explain meningitis pathology from robbins pathology book
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have everything needed to provide a comprehensive answer. Here is the full meningitis pathology from Robbins:
Meningitis — Robbins Pathology
Sources: Robbins & Kumar Basic Pathology (9780323790185) and Robbins, Cotran & Kumar Pathologic Basis of Disease (9780443264528)
Definition
Meningitis is an inflammatory process involving the leptomeninges and the CSF within the subarachnoid space, typically caused by infection. When the inflammation extends into the underlying brain parenchyma, it is termed meningoencephalitis. The term is also applied to non-infectious settings:
- Chemical meningitis — response to irritants (e.g., debris from a ruptured epidermoid cyst)
- Carcinomatous meningitis — spread of metastatic cancer cells to the subarachnoid space
- Autoimmune meningitis — seen with systemic autoimmune disease
Classification
Infectious meningitis is classified into three subtypes based on etiology and clinical evolution:
| Type | Usual Cause | CSF Pattern |
|---|---|---|
| Acute Pyogenic | Bacterial | Neutrophilic pleocytosis, ↑↑ protein, ↓↓ glucose |
| Aseptic (Viral) | Viral (enteroviruses most common) | Lymphocytic pleocytosis, ↑ protein (moderate), normal glucose |
| Chronic | TB, spirochetes, fungi | Mixed cellularity, ↑ protein, ↓ or normal glucose |
1. Acute Pyogenic (Bacterial) Meningitis
Causative Organisms by Age
| Age Group | Common Organisms |
|---|---|
| Neonates | Escherichia coli, Group B Streptococci |
| Adolescents/Young Adults | Neisseria meningitidis |
| Elderly | Streptococcus pneumoniae, Listeria monocytogenes |
- Haemophilus influenzae was previously a major cause in infants but immunization has dramatically reduced its incidence.
- In immunosuppressed patients, organisms such as Klebsiella or anaerobes may be causative with atypical clinical presentations.
Clinical Features
- Systemic signs of infection (fever, malaise)
- Meningeal irritation: headache, photophobia, neck stiffness
- Neurologic impairment: irritability, clouding of consciousness
CSF Findings
- Increased pressure; cloudy or frankly purulent
- Abundant neutrophils
- Elevated protein
- Markedly reduced glucose
Morphology (Gross and Microscopic)
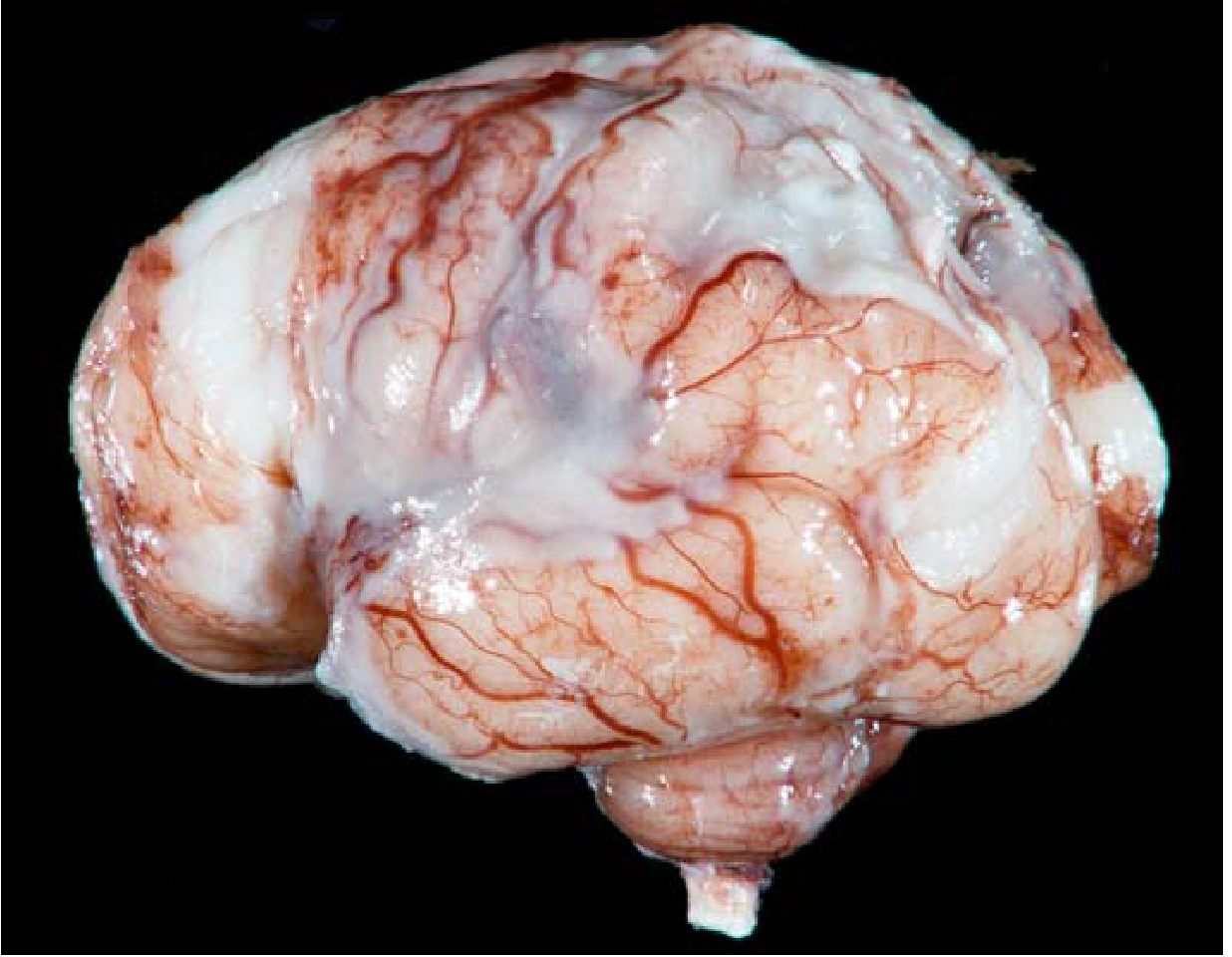
Gross:
- Exudate evident within the leptomeninges on the brain surface
- Meningeal vessels are engorged and prominent
- Tracts of pus extend along blood vessels; distribution varies by organism (H. influenzae → basal; pneumococcal → over cerebral convexities near the sagittal sinus)
- In fulminant cases, inflammation extends to the ventricles (ventriculitis); the choroid plexus lacks a blood-brain barrier and may serve as a portal of entry
Microscopic:
- Neutrophils fill the subarachnoid space in severe cases; in milder cases they surround leptomeningeal blood vessels
- Gram stain reveals bacteria, particularly in untreated cases
- In fulminant meningitis: inflammatory cells infiltrate leptomeningeal vein walls and extend focally into the brain parenchyma (cerebritis); secondary vasculitis and venous thrombosis → hemorrhagic cerebral infarction
Sequelae:
- Leptomeningeal fibrosis → hydrocephalus (more common with TB meningitis, but occurs in bacterial meningitis too)
- In pneumococcal meningitis specifically: large quantities of capsular polysaccharide produce a gelatinous exudate → chronic adhesive arachnoiditis (arachnoid fibrosis)
- Waterhouse-Friderichsen syndrome: meningitis-associated septicemia with hemorrhagic infarction of the adrenal glands — most often with meningococcal and pneumococcal infection
2. Aseptic (Viral) Meningitis
Key Features
- A clinical term for meningitis manifestations (meningeal irritation, fever, altered consciousness) without organisms identifiable by bacterial culture
- Generally viral in etiology; may be rickettsial or autoimmune
- Enteroviruses account for ~80% of identified cases
- Usually self-limited; treated symptomatically
CSF Findings
- Lymphocytic pleocytosis
- Moderate protein elevation
- Normal glucose (key distinction from bacterial meningitis)
Morphology
- Less dramatic than bacterial meningitis
- Leptomeningeal infiltration by lymphocytes and monocytes rather than neutrophils
- No suppurative exudate
3. Chronic Meningitis
Caused by mycobacteria, some spirochetes, and fungi; these infections often involve the brain parenchyma as well.
A. Tuberculous Meningitis
- Symptoms: headache, malaise, mental confusion, vomiting
- CSF: moderate ↑ cellularity (mononuclear or mixed), ↑↑ protein, moderately ↓ or normal glucose
- Tuberculoma: well-circumscribed intraparenchymal mass of M. tuberculosis; may coexist with meningitis
- Complication: chronic tuberculous meningitis → arachnoid fibrosis (particularly at the base of the brain) → hydrocephalus from impaired CSF resorption
B. Spirochetal Infections (Neurosyphilis)
- Occurs in ~10% of untreated Treponema pallidum infection (tertiary syphilis); more aggressive with HIV co-infection
- Patterns of CNS involvement:
- Meningovascular neurosyphilis: chronic meningitis (usually basal), associated with obliterative endarteritis of meningeal/cortical vessels → strokes
- Paretic neurosyphilis (general paresis): progressive dementia from direct parenchymal invasion
- Tabes dorsalis: degeneration of posterior spinal columns and dorsal nerve roots
- Lyme Neuroborreliosis (Borrelia burgdorferi): can cause meningitis, cranial nerve palsies, and radiculopathy
C. Fungal Meningitis
- Cryptococcus neoformans: most important fungal cause of meningitis, especially in HIV/immunocompromised patients
- Produces a gelatinous meningitis as the organisms fill the subarachnoid space
- Characteristic "soap-bubble" lesions in basal ganglia/cortex (pseudocysts of cryptococcal organisms)
Summary of CSF Interpretation
| Parameter | Bacterial | Viral | Tuberculous/Fungal |
|---|---|---|---|
| Appearance | Turbid/purulent | Clear | Clear/viscous |
| Cells | Neutrophils ↑↑ | Lymphocytes ↑ | Lymphocytes/mixed ↑ |
| Protein | ↑↑ | Mildly ↑ | ↑↑ |
| Glucose | ↓↓ | Normal | ↓ or normal |
— Robbins & Kumar Basic Pathology (Robbins Pathology), Chapter 21; Robbins, Cotran & Kumar Pathologic Basis of Disease, Chapter 28
make pdf
Reading File
Running Command
Running Command
Writing File
Running Command
PDF generated successfully. Here's your download link:
Meningitis Pathology Robbins
PDF Document · PDF
The PDF includes:
- Definition & classification table
- Acute Pyogenic Meningitis — organisms by age, clinical features, CSF findings, gross & microscopic morphology, sequelae
- Gross pathology image from Robbins (Fig. 21.16)
- Aseptic (Viral) Meningitis section
- Chronic Meningitis — TB, neurosyphilis (with pattern table), and cryptococcal
- Full CSF comparison table across all three types
- Sourced from both Robbins editions throughout
This is a shared conversation. Sign in to Orris to start your own chat.