Use of NSAIDS drugs
Reading File
Finding Sources
Searching PubMed
"NSAIDs" AND "clinical use"
Finding Sources
Searching PubMed
"nonsteroidal anti-inflammatory drugs" AND "adverse effects"
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
I now have comprehensive information from multiple authoritative textbooks. Let me compile the complete answer.
NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) — A Comprehensive Overview
1. What Are NSAIDs?
NSAIDs are a chemically diverse group of drugs that share a common mechanism: inhibition of cyclooxygenase (COX) enzymes, blocking prostaglandin synthesis. They produce analgesic, antipyretic, and anti-inflammatory effects. — Miller's Anesthesia, 10e; Morgan & Mikhail's Clinical Anesthesiology, 7e
2. Mechanism of Action
The COX pathway is central to understanding NSAIDs:
| Enzyme | Nature | Key Functions |
|---|---|---|
| COX-1 | Constitutive (always present) | Gastric mucosal protection, platelet aggregation, hemostasis, renal perfusion |
| COX-2 | Inducible (upregulated by inflammation) | Pain, fever, inflammation; also vascular endothelial function |
- Non-selective NSAIDs (e.g., ibuprofen, naproxen, diclofenac, ketorolac, indomethacin) block both COX-1 and COX-2
- Selective COX-2 inhibitors (coxibs) (e.g., celecoxib, etoricoxib) preferentially block COX-2, sparing platelets and gastric mucosa
- Aspirin is unique: it irreversibly acetylates a serine residue on COX-1, causing platelet effects that last ~7–10 days (the lifespan of the platelet)
NSAIDs also exert analgesic effects via spinal COX inhibition, providing central as well as peripheral analgesia. — Miller's Anesthesia, 10e
COX inhibitors bind the active site of the enzyme. The COX-2 binding site is larger, allowing bulkier selective molecules (heterocyclics like celecoxib) to fit only there. — Morgan & Mikhail's Clinical Anesthesiology, 7e
3. Classification and Examples
| Class | Examples |
|---|---|
| Salicylic acids | Aspirin |
| Propionic acid derivatives | Ibuprofen, naproxen, ketoprofen |
| Acetic acid derivatives | Diclofenac, indomethacin, ketorolac |
| Oxicams | Piroxicam, meloxicam |
| Selective COX-2 inhibitors | Celecoxib, etoricoxib, parecoxib |
4. Pharmacokinetics
- Absorption: Most reach peak plasma concentrations within < 3 hours of oral dosing. Some are available as topical gels (joint/eye drops) or IV formulations (ketorolac, ibuprofen, diclofenac).
- Distribution: Highly bound to plasma proteins (mainly albumin). Lipid-soluble — penetrate the blood-brain barrier and joint spaces readily.
- Metabolism: Primarily hepatic biotransformation.
- Excretion: Renally eliminated after biotransformation. — Morgan & Mikhail's Clinical Anesthesiology, 7e
5. Clinical Indications
| Indication | Notes |
|---|---|
| Mild-to-moderate pain | Postoperative, musculoskeletal, dental, headache |
| Moderate-to-severe pain | Adjunct to opioids (opioid-sparing effect) |
| Fever | Antipyresis via COX inhibition |
| Inflammation | Arthritis (OA, RA), tendinitis, bursitis, gout |
| Dysmenorrhea | Highly effective |
| Pericarditis | NSAIDs (esp. ibuprofen + colchicine) are first-line (JAMA 2024) |
| Closure of PDA | IV indomethacin or ibuprofen in neonates |
| Cardiovascular prophylaxis | Low-dose aspirin only (irreversible COX-1 inhibition → anti-platelet) |
| Perioperative multimodal analgesia | Part of ERAS protocols — reduces opioid requirements |
Meta-analyses confirm that NSAIDs added to IV-PCA opioids significantly reduce nausea, vomiting, and sedation — without meaningful increases in pain scores. — Miller's Anesthesia, 10e
Relative Analgesic Efficacy (NNT for >50% pain relief in moderate–severe postoperative pain):
| Drug | NNT |
|---|---|
| Diclofenac 100 mg | 1.9 |
| Diclofenac 50 mg | 2.3 |
| Ibuprofen 600 mg | 2.4 |
| Ketorolac 10 mg | ~2.6 |
| Aspirin 1000 mg | 4.0 |
— Miller's Anesthesia, 10e, Table 77.2
6. Adverse Effects
A. Gastrointestinal (most common)
- Inhibition of COX-1 → reduced prostaglandin-mediated mucin/bicarbonate secretion, reduced mucosal blood flow → gastric and duodenal ulcers
- NSAIDs cause a 3–4× higher risk of peptic ulcer disease (PUD), independent of H. pylori
- NSAID-induced ulcers are more common in the stomach (Type V gastric ulcer = any location, associated with long-term NSAID use)
- NSAID enteropathy: small intestinal increased permeability, mucosal breaks, diaphragm-like strictures — seen in up to 70% of chronic NSAID users on capsule endoscopy
- Can cause iron-deficiency anemia, hypoalbuminemia, perforation, obstruction — Sabiston Surgery, 5e; Sleisenger & Fordtran's GI, 10e
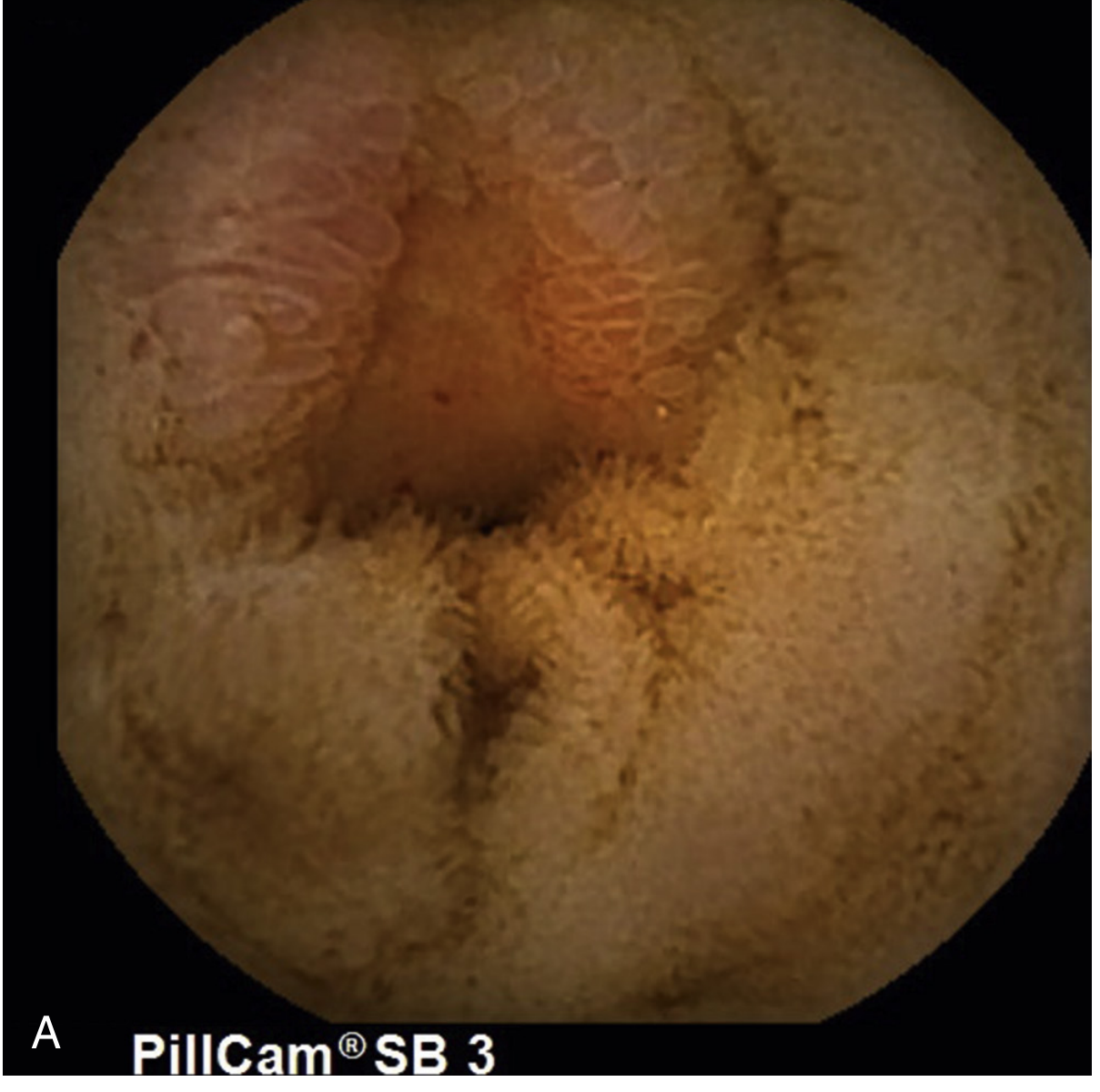
GI protection strategies:
- Add a proton pump inhibitor (PPI) or misoprostol in high-risk patients
- Use selective COX-2 inhibitors when GI protection is needed without antiplatelet effects
B. Cardiovascular
- All NSAIDs except low-dose aspirin increase risk of MI, stroke, and thrombosis
- Selective COX-2 inhibitors carry the highest CV risk: unchecked inhibition of vascular endothelial COX-2 → reduced prostacyclin (vasodilator/antiplatelet) while platelet thromboxane A2 (COX-1-mediated) is unaffected → pro-thrombotic state
- Aspirin paradox: low-dose aspirin is uniquely cardioprotective via irreversible COX-1 inhibition in platelets — Barash Clinical Anesthesia, 9e; Morgan & Mikhail, 7e
C. Renal
- NSAIDs block prostaglandin-mediated afferent arteriole vasodilation → reduced GFR
- High-risk groups: hypovolemia, heart failure, cirrhosis, diabetic nephropathy, pre-existing CKD, hypercalcemia
- Can precipitate acute kidney injury, sodium/water retention, hypertension
- Rarely: membranous glomerulopathy (nephrotic syndrome) — Morgan & Mikhail, 7e; Brenner & Rector's The Kidney
D. Platelet / Hematologic
- Non-selective NSAIDs: reversible platelet inhibition (resolves when drug clears)
- Aspirin: irreversible — hold 7–10 days before elective surgery
- Selective COX-2 inhibitors: no significant platelet effect (safe perioperatively)
E. Respiratory
- Aspirin-exacerbated respiratory disease (AERD): triad of asthma, nasal polyps, aspirin/NSAID sensitivity
- At therapeutic doses, no direct respiratory effects
F. Hepatic
- Generally mild; rare hepatotoxicity with some agents (e.g., diclofenac)
7. Contraindications
| Contraindication | Reason |
|---|---|
| Active peptic ulcer / GI bleeding | Worsens mucosal injury |
| Severe CKD or AKI | Loss of prostaglandin-dependent renal perfusion |
| Severe heart failure | Sodium retention, AKI risk |
| Aspirin-exacerbated respiratory disease | Bronchospasm risk |
| Third trimester of pregnancy | Premature ductus arteriosus closure, delayed labor; oligohydramnios |
| Perioperative period (selected surgeries) | Bleeding risk (non-selective agents) |
| Anticoagulant use | Additive bleeding risk |
2024 EULAR guidelines updated recommendations for antirheumatic drugs (including NSAIDs) in reproduction and pregnancy — NSAIDs should be avoided after 20 weeks gestation (PMID 40287311).
8. Drug Interactions
| Drug | Interaction |
|---|---|
| Warfarin / anticoagulants | Increased bleeding risk |
| ACE inhibitors / ARBs | Blunt antihypertensive effect; AKI in vulnerable patients |
| Diuretics | Blunt diuretic effect; sodium retention |
| Corticosteroids | Additive GI toxicity |
| Lithium | NSAIDs reduce lithium clearance → toxicity |
| Methotrexate | Reduced elimination → toxicity |
9. Selective COX-2 Inhibitors vs. Non-Selective NSAIDs
| Feature | Non-Selective NSAID | COX-2 Inhibitor |
|---|---|---|
| GI protection | ❌ Less protective | ✅ Better GI safety |
| Platelet effect | ❌ Inhibits platelet aggregation | ✅ No platelet effect |
| CV risk | Moderate | ⚠️ Higher (esp. rofecoxib, withdrawn) |
| Perioperative use | Use with caution | Safe (no bleeding risk) |
| Cost | Lower | Higher |
10. Topical NSAIDs
- Diclofenac gel/solution: useful for localized OA (knee) with minimal systemic absorption
- Reduced GI and cardiovascular risks compared to oral administration
Key Summary
NSAIDs are highly effective analgesics, anti-inflammatories, and antipyretics acting via COX inhibition. Their clinical use is limited by a well-characterized adverse effect profile:
- GI toxicity (ulcers, enteropathy) — use PPIs or COX-2 inhibitors to mitigate
- Cardiovascular risk — avoid in high CV risk; use lowest effective dose for shortest duration
- Renal impairment — avoid in CKD, hypovolemia, heart failure
- Aspirin stands apart: irreversible COX-1 inhibition makes it uniquely anti-platelet and cardioprotective at low doses
In perioperative settings, NSAIDs are a cornerstone of multimodal (opioid-sparing) analgesia, reducing opioid requirements and opioid-related side effects. — Miller's Anesthesia, 10e; Morgan & Mikhail's Clinical Anesthesiology, 7e; Sabiston Surgery, 5e; Sleisenger & Fordtran's GI Disease, 10e
This is a shared conversation. Sign in to Orris to start your own chat.