Otitis media
Reading File
Finding Sources
Searching PubMed
"otitis media"[MeSH Terms] AND "treatment"[MeSH Terms]
Reading File
Reading File
Reading File
Searching Images
acute otitis media tympanic membrane
Reading File
I now have comprehensive information to construct a thorough answer. Let me compile the full response.
Otitis Media
Definition & Types
Otitis media (OM) refers to inflammation of the middle ear. Three main forms exist:
| Type | Key Feature |
|---|---|
| Acute Otitis Media (AOM) | Acute middle ear infection with effusion and inflammation |
| Otitis Media with Effusion (OME) | "Glue ear" — fluid without signs of acute infection |
| Chronic Otitis Media (COM) | Persistent perforation ± cholesteatoma |
Epidemiology
- Most common infection for which children visit a physician
- By age 7, 93% of children have had at least one AOM episode; 75% have had recurrent infections
- Peak incidence: 6–24 months
- Annual cost in the US: ~$2.88 billion
Pathophysiology
Primary cause is eustachian tube dysfunction — abnormal tubal compliance and delayed innervation of the tensor veli palatini muscle leads to tube collapse, impaired drainage, and negative middle ear pressure. Nasopharyngeal bacteria colonize the middle ear space through this dysfunctional tube. A viral URI typically precedes AOM.
Microbiology
| Organism | Frequency |
|---|---|
| Streptococcus pneumoniae | 25–40% |
| Haemophilus influenzae | 10–30% |
| Moraxella catarrhalis | 2–15% |
Viruses and anaerobes also contribute. S. pneumoniae resistance to penicillin (via altered penicillin-binding proteins, not β-lactamase) ranges 15–50% regionally and is higher in children in daycare or with recent antibiotic exposure.
Risk Factors
- Male sex
- Age < 2 years
- Bottle feeding in supine position
- Daycare attendance / winter season
- Parental smoking
- Pacifier use
- Allergy
- Craniofacial abnormalities (e.g., cleft palate)
- Previous AOM within 3 months
- Genetic/ethnic factors (Inuit, Native American)
Clinical Features
Symptoms: ear pain (tugging/holding/rubbing in nonverbal children), fever, irritability, otorrhea, diminished hearing, tinnitus, vertigo, vomiting, loss of appetite.
Diagnosis of AOM requires ALL of:
- Middle ear effusion (MEE) — visualized as air-fluid level, bulging drum, reduced/absent TM mobility on pneumatic otoscopy, or flat tympanogram
- Signs of inflammation — acute onset of ear pain OR intense TM erythema, moderate to severe bulging of the TM, or new-onset otorrhea not due to otitis externa
Erythema of the TM alone (without MEE) = myringitis/tympanitis, not AOM.
Bullous myringitis (bullae on TM) is a variant of AOM — treatment does not differ.
Otoscopic Appearances
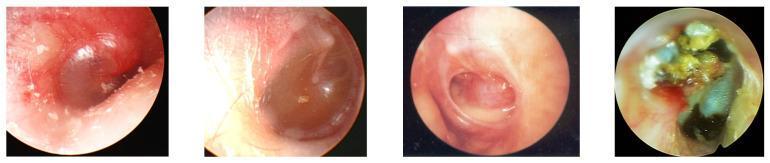
From left to right: AOM (erythema, bulging, loss of landmarks), OME (translucent, fluid with air-fluid level), COM (central perforation), COM with cholesteatoma (keratin debris, destruction).
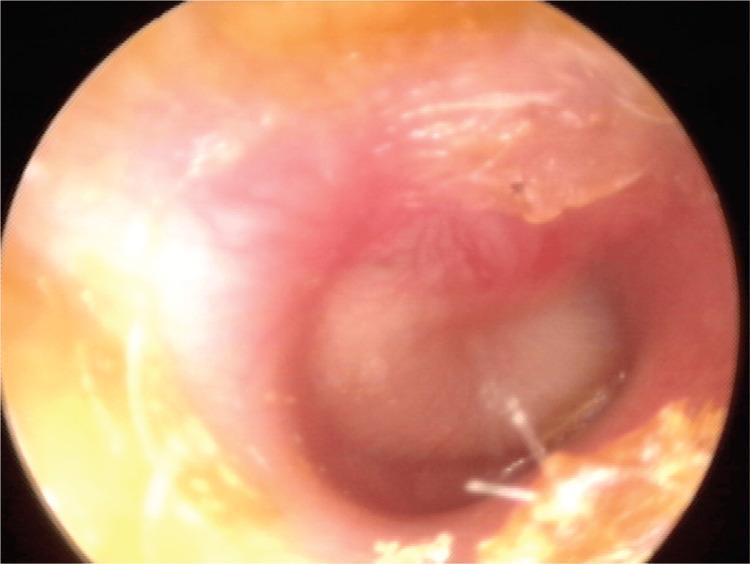
Treatment
Watchful Waiting vs. Immediate Antibiotics
Most AOM resolves spontaneously. The observation option (48–72 hours) is valid in appropriately selected patients — this is not validated in adults.
| Age | Criteria | Recommendation |
|---|---|---|
| < 6 months | Any | Immediate antibiotics |
| 6 months – 2 years | Bilateral AOM | Immediate antibiotics |
| 6 months – 2 years | Unilateral, non-severe | Observation acceptable |
| > 2 years | Severe (otalgia + fever > 39°C) | Immediate antibiotics |
| > 2 years | Non-severe, reliable follow-up | Observation acceptable |
Antibiotic Therapy
| Scenario | Drug & Dose |
|---|---|
| Low-risk (>6 yr, no recent antibiotics, afebrile, not in daycare, no otorrhea) | Amoxicillin 40–50 mg/kg/day ÷ doses × 5 days |
| High-risk (<2 yr, daycare, recent antibiotics, fever >38°C, otorrhea) | Amoxicillin 80–90 mg/kg/day ÷ doses × 10 days |
| Treatment failure (symptoms persist after 3 days) | Amoxicillin-clavulanate 80–90 mg/kg/day × 7–10 days OR Cefuroxime axetil 20–30 mg/kg/day × 7–10 days OR Ceftriaxone IM 50 mg/kg × 1–3 days |
| Penicillin allergy | Cefuroxime axetil, cefpodoxime, or ceftriaxone |
Note: Antibiotics alone do NOT relieve pain in the first 24 hours. Always add analgesics (acetaminophen or ibuprofen) for pain.
Special Situations
- Acute perforation with otorrhea: treat same as AOM without perforation; small perforations usually heal spontaneously
- Tympanostomy tube with acute otorrhea: ototopical fluoroquinolone drops (NOT aminoglycosides — these are ototoxic if TM is non-intact)
Otitis Media with Effusion (OME)
- Fluid in middle ear without signs of acute infection
- Common after AOM; may persist for weeks
- Most resolve spontaneously — monitor with tympanometry and audiometry
- Tympanostomy tubes indicated for persistent bilateral OME with hearing loss, especially in children with developmental concerns
Complications
| Complication | Notes |
|---|---|
| Tympanic membrane perforation | Usually small, heals spontaneously; keep ear dry; refer if not healed in weeks |
| Mastoiditis | Most common suppurative complication; presents with postauricular erythema/tenderness, auricle protrusion; CT if intracranial involvement suspected |
| Cholesteatoma | Keratin-filled cyst in middle ear/mastoid; destructive; requires surgical excision |
| Meningitis, brain abscess, sinus thrombosis | Rare intracranial extensions |
| Conductive hearing loss | From persistent MEE or ossicular damage |
Recurrent AOM
Defined as ≥3 episodes in 6 months or ≥4 in 12 months. Options include:
- Observation without prophylactic antibiotics (preferred)
- Tympanostomy tube insertion — reduces frequency of AOM and restores hearing in OME
Sources: Textbook of Family Medicine 9e, ch. 18; Rosen's Emergency Medicine, ch. 10
This is a shared conversation. Sign in to Orris to start your own chat.