Oct in ent in detail and explain me in creative manner so that I understand it better
Reading File
Finding Sources
Finding Sources
Searching the Web
optical coherence tomography OCT in ENT otolaryngology applications 2024
Reading File
Finding Sources
Finding Sources
Searching Images
optical coherence tomography ear middle ear tympanic membrane OCT
Reading File
Loading Image
Loading Image
Loading Image
Loading Image
Finding Sources
I now have all the material I need to construct a comprehensive, creative answer about OCT in ENT. Let me compile it.
🔦 OCT in ENT — The "Ultrasound of Light" for Your Ear, Nose & Throat
Imagine if you could peel back the skin of a vocal cord — layer by layer — without ever picking up a scalpel. Or peer through an eardrum and see fluid hiding in the middle ear without sticking a needle in. That's exactly what Optical Coherence Tomography (OCT) does. Think of it as the ultrasound of light: instead of bouncing sound waves off tissue, it bounces near-infrared light.
🎯 The Big Picture: What Is OCT?
OCT = a microscope for living tissue, in real time, without touching it.
It works on the principle of low-coherence interferometry — the same physics as how radar works, but with light waves (~800–1300 nm wavelength). It produces:
- Cross-sectional (B-scan) images showing tissue layers at microscopic resolution (~5–15 µm)
- 3D volumetric reconstructions
- Depth penetration of 1–3 mm into soft tissue
The analogy: if a CT scan gives you a map of a city from a satellite, OCT gives you a cross-section of a single wall of a single building — at the level of individual bricks.
🏗️ The Three Big Arenas of OCT in ENT
1. 👂 THE EAR — Seeing Through the Drum
The problem OCT solves: Your eardrum is like a frosted glass window. Standard otoscopy shows you the surface — but what's happening behind it? Is it fluid? Cholesteatoma? Air? You couldn't tell without a needle or surgery.
OCT changes the game by firing near-infrared light through the tympanic membrane (TM) and measuring the reflections from deeper layers. The TM appears as a bright "white ribbon" in cross-section, and what lies beneath tells the whole story.
🔍 What OCT Reveals in the Ear:
| Condition | What OCT Shows |
|---|---|
| Normal ear | Clear dark space behind TM = just air |
| Otitis media with effusion (OME) | Dense speckled signal behind TM = fluid |
| Acute otitis media (AOM) | Bright, turbid backscatter = thick pus |
| Cholesteatoma | Layered, highly reflective mass with characteristic texture |
| TM retraction | TM displaced inward, touching ossicles |
| TM perforation | Structural gap in the ribbon |
| Post-surgical reconstruction | Graft position and healing assessment |
Here's OCT in action — comparing healthy vs. pathological ears:
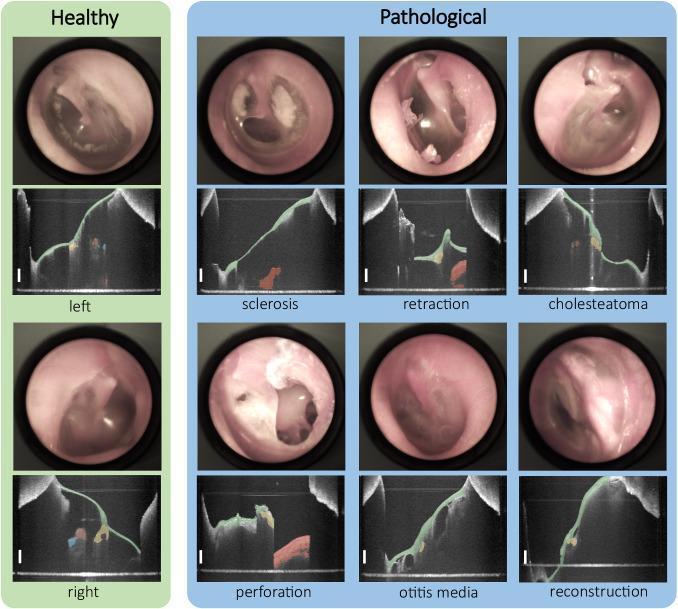
In the image: each pair shows an otoscope view (top) and OCT B-scan (bottom). Color-coded segments identify the TM (green), malleus/incus (orange/yellow). Scale bars = 1 mm.
And here's OCT in pediatric cases — diagnosing ear fluid:
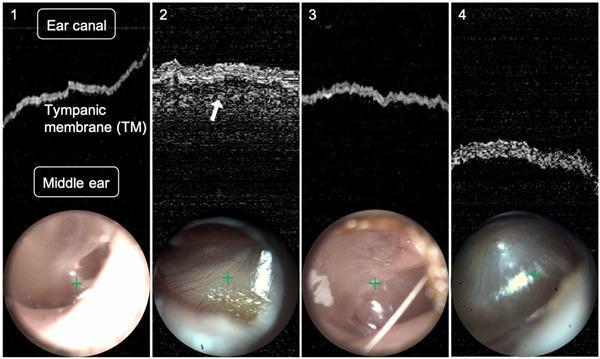
Panel 1 = normal (clear dark middle ear). Panel 2 = AOM — the white arrow points to the effusion signal. Panels 3 & 4 = borderline cases.
OCT can even visualize the ossicular chain (malleus + incus) that traditional otoscopy cannot see:
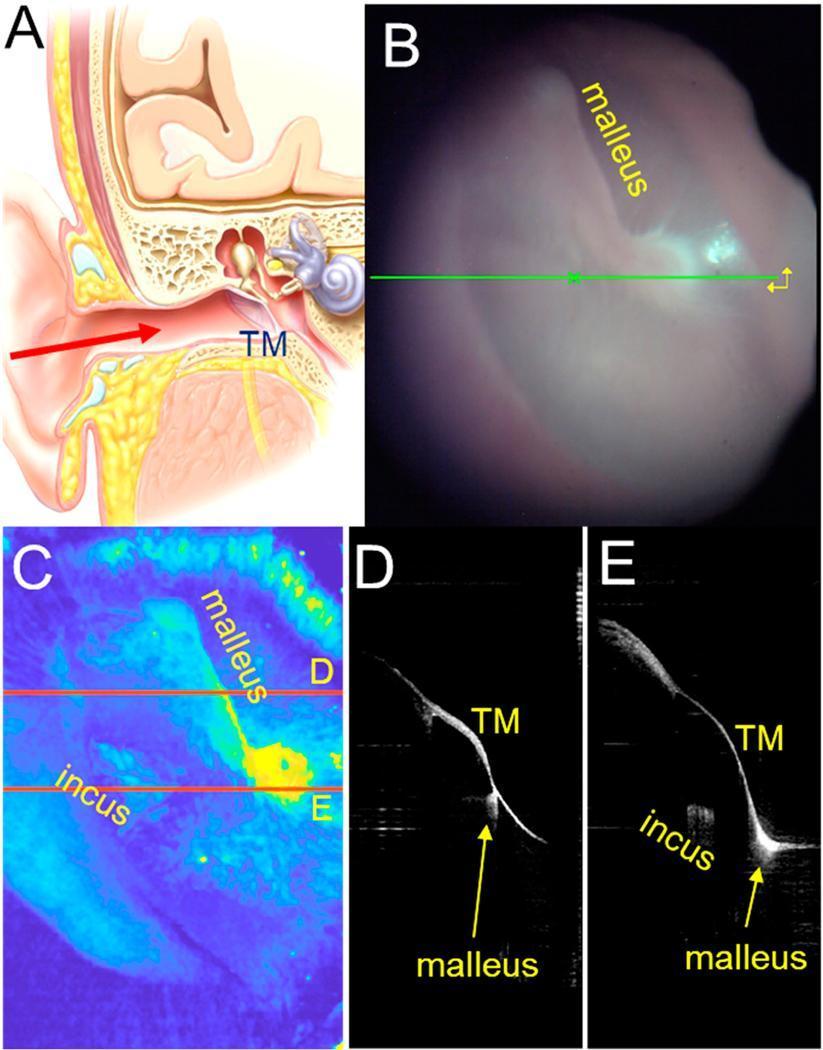
Panel A = anatomy diagram. B = otoscope view. C = OCT pseudocolor 3D showing malleus (yellow = high reflectivity) and incus. D & E = cross-sectional B-scans showing the TM-malleus-incus relationship.
🧫 The Inner Ear & Cochlea — OCT's Most Exciting Frontier
OCT has been adapted to image the living cochlea during ear surgery. In a landmark study from USC's Keck School of Medicine (2024), OCT measured fluid levels inside the inner ear during surgery — something never before possible noninvasively. Elevated endolymph correlated directly with the degree of hearing loss in Ménière's disease patients.
Researchers at USC are also developing an OCT otoscope — a handheld device combining standard otoscopy with OCT in a single tool for the clinic.
In research, high-speed OCT has directly measured basilar membrane vibration and outer hair cell (OHC) motion in living animals:
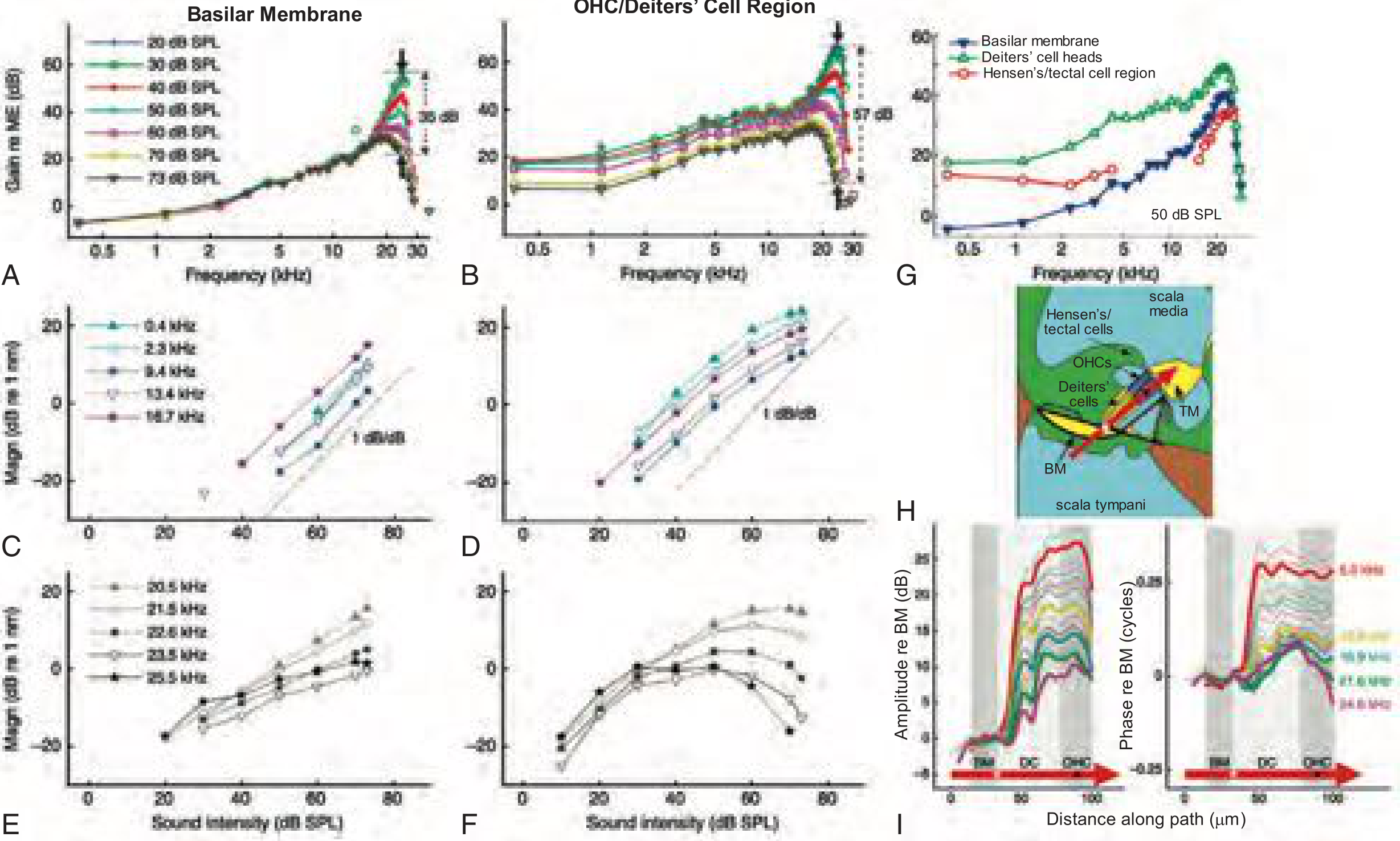
Panels A–I: OCT measuring nanometer-scale vibrations of the organ of Corti in a living gerbil. Note the OHC/Deiters' cell region shows 57 dB gain vs. only 35 dB in the basilar membrane — demonstrating how OHCs amplify sound. (Cummings Otolaryngology, Fig. 148.5)
2. 🗣️ THE LARYNX — Seeing Inside the Vocal Cord
The problem: Laryngeal cancers and precancerous lesions can be subtle. Biopsy is the gold standard but requires taking tissue. What if you could "biopsy" with light?
OCT of the larynx uses infrared light delivered via a fiber-optic probe through a laryngoscope to generate cross-sectional images of the vocal cord epithelium in real time.
From Cummings Otolaryngology:
"OCT is a technique that uses infrared light to provide cross-sectional imaging of the laryngeal epithelium with acute resolution. This technique has received recent support as a tool in the diagnosis of smaller epithelial lesions, guiding resections, and to monitor the larynx after therapy." — Cummings Otolaryngology Head and Neck Surgery
What OCT Shows in the Larynx:
| Finding | OCT Appearance |
|---|---|
| Normal epithelium | Thin, uniform superficial layer; clear basement membrane |
| Dysplasia / CIS | Thickened, irregular epithelium; disrupted architecture |
| Invasive carcinoma | Loss of layered structure; irregular deep infiltration |
| Subglottic scarring | Fibrous, hyporeflective bands below surface |
Clinical Uses:
- 🔍 Detect precancerous changes (dysplasia) without biopsy
- ✂️ Guide phonomicrosurgery — know exactly where to cut
- 📊 Monitor response to therapy — has the cancer been fully treated?
- 🩺 Office-based surveillance of at-risk patients (smokers, post-radiation)
3. 👃 THE NOSE & SINUSES — Emerging Territory
OCT in rhinology is less established but growing. Key applications include:
- Sinonasal mucosal assessment — measuring cilia and subepithelial layers
- Ciliary beat frequency measurement — relevant in primary ciliary dyskinesia (PCD) and chronic rhinosinusitis
- Nasopharyngeal tumor margin assessment
- Endoscopic-guided OCT during sinus surgery to check resection margins
🛠️ How It's Done — OCT Delivery in ENT
| Body Part | OCT Delivery Method |
|---|---|
| Middle ear | Handheld OCT otoscope (point at the drum) |
| Cochlea | Miniaturized probe via middle ear approach during surgery |
| Larynx | Fiber-optic probe through working channel of laryngoscope |
| Nose/sinuses | Endoscope-integrated probe |
⚡ OCT vs. Other Imaging Modalities — The "Olympics" of ENT Imaging
| Feature | OCT | Ultrasound | CT | MRI |
|---|---|---|---|---|
| Resolution | ⭐⭐⭐⭐⭐ (~5–15 µm) | ⭐⭐ (~0.1 mm) | ⭐⭐ (~0.5 mm) | ⭐⭐⭐ |
| Penetration | ⭐⭐ (1–3 mm) | ⭐⭐⭐⭐ | ⭐⭐⭐⭐⭐ | ⭐⭐⭐⭐⭐ |
| Real-time | ✅ | ✅ | ❌ | ❌ |
| Radiation | ✅ None | ✅ None | ❌ Yes | ✅ None |
| Cost | ⭐⭐⭐ | ⭐⭐ | ⭐⭐⭐⭐ | ⭐⭐⭐⭐⭐ |
| Tissue contact needed | ❌ No | ✅ Yes | ❌ | ❌ |
🧠 The Creative Summary: OCT as a "Story"
Imagine your ENT doctor's clinic of the future:
-
A child comes in with a red ear and a crying parent. Instead of guessing — the doctor picks up an OCT otoscope, fires a beam of light at the eardrum, and sees a swirling cloud of fluid in the middle ear on the screen. Diagnosis: acute otitis media. Antibiotic prescribed. No needle, no tears.
-
A singer notices hoarseness. Instead of going to the OR for a biopsy under general anesthesia, the ENT passes a fiber-optic OCT probe through a flexible scope. Cross-sectional images reveal a thickened, irregular epithelial layer at the anterior commissure. Early dysplasia. Treated before it became cancer.
-
A Ménière's patient undergoes ear surgery and the surgeon deploys an OCT probe into the inner ear. The endolymph volume is elevated — confirming the hydrops. The surgical approach is adjusted in real time.
📚 Sources
- Cummings Otolaryngology Head and Neck Surgery — Endoscopic Imaging (Ch. 106); Cochlear Mechanics (Ch. 148)
- Recent evidence: OCT for pediatric middle ear effusion shows performance comparable to pneumatic otoscopy and tympanometry (The Laryngoscope, 2025 — PMID 41342403)
- USC Keck School of Medicine research on inner ear OCT for Ménière's disease (2024)
This is a shared conversation. Sign in to Orris to start your own chat.