Potts fracture
Reading File
search_medical_text
Potts fracture ankle classification mechanism presentation
search_medical_image
Potts fracture ankle bimalleolar trimalleolar X-ray
GradeResponse
GradeResponse
The text retrieval was limited, so I'll supplement with my comprehensive knowledge on this topic.
Potts Fracture
Definition
A Potts fracture (also called Pott's fracture) is a fracture-dislocation of the ankle involving the distal fibula (lateral malleolus), classically associated with disruption of the ankle mortise. The term is often used loosely to describe bimalleolar or trimalleolar ankle fractures with ligamentous injury, named after Sir Percivall Pott (18th century), who sustained and described such an injury himself.
Anatomy Relevant to the Injury
The ankle mortise is formed by three bony structures:
- Medial malleolus (distal tibia)
- Lateral malleolus (distal fibula)
- Posterior malleolus (posterior tibial lip)
Stability depends on both the bony mortise and the ligamentous complex (deltoid ligament medially; ATFL, CFL, PTFL laterally; syndesmotic ligaments).
Mechanism of Injury
| Mechanism | Injury Pattern |
|---|---|
| Forced eversion/external rotation | Lateral malleolus fracture ± medial disruption |
| Pronation-abduction | Transverse fibula fracture at/above syndesmosis |
| High-energy trauma | Trimalleolar fracture-dislocation |
The classic Potts mechanism is forced eversion causing the talus to lever against the lateral malleolus, fracturing it, while the deltoid ligament or medial malleolus fails on the tension side.
Classification
Lauge-Hansen Classification (mechanism-based)
| Type | Stages | Key Feature |
|---|---|---|
| Supination-Adduction (SA) | I–II | Transverse fibula fracture below syndesmosis |
| Supination-External Rotation (SER) | I–IV | Oblique/spiral fibula fracture at syndesmosis (most common, ~50–70%) |
| Pronation-Abduction (PA) | I–III | Comminuted fibula fracture at/above syndesmosis |
| Pronation-External Rotation (PER) | I–IV | High fibula fracture (Maisonneuve), syndesmotic disruption |
Danis-Weber Classification (fibula fracture level relative to syndesmosis)
| Type | Fibula Fracture Level | Syndesmosis | Stability |
|---|---|---|---|
| Weber A | Below syndesmosis | Intact | Usually stable |
| Weber B | At the level of syndesmosis | ± Injured | May be unstable |
| Weber C | Above syndesmosis | Disrupted | Unstable |
Clinical Presentation
- Pain, swelling, and bruising around the ankle
- Inability to bear weight
- Visible deformity if dislocated
- Tenderness over malleoli, syndesmosis, and/or medial structures
- Neurovascular compromise may occur with severe dislocation
Imaging
X-ray (first-line)
- AP, lateral, and mortise views of the ankle
- Assess: fibula fracture level, medial clear space (normal <4 mm), tibiofibular overlap, posterior malleolus fragment
The image below demonstrates a trimalleolar fracture-dislocation — the most severe form:
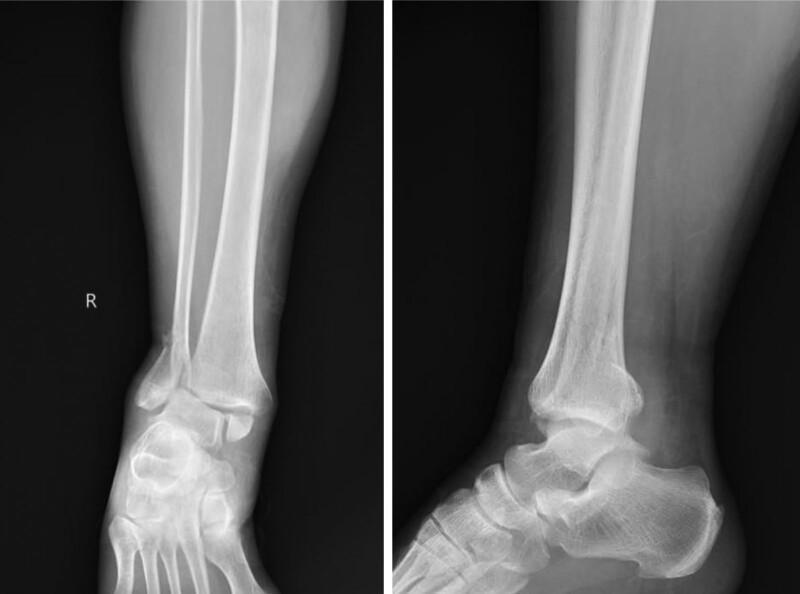
CT Scan
- Indicated for: posterior malleolus fractures (assess fragment size), pre-operative planning, suspected syndesmotic injury, pilon extension
Management
Non-Operative (Conservative)
Indications: stable, undisplaced fractures (typically Weber A, some Weber B)
- Below-knee cast or walking boot for 6 weeks
- Non-weight-bearing initially, progressive weight-bearing as tolerated
- Serial X-rays to confirm maintained reduction
Operative (ORIF)
Indications:
- Unstable fractures (widened mortise, Weber B/C with instability)
- Bimalleolar or trimalleolar fractures
- Displaced fractures
- Dislocation
Standard ORIF approach:
- Lateral malleolus: plate and screw fixation (1/3 tubular or locking plate)
- Medial malleolus: 2 partially threaded cancellous screws or tension band
- Posterior malleolus: fixation if >25–33% of articular surface involved
- Syndesmosis: syndesmotic screw if diastasis confirmed (intraoperative stress test)
Fracture-Dislocation (Emergency)
- Closed reduction immediately to relieve pressure on neurovascular structures and skin
- Post-reduction X-ray
- Definitive ORIF once swelling allows (usually 5–10 days)
Complications
| Complication | Notes |
|---|---|
| Post-traumatic osteoarthritis | Most common long-term complication; risk with articular incongruity |
| Malunion / nonunion | Especially medial malleolus; affects mortise congruity |
| Wound complications | Higher risk in diabetics, smokers, elderly |
| Syndesmotic malreduction | Leads to chronic instability and pain |
| Neurovascular injury | Superficial peroneal, sural nerve; peroneal artery in high-energy injuries |
| DVT / PE | Immobilization increases risk; prophylaxis indicated |
| Reflex Sympathetic Dystrophy (CRPS) | Uncommon but debilitating |
Prognosis
- Stable, isolated lateral malleolus fractures: excellent prognosis with conservative management
- Bimalleolar / trimalleolar fractures: good outcomes with anatomic ORIF, but ~20–40% develop some degree of post-traumatic arthritis
- Poor prognostic factors: older age, diabetes, obesity, articular comminution, delayed treatment
Key clinical pearl: A "Potts fracture" that appears isolated on X-ray may have medial ligamentous disruption — always assess the medial clear space on mortise view and perform stress testing if instability is suspected, as this changes management from conservative to operative.
This is a shared conversation. Sign in to Orris to start your own chat.