Corneal ulcer
Reading File
Finding Sources
Searching PubMed
"corneal ulcer" OR "infectious keratitis"
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Reading File
Finding Sources
Reading File
Reading File
Reading File
Searching Images
corneal ulcer hypopyon slit lamp
Loading Image
Reading File
I now have comprehensive information from multiple authoritative textbooks. Let me compile a thorough answer.
Corneal Ulcer (Ulcerative Keratitis)
Definition & Pathophysiology
A corneal ulcer is an infectious or inflammatory erosion involving both the outer epithelial layer and the underlying corneal stroma. It develops when breaks in the epithelial barrier allow infectious agents to invade stromal tissue. The majority of corneal damage is caused by the secondary inflammatory response, not the organism itself.
Mechanisms of epithelial disruption include:
- Trauma or corneal abrasion becoming secondarily infected
- Contact lens wear (especially extended-wear/overnight)
- Desiccation from incomplete lid closure (e.g., Bell's palsy → exposure keratitis)
- Immunosuppression (topical/systemic steroids, systemic immunosuppressants)
— Tintinalli's Emergency Medicine, block 20; Rosen's Emergency Medicine, block 9
Etiology / Causative Organisms
| Category | Organisms |
|---|---|
| Bacteria | Pseudomonas aeruginosa (contact lenses), S. pneumoniae, Staphylococcus spp., Moraxella spp. |
| Viruses | Herpes simplex virus (most common cause of central corneal ulcer), Varicella-zoster virus |
| Fungi | Candida, Aspergillus, Penicillium, Fusarium, Acremonium |
| Acanthamoeba | Contact lens wearers, contaminated water |
| Mycobacteria / Nocardia | Post-refractive surgery, trauma |
Key associations:
- Pseudomonas → contact lens wearers
- Fungal → corticosteroid drop users, agricultural workers (vegetation/soil inoculation)
- HSV → most common cause requiring corneal transplant in the USA
- Acanthamoeba → contact lens wearers swimming or using tap water
— Rosen's Emergency Medicine, p. 892; Tintinalli's, p. 241
Clinical Features
Symptoms:
- Ocular pain / foreign body sensation
- Photophobia (often consensual — ciliary spasm from associated iritis)
- Redness, tearing, mucopurulent discharge
- Blurred or decreased vision (if ulcer is in the visual axis, or if uveitis is present)
Signs:
- Eyelid/conjunctival erythema, mucopurulent discharge
- Corneal ulcer: round or irregular white/hazy base with heaped-up edges and stromal infiltration due to WBC infiltration
- Associated iritis: miotic pupil, ciliary flush
- Slit-lamp: flare and cells in anterior chamber
- Hypopyon (layering of inflammatory cells in the inferior anterior chamber) — indicates severe inflammation/infection
HSV-specific: Classic dendritic lesion on slit lamp with fluorescein; may present with amoeba-shaped ulceration or punctate epithelial erosions
HZV-specific: Dermatomal vesicular rash (forehead/upper eyelid), Hutchinson's sign (nasal tip involvement = naso-ciliary branch = high risk of ocular involvement), associated iritis/uveitis/choroiditis
Clinical Images
Corneal ulcer with marked perilimbal injection and hypopyon (arrow):
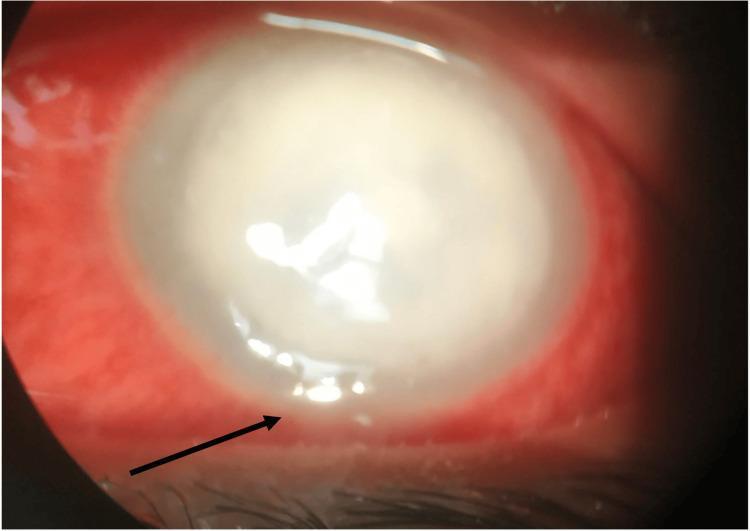
Slit-lamp photograph showing a large, dense yellowish-white central corneal abscess with marked perilimbal injection and a 1 mm hypopyon (arrow) in the inferior anterior chamber — characteristic of severe infectious keratitis.
Diagnosis
- Clinical — slit-lamp examination is the cornerstone
- Fluorescein staining — ulcer has "heaped-up" edges (vs. flat abrasion), with stromal edema/whitening
- Corneal scraping — should be performed in most cases; sent for:
- Gram stain (bacteria, fungi)
- Giemsa stain (bacteria, Acanthamoeba)
- Calcofluor white (Acanthamoeba, fungi — requires fluorescent microscope)
- Acid-fast stain (Mycobacteria, Nocardia)
- Culture & sensitivity
TIP: The causative organism cannot be reliably determined from the morphological appearance of the ulcer alone. Empirical broad-spectrum treatment is started before culture results return.
— Kanski's Clinical Ophthalmology, p. 230
Management
General Measures
- Discontinue contact lens wear immediately (mandatory)
- Protective eye shield if significant corneal thinning or perforation risk
- Emergent ophthalmology consultation — corneal ulcers can rapidly progress to permanent vision loss
- Consider hospital admission for: aggressive disease, an only eye, poor compliance
Antibiotic Treatment
Empirical (first-line):
- Fluoroquinolone monotherapy — ciprofloxacin or ofloxacin 1 drop every hour day and night for 24–48 h, then tapered
- Alternatively: moxifloxacin or gatifloxacin (newer-generation; better Gram-positive coverage, superior penetration)
- Duotherapy (aggressive disease or suspected streptococci): fortified cephalosporin + fortified aminoglycoside (e.g., cefuroxime 5% + gentamicin 1.5%)
Targeted:
| Isolate | Agent |
|---|---|
| Gram-positive cocci | Cefuroxime 0.3%, vancomycin 5%, or teicoplanin 1% |
| Gram-negative rods | Fortified gentamicin 1.5% or fluoroquinolone |
| Gram-negative cocci | Ceftriaxone 5% or ceftazidime |
| Mycobacteria | Amikacin 2% or clarithromycin 1% |
| Nocardia | Amikacin 2% or TMP-SMX |
TIP: Fluoroquinolones have limited activity against Gram-positive organisms, particularly Streptococcus. Ciprofloxacin drops can cause white corneal precipitates that may delay re-epithelialization.
Antifungal Treatment
- Natamycin (first-line for filamentous fungi)
- Amphotericin B or fluconazole (Candida/yeasts)
- Topical steroids are contraindicated when fungal infection is suspected
Antiviral Treatment
- HSV keratitis: Topical ganciclovir 0.15% gel (3–5×/day) or trifluridine 1% (5–9×/day × 14 days); systemic acyclovir/valacyclovir for severe or refractory cases. Avoid topical steroids (worsen HSV infection)
- HZV keratitis: Systemic therapy is standard — acyclovir 800 mg 5×/day, or valacyclovir 1000 mg 3×/day × 7–10 days. Treat within 72 hours of rash onset to reduce acute pain and ocular complications
Adjunctive
- Cycloplegics (cyclopentolate 1%, homatropine 2%, atropine 1%) — prevent posterior synechiae, reduce ciliary spasm pain
- Systemic antibiotics indicated for: N. meningitidis (life-saving — IM benzylpenicillin/ceftriaxone), N. gonorrhoeae (ceftriaxone), H. influenzae (amoxicillin-clavulanate), threatened corneal perforation (ciprofloxacin + doxycycline for anti-collagenase effect)
- Steroids (topical): controversial; reduce scarring but promote fungal/mycobacterial/HSV replication; use only after infection is controlled under specialist supervision
— Kanski's Clinical Ophthalmology, pp. 230–232; Tintinalli's, block 20
Complications
- Corneal perforation — may require bandage contact lens, tissue glue, or penetrating keratoplasty/patch graft
- Endophthalmitis
- Corneal scarring → permanent visual impairment
- Treatment failure — if no improvement in 24–48 h, review cultures; if still failing after a further 48 h, suspend treatment and re-scrape on broader media; consider corneal biopsy
- Consider PACK-CXL (photoactivated chromophore-enhanced collagen cross-linking) if corneal melting or antibiotic resistance is suspected
Disposition
Most corneal ulcers are treated as outpatients after ophthalmology consultation with topical (or systemic) antimicrobials. If ED ophthalmology is unavailable, refer for follow-up within 24 hours. Admission is considered for severe symptoms, an only eye, or inability to follow up urgently.
Recent Evidence
A 2025 Cochrane network meta-analysis (PMID: 40728038) on topical antibiotics for bacterial keratitis and a 2026 systematic review/meta-analysis on global burden and causative organisms in bacterial keratitis (PMID: 41422890) are the most recent high-quality evidence — these may update local resistance profiles and first-line antibiotic recommendations. Review these if managing antibiotic-refractory or region-specific cases.
This is a shared conversation. Sign in to Orris to start your own chat.