Thoracoplasty
Reading File
search_medical_text
thoracoplasty procedure indications technique complications
search_medical_image
thoracoplasty chest wall ribs surgery
GradeResponse
GradeResponse
The internal database returned no text results, so the answer below is drawn from comprehensive medical knowledge.
Thoracoplasty
Definition
Thoracoplasty is a surgical procedure involving the resection of multiple ribs (and sometimes their associated periosteum and intercostal bundles) to permanently collapse a portion of the chest wall, thereby obliterating an underlying space in the pleural cavity or lung.
Historical Background
Thoracoplasty was the cornerstone of tuberculosis (TB) surgery in the pre-antibiotic era (late 19th – mid 20th century). It was first systematized by de Cérenville (1885) and later refined by Alexander, Sauerbruch, and Schede. The principle was to collapse cavitary TB lesions by removing the bony support of the chest wall, thereby allowing the lung to "rest" and the cavity to close. With the advent of effective anti-TB chemotherapy in the 1950s–60s, its use declined dramatically but was never fully abandoned.
Indications
Historical (Classical)
- Pulmonary tuberculosis with large cavities unresponsive to collapse therapy (pneumothorax, pneumoperitoneum)
- Empyema thoracis with rigid, unyielding chest wall (Schede thoracoplasty)
Contemporary
| Indication | Details |
|---|---|
| Chronic empyema / bronchopleural fistula | Most common modern indication; obliterates the empyema space |
| Post-pneumonectomy space complications | Empyema or persistent space after pneumonectomy |
| Multidrug-resistant (MDR) / XDR tuberculosis | Adjunct to chemotherapy when cavities persist |
| Chest wall reconstruction | After tumor resection with significant chest wall defect |
| Thoracic scoliosis correction | Rib hump correction (costoplasty/thoracoplasty as component of spinal surgery) |
| Failed lung re-expansion | Residual pleural space after decortication or pulmonary resection |
Classification / Types
1. Extrapleural Thoracoplasty (Classic / Alexander type)
- Ribs resected outside the pleura; pleura left intact
- Aims to collapse underlying lung/cavity
- Usually performed in stages (2–3 sessions weeks apart) to avoid paradoxical respiration and respiratory failure
- Typically involves ribs 1–7 (upper lobe collapse) or specific segments
2. Intrapleural / Schede Thoracoplasty
- En-bloc resection of ribs, intercostal muscles, thickened parietal pleura, and sometimes the empyema wall
- Designed to obliterate a chronic empyema cavity
- More extensive; performed in a single stage
3. Tailoring / Limited Thoracoplasty
- Resection of only 1–3 ribs over a specific space
- Used after pulmonary resection to close residual apical spaces
- Less morbidity than classic thoracoplasty
4. Thoracoplasty with Muscle Flap (Modified)
- Combines rib resection with muscle transposition (latissimus dorsi, serratus anterior) to fill the dead space
- Preferred in bronchopleural fistula with contaminated spaces
Surgical Technique (Classical Extrapleural)
- Patient position: Lateral decubitus
- Incision: Posterior paravertebral incision (over erector spinae)
- Subperiosteal rib resection: Periosteum stripped, ribs excised in segments — typically starting at rib 1 (transverse process to costochondral junction)
- Number of ribs: Varies (commonly 3–8); determined by the extent of the space to be obliterated
- Staging: To prevent acute mediastinal shift and paradoxical motion, ribs may be resected in 2–3 sessions
- Closure: Drain placement; muscles closed in layers
Complications
Immediate / Early
- Paradoxical chest wall motion → respiratory failure (major risk when >4 ribs resected in one stage)
- Hemorrhage
- Pneumothorax / hemothorax
- Wound infection
Late
- Severe thoracic deformity (scoliosis, shoulder drop, rib crowding) — the most visible long-term consequence
- Chronic pain
- Brachial plexus injury (especially with 1st rib resection)
- Intercostal neuralgia
- Restrictive ventilatory defect — loss of chest wall compliance reduces total lung capacity (TLC) and FVC
- Cor pulmonale (in severe cases with significant lung reduction)
- Persistent or recurrent bronchopleural fistula
Postoperative Image
Below is a postoperative AP chest X-ray following thoracoplasty, showing titanium miniplates used for chest wall stabilization after reconstruction:
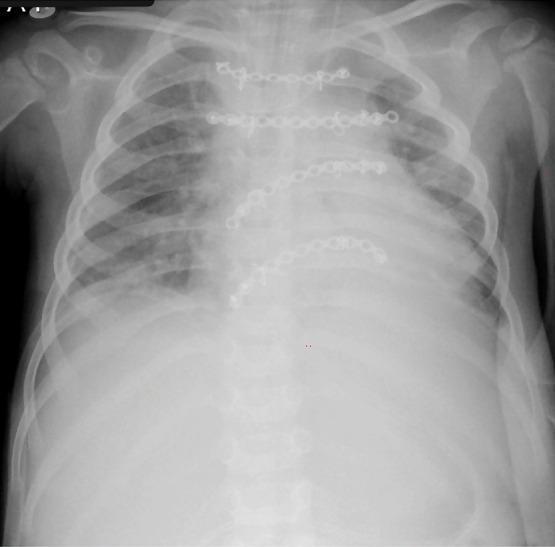
AP chest X-ray (postoperative day 6): Four titanium miniplates at ribs 1, 2, 4, and 5 securing the reconstructed thoracic cage. Lung fields are clear; no effusion or pneumothorax.
Functional Consequences
- Pulmonary function: Significant permanent reduction in FVC and FEV₁ (20–40% depending on extent); restrictive pattern on spirometry
- Exercise tolerance: Reduced in proportion to extent of resection
- Quality of life: Cosmetic deformity and shoulder asymmetry are common concerns; patients often adapt surprisingly well
Modern Perspective
Thoracoplasty is now a salvage procedure reserved for situations where:
- The pleural space cannot be obliterated by other means (decortication, muscle flap alone)
- Pulmonary re-expansion is impossible (trapped lung, destroyed lung)
- MDR-TB cavities persist despite adequate chemotherapy
It is rarely performed in resource-rich settings but remains relevant in high-TB-burden countries and in the management of complex post-resection complications. Limited thoracoplasty (1–3 ribs) combined with myoplasty represents the contemporary approach, minimizing deformity while effectively obliterating the target space.
Key Comparisons: Thoracoplasty vs. Alternative Space-Obliteration Methods
| Method | Best for | Advantage | Disadvantage |
|---|---|---|---|
| Thoracoplasty | Rigid chest, large space | Definitive obliteration | Deformity, lung restriction |
| Muscle flap (myoplasty) | Moderate space, BPF | Preserves chest wall | Limited by muscle availability |
| Decortication | Early empyema, re-expandable lung | Restores lung function | Fails if lung trapped |
| Clagett procedure | Post-pneumonectomy empyema | Open drainage then closure | Multi-stage, prolonged course |
| Eloesser flap | Palliative / poor surgical risk | Simple open drainage | Permanent opening |
This is a shared conversation. Sign in to Orris to start your own chat.