Anatomy and physiology of git system explained clearly notes
Reading File
search_medical_text
anatomy gastrointestinal tract structure layers organs
search_medical_text
physiology gastrointestinal motility secretion absorption digestion
search_medical_image
gastrointestinal tract anatomy diagram layers
GradeResponse
GradeResponse
GradeResponse
Good results. Now I have solid foundational content. Let me compile a comprehensive, well-structured set of notes covering all major aspects of GIT anatomy and physiology.
Anatomy & Physiology of the Gastrointestinal (GI) Tract
1. Overview
The gastrointestinal (GI) tract extends from the mouth to the anus and is a continuous hollow muscular tube (~9 meters long in a cadaver) responsible for ingestion, digestion, absorption, and excretion. It is compartmentalized by sphincters and associated with accessory organs (liver, gallbladder, pancreas).
(Harrison's Principles of Internal Medicine, 21st Ed., p. 8735)
2. Layers of the GI Wall
All hollow GI organs share a common 4-layer wall structure, from inside out:
| Layer | Components | Function |
|---|---|---|
| Mucosa | Epithelium + Lamina propria + Muscularis mucosae | Absorption, secretion, barrier |
| Submucosa | Connective tissue, blood vessels, Meissner's plexus | Support, secretory regulation |
| Muscularis externa | Inner circular + Outer longitudinal smooth muscle; Auerbach's plexus between them | Peristalsis, mixing |
| Serosa / Adventitia | Visceral peritoneum or fibrous coat | Support, external input |
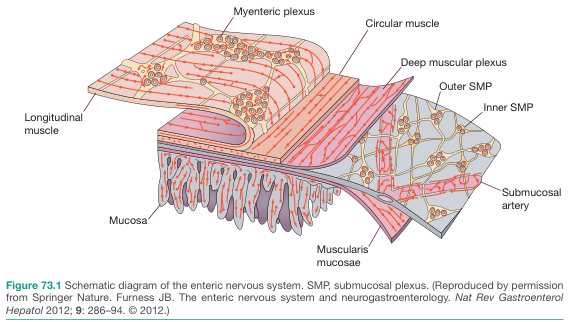
Enteric Nervous System (ENS) Plexuses
The GI wall contains two key neural networks:
- Myenteric plexus (Auerbach's) — between circular and longitudinal muscle layers → controls motility
- Submucosal plexus (Meissner's) — in the submucosa → controls secretion and absorption
- A deep muscular plexus is also embedded within the circular muscle layer
(Bailey & Love's Surgery, 28th Ed., p. 1310)
3. Organs of the GI Tract
A. Mouth & Oropharynx
- Function: Mastication (chewing), initial carbohydrate digestion
- Salivary glands (parotid, submandibular, sublingual) secrete salivary amylase (ptyalin) → breaks starch → maltose
- Mucus lubricates the food bolus
- Deglutition (swallowing) has 3 phases: voluntary (oral), involuntary pharyngeal, esophageal
B. Esophagus
- Length: ~25 cm; runs from cricopharyngeus to gastroesophageal junction
- Layers: Mucosa (stratified squamous epithelium), submucosa, muscularis (upper 1/3 skeletal, lower 2/3 smooth), adventitia (no serosa)
- Sphincters:
- Upper esophageal sphincter (UES) — cricopharyngeus muscle, prevents reflux into pharynx
- Lower esophageal sphincter (LES) — prevents gastric reflux; resting tone ~15–25 mmHg
- Function: Propels food via primary peristalsis (triggered by swallowing); secondary peristalsis clears residual food
C. Stomach
Anatomy
| Region | Features |
|---|---|
| Cardia | Entry from esophagus |
| Fundus | Dome above cardia; gas reservoir |
| Body (Corpus) | Main secretory region |
| Antrum | Pyloric region; gastrin secretion |
| Pylorus | Pyloric sphincter → controls gastric emptying |
- Rugae = mucosal folds that allow distension (capacity ~1–1.5 L)
- Gastric pits open into gastric glands
Gastric Secretion
- Principal secretory products: HCl (from parietal cells) and pepsinogen (from chief cells)
- Functions of gastric acid:
- Protein digestion (activates pepsinogen → pepsin)
- Absorption of Fe²⁺, Ca²⁺, Mg²⁺, vitamin B₁₂
- Bactericidal activity
Phases of Gastric Acid Secretion
| Phase | Stimulus | Mechanism |
|---|---|---|
| Cephalic | Sight, smell, taste of food | Vagus nerve (cholinergic) |
| Gastric | Food distension, peptides in stomach | Gastrin from G-cells, histamine from ECL cells |
| Intestinal | Chyme in duodenum | Gastrin-like peptides; inhibited by secretin, CCK |
- Basal acid secretion: follows a circadian rhythm — highest at night, lowest in the morning; driven by vagal and histaminergic tone
- Inhibition: secretin (acid in duodenum), CCK, GIP → enterogastric reflex
(Harrison's 21st Ed., p. 8896)
Cell Types in Gastric Glands
| Cell | Secretion | Function |
|---|---|---|
| Parietal (oxyntic) | HCl, Intrinsic Factor | Acid production; IF needed for B₁₂ absorption |
| Chief (zymogenic) | Pepsinogen | Protein digestion (activated by acid) |
| Mucous neck cells | Mucus | Cytoprotection |
| G-cells (antrum) | Gastrin | Stimulates parietal cells |
| ECL cells | Histamine | Potent stimulator of HCl via H₂ receptors |
| D-cells | Somatostatin | Inhibits gastrin and acid secretion |
D. Small Intestine
Largest site of digestion and absorption (~6–7 m long)
Divisions
| Part | Length | Key Features |
|---|---|---|
| Duodenum | ~25 cm (C-shaped) | Receives bile + pancreatic juice; Brunner's glands (alkaline mucus) |
| Jejunum | ~2.5 m | Main site of absorption; thick folds (plicae circulares) |
| Ileum | ~3.5 m | B₁₂ + bile salt reabsorption; Peyer's patches (lymphoid tissue) |
Mucosal Specializations (Increase Surface Area ~600×)
- Plicae circulares (valves of Kerckring) — circular folds of mucosa
- Villi — finger-like projections; each has lacteals (lymph) and capillaries
- Microvilli (brush border) — on enterocytes; contain digestive enzymes
Secretions
- Secretin (S-cells) — released by acid in duodenum → stimulates pancreatic bicarbonate
- CCK (I-cells) — released by fats/proteins → stimulates pancreatic enzymes + gallbladder contraction
- Brush border enzymes: lactase, sucrase, maltase, enterokinase (activates trypsinogen)
Absorption Summary
| Nutrient | Site | Mechanism |
|---|---|---|
| Carbohydrates (as monosaccharides) | Jejunum | SGLT1 (active), GLUT5 (fructose) |
| Amino acids | Jejunum | Na⁺-dependent cotransport |
| Fats (as fatty acids + monoglycerides) | Jejunum | Micelles → passive diffusion → chylomicrons → lacteals |
| Iron | Duodenum | Active (ferrous form) |
| Calcium | Duodenum | Active (vitamin D-dependent) |
| B₁₂ (cobalamin) | Terminal ileum | Intrinsic factor-dependent |
| Bile salts | Terminal ileum | Active transport (enterohepatic circulation) |
| Water | Entire small intestine | Osmosis |
E. Large Intestine (Colon)
Length: ~1.5 m
Divisions
- Cecum + Appendix (vermiform)
- Ascending colon → Transverse colon → Descending colon → Sigmoid colon
- Rectum (~15 cm) → Anal canal (~4 cm)
Anatomical Features
- Haustra — sacculations due to incomplete longitudinal muscle bands (taeniae coli)
- Epiploic appendages — fatty appendages on outer surface
- No villi — mucosa has crypts (Lieberkühn) only; lined by columnar cells + goblet cells
Physiology
- Water & electrolyte absorption: absorbs ~1.5 L/day of water; Na⁺ absorbed, K⁺ secreted
- Bacterial fermentation: gut microbiota ferments undigested carbohydrates → short-chain fatty acids (SCFAs: butyrate, propionate, acetate) → energy source for colonocytes
- Motility: haustral churning (slow mixing), mass movements (3–4×/day, especially after meals — gastrocolic reflex)
- Defecation reflex: rectal distension → internal anal sphincter relaxes (involuntary) → external anal sphincter (voluntary) relaxes
F. Rectum & Anal Canal
- Rectum: storage reservoir; highly distensible
- Internal anal sphincter: smooth muscle, involuntary
- External anal sphincter: skeletal muscle, voluntary (pudendal nerve)
- Anorectal angle: maintained by puborectalis muscle; important for continence
4. Accessory Digestive Organs
A. Liver
- Largest internal organ (~1.5 kg); right + left lobes; functional unit = hepatic lobule (portal triad: portal vein + hepatic artery + bile duct)
- Functions:
- Bile synthesis (500–1000 mL/day) → emulsification of fats
- Metabolism of carbohydrates, proteins, lipids
- Detoxification, drug metabolism (CYP450)
- Protein synthesis (albumin, clotting factors II, VII, IX, X)
- Storage of glycogen, vitamins A, D, B₁₂, iron
B. Gallbladder
- Stores and concentrates bile (~10× concentration)
- Bile: bile salts + bilirubin + cholesterol + phospholipids
- Released in response to CCK
- Enterohepatic circulation: bile salts reabsorbed at terminal ileum → portal vein → liver → re-secreted
C. Pancreas
- Exocrine (99% of mass): acini secrete digestive enzymes
- Proteases: trypsinogen, chymotrypsinogen, elastase (secreted as zymogens)
- Lipase, amylase, phospholipase
- Stimuli: CCK → enzymes; Secretin → bicarbonate-rich fluid (neutralizes duodenal acid)
- Endocrine (Islets of Langerhans):
- α-cells: glucagon
- β-cells: insulin
- δ-cells: somatostatin
5. GI Motility Overview
| Region | Type of Motility | Function |
|---|---|---|
| Esophagus | Primary/secondary peristalsis | Propulsion of bolus |
| Stomach | Receptive relaxation, peristalsis, antral grinding | Mixing, grinding, regulated emptying |
| Small intestine | Segmentation (mixing), peristalsis (propulsion), MMC (housekeeping) | Digestion + absorption |
| Large intestine | Haustral shuttling, mass movements | Water absorption, defecation |
Migrating Motor Complex (MMC): "housekeeper" contractions that clear the gut between meals; occur every ~90–120 min; abolished by eating
6. GI Hormones Summary
| Hormone | Source | Stimulus | Actions |
|---|---|---|---|
| Gastrin | G-cells (antrum) | Protein, vagus nerve | ↑ HCl, ↑ pepsinogen, ↑ gastric motility |
| Secretin | S-cells (duodenum) | Acid (low pH) | ↑ Pancreatic HCO₃⁻, ↓ gastric acid |
| CCK | I-cells (duodenum/jejunum) | Fat, protein | ↑ Pancreatic enzymes, ↑ bile, ↓ gastric emptying |
| GIP | K-cells (duodenum) | Fat + glucose | ↑ Insulin secretion, ↓ gastric acid |
| Motilin | Mo-cells (duodenum) | Fasting state | Initiates MMC |
| Somatostatin | D-cells (stomach, pancreas) | Many stimuli | Universal inhibitor of GI secretion |
| VIP | ENS neurons | Distension | Smooth muscle relaxation, ↑ intestinal secretion |
7. GI Blood Supply
| Organ | Arterial Supply |
|---|---|
| Stomach | Celiac trunk branches (left/right gastric, gastro-omental) |
| Duodenum (1st–2nd) | Gastroduodenal artery → superior pancreaticoduodenal |
| Duodenum (3rd–4th) + Small bowel | Superior mesenteric artery (SMA) |
| Ascending + Transverse colon | SMA |
| Descending + Sigmoid colon | Inferior mesenteric artery (IMA) |
| Rectum | Superior rectal (IMA) + Middle/inferior rectal (internal iliac) |
Watershed areas (susceptible to ischemia): Splenic flexure (SMA/IMA junction), Rectosigmoid junction
8. Nerve Supply
- Parasympathetic: Vagus nerve (CN X) — foregut + midgut; Pelvic splanchnic nerves (S2–S4) — hindgut → stimulates motility + secretion
- Sympathetic: Splanchnic nerves (T5–L2) → celiac, superior & inferior mesenteric ganglia → inhibits motility, causes vasoconstriction
- ENS (enteric nervous system): "second brain" — can function independently; ~500 million neurons; uses ACh, NO, VIP, serotonin (5-HT3/4 important targets for drugs)
Key Takeaways
- The GI wall has 4 layers; the ENS (Auerbach's + Meissner's plexuses) governs autonomous gut function
- Gastric acid secretion has 3 phases: cephalic, gastric, intestinal; parietal cells secrete HCl via H⁺/K⁺-ATPase
- The small intestine is the primary site for digestion and absorption; surface area is amplified ~600× by folds, villi, microvilli
- The colon mainly absorbs water, electrolytes, and produces SCFAs via bacterial fermentation
- GI hormones (gastrin, secretin, CCK, GIP, motilin) coordinate digestion in a highly regulated sequence
- The liver, gallbladder, and pancreas are essential accessory organs; bile and pancreatic enzymes are critical for fat and protein digestion
This is a shared conversation. Sign in to Orris to start your own chat.