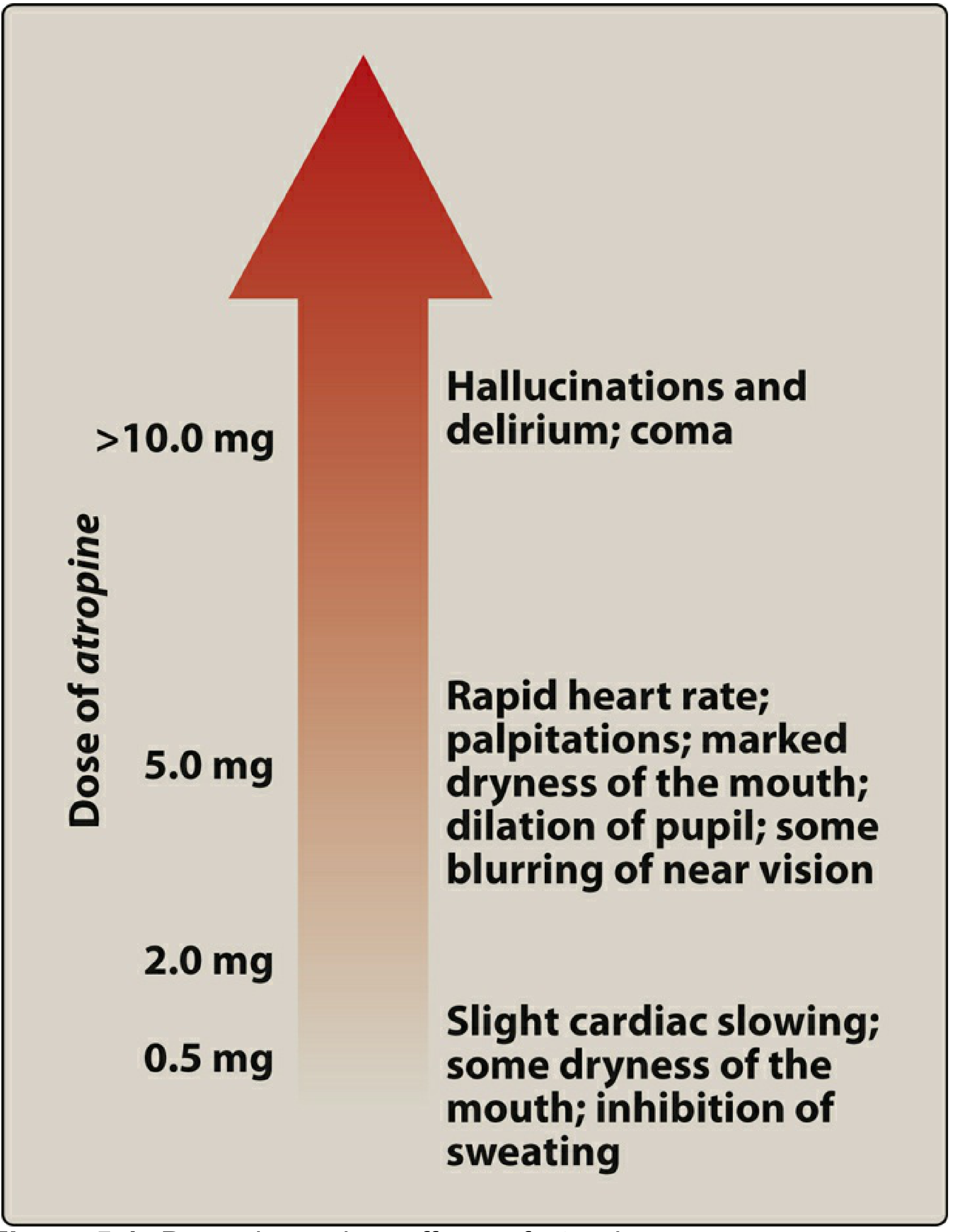
Fig. Dose-dependent effects of atropine — Lippincott Illustrated Reviews: Pharmacology
| Dose | Effect |
|---|---|
| 0.5 mg | Slight cardiac slowing; dry mouth; ↓ sweating |
| 2 mg | Marked dry mouth; tachycardia; mild mydriasis |
| 5 mg | Rapid heart rate; palpitations; blurred vision; marked dry mouth |
| >10 mg | Hallucinations; delirium; coma |
7. Therapeutic Uses
| Indication | Rationale |
|---|---|
| Symptomatic bradycardia | Blocks M2 at SA/AV node → increases heart rate |
| Organophosphate / nerve agent poisoning | Reverses muscarinic excess (SLUDGE); large repeated doses needed; also acts centrally |
| Pre-anesthetic medication | Reduces secretions (antisialagogue), prevents reflex bradycardia |
| Ophthalmic exam (mydriasis/cycloplegia) | Measures refractive error; fundus exam; uveitis treatment (prevent synechiae) |
| GI antispasmodic | Irritable bowel, renal/biliary colic (as hyoscyamine) |
| Mushroom poisoning (Inocybe, muscarine-containing) | Reverses muscarinic toxidrome; 1–2 mg IV |
| AV block (vagally mediated) | Increases AV conduction |
| Anticholinesterase overdose reversal | Counteracts physostigmine, neostigmine muscarinic excess |
In organophosphate poisoning, atropine is titrated to drying of secretions, NOT heart rate.
8. Adverse Effects
- Anticholinergic syndrome (mnemonic):
"Hot as a hare, Blind as a bat, Dry as a bone, Red as a beet, Mad as a hatter"
- Hyperthermia (↓ sweating)
- Mydriasis, cycloplegia (blurred vision)
- Dry mouth, xerostomia
- Flushing (cutaneous vasodilation — compensatory)
- Delirium, hallucinations, confusion (high doses)
- Tachycardia
- Urinary retention
- Constipation
- Geriatric patients: High risk of confusion, disorientation, cognitive decline (BBB penetration)
- Children: Extremely sensitive; fever and CNS toxicity common
9. Contraindications
| Condition | Reason |
|---|---|
| Angle-closure glaucoma | Mydriasis → ↑ IOP → acute attack |
| Benign prostatic hyperplasia | Urinary retention worsened |
| Myasthenia gravis | Blocks therapeutic cholinergic tone |
| Obstructive GI/uropathy | Worsens obstruction |
| Tachyarrhythmias | Further increases HR |
| Thyrotoxicosis | Exacerbates tachycardia |
10. Toxicity and Management
Atropine poisoning presents as the full anticholinergic toxidrome.
Treatment:
- Supportive care
- Physostigmine (cholinesterase inhibitor, crosses BBB) — reverses both central and peripheral effects; dose: 1–2 mg IV slowly
- Avoid for bradycardia or seizure risk patients
- Neostigmine/pyridostigmine only reverse peripheral effects (quaternary, don't cross BBB)
11. Comparison with Related Drugs
| Feature | Atropine | Scopolamine | Glycopyrrolate |
|---|---|---|---|
| Type | Tertiary amine | Tertiary amine | Quaternary ammonium |
| Crosses BBB | Yes | Yes (more) | No |
| CNS effects | At toxic doses | At therapeutic doses | Absent |
| Primary use | Bradycardia, OPC poisoning | Motion sickness, pre-op | Pre-op antisialagogue |
| Duration | ~4 hours | Longer | Longer |
12. Summary
Atropine is a non-selective, competitive muscarinic antagonist with wide-ranging physiological effects. Its dose-dependent cardiovascular effects, ability to cross the BBB, and role as the definitive antidote in organophosphate poisoning make it a cornerstone drug in emergency medicine, anesthesia, and ophthalmology. Its major adverse effects stem from generalized parasympathetic blockade — collectively described as the anticholinergic syndrome.
Sources: Lippincott Illustrated Reviews: Pharmacology; Katzung's Basic & Clinical Pharmacology, 16th Ed.
This is a shared conversation. Sign in to Orris to start your own chat.