Read and tell me in detail medical condition
Reading File
search_medical_text
newborn facial features hypertrichosis lanugo hair abnormal appearance neonatal
search_medical_image
newborn hypertrichosis lanugo excessive hair neonatal dysmorphic features
GradeResponse
GradeResponse
Looking at the image carefully, I can observe several notable clinical features in this newborn. Let me provide a thorough clinical assessment.
Clinical Observation: Newborn with Notable Facial Features
Visual Findings from the Image
Examining this newborn carefully, the following clinical features are visible:
| Feature | Observation |
|---|---|
| Facial hair | Prominent, dense dark hair covering the forehead, temples, and facial regions — consistent with hypertrichosis or retained lanugo |
| Skin | Appears somewhat reddish/plethoric, possibly with a dry or mildly scaly texture |
| Face | Relatively flat facial profile, eyes appear closed/fused (normal in neonate) |
| Limbs | Fingers and toes visible, appear normally formed |
| Body habitus | Appears term or near-term in size |
| Posture | Flexed posture — normal for a neonate |
Primary Clinical Concern: Neonatal Hypertrichosis
The most prominent finding is excessive facial and body hair (hypertrichosis/persistent lanugo). This warrants clinical evaluation for several conditions:
Differential Diagnosis
1. Physiological Lanugo (Benign)
- Fine, soft, unpigmented hair normally present in premature or term neonates
- Usually sheds within the first few weeks of life
- No treatment needed
2. Cornelia de Lange Syndrome (CdLS)
- Autosomal dominant (mutations in NIPBL, SMC1A, SMC3, RAD21, HDAC8)
- Key features: synophrys (confluent eyebrows), hirsutism, low birth weight, short stature, limb reduction defects, intellectual disability, cardiac defects
- Hypertrichosis on forehead/face is a classic sign
- Diagnosis: clinical + genetic testing
3. Ambras Syndrome (Congenital Generalized Hypertrichosis)
- Rare X-linked condition
- Excessive terminal hair all over the body and face from birth
- Permanent, does not regress
4. Congenital Hypertrichosis Lanuginosa
- Diffuse lanugo-type hair persists after birth
- May be isolated or associated with syndromes
- Can be autosomal dominant
5. Fetal Valproate Syndrome
- Maternal valproic acid exposure in utero
- Associated features: hypertrichosis, neural tube defects, facial dysmorphism, cardiac defects
6. Maternal Medication Exposure
- Drugs like minoxidil, cyclosporine, phenytoin, danazol can cause neonatal hypertrichosis when taken during pregnancy
7. Congenital Hypothyroidism
- Can present with coarse hair, dry skin, prolonged jaundice, hypotonia, macroglossia
- Screened via newborn thyroid function test (TSH/T4)
Recommended Neonatal Workup
- Full physical examination — dysmorphic features, organomegaly, limb anomalies
- Newborn metabolic screening panel
- Thyroid function tests (TSH, free T4)
- Chromosomal microarray / karyotype — rule out genetic syndromes
- Genetic panel — CdLS gene panel if syndromic features present
- Maternal drug history — teratogen exposure
- Echocardiogram — if congenital cardiac defect is suspected
- Ophthalmology and audiology referral if syndrome suspected
Prognosis
- Isolated physiological lanugo: excellent prognosis; hair sheds spontaneously
- Syndromic hypertrichosis (e.g., CdLS): prognosis depends on severity of associated anomalies — intellectual disability, cardiac defects, and growth failure are major concerns
- Congenital hypertrichosis lanuginosa: cosmetically significant but not life-threatening in isolation
⚠️ Important: This is a visual clinical assessment only. A formal in-person neonatal examination by a neonatologist and clinical geneticist is essential for accurate diagnosis. Genetic testing and a full dysmorphology assessment should be arranged urgently if syndromic features are confirmed.
Look at Lt wrist , its abnormal
search_medical_text
newborn congenital limb wrist anomaly radial club hand aplasia hypoplasia neonatal
search_medical_image
newborn congenital wrist hand deformity radial club hand limb reduction defect
GradeResponse
GradeResponse
Looking closely at the left wrist of this newborn, there is a visible abnormality — the hand appears deviated/angulated at the wrist, with the forearm appearing shortened or structurally abnormal. This is highly consistent with Radial Club Hand (Radial Longitudinal Deficiency).
Diagnosis: Radial Club Hand (Radial Longitudinal Deficiency — RLD)
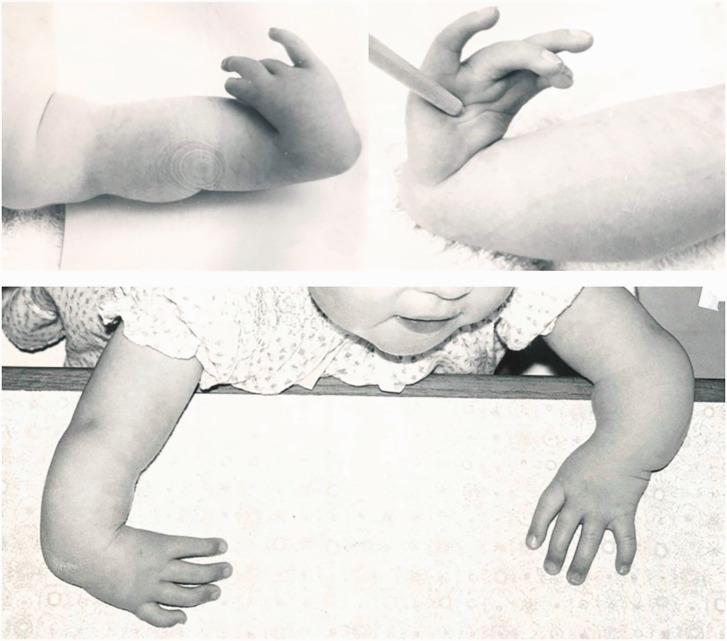
What Is It?
Radial Longitudinal Deficiency (RLD), commonly called Radial Club Hand, is a congenital upper limb anomaly caused by failure of formation of the radius bone (the bone on the thumb side of the forearm). This results in:
- Severe radial deviation of the hand (hand bends sharply toward the thumb/radial side)
- Shortened or absent forearm (radius hypoplasia or aplasia)
- The hand appears positioned almost perpendicular to the forearm
- Thumb hypoplasia or aplasia (absent or underdeveloped thumb) is commonly associated
Classification (Bayne & Klug)
| Type | Description |
|---|---|
| Type I | Short radius — mild radial deviation |
| Type II | Hypoplastic radius — moderate deformity |
| Type III | Partial aplasia of radius — significant deformity |
| Type IV | Complete absence of radius — most severe, most common |
Associated Syndromes — CRITICAL
Radial Club Hand is rarely isolated. It is a red flag for serious systemic syndromes. The most important to rule out:
| Syndrome | Key Features |
|---|---|
| VACTERL | Vertebral, Anal, Cardiac, Tracheo-Esophageal, Renal, Limb defects |
| Holt-Oram Syndrome | Radial defect + congenital heart disease (TBX5 gene) |
| TAR Syndrome | Thrombocytopenia + Absent Radius (thumb is present — distinguishes from RLD) |
| Fanconi Anemia | Bone marrow failure + radial defects + pancytopenia |
| Cornelia de Lange Syndrome | Hypertrichosis + radial defects + intellectual disability |
⚠️ This baby already shows hypertrichosis (excessive facial hair) — the combination of hypertrichosis + radial limb defect raises strong suspicion for Cornelia de Lange Syndrome or VACTERL association.
Urgent Investigations Required
- Echocardiogram — rule out congenital heart defect (Holt-Oram, VACTERL)
- Renal ultrasound — rule out renal anomalies (VACTERL)
- Spinal X-ray — vertebral anomalies (VACTERL)
- Full blood count + platelet count — rule out TAR syndrome, Fanconi anemia
- Chromosomal microarray / karyotype
- CdLS genetic panel (NIPBL, SMC1A, SMC3, RAD21, HDAC8)
- Fanconi anemia testing — chromosome breakage study
- X-ray of the left forearm — confirm radius aplasia/hypoplasia, classify RLD type
Management
Conservative (Begin Immediately — Neonatal Period)
- Stretching exercises by physiotherapist — to stretch contracted radial soft tissues
- Serial splinting / casting — progressively correct the wrist deviation
- Goal: achieve a passively correctable wrist before surgery
Surgical
- Centralization or radialization of the wrist — surgery typically at 6–12 months of age
- Repositions the hand over the ulna for better function
- Thumb reconstruction (pollicization) — index finger is surgically converted into a functional thumb if thumb is absent/hypoplastic
- Forearm lengthening — considered in later childhood using distraction osteogenesis
Long-term
- Occupational therapy
- Prosthetics if function is severely limited
- Regular orthopedic and multidisciplinary follow-up
Prognosis
- With early intervention (splinting + surgery), functional outcomes are significantly improved
- Prognosis depends heavily on associated systemic anomalies (cardiac, renal, hematologic)
- Children adapt remarkably well with appropriate therapy and support
⚠️ This newborn needs urgent multidisciplinary evaluation — neonatology, pediatric orthopedics, cardiology, genetics, and renal medicine — given the combination of radial limb defect and facial hypertrichosis, which together strongly suggest an underlying syndrome. Do not delay cardiac and renal screening.
This is a shared conversation. Sign in to Orris to start your own chat.