Management of Racoon eye caused due to blunt force trauma to to forehead
Reading File
search_medical_text
raccoon eyes periorbital ecchymosis blunt trauma management
search_medical_text
anterior cranial fossa fracture basilar skull fracture diagnosis treatment
search_medical_image
raccoon eyes periorbital ecchymosis skull fracture
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive clinical overview:
Raccoon Eyes (Periorbital Ecchymosis) from Blunt Forehead Trauma
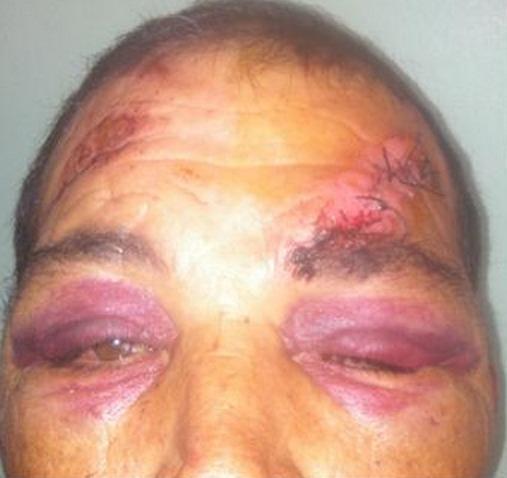
Pathophysiology
Blunt force to the forehead transmits force to the anterior cranial fossa floor (orbital plates of the frontal bone, cribriform plate, ethmoid). Blood from the fracture site tracks anteriorly through fascial planes and pools in the periorbital subcutaneous tissue, producing the characteristic bilateral "raccoon eyes." Because this is blood tracking from a deep fracture — not a direct contusion — it respects the orbital rim and appears without lid swelling initially.
What Raccoon Eyes Signify
| Sign | Likely Fracture Site |
|---|---|
| Raccoon eyes (bilateral periorbital ecchymosis) | Anterior cranial fossa / orbital plate fracture |
| Battle's sign (mastoid ecchymosis) | Middle cranial fossa / petrous temporal fracture |
| CSF rhinorrhoea | Dural tear + anterior skull base defect |
| CSF otorrhoea | Dural tear + petrous fracture |
| Anosmia | Cribriform plate / olfactory nerve injury |
Raccoon eyes from forehead trauma = basilar skull fracture until proven otherwise.
Initial Assessment & Stabilization
1. Primary Survey (ATLS Protocol)
- Airway — protect if GCS ≤ 8 or airway at risk
- C-spine immobilization — mandatory until cleared; associated cervical injury must be excluded
- Neurological status — GCS, pupils (size, reactivity, symmetry), focal deficits
2. Immediate Red Flags Requiring Urgent Neurosurgical Consultation
- GCS < 14 or deteriorating level of consciousness
- Unequal or blown pupil
- CSF rhinorrhoea (clear watery nasal discharge — confirm with β₂-transferrin assay)
- Signs of raised intracranial pressure (Cushing's triad: hypertension, bradycardia, irregular respirations)
- Coagulopathy or anticoagulant use
Investigations
| Investigation | Purpose |
|---|---|
| Non-contrast CT head (first-line) | Identify fracture, intracranial hemorrhage (EDH, SDH, contusion), pneumocephalus |
| High-resolution CT skull base | Delineate anterior cranial fossa bony defect, cribriform plate integrity |
| CT cervical spine | Exclude concomitant cervical injury |
| β₂-transferrin assay (nasal/ear fluid) | Confirm CSF leak |
| MRI brain | Assess dural tear, parenchymal injury, cranial nerve involvement |
| Ophthalmology consult | Visual acuity, fundoscopy (retinal hemorrhage, optic nerve injury) |
Management
A. Conservative (Most Anterior Fossa Fractures Without Complications)
Most basilar skull fractures — including anterior fossa fractures causing raccoon eyes — heal without operative intervention.
- Bed rest with head elevated 30–45°
- Strict avoidance of nose-blowing, sneezing with open mouth, straining (Valsalva maneuver) — prevents pneumocephalus and CSF leak exacerbation
- Analgesia — paracetamol preferred; NSAIDs and aspirin avoided (bleeding risk)
- Monitor neurological status closely; repeat CT if deterioration
B. CSF Rhinorrhoea Management
(Bailey & Love's, p. 786)
- Conservative first — most CSF leaks from anterior skull base settle spontaneously within 7–10 days with bed rest and head elevation
- Lumbar drain — if leak persists beyond 7–10 days, reduces CSF pressure and allows dural healing
- Endoscopic endonasal repair — definitive treatment for persistent or recurrent CSF leaks; bony defect identified on high-resolution CT and patched (fat, fascia, mucosal flap ± synthetic material)
- Open craniotomy — reserved for large defects not amenable to endoscopic repair
C. Prophylactic Antibiotics
- Controversial — routine prophylactic antibiotics for basilar skull fracture are not recommended by most guidelines (Cochrane evidence shows no reduction in meningitis; may select resistant organisms)
- Treat established meningitis or sinusitis aggressively if it develops
D. Surgical Indications (Neurosurgical)
- Epidural/subdural hematoma with mass effect
- Depressed skull fracture over anterior fossa
- Persistent CSF leak (>10–14 days) or recurrent meningitis
- Significant pneumocephalus (tension pneumocephalus is a neurosurgical emergency)
- Optic canal fracture with visual compromise — decompression may be considered
E. Ophthalmological Management
- Rule out traumatic optic neuropathy, retrobulbar hematoma, globe injury
- Retrobulbar hematoma causing orbital compartment syndrome: lateral canthotomy + cantholysis is an emergency procedure
F. The Raccoon Eyes Themselves
- No specific local treatment is required for the periorbital ecchymosis per se — it resolves spontaneously over 2–3 weeks
- Cold compresses in the first 24–48 hours may limit spread
- The ecchymosis is a sign, not the primary problem; management targets the underlying injury
Complications to Monitor
| Complication | Timeframe | Action |
|---|---|---|
| Extradural/subdural hematoma | Acute (hours) | Emergency surgical evacuation |
| Tension pneumocephalus | Acute | Urgent needle decompression / surgery |
| Meningitis / brain abscess | Days–weeks | Antibiotics + source control |
| CSF leak persistence | Days | Endoscopic repair |
| Anosmia | Immediate / delayed | Olfactory rehabilitation; often permanent |
| Post-traumatic epilepsy | Weeks–months | EEG; antiepileptics if indicated |
| Traumatic optic neuropathy | Immediate | Ophthalmology; consider decompression |
Key Takeaway
Raccoon eyes following blunt forehead trauma are a reliable clinical marker of anterior cranial fossa fracture. The management priority is not the ecchymosis itself but:
- Ruling out life-threatening intracranial injury (CT head urgently)
- Detecting and managing CSF leak (β₂-transferrin, conservative vs. endoscopic repair)
- Preventing infectious complications (meningitis, abscess)
- Neurosurgical and ophthalmological consultation based on findings
(Bailey and Love's Short Practice of Surgery, 28th Ed., p. 786)
Without skull fracture
search_medical_text
periorbital ecchymosis raccoon eyes without skull fracture blunt trauma management
search_medical_text
periorbital hematoma soft tissue injury forehead blunt trauma treatment
GradeResponse
GradeResponse
This is an important clinical distinction. Here is the focused answer:
Raccoon Eyes from Blunt Forehead Trauma — Without Skull Fracture
Understanding the Mechanism
When blunt force hits the forehead without fracturing the skull, raccoon eyes result from direct soft tissue injury:
- Trauma ruptures small subcutaneous and periorbital vessels in the forehead/supraorbital region
- Blood tracks downward by gravity through loose areolar tissue of the eyelids (which has virtually no resistance)
- It pools in both periorbital regions, producing bilateral ecchymosis
- The orbital septum confines the blood, giving the characteristic circumferential "raccoon" appearance
This is a purely soft tissue phenomenon — no dural tear, no CSF, no intracranial pathology.
Confirming the Absence of Fracture
Before managing conservatively, fracture must be adequately excluded:
| Step | Detail |
|---|---|
| CT head (non-contrast) | Gold standard — rules out skull fracture, intracranial hemorrhage |
| Clinical exam | No CSF rhinorrhoea, no anosmia, no Battle's sign, no hemotympanum, no focal neuro deficit |
| β₂-transferrin | Only if any doubt about nasal clear discharge being CSF |
| GCS assessment | Must be normal (15) for conservative soft-tissue management |
Once fracture and intracranial injury are excluded, management is entirely supportive and symptomatic.
Management of Soft-Tissue Raccoon Eyes (No Fracture)
1. Immediate Phase (0–48 hours)
- Ice/cold compresses applied intermittently (20 min on, 20 min off) — reduces ongoing extravasation, limits ecchymosis spread and swelling
- Head elevation (30°) — reduces dependent pooling of blood in periorbital tissue
- Rest — avoid straining, bending forward
- Analgesia — paracetamol; avoid NSAIDs and aspirin (antiplatelet effect worsens bleeding)
2. Subacute Phase (48 hours–2 weeks)
- Warm compresses after 48 hours — promotes vasodilation and reabsorption of the hematoma
- Gentle massage (after 48–72 hours) — aids lymphatic drainage
- No patching or occlusion of the eye is necessary unless there is corneal/conjunctival injury
3. Eye Care
- Ophthalmology review if:
- Visual acuity is reduced
- Diplopia (suggests orbital floor blow-out or extraocular muscle injury)
- Subconjunctival hemorrhage extending posteriorly (may indicate orbital fracture)
- Proptosis or restricted eye movements
- Routine lubricating eye drops if periorbital swelling causes incomplete lid closure (exposure keratopathy risk)
4. Associated Forehead Laceration (if present)
(Bailey & Love's, 28th Ed., p. 430)
- Clean and irrigate wound thoroughly
- Repair in layers under local anaesthesia within 24 hours
- Debride only frankly necrotic tissue — the face has rich blood supply and heals well
- Tetanus prophylaxis as appropriate
5. Patient Education
- Inform the patient the discolouration will worsen for 48–72 hours before improving — this is normal tracking of blood, not a sign of progression
- Full resolution expected in 2–3 weeks
- Return immediately if: vision changes, headache worsens, any clear nasal discharge, vomiting, or drowsiness develop
Natural History
| Timeframe | Expected Change |
|---|---|
| 0–48 hours | Ecchymosis spreads, darkens (purple-black) |
| 48–72 hours | Peak discolouration |
| Days 3–7 | Colour begins changing (green/yellow) as haemoglobin breaks down |
| 2–3 weeks | Complete resolution |
Key Points
- Without skull fracture, raccoon eyes are a benign self-limiting soft tissue condition
- No specific treatment accelerates resolution significantly — management is supportive
- The priority remains excluding intracranial and orbital injury before labelling it as purely soft tissue
- No antibiotics, no surgery, no steroids are indicated
- Ophthalmology referral is only needed if ocular symptoms are present
This is a shared conversation. Sign in to Orris to start your own chat.