Laboratory and Instrumental methods for diagnosing infiltrative syndrome
Reading File
Infiltrative syndrome (mainly pulmonary infiltration) is diagnosed by combining laboratory evidence of inflammation/infection or systemic disease with imaging and sometimes invasive procedures.
1) Laboratory methods
A. Basic blood tests
- CBC with differential
- Leukocytosis + neutrophilia: often bacterial process
- Lymphocytosis: more often viral/atypical
- Eosinophilia: eosinophilic lung disease, parasitic/drug-related
- ESR, CRP
- Nonspecific inflammatory activity markers
- Procalcitonin
- Higher values support bacterial infection (helps antibiotic decisions)
B. Microbiologic tests
- Sputum microscopy (Gram stain), culture, sensitivity
- Acid-fast bacilli smear/culture/PCR when TB suspected
- Blood cultures in febrile/severe cases
- Nasopharyngeal PCR panels for respiratory viruses/atypicals
- Urinary antigens (e.g., pneumococcus, Legionella in selected settings)
C. Gas exchange and severity assessment
- Pulse oximetry (SpO₂)
- Arterial blood gas (ABG) for hypoxemia/hypercapnia, respiratory failure severity
D. Etiology-oriented/immunologic tests (when indicated)
- Fungal biomarkers/serology (e.g., galactomannan, β-D-glucan in risk groups)
- Autoimmune panel (ANA, ANCA, anti-GBM, RF, etc.) if vasculitis/connective tissue disease suspected
- Total/specific IgE, eosinophil profile in allergic/eosinophilic infiltration
- D-dimer only in proper thromboembolic diagnostic pathways (not for routine pneumonia workup)
2) Instrumental methods
A. First-line imaging
- Chest X-ray (PA/lateral)
- Detects focal, segmental, lobar, diffuse infiltrates
- Monitors dynamics during treatment
- Lung ultrasound (LUS)
- Subpleural consolidations, B-lines, pleural effusion
- Useful bedside/ICU tool
B. Advanced imaging
- Chest CT (preferably HRCT when interstitial process suspected)
- Better characterization of infiltrate pattern:
- ground-glass opacity
- consolidation
- nodules/tree-in-bud
- cavitation
- interstitial/reticular change
- Better characterization of infiltrate pattern:
- CT pulmonary angiography (CTPA)
- If pulmonary embolism with infarction is a differential
- MRI
- Limited pulmonary role; useful for mediastinal/chest wall assessment in selected cases
C. Endoscopic/invasive diagnostics
- Bronchoscopy with bronchoalveolar lavage (BAL)
- Cytology + microbiology (bacteria, fungi, mycobacteria, PCR)
- Especially for nonresolving, atypical, immunocompromised cases
- Transbronchial or CT-guided lung biopsy
- For unclear infiltrates, suspected malignancy, organizing pneumonia, ILD, granulomatous disease
- Pleural puncture/thoracentesis (if effusion present)
- Biochemistry, cytology, microbiology
D. Functional studies (adjunctive)
- Spirometry/PFTs, DLCO for chronic/interstitial infiltrative diseases
- ECG/Echocardiography to distinguish cardiogenic edema from pulmonary inflammatory infiltration
3) Practical diagnostic algorithm (short)
- Clinical exam + SpO₂
- CBC, CRP/ESR ± procalcitonin
- Chest X-ray
- If severe/unclear/atypical or poor response: CT chest
- Parallel etiologic workup: sputum/blood cultures, PCR, TB tests, targeted serology
- If still undiagnosed: bronchoscopy with BAL ± biopsy
4) Key differential diagnoses of “infiltrative shadow”
- Infectious pneumonia (bacterial/viral/fungal/TB)
- Pulmonary edema (cardiogenic/noncardiogenic)
- Pulmonary hemorrhage
- Interstitial lung disease/organizing pneumonia
- Neoplasm (including lepidic adenocarcinoma, lymphoma)
- Eosinophilic lung disease
- Pulmonary infarction
If you want, I can convert this into:
- a table by cause vs recommended tests, or
- a stepwise protocol for adults vs children.
Xray findings
search_medical_image
chest X-ray infiltrative syndrome radiological findings consolidation ground glass
search_medical_text
chest X-ray findings infiltrative syndrome pulmonary infiltration radiological signs
GradeResponse
GradeResponse
Here is a comprehensive overview of X-ray findings in infiltrative syndrome:
Chest X-Ray Findings in Infiltrative Syndrome
Core Radiological Signs
| Sign | Description | Typical Association |
|---|---|---|
| Consolidation | Homogeneous opacity that obscures vessels; air bronchograms often visible | Bacterial pneumonia, organizing pneumonia |
| Ground-glass opacity (GGO) | Hazy increased opacity; vessels still visible through it | Viral pneumonia (e.g., COVID-19), early PCP, cardiogenic edema |
| Air bronchogram | Air-filled bronchi visible within consolidated lung | Confirms alveolar filling (infection, edema, hemorrhage) |
| Reticulonodular pattern | Fine net-like + nodular shadowing | Interstitial infiltration, TB, fungal, sarcoidosis |
| Lobar/segmental opacity | Opacity confined to a lobe or segment | Classical bacterial lobar pneumonia |
Distribution Patterns and Their Significance
| Distribution | Likely Cause |
|---|---|
| Unilateral, lobar/segmental | Bacterial pneumonia (e.g., pneumococcal), aspiration |
| Bilateral lower zone + perihilar ("bat wing") | Cardiogenic pulmonary edema |
| Bilateral peripheral/subpleural + lower zones | Viral pneumonia (COVID-19, influenza), eosinophilic pneumonia |
| Upper lobe predominance | Tuberculosis (primary or reactivation), silicosis |
| Diffuse bilateral | ARDS, hematogenous spread, miliary TB |
| Hilar-peribronchial | Sarcoidosis, lymphoma, atypical pneumonia |
Additional Associated Findings
- Pleural effusion — suggests parapneumonic effusion, empyema, or heart failure
- Hilar lymphadenopathy — TB, sarcoidosis, lymphoma, fungal
- Cavitation within infiltrate — abscess, necrotizing pneumonia, TB, Klebsiella, aspergillosis
- Kerley B lines (short horizontal lines at lung periphery) — interstitial edema, lymphatic engorgement
- Cardiomegaly (cardiothoracic ratio > 0.5) — cardiogenic infiltration origin (Harrison's, p. 7154)
- Upper zone vascular redistribution — early sign of elevated pulmonary capillary wedge pressure
Classic Example: Bilateral Viral Pneumonia (COVID-19)
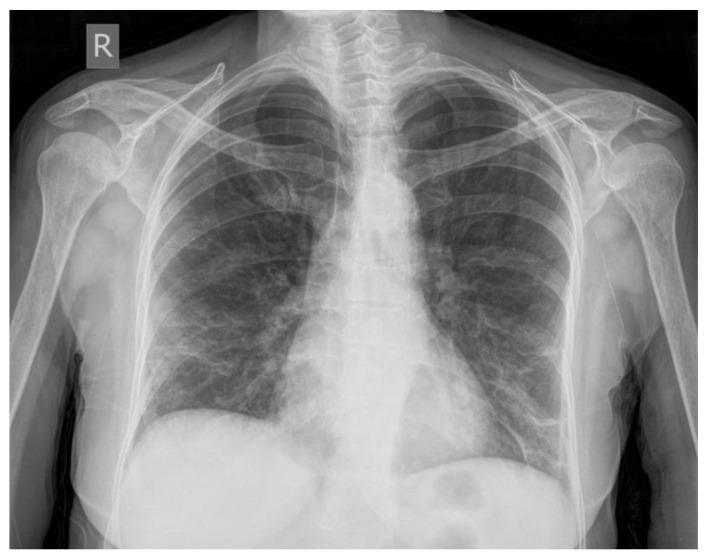
AP chest X-ray: diffuse bilateral ground-glass opacities and consolidations predominantly in the lower lobes and peripheral/subpleural regions. Reticulonodular interstitial changes visible. Cardiac silhouette normal — excludes cardiogenic etiology.
Practical Interpretation Tips
- Always assess distribution first (unilateral/bilateral, upper/lower, central/peripheral)
- Check for air bronchograms — confirms alveolar rather than atelectatic process
- Compare with prior films — dynamic changes guide diagnosis (rapid spread = ARDS/infection; slow = malignancy/ILD)
- Negative X-ray does not exclude early infiltration — HRCT is significantly more sensitive, especially for early interstitial disease and PCP
- Clinical correlation is mandatory — cardiogenic and infectious infiltrates can appear identical on plain film
Would you like HRCT patterns for infiltrative syndrome next?
This is a shared conversation. Sign in to Orris to start your own chat.