Motor ,sensory,cerebellar Reflexes, how to do that and what are the normal and abnormal findings, how to grade that
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
deep tendon reflex grading scale neurological examination
I now have comprehensive information from Harrison's (22E), Bradley & Daroff's Neurology, Textbook of Family Medicine, and Adams & Victor's. Let me compile the full answer.
Neurological Examination: Motor, Sensory, Cerebellar & Reflexes
1. MOTOR EXAMINATION
How to Do It
A. Appearance / Inspection
- Inspect and palpate muscle groups in good light, patient in a comfortable, symmetric position.
- Look for: muscle atrophy, hypertrophy, fasciculations, tenderness.
- Observe for involuntary movements at rest (e.g., pill-rolling tremor of Parkinson's), during maintained posture (essential tremor), or with voluntary movement (intention tremor of cerebellar disease).
B. Muscle Tone
Test by measuring resistance to passive movement of a relaxed limb. Distract the patient to minimize voluntary contraction.
| Region | Technique |
|---|---|
| Upper limb | Rapid pronation/supination of forearm + flexion/extension at wrist |
| Lower limb | Patient supine; examiner places hands behind knees and rapidly raises them — with normal tone, the ankles drag along the table before rising |
C. Strength Testing
- Pronator drift: Ask patient to hold both arms fully extended, parallel to the ground, with eyes closed for ~10 seconds. Any flexion at elbow/fingers or pronation of the forearm (especially asymmetric) = sign of weakness.
- Isolate each muscle group and ask patient to exert maximal effort against examiner resistance.
Muscle Strength Grading (MRC Scale)
| Grade | Meaning |
|---|---|
| 0 | No movement |
| 1 | Flicker/trace of contraction, no joint movement |
| 2 | Movement with gravity eliminated |
| 3 | Movement against gravity, not against resistance |
| 4− | Movement against mild resistance |
| 4 | Movement against moderate resistance |
| 4+ | Movement against strong resistance |
| 5 | Full power |
Normal vs. Abnormal Findings
| Finding | Normal | Abnormal |
|---|---|---|
| Tone | Slight, symmetric resistance to passive movement | Spasticity (corticospinal tract) · Rigidity/cogwheeling (extrapyramidal/Parkinson's) · Flaccidity (LMN/peripheral nerve) · Paratonia (frontal lobe) |
| Strength | 5/5 all muscle groups | ≤4 = weakness; pattern matters (see below) |
| Pronator drift | No drift in 10 seconds | Drift = contralateral corticospinal lesion |
| Involuntary movements | None at rest | Fasciculations (LMN), tremor, chorea, myoclonus, dystonia |
Pattern of Weakness:
- Pyramidal pattern (UMN) — upper limb extensors + lower limb flexors weak → corticospinal tract lesion
- Bilateral proximal → myopathy
- Bilateral distal → peripheral neuropathy
- UMN features — increased tone, hyperreflexia, Babinski sign
- LMN features — wasting, fasciculations, decreased tone, absent reflexes
2. SENSORY EXAMINATION
How to Do It
Test five primary sensory modalities in each limb:
| Modality | Technique | Pathway |
|---|---|---|
| Light touch | Wisp of cotton / fingertip — single gentle touches | Dorsal column / spinothalamic |
| Pain (pinprick) | New pin; ask "sharp or dull?" | Spinothalamic (lateral) |
| Temperature | Metal tuning fork immersed in cold/warm water | Spinothalamic (lateral) |
| Vibration | 128-Hz tuning fork on distal phalanx of great toe or index finger at nail bed; examiner places finger on opposite side of joint to compare thresholds | Dorsal column |
| Joint position (proprioception) | Grasp digit laterally, make 1–2 mm excursions; patient identifies "up" or "down" | Dorsal column |
Romberg Maneuver: Patient stands with feet together, eyes open → then closed. Loss of balance with eyes closed = abnormal (proprioceptive loss — peripheral or posterior column).
Cortical Sensation (only test if primary sensation intact):
- Double simultaneous stimulation — touch both hands; parietal lesion = extinction of contralateral stimulus
- Two-point discrimination — ability to distinguish two closely placed stimuli
- Stereognosis — identify object by touch alone
- Graphesthesia — identify numbers/letters written on skin
Normal vs. Abnormal Findings
| Test | Normal | Abnormal |
|---|---|---|
| Light touch | Felt equally both sides | Loss in dermatomal, glove-stocking, or hemisensory pattern |
| Pinprick | Sharp perceived symmetrically | Dissociated sensory loss (pain/temp lost, vibration intact) = spinothalamic lesion |
| Vibration | Felt at distal phalanx; diminishes symmetrically with age | Early loss in peripheral neuropathy; posterior column disease |
| Joint position | Correctly identifies all movements | Loss → sensory ataxia, pseudoathetosis |
| Romberg | Stable with eyes closed | Positive Romberg = posterior column or peripheral proprioceptive loss |
| Cortical sensation | Correctly identifies all bilateral stimuli | Extinction, astereognosis, agraphesthesia → parietal lesion |
3. CEREBELLAR EXAMINATION (Coordination)
The cerebellar exam covers 5 domains: eyes, speech, hands, legs, and gait. The SARA scale is used for formal rating.
How to Do It
| Test | Technique | What Is Assessed |
|---|---|---|
| Finger-to-nose | Patient touches their index finger → nose → examiner's outstretched finger (which moves each rep) | Limb dysmetria, intention tremor |
| Finger chase | Patient's index finger follows examiner's moving finger | Dysmetria, overshoot |
| Rapid alternating movements (RAM/dysdiadochokinesis) | Patient makes fist → extends index finger → taps distal thumb as fast as possible; lower limb = rapid foot tapping | Cerebellar hemisphere function |
| Heel-knee-shin | Supine patient lifts heel → places on opposite knee → slides down shin to ankle | Leg dysmetria |
| Gait | Walk normally, then tandem (heel-to-toe), walk up/down stairs | Truncal ataxia, wide-based gait |
| Stance | Stand with feet together → tandem stance → one foot → hop | Truncal sway, balance |
| Speech | Listen during history | Scanning/staccato speech |
| Eye movements | Fixation, smooth pursuit, saccades | Nystagmus, saccadic pursuit |
Normal vs. Abnormal Findings
| Finding | Normal | Abnormal (Cerebellar Sign) |
|---|---|---|
| Finger-to-nose | Smooth, accurate | Intention tremor (tremor worsens as approaching target), dysmetria (past-pointing) |
| RAM | Fast, rhythmic, symmetric | Dysdiadochokinesis (imprecise, irregular rhythm/amplitude) |
| Heel-knee-shin | Heel stays on shin smoothly | Heel falls off shin |
| Gait | Normal stride, arm swing | Wide-based, staggering, veering to one side |
| Stance | Stable feet-together | Truncal sway (even while sitting without support) |
| Speech | Clear, fluent | Scanning speech — slow, slurred, irregular syllable force |
| Eye movements | Smooth pursuit, accurate saccades | End-gaze nystagmus, saccadic pursuit, square-wave jerks |
Important: Slow RAM compared with contralateral side suggests a pyramidal tract lesion rather than cerebellar — distinguish carefully.
4. REFLEX EXAMINATION
How to Do It
Key principle: Patient must be relaxed; position muscle midway between full contraction and extension. Compare both sides. Find the smallest stimulus to elicit the reflex (not the maximal response).
Jendrassik Maneuver (reinforcement): To enhance reflexes — upper limb reflexes reinforced by voluntary teeth-clenching; Achilles reflex by hooking the flexed fingers of both hands together and trying to pull apart.
Standard Deep Tendon Reflexes (DTRs)
| Reflex | Technique | Spinal Level |
|---|---|---|
| Biceps | Strike biceps tendon with finger interposed | C5, C6 |
| Brachioradialis | Strike brachioradialis tendon at radial styloid | C5, C6 |
| Triceps | Strike triceps tendon above olecranon | C6, C7 |
| Finger flexor | Strike examiner's finger over patient's finger flexors | C8, T1 |
| Patellar (knee jerk) | Legs hanging freely; strike patellar tendon just below patella | L3, L4 |
| Achilles (ankle jerk) | Foot slightly dorsiflexed; strike Achilles tendon | S1, S2 |
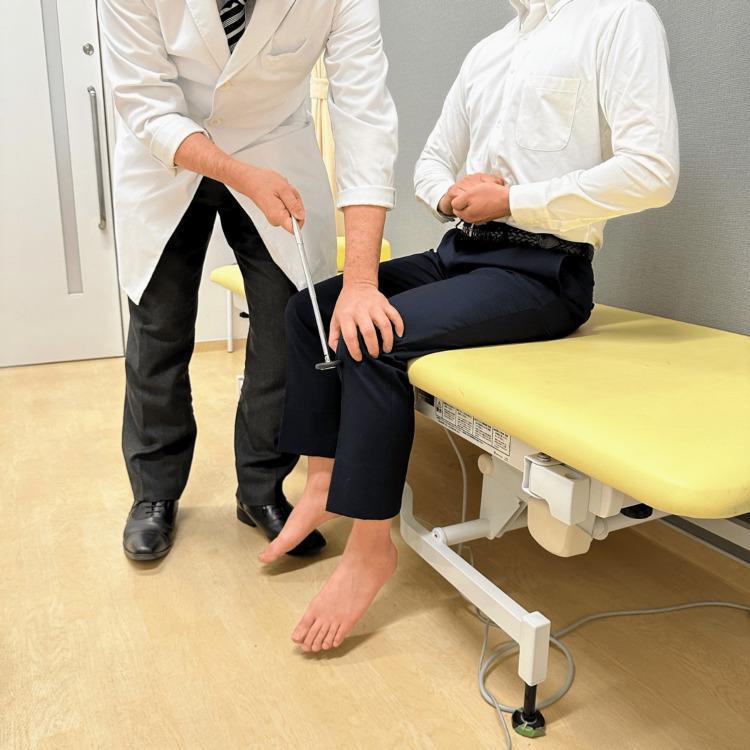
Eliciting the patellar reflex with the Jendrassik maneuver (patient interlocks fingers and pulls apart)
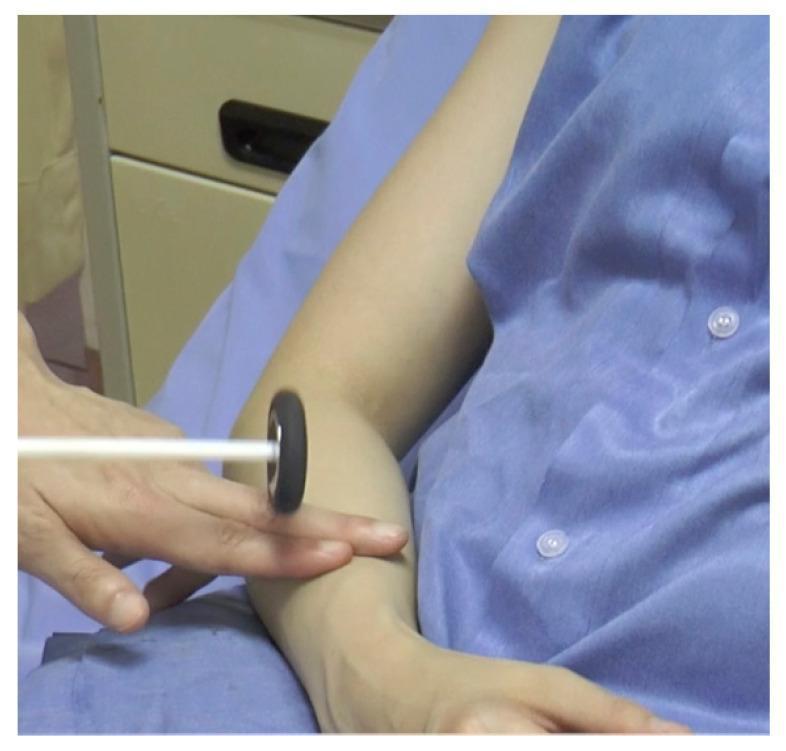
Brachioradialis reflex technique (C5–C6)
Reflex Grading Scale
| Grade | Meaning |
|---|---|
| 0 | Absent |
| 1 | Present but diminished |
| 2 | Normoactive (normal) |
| 3 | Increased (hyperreflexia) without clonus |
| 4 | Clonus present |
Cutaneous Reflexes
| Reflex | Technique | Normal | Abnormal |
|---|---|---|---|
| Plantar (Babinski) | Stroke lateral sole from heel across ball to great toe with noxious stimulus | Plantar flexion of toes | Babinski sign = extension of great toe + fanning of other toes → UMN lesion above S1 |
| Superficial abdominal | Stroke abdomen diagonally near umbilicus | Umbilicus pulls toward stimulated quadrant | Absent with UMN lesion; helps localize spinal level (T9–T12) |
| Cremasteric | Stroke medial thigh | Ipsilateral testicular elevation | Absent with L1–L2 or UMN lesion |
| Anal | Scratch perianal skin | Anal sphincter contraction | Absent → S2–S4 injury or cord lesion |
Primitive (Frontal Release) Reflexes
Normally absent in adults; reappear with frontal lobe disease:
| Reflex | Stimulus | Response |
|---|---|---|
| Suck | Light touch center of lips with tongue blade | Sucking movement |
| Root | Touch corner of lips | Mouth turns toward stimulus |
| Grasp | Touch palm between thumb and index finger | Patient grabs examiner's hand |
| Palmomental | Scratch palm diagonally | Ipsilateral chin muscle (mentalis) contraction |
Summary: UMN vs. LMN Pattern
| Feature | UMN Lesion | LMN Lesion |
|---|---|---|
| Tone | Increased (spasticity) | Decreased (flaccidity) |
| Reflexes | Hyperreflexia, clonus | Hyporeflexia / areflexia |
| Babinski | Positive (extensor) | Absent (normal plantar flexion) |
| Atrophy | Minimal | Significant, early |
| Fasciculations | Absent | Present |
| Weakness pattern | Pyramidal distribution | Segmental / dermatomal |
Sources: Harrison's Principles of Internal Medicine 22E, pp. 3424–3425 · Bradley and Daroff's Neurology in Clinical Practice · Textbook of Family Medicine 9e, p. 1214 · Adams and Victor's Principles of Neurology, 12th Edition, p. 174
This is a shared conversation. Sign in to Orris to start your own chat.