Pulmonary infiltrate syndrome
Reading File
search_medical_text
pulmonary infiltrate syndrome etiology classification clinical presentation
search_medical_text
pulmonary infiltrates diagnosis differential management treatment
search_medical_image
pulmonary infiltrates chest X-ray CT imaging patterns
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive overview of Pulmonary Infiltrate Syndrome.
Pulmonary Infiltrate Syndrome
Definition
Pulmonary infiltrate syndrome refers to the constellation of clinical and radiographic findings resulting from material (fluid, cells, protein, or organisms) filling or replacing normal air spaces and/or interstitium of the lung. It is not a single disease but a syndromic presentation — a sign with many causes — characterized by:
- Radiographic infiltrates on chest X-ray or CT (opacities, consolidation, ground-glass changes)
- Respiratory symptoms (cough, dyspnea, chest pain)
- Physiologic impairment (hypoxia, reduced gas exchange)
Pathophysiologic Categories of Infiltrates
| Pattern | Mechanism | Examples |
|---|---|---|
| Alveolar (airspace) | Fluid/cells fill alveoli | Pneumonia, pulmonary edema, DAH, ARDS |
| Interstitial | Thickening of alveolar walls/septa | ILD, viral pneumonia, lymphangitic carcinomatosis |
| Mixed alveolar-interstitial | Both components | Atypical pneumonia, drug toxicity |
| Eosinophilic | Eosinophil-predominant infiltration | Eosinophilic pneumonia, drug reaction, parasitic infection |
| Nodular | Discrete nodules/masses | Fungal infection, malignancy, sarcoidosis |
Etiology — Major Causes
1. Infectious
- Bacterial: Streptococcus pneumoniae, Staphylococcus aureus, gram-negative bacilli, Legionella, Mycoplasma pneumoniae
- Viral: Influenza, SARS-CoV-2, CMV, RSV
- Fungal: Aspergillus, Pneumocystis jirovecii (PCP), Histoplasma, Cryptococcus
- Parasitic: Löffler syndrome, pulmonary larva migrans
2. Non-infectious Inflammatory
- Hypersensitivity pneumonitis (extrinsic allergic alveolitis)
- Eosinophilic pneumonia (acute or chronic)
- Sarcoidosis
- Connective tissue disease-associated ILD (RA, SLE, SSc)
- Cryptogenic organizing pneumonia (COP/BOOP)
3. Vascular / Hemodynamic
- Cardiogenic pulmonary edema
- Non-cardiogenic pulmonary edema (ARDS)
- Diffuse alveolar hemorrhage (DAH)
- Pulmonary infarction post-embolism
- Acute chest syndrome (in sickle cell disease)
4. Drugs and Toxins
A broad range of medications cause pulmonary infiltrates, particularly with peripheral eosinophilia (Harrison's, p. 7968). Common culprits include:
- NSAIDs
- Systemic antibiotics (nitrofurantoin, sulfonamides)
- Amiodarone, methotrexate, bleomycin
- Inhaled drugs of abuse
- Radiation therapy (e.g., post-breast cancer RT → eosinophilic infiltration)
5. Malignancy
- Bronchoalveolar carcinoma (now called lepidic-predominant adenocarcinoma)
- Lymphangitic carcinomatosis
- Lymphoma
6. Miscellaneous
- Aspiration pneumonitis/pneumonia
- Alveolar proteinosis
- Lipoid pneumonia
Radiographic Patterns and Imaging
The chest X-ray and CT scan are central to characterizing infiltrates.
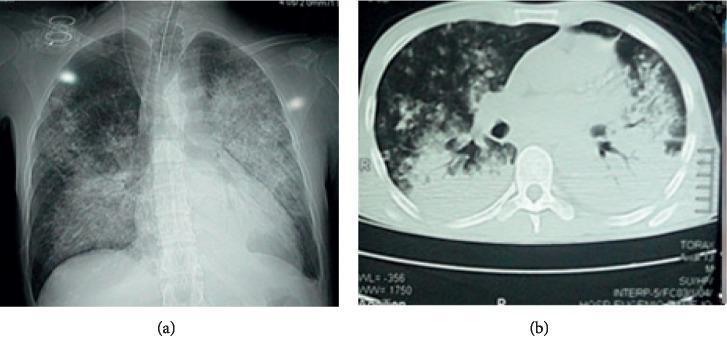
AP chest X-ray (left) showing diffuse bilateral alveolar opacities with basal predominance and relative apical sparing. Axial CT (right) demonstrating bilateral ground-glass opacities and consolidation in perihilar and posterior/basal regions — consistent with ARDS, pulmonary edema, or diffuse alveolar hemorrhage.
Key Imaging Patterns
| CT Pattern | Typical Associations |
|---|---|
| Ground-glass opacity (GGO) | Pulmonary edema, viral pneumonia, PCP, early ILD |
| Consolidation | Bacterial pneumonia, organizing pneumonia, DAH |
| Reticular/honeycombing | Fibrotic ILD, UIP pattern |
| Nodular | Fungal, mycobacterial, sarcoidosis, metastases |
| Crazy-paving | Alveolar proteinosis, COVID-19, Pneumocystis |
| Peripheral GGO + consolidation | Eosinophilic pneumonia, COP |
| Bilateral perihilar "bat-wing" | Pulmonary edema, ARDS |
Distribution Clues
- Basal/peripheral: Aspiration, COP, eosinophilic pneumonia
- Upper lobe: TB, hypersensitivity pneumonitis (chronic), sarcoidosis
- Perihilar/central: Pulmonary edema, sarcoidosis, PCP
- Random: Hematogenous spread, miliary TB
Clinical Presentation
Cardinal Features
| Feature | Details |
|---|---|
| Cough | Productive (bacterial) or dry (atypical/viral) |
| Dyspnea | Ranges from exertional to rest |
| Fever/chills | Suggests infection; may be absent in immunocompromised |
| Chest pain | Pleuritic (pneumonia, PE) or retrosternal |
| Hemoptysis | Suggests DAH, TB, necrotizing pneumonia, malignancy |
| Hypoxia | O₂ saturation <95% indicates significant disease |
Diagnostic Approach
Step-by-Step Workup
- History: Travel, exposures (animals, birds, dusts), medications, immunocompromise, HIV status, smoking, occupation
- Chest X-ray: First-line; establish pattern and distribution
- HRCT chest: Superior for characterizing infiltrate pattern, distribution, and associated findings
- Blood tests:
- CBC (eosinophilia → eosinophilic syndrome, drug reaction)
- Blood cultures (bacteremia)
- Procalcitonin, CRP, ESR
- LDH (elevated in PCP, lymphoma)
- BNP/NT-proBNP (cardiogenic edema)
- ANA, ANCA, anti-GBM (for autoimmune/DAH)
- Sputum: Gram stain, culture, AFB, fungal stains
- Bronchoalveolar lavage (BAL): Crucial for immunocompromised; cytology, cultures, hemosiderin-laden macrophages (DAH)
- Lung biopsy: Transbronchial or surgical, when non-invasive workup is unrevealing
- Echocardiogram: Evaluate for cardiac cause of pulmonary edema
Prioritizing the Differential
| Clinical Context | Leading Diagnoses |
|---|---|
| Immunocompetent + fever + acute | Community-acquired pneumonia |
| HIV/immunocompromised | PCP, CMV, fungal, atypical mycobacteria |
| Eosinophilia + infiltrates | Drug reaction, eosinophilic pneumonia, parasites |
| Sickle cell disease | Acute chest syndrome (Harrison's, p. 2920) |
| Drug history | Drug-induced pneumonitis |
| Exposure to mold/birds/hay | Hypersensitivity pneumonitis |
| Bilateral + acute + ICU | ARDS |
Management Principles
Management is directed by the underlying cause:
Infectious
- Community-acquired pneumonia: Beta-lactam ± macrolide (or fluoroquinolone monotherapy)
- Hospital-acquired/VAP: Broad-spectrum coverage (anti-pseudomonal ± MRSA coverage)
- PCP: High-dose TMP-SMX; adjuvant steroids if PaO₂ < 70 mmHg
- Fungal: Azoles or amphotericin B depending on organism
Inflammatory / Drug-Induced
- Discontinue offending drug (mainstay for drug-induced — Harrison's, p. 7968)
- Corticosteroids: First-line for eosinophilic pneumonia, COP, hypersensitivity pneumonitis (acute), DAH
Hemodynamic / Vascular
- Cardiogenic pulmonary edema: Diuresis, afterload reduction, treat underlying cardiac cause
- ARDS: Lung-protective ventilation (TV 6 mL/kg IBW, plateau pressure <30 cmH₂O), prone positioning, conservative fluids
Acute Chest Syndrome (Sickle Cell)
- Supplemental O₂ for SpO₂ <95%
- Empiric antibiotics (even if no clear organism)
- Avoid overhydration and excessive opioids
- Exchange transfusion for severe cases with rapid progression (Harrison's, p. 2920)
Supportive
- Supplemental oxygen (target SpO₂ ≥92–95%)
- Bronchodilators if bronchospasm component
- ICU admission for severe hypoxia, multiorgan involvement
Complications
- Respiratory failure requiring mechanical ventilation
- ARDS
- Septicemia / multiorgan failure
- Lung abscess or empyema (in necrotizing pneumonia)
- Pulmonary fibrosis (late sequela of severe or chronic infiltrative processes)
- Death (especially in immunocompromised or severe ARDS)
Summary
Pulmonary infiltrate syndrome is a syndromic framework encompassing a wide etiologic spectrum. The key clinical task is to characterize the infiltrate (pattern, distribution, acuity, associated findings) and contextualize it within the patient's clinical profile (immune status, medications, exposures, comorbidities) to arrive at the correct diagnosis and target therapy effectively.
This is a shared conversation. Sign in to Orris to start your own chat.