Differential diagnostic criteria for pneumonia and pulmonary infarction.
Reading File
search_medical_text
differential diagnosis pneumonia vs pulmonary infarction clinical features
search_medical_text
pulmonary infarction imaging findings chest X-ray CT diagnosis
search_medical_image
pneumonia vs pulmonary infarction chest X-ray Hampton hump consolidation
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive differential diagnostic framework for pneumonia vs. pulmonary infarction:
Differential Diagnosis: Pneumonia vs. Pulmonary Infarction
Clinical Presentation
| Feature | Pneumonia | Pulmonary Infarction (PE + Infarct) |
|---|---|---|
| Onset | Subacute to gradual (hours–days) | Sudden, often abrupt |
| Chest pain | Pleuritic, localized | Pleuritic or crushing; may radiate to shoulder/supraclavicular area |
| Dyspnea | Present, proportional to consolidation | Often disproportionate to radiographic findings |
| Cough | Productive; purulent, rusty, or blood-tinged sputum | Non-productive or hemoptysis (frank blood) |
| Fever | High-grade, often with chills/rigors | Low-grade or absent (fever >39°C makes infarction less likely) |
| Hemoptysis | Uncommon; if present, mixed with purulent sputum | More characteristic; bright red blood |
| Tachycardia | Present | Often prominent, out of proportion to fever |
| Pleuritic referred pain | May refer to right upper quadrant or subscapular region via diaphragmatic pleuritis | Same pattern — diaphragmatic pleuritis from infarction mimics biliary pain (Harrison's, p. 560) |
| Risk factors | URI prodrome, immunosuppression, alcohol, aspiration, elderly | DVT history, immobility, surgery, OCP, malignancy, hypercoagulable state |
| Leg swelling/DVT signs | Absent | Present in ~50% of cases |
Laboratory Findings
| Test | Pneumonia | Pulmonary Infarction |
|---|---|---|
| WBC | Elevated (neutrophilia, often >15,000) | Normal or mildly elevated |
| CRP / Procalcitonin | Markedly elevated | Mildly elevated or normal |
| D-dimer | May be mildly elevated (non-specific) | Elevated (sensitive but non-specific) |
| Sputum culture | May identify pathogen | Sterile |
| Blood cultures | May be positive in bacteremic pneumonia | Negative |
| ABG / SpO₂ | Hypoxemia with hypercapnia possible | Hypoxemia + hypocapnia (respiratory alkalosis) |
| Troponin / BNP | Normal | May be elevated in massive PE with RV strain |
| ECG | Non-specific | S1Q3T3 pattern, sinus tachycardia, new RBBB, RV strain |
Imaging
Chest X-Ray
| Finding | Pneumonia | Pulmonary Infarction |
|---|---|---|
| Opacity pattern | Lobar/segmental consolidation, often central-to-peripheral | Peripheral wedge-shaped opacity, pleural-based |
| Air bronchograms | Present (key distinguishing sign) | Absent (Harrison's, p. 8247) |
| Hampton's Hump | Not seen | Classic: wedge-shaped pleural-based opacity with convex apex toward the hilum |
| Westermark sign | Absent | Regional vascular oligemia (focal hyperlucency) |
| Pleural effusion | Exudative; parapneumonic or empyema | Small hemorrhagic effusion; tracks into fissures |
| Pulmonary artery | Normal | Enlarged (Fleischner sign) possible |
| Distribution | Any lobe; lower lobes predominate | Lower lobes, peripherally; right > left |
Hampton's Hump — Classic Pulmonary Infarction Radiograph:
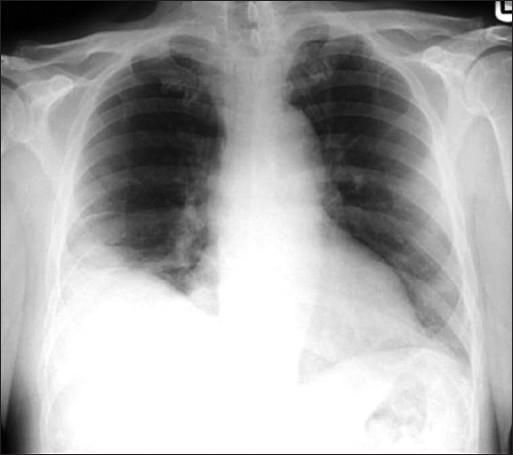
AP chest X-ray demonstrating Hampton's Hump: a wedge-shaped, pleural-based opacity in the right lower zone with convex apex toward the hilum. No air bronchograms are visible. A small right pleural effusion with blunting of the costophrenic angle is present. Left lung is clear. (Source: PMC Clinical VQA)
CT Findings
| Feature | Pneumonia | Pulmonary Infarction |
|---|---|---|
| CT chest (parenchyma) | Ground-glass or consolidative opacity; air bronchograms; tree-in-bud for bronchopneumonia | Peripheral wedge-shaped consolidation, no air bronchograms |
| CT pulmonary angiogram | Normal vasculature | Filling defect in pulmonary artery (diagnostic for PE) |
| Enhancement pattern | Consolidated areas enhance with contrast | Infarcted segments may show no enhancement |
Distinguishing Diagnostic Clues (Summary)
| Criterion | Favors Pneumonia | Favors Pulmonary Infarction |
|---|---|---|
| Air bronchograms on CXR/CT | ✅ Present | ❌ Absent |
| Hampton's Hump | ❌ Absent | ✅ Present |
| High fever (>38.5°C) | ✅ | ❌ |
| DVT signs / PE risk factors | ❌ | ✅ |
| Productive purulent cough | ✅ | ❌ |
| Disproportionate hypoxemia | ❌ | ✅ |
| Elevated D-dimer + low procalcitonin | ❌ | ✅ |
| Hypocapnia on ABG | ❌ | ✅ |
| CTA pulmonary filling defect | ❌ | ✅ (diagnostic) |
| Sputum/blood cultures positive | Possible | ❌ |
Key Caveat
These two conditions can coexist — pulmonary infarction can become superinfected and present with a clinical picture indistinguishable from pneumonia (so-called "infarct pneumonia"). Diaphragmatic pleuritis from either condition may also mimic acute abdominal pathology (right upper quadrant or subscapular pain), which can delay the diagnosis (Harrison's, p. 560).
When clinical uncertainty persists, CTPA is the definitive test to exclude pulmonary embolism with infarction, while sputum culture + procalcitonin support or refute an infectious etiology.
This is a shared conversation. Sign in to Orris to start your own chat.