Hello
Explain diabetes retinopathy stages
Reading File
Finding Sources
Searching PubMed
"diabetic retinopathy"[MeSH Terms] AND classification
Reading File
Reading File
Searching Images
diabetic retinopathy stages fundus
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Reading File
I now have everything needed to provide a comprehensive, well-sourced answer. Here it is:
Diabetic Retinopathy — Stages & Classification
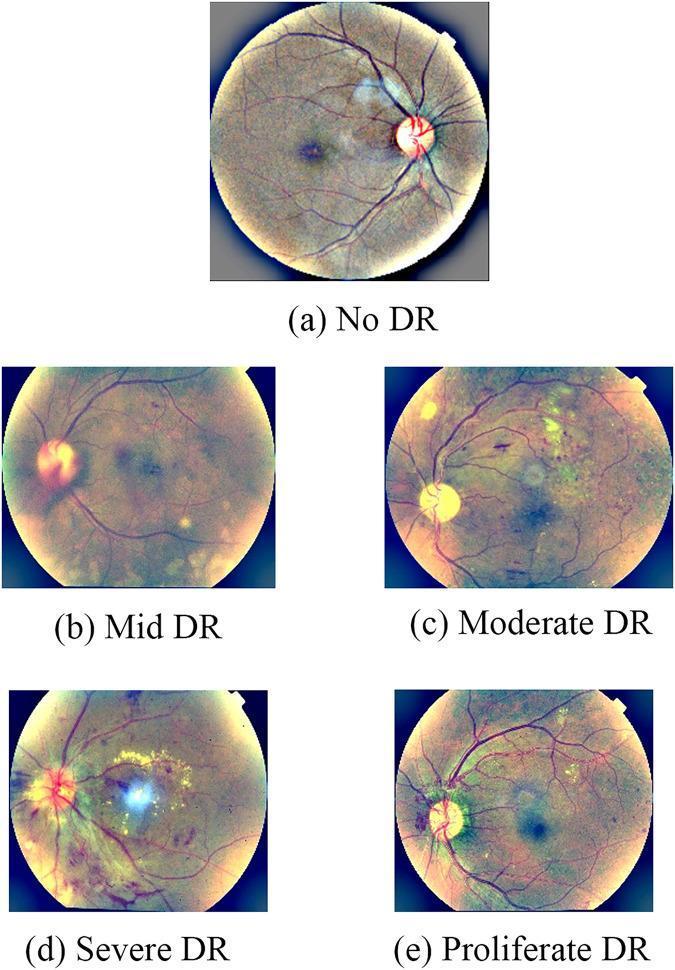
Diabetic retinopathy (DR) is predominantly a microangiopathy — high glucose levels damage small retinal blood vessels, leading to capillary pericyte loss, basement membrane thickening, and ultimately ischaemia. VEGF is a key mediator of the neovascular complications. It is the commonest cause of new blindness in most industrialised countries.
Classification Systems
Two overlapping systems are used:
- ETDRS (modified Airlie House) classification — the international gold standard, used in clinical trials and screening programmes
- Descriptive clinical categories — widely used in day-to-day practice
Stage-by-Stage Breakdown (ETDRS)
🔵 No Diabetic Retinopathy
- Normal fundus; no lesions visible
- Follow-up: 12 months
🟡 Non-Proliferative Diabetic Retinopathy (NPDR)
NPDR represents progressively worsening microvascular damage without new vessel growth.
| Stage | Key Features | Risk of Progression | Follow-up |
|---|---|---|---|
| Very Mild NPDR | Microaneurysms only | Low | 12 months |
| Mild NPDR | Microaneurysms + any/all of: dot-blot haemorrhages, hard exudates, cotton-wool spots — but no IRMA | Low | 6–12 months |
| Moderate NPDR | Severe haemorrhages (>20 medium-large per quadrant) in 1–3 quadrants; mild IRMA; venous beading in ≤1 quadrant | PDR in up to 26%, high-risk PDR in up to 8% within 1 year | ~6 months |
| Severe NPDR ("4-2-1 rule") | Any one of: haemorrhages in all 4 quadrants, venous beading in ≥2 quadrants, moderate IRMA in ≥1 quadrant | PDR in up to 50%, high-risk PDR in up to 15% within 1 year | 4 months |
| Very Severe NPDR | Two or more criteria from severe NPDR | High-risk PDR in up to 45% within 1 year | 2–3 months |
Key individual signs in NPDR:
- Microaneurysms — earliest sign; saccular outpouchings of capillary walls, appear as tiny red dots
- Dot and blot haemorrhages — intraretinal blood from ruptured microaneurysms/capillaries
- Hard exudates — yellow, waxy lipid deposits from leaky vessels, often arranged in rings (circinate pattern)
- Cotton-wool spots (CWS) — white fluffy patches from nerve fibre layer infarcts; indicate ischaemia
- Venous beading — sausage-like irregularity of veins; marker of significant ischaemia
- IRMA (intraretinal microvascular abnormalities) — dilated, abnormal intraretinal vessels bypassing occluded capillaries; precursor to NVD/NVE
🟠 Proliferative Diabetic Retinopathy (PDR)
Retinal ischaemia triggers neovascularisation — fragile new vessels grow on the disc or retinal surface, prone to haemorrhage.
| Stage | Key Features | Management |
|---|---|---|
| Mild–Moderate PDR | NVD or NVE present, but below high-risk criteria | Treatment considered; review within 2 months if not treated |
| High-Risk PDR | Any of: NVD >1/3-disc area; any NVD + vitreous haemorrhage; NVE >1/2-disc area + vitreous haemorrhage; or any NVI/NVA | Immediate treatment — panretinal photocoagulation (PRP) or anti-VEGF |
- NVD = new vessels on/within 1 disc diameter of the optic disc
- NVE = new vessels elsewhere in the retina
- NVI/NVA = neovascularisation of iris/angle → neovascular glaucoma risk
🔴 Advanced Diabetic Eye Disease
The end-stage of untreated PDR:
- Tractional retinal detachment — fibrovascular membranes contract and pull the retina
- Persistent/dense vitreous haemorrhage — obscures vision, may require vitrectomy
- Neovascular glaucoma (NVG) — rubeosis iridis (iris neovascularisation) → raised IOP
Diabetic Macular Oedema (DMO/DME)
DMO can occur at any stage of DR and is the commonest cause of vision loss in diabetic patients (especially type 2). It results from breakdown of the blood-retinal barrier and fluid accumulation in the macula.
- Clinically significant macular oedema (CSMO): retinal thickening or hard exudates at or threatening the foveal centre → treatment indication
- Detected clinically by slit-lamp biomicroscopy; confirmed by OCT
- Treatment: intravitreal anti-VEGF (first-line), focal/grid laser, or intravitreal steroids
Risk Factors for Progression
| Factor | Effect |
|---|---|
| Duration of diabetes | Strongest predictor overall |
| Poor glycaemic control (↑HbA1c) | Strongest modifiable risk |
| Hypertension | Accelerates progression |
| Nephropathy | Closely parallels retinopathy severity |
| Pregnancy | Can rapidly worsen existing retinopathy |
| Dyslipidaemia | Associated with hard exudate formation |
Treatment Summary by Stage
| Stage | Treatment |
|---|---|
| No DR / Mild NPDR | Optimise glycaemia, BP, lipids; regular screening |
| Moderate–Severe NPDR | Medical optimisation; consider anti-VEGF if DMO present |
| High-Risk PDR | PRP (panretinal photocoagulation) or anti-VEGF |
| DMO affecting fovea | Intravitreal anti-VEGF (ranibizumab, aflibercept, bevacizumab) |
| Advanced eye disease | Vitrectomy (for dense VH, tractional RD, ERM) |
With effective screening and current treatments, the risk of severe visual loss from DR can be reduced to less than 5%.
Sources: Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed.; The Wills Eye Manual, 8th ed.; Goldman-Cecil Medicine, International Edition
This is a shared conversation. Sign in to Orris to start your own chat.