I want to study yhroid gland in detail..brom basic to advance in a way so that i become clinically sound also do provide the related clinical examination how to interpret thyroid profile , other investigation to be done... divide the data ino chunks so that it become easy for me to undesrstand it better ..also do provide the related mnemonics so i can learn easily
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
Here is your complete, chunk-based thyroid study guide — from embryology to clinical exam and drug management — drawn from Gray's Anatomy, Junqueira's Histology, Robbins Pathology, Ganong's Physiology, Lippincott's Pharmacology, and Henry's Lab Methods.
🦋 THE THYROID GLAND — Complete Study Guide
CHUNK 1 — EMBRYOLOGY
Origin & Descent
- Arises as a median outgrowth (diverticulum) from the floor of the pharynx at the foramen cecum (base of tongue), between the tuberculum impar and copula
- Descends anterior to the pharyngeal gut as a bilobed diverticulum, connected to the tongue by the thyroglossal duct (normally obliterates)
- Reaches final position anterior to the trachea by week 7
- Begins functioning (first colloid follicles appear) by end of month 3
- C cells (parafollicular cells) — derived from the ultimobranchial body (neural crest origin); produce calcitonin
Clinical Correlates
| Anomaly | Cause | Feature |
|---|---|---|
| Thyroglossal duct cyst | Remnant of duct fails to obliterate | Midline neck swelling that moves on swallowing AND tongue protrusion |
| Lingual thyroid | Failure to descend | Mass at base of tongue; may be the ONLY thyroid tissue |
| Ectopic thyroid | Abnormal migration | Anywhere along descent path |
| Pyramidal lobe | Persistent lower duct portion | Extends upward from isthmus; seen in ~50% |
📌 Mnemonic — Thyroglossal Duct Cyst vs Branchial Cyst: "Throglossal — Tongue protrusion moves it; Branchial — Behind/lateral neck"
CHUNK 2 — ANATOMY
Position
- Located anterior to trachea, below and lateral to thyroid cartilage
- Lies deep to sternohyoid, sternothyroid, and omohyoid muscles
- Enclosed in pretracheal fascia (visceral compartment)
- Consists of two lateral lobes + isthmus (crosses 2nd–3rd tracheal cartilages)
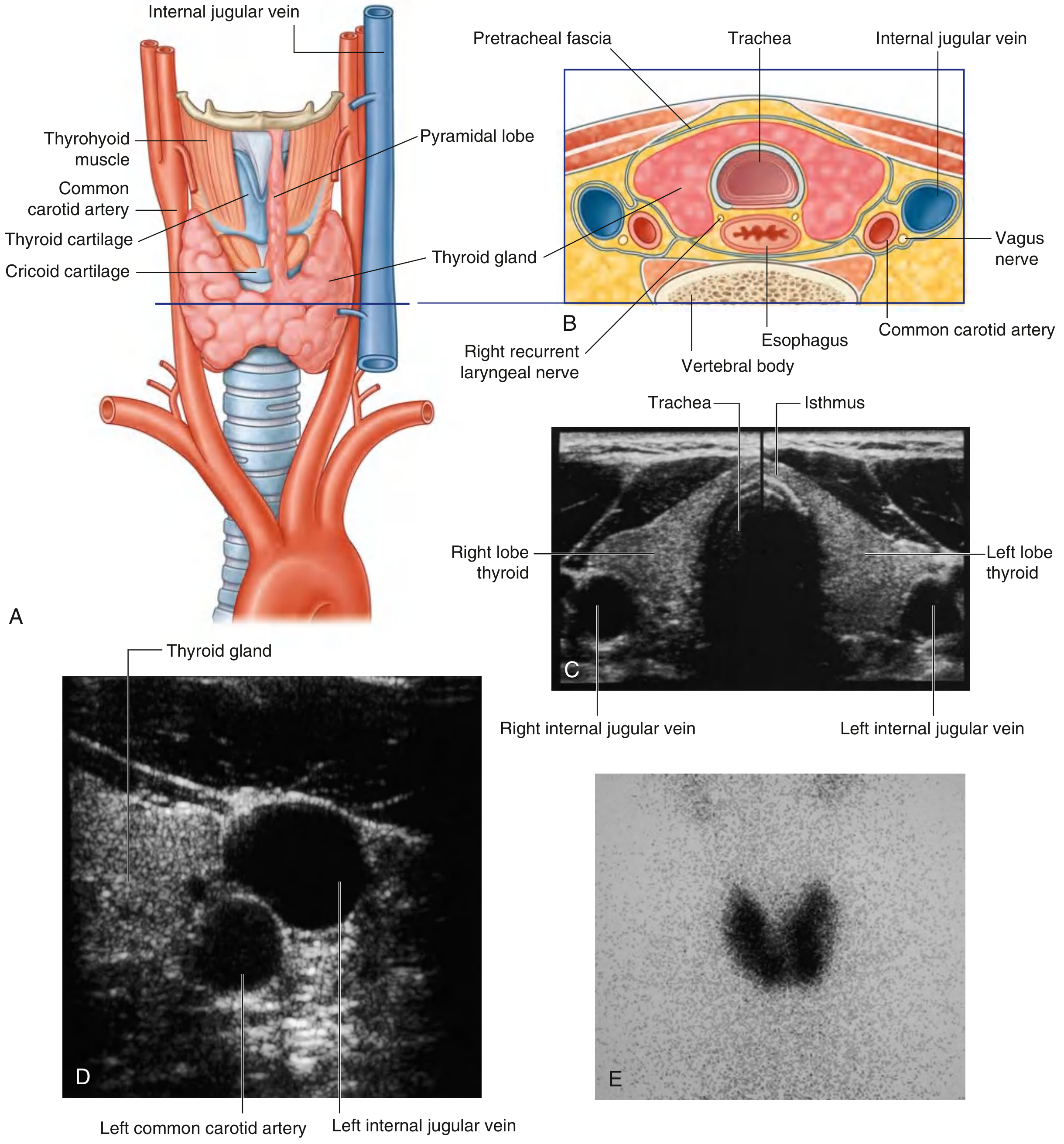
Blood Supply
| Artery | Origin | Supplies |
|---|---|---|
| Superior thyroid artery | 1st branch of external carotid | Superior pole; runs near external laryngeal nerve |
| Inferior thyroid artery | Thyrocervical trunk → subclavian | Inferior pole; runs near recurrent laryngeal nerve (RLN) |
| Thyroid ima artery | Brachiocephalic/arch (variable, ~10%) | Isthmus |
Venous Drainage
- Superior thyroid vein → internal jugular
- Middle thyroid vein → internal jugular
- Inferior thyroid vein → brachiocephalic vein
Important Nerves — Surgical Danger Zones
| Nerve | Risk | Injury consequence |
|---|---|---|
| Recurrent laryngeal nerve (RLN) | Passes behind/near inferior thyroid artery | Hoarseness (unilateral), stridor/aphonia (bilateral) |
| External laryngeal nerve | Near superior thyroid artery | Loss of cricothyroid function → voice fatigue, loss of high pitch |
📌 Mnemonic — "STA hunts ELN; ITA hunts RLN" Superior Thyroid Artery near External Laryngeal Nerve Inferior Thyroid Artery near Recurrent Laryngeal Nerve
CHUNK 3 — HISTOLOGY
Normal Structure
- Parenchyma = millions of follicles (variable diameter), lined by simple epithelium, with central colloid-filled lumen
- Colloid = gelatinous, acidophilic; contains thyroglobulin (660 kDa glycoprotein) — the precursor for thyroid hormones
- Covered by fibrous capsule → septa → lobules (20–40 follicles each)
- Stroma: sparse reticular CT with fenestrated capillaries
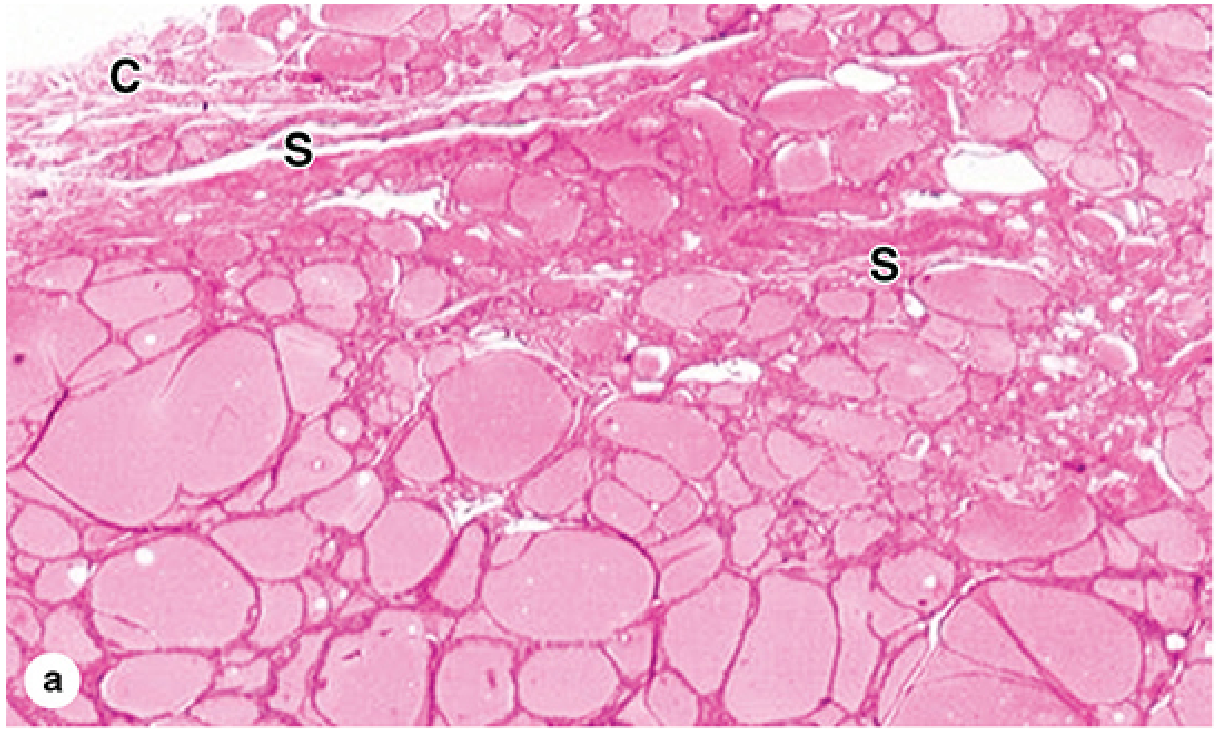
Two Cell Types
| Cell | Location | Function |
|---|---|---|
| Follicular cells (thyrocytes) | Lining of follicle | Synthesise & secrete T3, T4 |
| Parafollicular cells (C cells) | Between follicles, in stroma | Synthesise calcitonin |
Thyrocyte Shape = Activity Indicator
- Tall columnar = hyperactive (high TSH stimulation)
- Squamous/flat = hypoactive (suppressed gland)
📌 Mnemonic — "TALL = Turbo-Active; LOW = Lazy" When the follicular cell is tall, the gland is active (TSH-driven); when flat, it is suppressed.
Unique Feature
The thyroid is the only endocrine gland that stores hormone extracellularly (in colloid). It has up to 3 months' worth of stored hormone — explaining why antithyroid drugs take weeks to work.
CHUNK 4 — PHYSIOLOGY: HORMONE SYNTHESIS (The Most Important Chunk!)
The HPT Axis (Feedback Loop)
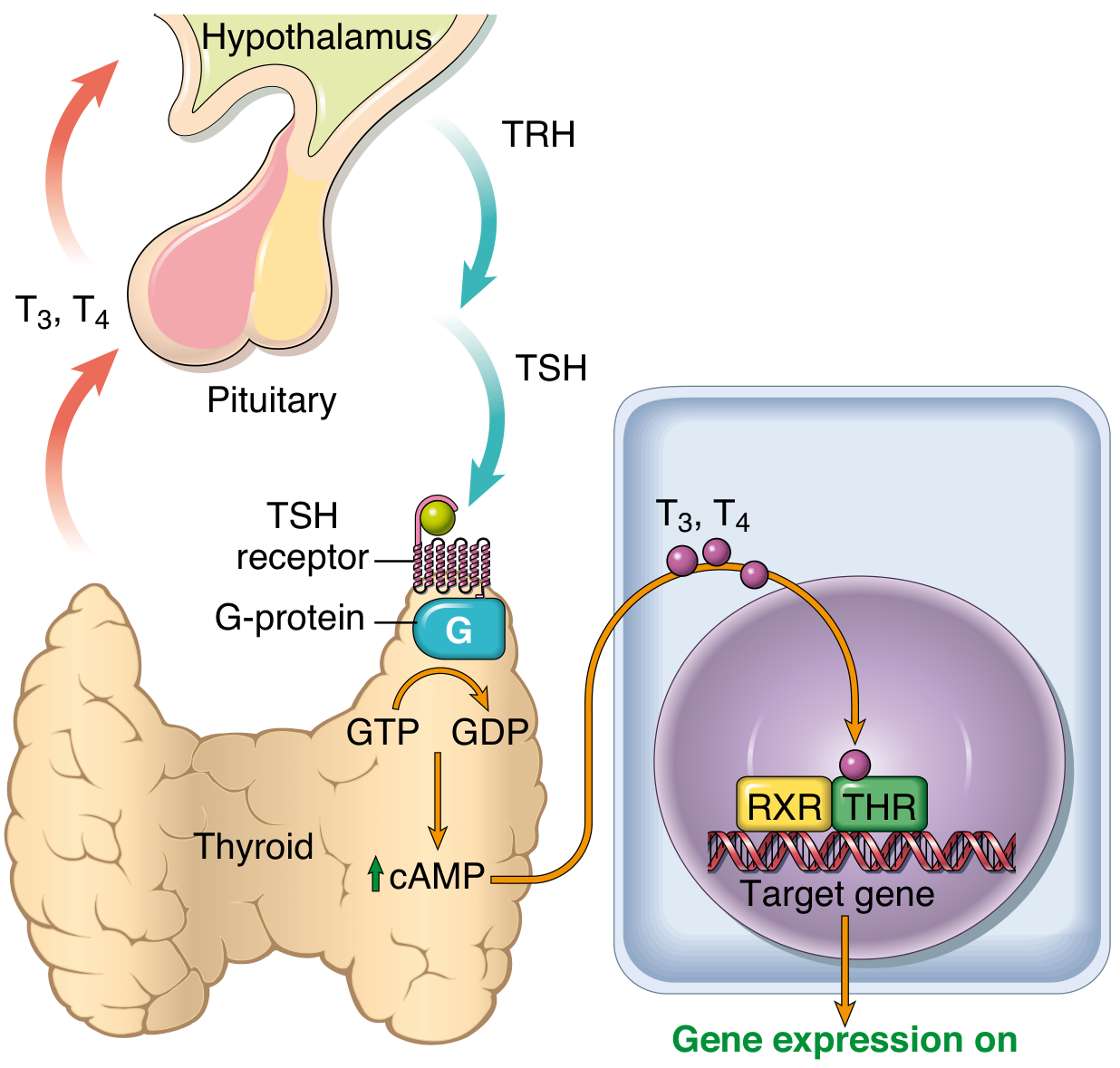
Axis:
- Hypothalamus → TRH (thyrotropin-releasing hormone)
- Anterior pituitary → TSH (thyroid-stimulating hormone / thyrotropin)
- TSH binds TSH receptor → Gs protein → ↑cAMP → thyroid growth + hormone synthesis
- T3/T4 → negative feedback on both hypothalamus and pituitary
Steps of Thyroid Hormone Synthesis
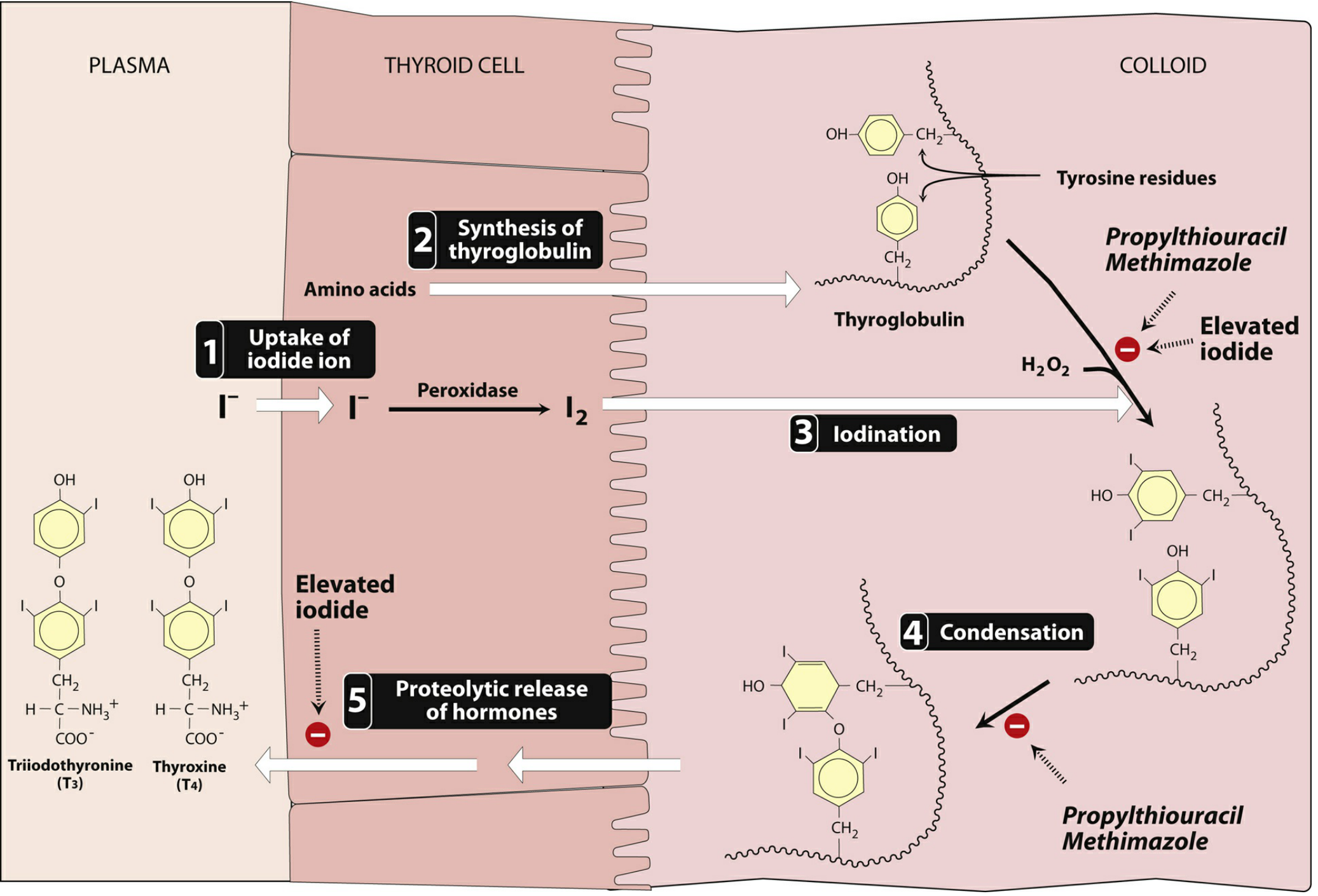
| Step | Process | Key Enzyme/Protein |
|---|---|---|
| 1 | Iodide (I⁻) uptake from plasma into thyrocyte | NIS (Na⁺/I⁻ symporter) — basolateral |
| 2 | Synthesis of thyroglobulin (Tg); secreted into colloid | Rough ER |
| 3 | Oxidation of I⁻ → I₂ ; Organification — iodination of tyrosine on Tg to form MIT then DIT | Thyroid peroxidase (TPO) |
| 4 | Coupling/condensation: DIT+DIT → T4; MIT+DIT → T3 | Thyroid peroxidase (TPO) |
| 5 | Tg reabsorbed by endocytosis → lysosomal hydrolysis → free T3 & T4 released into blood | Lysosomes |
📌 Mnemonic — "I OTIC" for synthesis steps: Iodide uptake → Organification → Tg iodination → Iodotyrosine coupling → Cleavage & release
T4 vs T3 — The Prohormone Concept
| T4 | T3 | |
|---|---|---|
| Secretion from thyroid | 80 µg/day (major) | 4 µg/day (minor) |
| Binding affinity for THR | Low | 10× higher |
| Peripheral conversion | T4 → T3 by 5'-deiodinase | Active hormone |
| Protein binding | 99.97% bound (to TBG, transthyretin, albumin) | 99.7% bound |
| Clinical significance | "Prohormone"; measured as FT4 | "Active hormone"; measured as FT3 |
| Half-life | ~7 days | ~1 day |
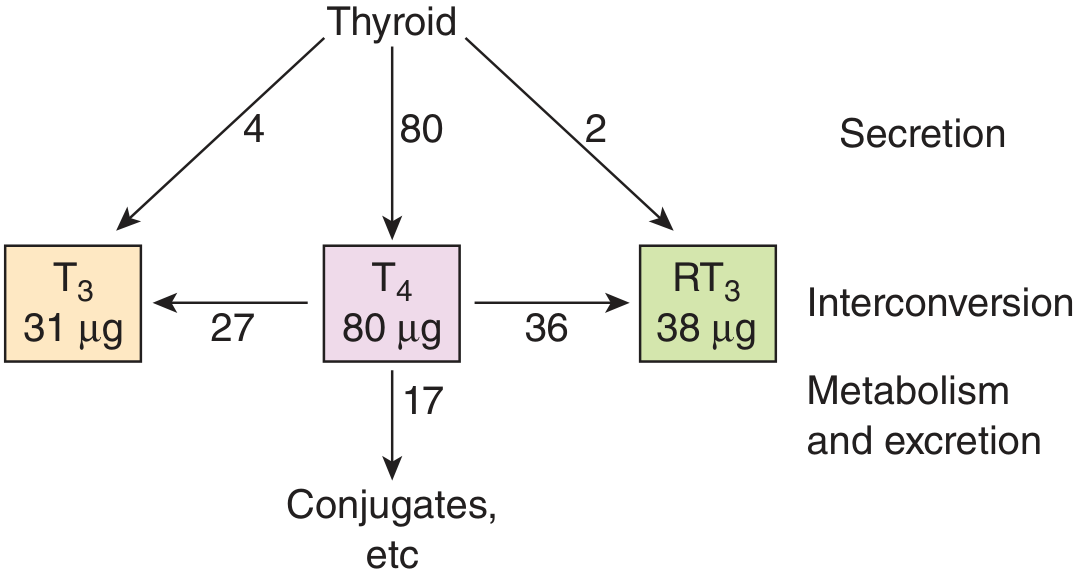
📌 Mnemonic — "DIT + DIT = T4 (4 iodines); MIT + DIT = T3 (3 iodines)" Count the iodines: MIT = 1 iodine, DIT = 2 iodines → MIT+DIT = 3 = T3; DIT+DIT = 4 = T4
Actions of Thyroid Hormones
- ↑ Basal metabolic rate (BMR)
- ↑ O₂ consumption and heat production
- ↑ Protein synthesis AND catabolism
- ↑ Carbohydrate & lipid catabolism
- Critical for brain development in fetus/neonate (congenital hypothyroidism = cretinism)
- Potentiates catecholamine actions (↑ β-adrenergic receptor expression)
- Stimulates bone resorption
CHUNK 5 — CLINICAL DISORDERS
5A — Hyperthyroidism / Thyrotoxicosis
Causes (GRAVES is #1 — 85%)
| Cause | Feature |
|---|---|
| Graves disease | TSI (thyroid-stimulating immunoglobulin) mimics TSH; autoimmune |
| Toxic multinodular goiter | Multiple hot nodules |
| Toxic adenoma | Single hot nodule |
| Iodine-induced (Jod-Basedow) | Excess iodine in iodine-deficient patient |
| Thyroiditis (de Quervain, silent) | Release of preformed hormone |
| TSH-secreting pituitary tumor | Rare; TSH elevated (secondary) |
| Struma ovarii | Ovarian teratoma with ectopic thyroid |
| Factitious thyrotoxicosis | Exogenous T4 ingestion |
📌 Mnemonic for Graves disease features — "TAGS": Tremor/Tachycardia · Autoimmmune/Atrial fibrillation · Goitre/Graves ophthalmopathy · Sweating/Skin warm
Clinical Features of Thyrotoxicosis — "SWEATING":
Sweating & heat intolerance · Weight loss (despite ↑ appetite) · Emotion/anxiety/tremor · Atrial fibrillation/tachycardia/palpitations · Thinning hair/brittle nails · Increased bowel frequency · Neuromuscular — proximal myopathy · Gaze/lid lag (sympathetic)
Graves-Specific Features (not in other causes):
- Exophthalmos (proptosis) — infiltration of extraocular muscles by GAG-laden connective tissue
- Pretibial myxedema — skin thickening/induration over shins (despite hyperthyroidism)
- Thyroid acropachy — periosteal new bone formation, clubbing (rare)
5B — Hypothyroidism
| Type | Cause |
|---|---|
| Primary (most common) | Hashimoto's thyroiditis, post-RAI/thyroidectomy, iodine deficiency, drugs (lithium, amiodarone) |
| Secondary | Pituitary TSH deficiency |
| Tertiary | Hypothalamic TRH deficiency |
| Congenital | Cretinism |
Clinical Features — "COLD TIRED":
Cold intolerance · Obese (weight gain) · Lethargy/fatigue · Depression/slow mentation · Thick skin / dry / puffy (myxedema) · Increased TSH · Raspy/hoarse voice · Edema (periorbital, non-pitting) · Decreased reflexes (hung-up/delayed)
Myxedema Coma — life-threatening hypothyroidism; triggers: cold exposure, infection, sedatives; Rx: IV T3/T4 + hydrocortisone + warming
Cretinism (congenital hypothyroidism):
- Coarse features, macroglossia, umbilical hernia
- Intellectual disability (irreversible if untreated)
- Short stature
- Tx: Levothyroxine started within 2–4 weeks of birth
5C — Hashimoto's Thyroiditis
- Most common cause of hypothyroidism in iodine-sufficient areas
- Autoimmune: anti-TPO antibodies (diagnostic), anti-thyroglobulin antibodies
- Histology: lymphocytic infiltrate with germinal centres, Hürthle cell (oxyphilic) change
- May cause transient thyrotoxicosis early ("hashitoxicosis") then hypothyroidism
- ↑ risk of thyroid lymphoma
5D — Goiter
- Simple/diffuse goiter = enlarged gland due to iodine deficiency or goitrogens (↑TSH → hyperplastic stimulation)
- Multinodular goiter = long-standing hyperplasia → nodules; most euthyroid
- Goitrogens: propylthiouracil, methimazole, lithium, cassava, cabbage, turnips
CHUNK 6 — THYROID PROFILE INTERPRETATION (The Clinical Core)
Reference Ranges (Adults)
| Test | Normal | Notes |
|---|---|---|
| TSH | 0.4 – 4.0 mIU/L | Most sensitive test for thyroid dysfunction |
| Free T4 (FT4) | 0.8 – 1.8 ng/dL (10–23 pmol/L) | Better than total T4 |
| Free T3 (FT3) | 2.3 – 4.2 pg/mL | Useful in T3 toxicosis |
| Total T4 | 5 – 12 µg/dL | Affected by TBG levels |
| Anti-TPO Ab | < 35 IU/mL | Elevated in Hashimoto's, Graves' |
| Anti-TSH receptor Ab (TRAb) | < 1.75 IU/L | Specific for Graves disease |
| Thyroglobulin | 2 – 40 µg/L | Tumor marker post-thyroidectomy for differentiated thyroid cancer |
| Calcitonin | < 10 pg/mL | Elevated in medullary thyroid carcinoma |
Interpretation Algorithm
STEP 1: Check TSH (most sensitive first-line test)
│
├── TSH LOW (↓)
│ ├── FT4 HIGH → PRIMARY HYPERTHYROIDISM
│ ├── FT4 NORMAL → SUBCLINICAL HYPERTHYROIDISM
│ └── FT4 LOW → SECONDARY HYPOTHYROIDISM (pituitary failure)
│
├── TSH HIGH (↑)
│ ├── FT4 LOW → PRIMARY HYPOTHYROIDISM
│ ├── FT4 NORMAL → SUBCLINICAL HYPOTHYROIDISM
│ └── FT4 HIGH → SECONDARY HYPERTHYROIDISM (TSH-secreting tumor)
│
└── TSH NORMAL → EUTHYROID (if clinically suspected, check FT4)
Pattern Summary Table
| Condition | TSH | FT4 | FT3 |
|---|---|---|---|
| Primary hypothyroidism | ↑ | ↓ | ↓ |
| Subclinical hypothyroidism | ↑ | Normal | Normal |
| Primary hyperthyroidism | ↓ | ↑ | ↑ |
| Subclinical hyperthyroidism | ↓ | Normal | Normal |
| T3 toxicosis | ↓ | Normal | ↑ |
| Secondary hypothyroidism | ↓/Normal | ↓ | ↓ |
| TSH-secreting tumor | ↑ | ↑ | ↑ |
| Non-thyroidal illness (sick euthyroid) | Variable | Normal/↓ | ↓ (RT3 ↑) |
📌 Mnemonic — "TSH is the THERMOSTAT": When T3/T4 are HIGH (hot) → thermostat turns DOWN (TSH ↓) When T3/T4 are LOW (cold) → thermostat turns UP (TSH ↑)
CHUNK 7 — DRUGS THAT AFFECT THYROID TESTS (Clinically Critical)
| Drug | Effect on TFTs | Mechanism |
|---|---|---|
| Estrogen/OCP | ↑ Total T4 & T3; TSH normal | ↑ TBG → ↑ bound hormone |
| Glucocorticoids (high dose) | ↓ TSH; ↓ T4→T3 conversion | Suppress TRH/TSH + ↓ deiodinase |
| Propranolol (high dose) | ↓ T4→T3 conversion | Blocks 5'-deiodinase |
| Amiodarone | Hypo OR hyperthyroidism | Contains 37% iodine by weight; inhibits T4→T3 |
| Lithium | Hypothyroidism (15–50%) | Inhibits hormone synthesis and release (like iodide) |
| Phenytoin/carbamazepine/rifampin | ↓ Total T4 | Displace T4 from TBG + ↑ hepatic metabolism |
| Heparin | Falsely ↑ FT4 | Liberates free fatty acids → displace T4 from binding proteins |
| Dopamine | ↓ TSH | Suppresses TSH secretion |
| Iodide excess (Wolff-Chaikoff) | Hypothyroidism | High I⁻ blocks organification |
| Iodide in iodine-deficient patient (Jod-Basedow) | Hyperthyroidism | Provides substrate for excess synthesis |
CHUNK 8 — CLINICAL EXAMINATION OF THE THYROID
Inspection
- Look for swelling in the anterior midline neck below thyroid cartilage
- Ask patient to swallow: thyroid and thyroglossal cysts move up on swallowing (attached to pretracheal fascia)
- Thyroglossal cysts also move on tongue protrusion (unlike thyroid swelling)
- Look for: distended neck veins (retrosternal extension), tracheal deviation, scars
Palpation
Technique:
- Stand behind the patient (or in front for small glands)
- Ask patient to flex neck slightly (relaxes strap muscles)
- Ask patient to swallow while you feel — confirm movement
- Palpate each lobe: size, consistency, surface, tenderness, nodules
- Check for cervical lymphadenopathy (carcinoma)
- Palpate trachea — deviation suggests large/asymmetric goiter or retrosternal extension
What to characterize:
- Size (use WHO grading: 0, 1a, 1b, 2, 3)
- Diffuse vs nodular (single vs multinodular)
- Consistency: soft (simple goiter), firm (Hashimoto's), hard/rocky (malignancy)
- Tenderness (de Quervain's subacute thyroiditis — exquisitely tender)
- Surface: smooth vs bosselated
- Mobility with swallowing
Percussion
- Over the manubrium → dull = retrosternal goiter (Pemberton's sign: arm elevation → facial congestion + distended neck veins)
Auscultation
- Bruit over thyroid = increased vascularity = Graves disease (pathognomonic when present)
Signs to Elicit in Thyroid Examination (Hyperthyroidism)
| Sign | How | Indicates |
|---|---|---|
| Lid lag | Ask patient to follow finger moving downward — lid lags behind eyeball | Sympathetic overactivity |
| Lid retraction | Upper lid above the limbus at rest (startled look) | Sympathetic overactivity |
| Exophthalmos | Protrusion of globe beyond orbital rim; use Hertel exophthalmometer | Graves' ophthalmopathy |
| Chemosis | Conjunctival edema | Graves' ophthalmopathy |
| Ophthalmoplegia | Restricted eye movement | Graves' (inferior & medial rectus most affected) |
| Tremor | Fine tremor of outstretched hands (paper test) | Thyrotoxicosis |
| Pretibial myxedema | Skin thickening/induration over shins | Graves' disease (specific) |
| Thyroid acropachy | Clubbing + periosteal new bone | Graves' (rare) |
Pulse in Thyroid Disease
- Hyperthyroid: Tachycardia, irregularly irregular (AF), bounding pulse
- Hypothyroid: Bradycardia, slow-rising, slow peripheral pulse
CHUNK 9 — INVESTIGATIONS (Beyond TFTs)
First-Line
| Test | When | What it shows |
|---|---|---|
| TSH + FT4 | All suspected thyroid disease | Screen + confirm |
| Anti-TPO antibodies | Suspected Hashimoto's / autoimmune | Elevated in >90% Hashimoto's |
| TRAb (TSH receptor antibodies) | Suspected Graves | Confirms autoimmune hyperthyroidism |
| Thyroid ultrasound | Any nodule, goiter | Size, echotexture, vascularity, nodule characterization (TIRADS) |
For Thyroid Nodule Workup
| Test | When | What it shows |
|---|---|---|
| Radioiodine (¹³¹I / ⁹⁹ᵐTc) scan | Nodule + low/normal TSH | Hot (functioning) vs Cold (non-functioning) nodule |
| FNAC (Fine Needle Aspiration Cytology) | Cold nodule, suspicious on USG | Bethesda system: I–VI (I=non-diagnostic; VI=malignant) |
| Serum calcitonin | Suspicious for medullary ca | ↑ in medullary thyroid carcinoma |
| Thyroglobulin | Post-thyroidectomy monitoring | Recurrence marker for differentiated thyroid ca |
📌 Mnemonic for nodule assessment — "CITRUS": Consistency hard? Irrregular margins on USG? Technecium scan hot or cold? Recurrent laryngeal nerve palsy? Ultrasound TIRADS? Swimming/cervical nodes?
For Thyroid Storm
- Clinical diagnosis (Burch-Wartofsky score)
- TFTs (very ↑ T3/T4), CBC (leukocytosis if trigger is infection), LFTs, ECG
Imaging
| Modality | Use |
|---|---|
| Ultrasound | First-line imaging; cheap, no radiation; measures size, detects nodes, guides FNAC |
| Radioiodine scan | Functional assessment; hot/cold nodes; whole body scan for metastases |
| CT/MRI neck | Retrosternal goiter, tracheal compression, surgical planning |
| PET scan | Thyroid cancer recurrence (FDG-avid for dedifferentiated tumors) |
CHUNK 10 — PHARMACOLOGY: TREATMENT
Hypothyroidism Treatment
- Levothyroxine (T4) — drug of choice
- Once daily, on empty stomach (avoid calcium, iron, antacids within 4h)
- Steady state in 6–8 weeks → recheck TSH then
- Monitor: TSH (target 0.5–2.5 for most patients)
- Enzyme inducers (phenytoin, rifampin, phenobarbital) → ↑ T4 metabolism → ↑ dose needed
Hyperthyroidism Treatment
1. Thioamides (block TPO)
| Drug | Feature |
|---|---|
| Methimazole (MMI) | Preferred; once daily; fewer side effects |
| Propylthiouracil (PTU) | Also blocks T4→T3 conversion; preferred in 1st trimester of pregnancy and thyroid storm; risk of hepatotoxicity |
| Adverse effects | Agranulocytosis (~0.3%) — check WBC if fever/sore throat; rash, arthralgia |
2. Radioiodine (¹³¹I)
- Destroys thyroid follicular cells
- Most develop hypothyroidism post-RAI → lifelong levothyroxine
- Contraindicated: pregnancy, breastfeeding, Graves' ophthalmopathy (can worsen)
3. Surgery (thyroidectomy)
- For large goiters, compression, suspected malignancy, patient preference
- Complications: hypocalcemia (parathyroid removal), RLN damage, hypothyroidism
4. Adjunctive
- β-blockers (propranolol): rapid symptomatic relief; also blocks T4→T3
- Lugol's iodine (SSKI): pre-operative use; blocks hormone release (Wolf-Chaikoff); used in thyroid storm
- Glucocorticoids: thyroid storm (block T4→T3 + treat adrenal insufficiency)
📌 Mnemonic for thyroid storm management — "BLIST": Beta-blocker (propranolol) · Lugol's iodine · IV fluids/cooling · Steroids · Thioamide (PTU first, given before iodine)
CHUNK 11 — THYROID CANCER (Quick Reference)
| Type | Frequency | Markers | Key Features |
|---|---|---|---|
| Papillary | 80% | Thyroglobulin | Psammoma bodies; Orphan Annie eye nuclei; BRAF mutation; excellent prognosis |
| Follicular | 10% | Thyroglobulin | Hematogenous spread; no psammoma bodies; RAS mutation |
| Medullary | 5% | Calcitonin, CEA | C-cell origin; familial (MEN 2A, 2B); RET mutation |
| Anaplastic | <5% | None specific | Most aggressive; rapidly fatal; elderly |
📌 Mnemonic for thyroid cancer — "PFMA" (Papillary-Follicular-Medullary-Anaplastic) = "Patients Fear More Agony" with worsening prognosis
QUICK SUMMARY CARD — "The THYROID in a Box"
ANATOMY: Butterfly, anterior trachea, deep to strap muscles
STA → ELN risk; ITA → RLN risk
HISTOLOGY: Follicles + colloid (thyroglobulin); C cells for calcitonin
EMBRYOLOGY: Foramen cecum → thyroglossal duct → trachea by week 7
SYNTHESIS: I⁻ uptake → Tg synthesis → Organification → Coupling → Cleavage
(TPO does steps 3 & 4 — blocked by thioamides)
HPT AXIS: TRH→TSH→T3/T4 (negative feedback)
T4 = prohormone (80µg/day); T3 = active (10× potency)
INTERPRET: TSH = thermostat; High TSH = hypo; Low TSH = hyper
HYPER Rx: PTU/MMI + β-blocker + ¹³¹I/surgery
HYPO Rx: Levothyroxine (T4) once daily
EXAM: Swallows moves it; bruit = Graves; hard = cancer
Pemberton sign = retrosternal extension
Sources: Gray's Anatomy for Students | Junqueira's Basic Histology 17e | Robbins & Cotran Pathologic Basis of Disease | Ganong's Review of Medical Physiology 26e | Lippincott Illustrated Reviews Pharmacology | Henry's Clinical Diagnosis and Management by Laboratory Methods
This is a shared conversation. Sign in to Orris to start your own chat.