urticaria
Reading File
Finding Sources
Searching PubMed
urticaria management guidelines
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
urticaria hives wheal and flare skin
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
I now have comprehensive content. Let me compile the full answer.
Urticaria (Hives)
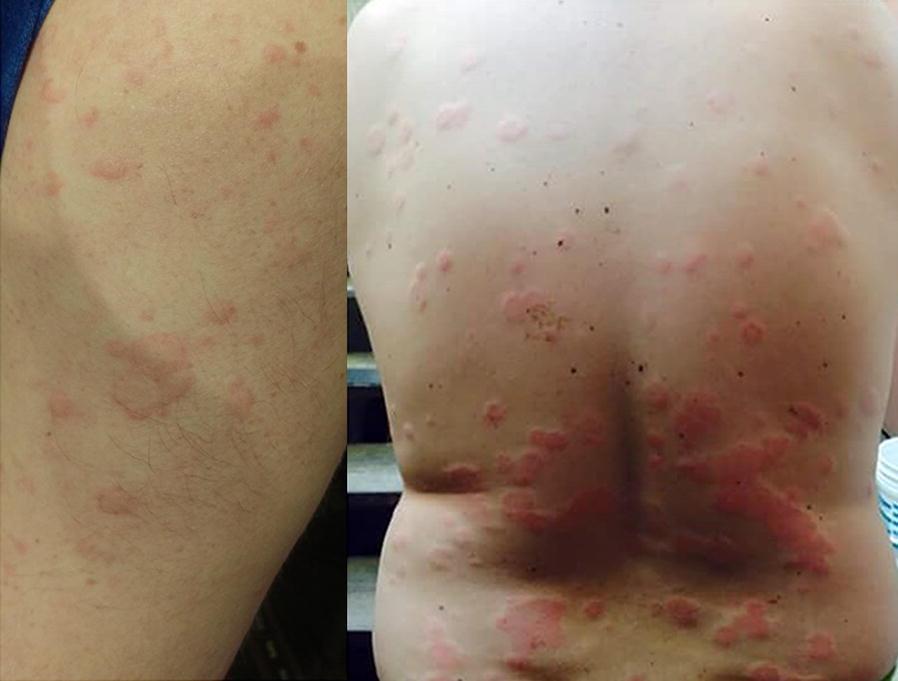
Definition
Urticaria consists of transient, pruritic, edematous plaques (wheals) with pale centers and red borders — the classic "wheal and flare" reaction. Individual lesions reflect localized dermal edema from transvascular fluid extravasation and resolve within <24 hours, although new lesions may continuously appear. Angioedema represents the same process in the subcutaneous/submucosal layer.
Epidemiology
- ~15–20% of the population experiences at least one episode during their lifetime
- Acute urticaria: seen equally in both sexes; common in children with atopic dermatitis
- Chronic urticaria: more common in women in their 40s–50s; peaks in the 3rd–4th decade overall
- 50% of patients with chronic urticaria have disease lasting ≥5 years
- Dermographism alone affects ~5% of the general population
Classification (EAACI 2013 Consensus)
| Duration | Type | Subtypes |
|---|---|---|
| Acute | <6 weeks | Spontaneous |
| Chronic | ≥6 weeks | Spontaneous (CSU) — no identifiable trigger |
| Inducible — physical stimuli |
Inducible (Physical) Urticaria Types:
- Symptomatic dermographism — linear wheals from minor pressure/scratching; most common physical type
- Cold urticaria — exposed skin after cold exposure; risk of wheezing and syncope (avoid cold water swimming); associated with cryoglobulins; autosomal dominant form linked to cryopyrin dysfunction
- Delayed pressure urticaria (DPU) — urticaria/angioedema hours after sustained pressure
- Heat urticaria — provoked by local heat application
- Solar urticaria — within minutes of sun exposure; skin sign of erythropoietic protoporphyria
- Cholinergic urticaria — small wheals with large flares; triggered by heat, exercise, or emotion; occasionally associated with wheezing
- Vibratory angioedema — vibratory stimuli
- Aquagenic urticaria — water contact regardless of temperature
- Contact urticaria — direct skin contact with causative agent
Pathophysiology
Common final pathway: Local mast cell degranulation → release of histamine, bradykinin, kallikrein, acetylcholine, slow-reacting substance of anaphylaxis → dermal edema and vasodilation.
Mechanisms:
| Immunologic | Nonimmunologic |
|---|---|
| IgE-dependent (type I hypersensitivity) | Direct mast cell degranulation (opioids, contrast dye, strawberries, lobster) |
| Autoimmune: functional IgE autoantibodies releasing histamine from mast cells | NSAID/aspirin inhibition (non-IgE; effects persist weeks) |
| Immune complex–mediated (type III) | Vasoactive stimuli |
| Complement-kinin dependent (C1-esterase inhibitor deficiency → hereditary angioedema) |
Causes / Triggers
| Category | Examples |
|---|---|
| Drugs | Penicillin (most common), aspirin/NSAIDs, opioids (virtually any medication can cause urticaria) |
| Foods | Shellfish, tree nuts, peanuts, eggs; histamine releasers: strawberries, lobster |
| Infections | Viral (rhinovirus, rotavirus, hepatitis B/C, EBV, coxsackievirus, SARS-CoV-2); occult Candida, dermatophytes, Helicobacter pylori, parasites |
| Contact | Animal dander/saliva, plants, cosmetics, topical medications, textiles |
| Systemic diseases | Mastocytosis, thyroid disease (hypo/hyperthyroidism), SLE, Sjögren's, rheumatoid arthritis, celiac disease, type 1 DM, Schnitzler's syndrome, Still's disease, serum sickness, hepatitis B/C, cryoglobulinemia, HES, malignancy |
| Physical | Cold, pressure, heat, sun, exercise, vibration, water |
| Idiopathic | ~50% of CSU has no identifiable cause |
Clinical Features
- Morphology: Raised, blanching, erythematous papules/plaques; pale center; red border
- Pruritus: Often intense; stinging or prickling sensation also common
- Duration of individual lesions: <24 hours (key diagnostic feature)
- Angioedema: Eyelids, lips, tongue, larynx, GI tract — occurs in combination with or separate from urticaria; laryngeal involvement is life-threatening
- Urticarial vasculitis: Individual lesions persist >24 hours, may leave bruising; associated with hypocomplementemia and systemic vasculitis
Diagnosis
Acute urticaria: Usually clinical; no routine workup needed for a single episode.
Chronic spontaneous urticaria (CSU) — baseline workup:
- CBC with differential
- ESR and/or CRP
- Thyroid function tests + anti-thyroid antibodies
- Autologous serum skin test (ASST) — assesses for circulating histamine-releasing autoantibodies
Extended workup (based on history):
- Infectious screen (H. pylori, hepatitis serology, stool parasites)
- Allergen-specific IgE / skin prick testing
- Tryptase (rule out mastocytosis)
- ANA, complement levels (if vasculitis suspected)
- Skin biopsy (if lesions >24h, non-blanching, or vasculitis suspected — biopsy shows perivascular eosinophilic/neutrophilic infiltrate)
Inducible urticarias: Provocation + threshold testing with the relevant stimulus (ice cube test for cold urticaria, dermographometer for symptomatic dermographism, etc.) — see Fitzpatrick's Table 41-1.
Differential Diagnosis
- Drug eruption / morbilliform exanthem
- Erythema multiforme (targetoid, non-transient)
- Erythema marginatum
- Urticarial bullous pemphigoid (lesions persist >24h; biopsy required)
- Urticarial vasculitis
- Still's disease (neutrophilic urticarial dermatosis — coincides with fever spikes)
- Mastocytosis (urticaria pigmentosa)
- Neutrophilic urticaria, papular urticaria
Management
Step 1 — Identify and remove triggers
Discontinue offending drug, allergen avoidance, treat underlying infection.
Step 2 — Pharmacotherapy (Stepwise)
| Step | Agent | Notes |
|---|---|---|
| 1st line | 2nd-generation (non-sedating) H1 antihistamines | Cetirizine, fexofenadine, loratadine, desloratadine, bilastine — preferred for chronic use |
| Adjunct | H2 antihistamine (ranitidine/famotidine) added to H1 blocker | Modest additional benefit |
| Acute severe | Systemic corticosteroids | Prednisone or dexamethasone for moderate–severe episodes; 14–21 days with taper for recurrent urticaria; chronic steroid use NOT recommended |
| Refractory CSU | Omalizumab (anti-IgE monoclonal antibody) | Standard of care for H1-antihistamine-resistant CSU; approved and highly effective |
| Refractory CSU | Cyclosporine | Immunosuppressant for omalizumab failure/intolerance |
| Symptom relief | Hydroxyzine | Sedating H1 blocker; for acute pruritus relief |
Anaphylaxis/angioedema with airway involvement: Epinephrine IM immediately → antihistamines + corticosteroids → observation.
Urticaria vs. Angioedema
| Feature | Urticaria | Angioedema |
|---|---|---|
| Layer | Dermis | Subcutis / submucosa |
| Lesion | Wheal + flare, pruritic | Deep swelling, may be painful or burning |
| Sites | Anywhere | Face, lips, tongue, larynx, GI |
| Risk | Discomfort | Airway compromise (laryngeal) |
Key Associations to Remember
- Penicillin → most common drug cause (traces in dairy may sensitize)
- Aspirin/NSAIDs → non-immunologic; effects persist weeks after stopping
- Cholinergic urticaria + cold urticaria → common co-occurring inducible types
- Cold urticaria + cryoglobulins → screen for hematologic/lymphoproliferative disease
- Solar urticaria → consider erythropoietic protoporphyria (pitted nasal/hand scarring)
- CSU + thyroid autoimmunity → well-established association (screen all CSU patients)
- Omalizumab → backed by multiple RCTs and now guideline-recommended for antihistamine-refractory CSU (PMID 41182242 — 2025 Asian-Pacific clinical practice guideline)
Sources: Goldman-Cecil Medicine, Rosen's Emergency Medicine, Fitzpatrick's Dermatology, Harrison's Principles of Internal Medicine (22nd ed.), Dermatology 5e (Elsevier).
This is a shared conversation. Sign in to Orris to start your own chat.