Give me full information about varicose veins needed for surgery mbbs subject- theory and practical examination aspect with a case presentation and all ruling out aspects with reason in detail with summary for each point
Reading File
search_medical_text
varicose veins anatomy pathophysiology etiology classification CEAP
search_medical_text
varicose veins clinical examination Trendelenburg Perthe's Schwartz test investigations management surgery
search_medical_image
varicose veins anatomy saphenous vein clinical examination surgery
GradeResponse
GradeResponse
GradeResponse
I now have strong foundational results. Let me compile a comprehensive, MBBS-level examination-oriented answer covering all aspects requested.
Varicose Veins — Complete MBBS Surgery Reference
Covers: Theory | Practical/Clinical Examination | Case Presentation | Differentials with Reasoning | Summary per Section
1. DEFINITION
Varicose veins are abnormally dilated, tortuous, elongated superficial veins of the lower limb due to incompetence of venous valves, resulting in reversal of blood flow (reflux) and venous hypertension.
Key distinction: "Varix" = dilated vein. Varicosities must be >3 mm in diameter to be classified as varicose veins; smaller dilations are called reticular veins (<3 mm) or telangiectasias (<1 mm).
Summary: Varicose veins = dilated, tortuous superficial veins with valve incompetence causing reflux and venous hypertension.
2. SURGICAL ANATOMY (High-Yield for Exams)
Long Saphenous Vein (Great Saphenous Vein — GSV)
- Longest vein in the body
- Originates from the medial end of the dorsal venous arch of the foot
- Passes anterior to the medial malleolus, then runs along the medial aspect of the leg and thigh
- Passes through the saphenous opening (fossa ovalis) in the deep fascia 3.5–4 cm below and lateral to the pubic tubercle
- Drains into the femoral vein at the saphenofemoral junction (SFJ)
- Tributaries at SFJ (the "5 tributaries" — SEPIA mnemonic):
- Superficial external pudendal
- Epifascial circumflex iliac
- Posterolateral (posteromedial) thigh vein
- Inguinal (anterior femoral cutaneous) vein
- Anterior lateral thigh vein
Short Saphenous Vein (Small Saphenous Vein — SSV)
- Originates from the lateral end of the dorsal venous arch
- Passes posterior to the lateral malleolus, then up the posterior midline of the calf
- Pierces deep fascia in the popliteal fossa to drain into the popliteal vein at the saphenopopliteal junction (SPJ)
Perforating (Communicating) Veins
- Connect superficial and deep systems, with valves directing blood superficial → deep
- Cockett's perforators (medial lower leg, 7, 12, 18 cm above medial malleolus) — most clinically important
- Boyd's perforator — below the knee medially
- Hunterian (Dodd's) perforator — mid-thigh medially
Venous Valves
- Semilunar bicuspid valves; prevent retrograde flow
- Absent in: common iliac vein, inferior vena cava
- GSV has 8–20 valves; denser distally
Summary: GSV runs anteromedially from foot to SFJ; SSV runs posteriorly to SPJ in popliteal fossa. Cockett's perforators connect the two systems. Valve incompetence at SFJ is the most common cause of varicose veins.
3. ETIOLOGY AND RISK FACTORS
Primary Varicose Veins (Most Common — ~95%)
- Intrinsic weakness of the vein wall (structural defect in elastin/collagen)
- Congenital valve deficiency
- No identifiable secondary cause
Secondary Varicose Veins (~5%)
| Cause | Mechanism |
|---|---|
| Deep vein thrombosis (DVT) | Post-thrombotic deep vein obstruction → pressure transmitted to superficial veins |
| Pregnancy | Compression of IVC + progesterone-mediated smooth muscle relaxation |
| Pelvic tumour/mass | External compression of iliac veins |
| AV fistula (congenital/acquired) | Increased venous pressure |
| Klippel-Trénaunay syndrome | Congenital absence of deep veins |
Risk Factors (MBBS Exam Favourite)
- Female sex (progesterone effect) — F:M ratio 3:1
- Prolonged standing (occupational — barbers, surgeons, teachers)
- Obesity (increased intra-abdominal pressure)
- Multiparity
- Positive family history (50–70% of cases)
- Constipation/straining
- Age >40
Summary: Primary varicose veins result from intrinsic vein wall/valve weakness. Secondary causes include DVT, pregnancy, and pelvic masses. Key risk factors: female sex, prolonged standing, obesity, multiparity, family history.
4. PATHOPHYSIOLOGY
Valve incompetence (SFJ most common)
↓
Retrograde blood flow (reflux) in superficial veins
↓
Increased hydrostatic pressure in superficial veins
↓
Vein wall dilation and tortuosity
↓
Further valve incompetence (progressive)
↓
Sustained venous hypertension
↓
Capillary leak → Fibrin cuff deposition → Impaired O₂ diffusion
↓
Lipodermatosclerosis, eczema, ulceration
Key concept: The "Fibrin cuff theory" (Browse & Burnand) — venous hypertension causes pericapillary fibrin deposition that acts as a barrier to oxygen and nutrient diffusion → tissue ischaemia → ulceration.
Summary: Core pathology is valve incompetence → reflux → venous hypertension → structural vein changes → skin/tissue changes distally.
5. CEAP CLASSIFICATION (Harrison's, p. 7797)
The CEAP Classification (Clinical, Etiologic, Anatomic, Pathophysiologic) is the standard international classification:
C — Clinical
| Grade | Description |
|---|---|
| C0 | No visible/palpable signs |
| C1 | Telangiectasias or reticular veins |
| C2 | Varicose veins (≥3 mm diameter) |
| C3 | Oedema without skin changes |
| C4a | Pigmentation or eczema |
| C4b | Lipodermatosclerosis or atrophie blanche |
| C5 | Healed venous ulcer |
| C6 | Active venous ulcer |
Each grade is further subclassified as:
- s = symptomatic
- a = asymptomatic
E — Etiologic
- Ec = Congenital | Ep = Primary | Es = Secondary | En = No venous cause identified
A — Anatomic
- As = Superficial | Ap = Perforator | Ad = Deep
P — Pathophysiologic
- Pr = Reflux | Po = Obstruction | Pr,o = Both
Summary: CEAP is the standard classification. C2 = varicose veins; C6 = active ulcer. Always use this in theory exams.
6. CLINICAL FEATURES
Symptoms
| Symptom | Notes |
|---|---|
| Aching/heaviness | Worse after prolonged standing; relieved by elevation |
| Itching | Due to venous eczema |
| Cosmetic disfigurement | Most common presenting complaint in women |
| Night cramps | Calf cramps, especially at night |
| Ankle swelling | Worse in the evening |
| Restless legs | Poorly described discomfort |
Important: Pain is NOT a cardinal feature of uncomplicated varicose veins. Severe pain should raise suspicion of thrombophlebitis, DVT, or other diagnosis.
Signs
- Dilated, tortuous, visible veins along GSV/SSV territory
- Ankle oedema (pitting)
- Haemosiderin pigmentation (brownish discoloration around ankle — "gaiter area")
- Lipodermatosclerosis — woody induration of skin/subcutaneous tissue; "inverted champagne bottle" appearance
- Venous eczema (varicose eczema)
- Atrophie blanche — whitish, sclerotic plaques (marker of severe disease)
- Venous ulcer — typically over the medial malleolus (gaiter area)
- Corona phlebectatica — fan-shaped telangiectasias around the ankle (marker of severe CVI)
Summary: Main symptoms are aching, heaviness, itching, cosmetic concerns. Signs range from visible veins to lipodermatosclerosis and venous ulcers in advanced disease.
7. CLINICAL EXAMINATION (PRACTICAL/VIVA EXAM FAVOURITE)
Sequence (IPAC — Inspection, Palpation, Auscultation, Special Tests)
7.1 INSPECTION
- Patient standing (veins fill best in standing)
- Note: distribution (GSV, SSV, or both), tortuosity, dilatation
- Skin changes: pigmentation, eczema, lipodermatosclerosis, ulcer
- Saphena varix — dilatation of the terminal part of GSV at SFJ; seen as a bluish swelling at the saphenous opening → disappears on lying down; cough impulse positive
7.2 PALPATION
- Temperature of skin over varices
- Tenderness (thrombophlebitis)
- Consistency of swellings
- Tap test (Schwartz test):
- Tap the vein at one point; a transmitted fluid impulse felt at another point confirms continuity of the column of blood
- Indicates: varicose veins are present and blood column is continuous
- Limitation: Does not determine cause or competency
7.3 SPECIAL CLINICAL TESTS
A. Trendelenburg (Brodie-Trendelenburg) Test
Purpose: To identify the level of incompetence (SFJ vs. perforators)
Procedure:
- Patient lies supine; leg elevated to empty veins
- Compress the SFJ with thumb or tourniquet applied to upper thigh
- Patient stands
- Observe vein filling pattern
Interpretation:
| Finding | Diagnosis |
|---|---|
| Veins remain empty while tourniquet on → fill rapidly when released | SFJ incompetence (positive Trendelenburg test) |
| Veins fill rapidly from below even with tourniquet on | Perforator incompetence (below tourniquet) |
| Both patterns | SFJ + perforator incompetence |
According to Harrison's Principles (p. 7796): "Filling of varicose veins within 30 s indicates varicose veins caused by deep-venous insufficiency and incompetent perforating veins."
B. Multiple Tourniquet Test (Modified Trendelenburg)
- Tourniquets applied at multiple levels (upper thigh, lower thigh, below knee)
- Identifies the specific level of perforator incompetence
- The segment between two tourniquets where veins fill = site of incompetent perforator
C. Perthe's Test
Purpose: To assess patency and adequacy of deep veins (BEFORE any surgery)
Procedure:
- Apply tourniquet to upper thigh while patient standing
- Patient walks/exercises for 5 minutes
Interpretation:
| Finding | Diagnosis |
|---|---|
| Veins become less prominent / empty | Deep veins patent and functioning (safe to operate) |
| Veins become more prominent / painful | Deep veins obstructed (do NOT operate — superficial veins are collaterals; removing them causes venous gangrene) |
Critical for surgery: Perthe's test must be done before surgical intervention.
D. Fegan's Method (for Perforator Mapping)
- Patient stands; mark varices
- Elevate leg; palpate along medial aspect for fascial defects (gaps)
- Fascial defects = sites of perforating vein incompetence
- Most common: Cockett's zone (4–8 cm above medial malleolus)
E. Schwartz (Percussion/Tap) Test
- As described above — confirms blood column continuity
F. Morrissey's Cough Impulse Test
- A cough impulse felt at the SFJ (saphena varix) = SFJ incompetence
Summary: Key tests — Trendelenburg (SFJ incompetence), Multiple tourniquet (perforator level), Perthe's (deep vein patency, MANDATORY before surgery), Fegan's (perforator mapping), Schwartz (blood column continuity).
8. CLINICAL IMAGE — Advanced Varicose Veins
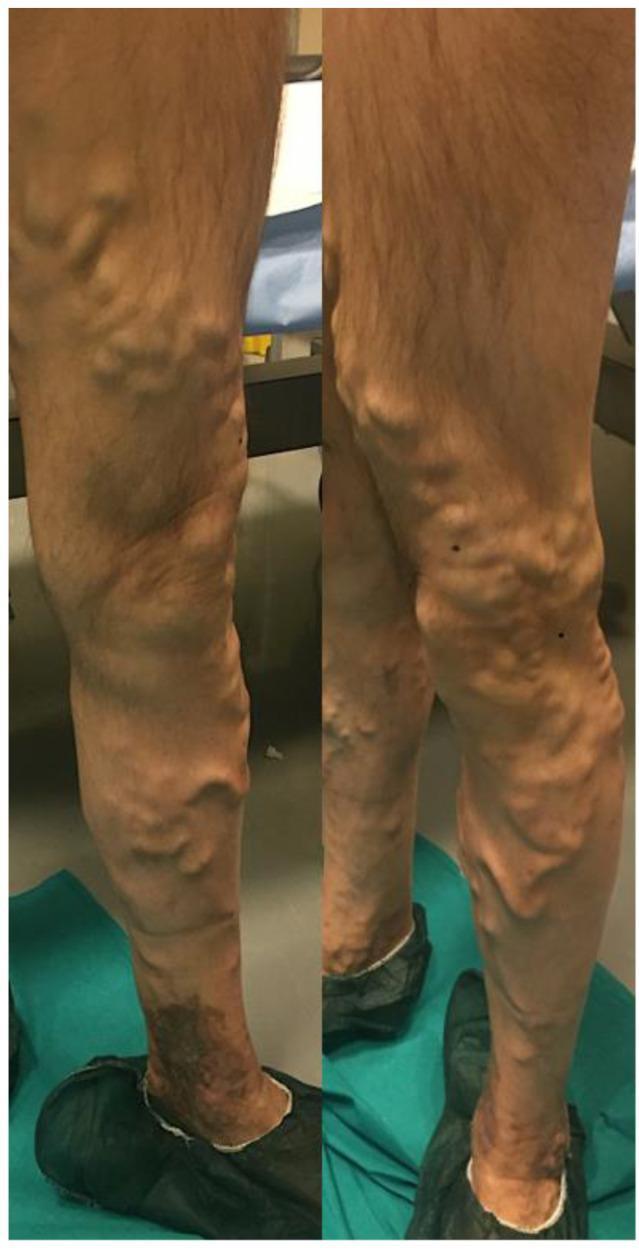
Posterior and medial views of the left lower limb showing extensive varicose veins in the GSV distribution with tortuous, protuberant varices from distal thigh to mid-calf. Note the hyperpigmentation and lipodermatosclerosis around the ankle — characteristic of advanced chronic venous insufficiency (CEAP C4b).
9. INVESTIGATIONS
9.1 Bedside
- Ankle-Brachial Pressure Index (ABPI): Must be >0.8 before applying compression or surgery; rules out arterial disease
9.2 Imaging (First-line)
Duplex Ultrasonography (Gold Standard)
- Combines B-mode ultrasound (anatomy) + Doppler (flow)
- Identifies:
- Site of SFJ/SPJ incompetence
- Reflux (retrograde flow >0.5 sec on Valsalva or calf release)
- Perforator incompetence
- Deep vein patency/thrombosis
- Mandatory before surgery
Hand-Held Doppler
- Detects reflux at SFJ and SPJ
- Cheaper but less accurate than duplex
9.3 Invasive (Rarely needed)
Ascending Venography
- Contrast injected into foot vein; outlines deep venous system
- Done when Klippel-Trénaunay syndrome or deep venous anomaly suspected
Descending Venography
- Contrast injected at femoral level; shows reflux
- Rarely used; replaced by duplex
9.4 Other
- Plethysmography (air/photoplethysmography) — measures venous refill time; not routinely used
- CT venography / MR venography — for pelvic vein assessment, May-Thurner syndrome
Pre-operative workup (Standard)
- CBC, blood grouping
- RFT, LFT
- Coagulation profile (PT/INR, aPTT)
- Blood glucose
- ECG, Chest X-ray
- Duplex ultrasound
Summary: Duplex ultrasound is the gold standard investigation — mandatory before surgery. ABPI must be checked before compression/surgery.
10. COMPLICATIONS OF VARICOSE VEINS (MBBS Exam — 5 marks commonly)
| Complication | Description |
|---|---|
| Superficial thrombophlebitis | Painful, tender, red cord along vein; treated conservatively |
| Haemorrhage | Spontaneous or traumatic; can be severe from thin skin over dilated vein; immediate treatment: elevation + pressure |
| Venous eczema | Itchy, weeping eczema over gaiter area |
| Lipodermatosclerosis | Induration and fibrosis of skin/fat (inverted champagne bottle leg) |
| Venous ulcer | Chronic, painless (unless infected), medial malleolus; shallow, irregular, sloping edges |
| Calcification | Phleboliths (calcified thrombi within veins) |
| Deep vein thrombosis | Propagation from superficial thrombophlebitis |
| Haemosiderin pigmentation | Brownish discoloration around ankle |
| Atrophie blanche | White sclerotic skin patches — high risk for ulceration |
Summary: Complications range from superficial thrombophlebitis to venous ulceration. Haemorrhage from varicose veins can be life-threatening due to the low-pressure but high-volume nature.
11. MANAGEMENT
11.1 Conservative (Non-operative)
Indications: Mild symptoms, patient unfit for surgery, pregnancy, patient preference
- Compression therapy:
- Graduated compression stockings (Class II: 18–24 mmHg or Class III: 25–35 mmHg)
- Compression bandages
- ABPI must be >0.8 before use
- Lifestyle modifications:
- Avoid prolonged standing
- Regular walking
- Weight loss
- Leg elevation (30° above heart level)
- Medications:
- Diosmin + Hesperidin (Daflon) — venotonic agents; reduce symptoms
- Topical steroids for eczema
11.2 Sclerotherapy
Principle: Injection of sclerosant causes endothelial damage → fibrosis → obliteration of vein
Types:
- Liquid sclerotherapy — for telangiectasias and small reticular veins
- Foam sclerotherapy (UGFS — Ultrasound-Guided Foam Sclerotherapy) — for larger veins; more effective
- Sclerosant: Sodium tetradecyl sulphate (STD) or Polidocanol (most used)
- Mixed with air/CO₂ in 1:4 ratio to create foam (Tessari technique)
Complications of sclerotherapy:
- Skin staining (hyperpigmentation)
- Allergic reaction
- Skin necrosis
- DVT, pulmonary embolism (rare)
- Matting (new telangiectasias)
- Visual disturbances (foam)
11.3 Endovenous Thermal Ablation (NICE-recommended first line for truncal veins)
a. Endovenous Laser Ablation (EVLA/EVLT)
- Laser fibre inserted into GSV under ultrasound guidance
- Thermal energy causes vein wall destruction → fibrosis
- Wavelengths: 810–1470 nm
- Done under tumescent anaesthesia
- Day-care procedure; rapid recovery
b. Radiofrequency Ablation (RFA/VNUS Closure)
- Radiofrequency catheter generates heat → collagen contraction → vein closure
- Segmental heating at 120°C
- Comparable outcomes to EVLA; slightly less bruising
11.4 Surgical Treatment
Indications for Surgery
- Progressive/troublesome symptoms
- Complications (ulcer, thrombophlebitis, haemorrhage)
- Cosmetic (patient choice)
- Failed conservative/sclerotherapy
Pre-operative Requirements
- Perthe's test — deep vein patency confirmed
- Duplex ultrasound mapping
- Mark veins while patient standing (day before surgery)
Operations
A. Trendelenburg Operation (Flush Ligation)
- SFJ ligation: Ligation of GSV at its junction with femoral vein, flush with the femoral vein
- All 5 tributaries at SFJ are also ligated
- Done through groin incision
- Critical point: Must be flush — leaving a stump = Neovascularisation → recurrence
B. Stripping of GSV
- Babcock's stripper inserted into the GSV from groin to knee level (not below knee — risks saphenous nerve injury)
- Vein stripped out
- Combined with SFJ ligation = Trendelenburg + Stripping
- Evidence shows stripping reduces recurrence compared to ligation alone
C. Phlebectomy (Stab Avulsion / Multiple Stab Avulsion)
- Multiple small (2–3 mm) stab incisions
- Varicose tributaries avulsed using hooks
- Excellent cosmetic result
- Done for tributaries not amenable to stripping
D. Subfascial Endoscopic Perforator Surgery (SEPS)
- For incompetent perforating veins
- Endoscopic ligation through small incisions
- Indicated for venous ulcers with perforator incompetence
E. Open Surgery for Perforators — Cockett's Operation
- Direct ligation of Cockett's perforators through a medial incision
Post-operative Care
- Compression bandaging for 1 week, then stockings
- Early ambulation (prevents DVT)
- Analgesics
- Monitor for: haematoma, nerve injury, DVT, wound infection
11.5 Comparative Summary of Treatments
| Treatment | Best For | Advantages | Disadvantages |
|---|---|---|---|
| Compression | Mild symptoms, pregnancy | Non-invasive | Not curative |
| Sclerotherapy (liquid) | Telangiectasias, reticular | Simple, outpatient | High recurrence for large veins |
| Foam sclerotherapy | Truncal veins, recurrence | Ultrasound guided, less invasive | DVT risk, visual disturbances |
| EVLA | Truncal GSV/SSV | Day-care, rapid recovery, low recurrence | Equipment cost |
| RFA | Truncal GSV/SSV | Less bruising than EVLA | Equipment cost |
| Surgery (Trendelenburg + strip) | All types, complex cases | Gold standard, low recurrence | GA/spinal, longer recovery |
Summary: NICE recommends EVLA/RFA as first-line for truncal varices. Surgery remains gold standard for complex/recurrent cases. Perthe's test must be performed before any intervention.
12. VENOUS ULCER (Important Exam Topic)
Features of Venous Ulcer
| Feature | Venous Ulcer |
|---|---|
| Site | Gaiter area — medial malleolus |
| Shape | Irregular, shallow |
| Edges | Sloping |
| Floor | Granulation tissue / pale/necrotic |
| Base | Indurated; lipodermatosclerosis |
| Pain | Mild to absent (unless infected) |
| Associated signs | Varicose veins, haemosiderin pigmentation, eczema |
| ABPI | >0.8 (distinguishes from arterial) |
Management of Venous Ulcer
- Four-layer compression bandaging (Charing Cross technique) — cornerstone
- Wound care: regular dressing, debridement
- Treat underlying varicose veins (after ulcer healing)
- Skin grafting (pinch grafts / split-skin grafts) for large ulcers
- SEPS / perforator ligation if perforator incompetence identified
Summary: Venous ulcers are medial, sloping-edged, shallow. Four-layer compression bandaging is the mainstay of treatment. ABPI must be >0.8 before compression.
13. DIFFERENTIAL DIAGNOSIS WITH DETAILED REASONING
13.1 Deep Vein Thrombosis (DVT)
| Feature | Varicose Veins | DVT |
|---|---|---|
| Location | Superficial | Deep (below fascia) |
| Tenderness | Only if thrombophlebitis | Present (calf tenderness) |
| Swelling | Localised vein distension | Diffuse limb swelling |
| Warmth | Localised | Diffuse |
| Homan's sign | Negative | Positive (calf pain on dorsiflexion) |
| Skin | Eczema, pigmentation | Erythema (in acute) |
| D-dimer | Normal | Elevated |
| Duplex US | Superficial incompetence | Deep vein thrombus |
Reason to rule out: DVT requires anticoagulation; surgical treatment of varicose veins is contraindicated in active DVT.
13.2 Superficial Thrombophlebitis
- A complication of varicose veins rather than a differential
- Presents as painful, tender, cord-like, erythematous superficial vein
- Management: NSAIDs, compression, warm soaks
- Rule out by: tenderness along exact vein cord, no deep swelling, duplex confirms superficial thrombus only
13.3 Lymphoedema
| Feature | Varicose Veins (venous oedema) | Lymphoedema |
|---|---|---|
| Onset | Gradual | Gradual |
| Nature | Pitting oedema initially | Non-pitting in chronic stage |
| Site | Ankles, lower leg | Foot + entire leg ("buffalo hump" dorsum of foot) |
| Skin | Eczema, pigmentation, ulcer | Thickened, hyperkeratotic (elephantiasis) |
| Varicosities | Present | Absent |
| Stemmer's sign | Negative | Positive (cannot pinch dorsal foot skin) |
| Investigation | Duplex US | Lymphoscintigraphy |
Reason to rule out: Lymphoedema does not benefit from vein surgery; treatment is compression, manual lymphatic drainage.
13.4 Klippel-Trénaunay Syndrome (KTS)
- Congenital condition: triad of port-wine stain + limb hypertrophy + varicose veins
- Varicosities are congenital and often involve unusual distributions (lateral aspect)
- Deep veins may be absent or hypoplastic
- Critical: Surgery/stripping CONTRAINDICATED if deep veins are absent (Perthe's test will be abnormal)
- Diagnosed by MRI venography showing deep venous abnormality
Reason to rule out: Removing superficial veins when deep veins are absent = catastrophic venous obstruction.
13.5 Arteriovenous (AV) Fistula
- Can cause secondary varicose veins with pulsatile flow
- Affected limb may be longer and warmer (due to increased blood flow stimulating bone growth)
- Bruit/thrill over the fistula
- Branham's sign: bradycardia on compression of feeding artery
- Reason to rule out: AV fistula requires separate treatment; vein surgery alone will not correct the cause and varices will recur.
13.6 Arterial Ulcer (vs. Venous Ulcer)
| Feature | Venous Ulcer | Arterial Ulcer |
|---|---|---|
| Site | Medial malleolus (gaiter) | Pressure points — heel, toes, lateral malleolus |
| Pain | Mild | Severe; worse at night; relieved by dependency |
| Edges | Sloping | Punched-out |
| Base | Granulation | Pale, necrotic, deep |
| Pulses | Present | Absent/reduced |
| ABPI | >0.8 | <0.8 |
| Skin | Eczema, pigmentation | Pale, shiny, hairless, cold |
| Varicosities | Present | Absent |
Reason to rule out: Compression therapy contraindicated in arterial ulcers (ABPI <0.8); worsens ischaemia.
13.7 Marjolin's Ulcer
- Squamous cell carcinoma arising in chronic venous ulcer
- Suspect when: raised, everted edges; rapid growth; failure to heal; bleeding; foul odour
- Reason to rule out: Requires excision with wide margins ± radiotherapy, not just wound care
13.8 Phlebitis Migrans (Migratory Thrombophlebitis)
- Recurrent thrombophlebitis at different sites
- Associated with Buerger's disease, malignancy (Trousseau's syndrome)
- Differentiates from varicose veins by: migratory nature, absence of varicosities, systemic associations
- Reason to rule out: Points to underlying systemic/malignant condition
Summary: Always rule out DVT (CONTRAINDICATION to surgery), KTS (deep vein absence), AV fistula (secondary cause), and arterial disease (ABPI before compression). Distinguish venous from arterial ulcers using ABPI and clinical features.
14. CASE PRESENTATION — MBBS PRACTICAL EXAMINATION
Model Case
"I am presenting a case of Mr. X, a 45-year-old male, a bus driver by occupation, presenting with dilated, tortuous veins over the medial aspect of the right leg for 10 years, associated with aching pain and heaviness of the right leg, worse after prolonged standing and relieved by limb elevation."
History
Chief Complaint: Dilated, prominent veins over right lower limb for 10 years
History of Present Illness:
- Onset: Gradual, insidious
- Site: Medial aspect of right leg, extending from ankle to upper thigh
- Duration: 10 years
- Progression: Initially small, now markedly prominent
- Associated symptoms:
- Aching pain and heaviness — worse after standing, relieved by elevation
- Ankle swelling in the evening
- Itching over the inner ankle (venous eczema)
- Occasional cramps at night
- No sudden severe pain (rules out acute thrombophlebitis)
- No history of DVT, previous leg swelling with fever
Past History: No previous leg surgery, no DVT, no malignancy
Personal/Occupational History: Bus driver — prolonged standing/sitting
Family History: Father had varicose veins
Obstetric history (in females): Multiparity, hormonal contraceptives
Physical Examination
General Examination:
- Conscious, oriented, afebrile
- BMI: 29 kg/m² (overweight)
- No pallor, icterus, lymphadenopathy
Systemic Examination: Lower Limb (right)
Inspection (patient standing):
- Dilated, tortuous, prominent veins along the medial aspect of right leg in GSV distribution
- Hyperpigmentation around medial malleolus
- No active ulcer (C4a CEAP)
- No lipodermatosclerosis visible
Palpation:
- Veins are soft and compressible
- No tenderness
- Fascial defect palpable 8 cm above medial malleolus (Cockett's perforator)
- No saphena varix felt
Special Tests:
-
Schwartz (Tap) Test: Positive — fluid impulse transmitted from ankle to thigh = confirms continuous varicose veins
-
Trendelenburg Test:
- Leg elevated → veins empty
- Tourniquet applied at upper thigh → patient stands
- Result: Veins remain empty with tourniquet → fill rapidly when tourniquet released
- Conclusion: SFJ incompetence (positive Trendelenburg)
-
Multiple Tourniquet Test:
- Tourniquet at upper thigh (empty) + below knee (veins fill in between)
- Conclusion: Perforator incompetence at mid-thigh level
-
Perthe's Test:
- Tourniquet applied → patient walks for 5 minutes
- Result: Veins become less prominent
- Conclusion: Deep veins are patent — safe to operate
-
Fegan's Test:
- Fascial gap palpable 8 and 14 cm above medial malleolus
- Conclusion: Cockett's perforator incompetence
Investigations (as requested):
- Duplex Doppler: SFJ incompetence + reflux in GSV; deep veins patent; Cockett's perforator incompetence
- ABPI: 1.0 (normal — no arterial disease)
Diagnosis
Working Diagnosis:
Primary varicose veins of the right lower limb in the GSV distribution with SFJ and Cockett's perforator incompetence — CEAP C4a, Ep, As+Ap, Pr
Treatment Plan
-
Pre-operatively:
- Compression stockings (class II)
- Vein marking while standing (by surgeon, day before surgery)
- Duplex mapping confirmed
- Routine pre-op workup (CBC, coagulation, ECG, CXR, blood glucose, renal function)
- ABPI confirmed >0.8
- Perthe's test confirmed positive (deep veins patent)
-
Surgery:
- Trendelenburg operation (flush SFJ ligation) via groin crease incision
- Babcock's stripping of GSV from groin to just below knee
- Multiple stab avulsion (phlebectomy) for tributary varices
- Subfascial ligation of Cockett's perforators (or SEPS)
- Under spinal/GA
-
Post-operative:
- Compression bandaging for 1 week
- Early ambulation from day 1
- Graduated compression stockings for 6 weeks
- Review at 6 weeks for residual varices
15. COMPLICATIONS OF SURGERY
| Complication | Notes |
|---|---|
| Haematoma | Most common; usually resolves |
| Wound infection | Groin incision at highest risk |
| Saphenous nerve injury | Medial lower leg dysaesthesia (avoid stripping below knee) |
| Sural nerve injury | SSV surgery |
| Recurrence | Due to: neovascularisation at SFJ, missed perforators, new sites |
| DVT/PE | Early ambulation reduces risk |
| Lymphoedema | Damage to inguinal lymphatics in groin dissection |
| Femoral vein injury | Catastrophic — flush ligation must be carefully performed |
Summary: Saphenous nerve injury (avoid stripping below knee) and femoral vein injury (proper flush ligation) are the most important surgical complications.
16. SPECIAL TOPICS (High-Yield Short Notes)
Saphena Varix
- Dilatation of terminal GSV at saphenous opening (SFJ)
- Mimics femoral hernia — bluish, soft, cough impulse positive
- Differentiating features:
- Disappears on lying down (hernia may not reduce)
- Fluid thrill transmitted to leg veins
- No bowel sounds
- Below and lateral to pubic tubercle (femoral hernia is medial to femoral artery)
Venous Gangrene
- Occurs when deep veins are thrombosed AND superficial veins are removed
- Catastrophic complication — Perthe's test prevents this
Phleboliths
- Calcified thrombi within varicose veins
- Seen on plain X-ray as circular calcific densities
- No treatment needed unless symptomatic
Ankle Flare / Corona Phlebectatica
- Fan-shaped cluster of intradermal varices at the ankle
- Indicates severe chronic venous insufficiency
- CEAP C4 marker
Recurrent Varicose Veins (REVAS — REcurrent Varicose veins After Surgery)
- Causes:
- Neovascularisation at SFJ (new vessels grow across ligation)
- Inadequate initial surgery (missed tributaries, incomplete stripping)
- New disease (different site)
- Technical error (ligation not flush)
- Management: UGFS (foam sclerotherapy) is first choice for recurrence; redo surgery if needed
17. QUICK REVISION TABLE — EXAMINATION SUMMARY
| Topic | Key Fact |
|---|---|
| Most common site of valve incompetence | Saphenofemoral junction (SFJ) |
| Gold standard investigation | Duplex ultrasonography |
| Most important pre-op test | Perthe's test (deep vein patency) |
| Contraindication to compression | ABPI <0.8 |
| Most important surgical step | Flush SFJ ligation (Trendelenburg op) |
| Nerve at risk during stripping | Saphenous nerve (strip only to below knee) |
| NICE first-line treatment for truncal veins | EVLA/RFA |
| Most common complication of surgery | Haematoma |
| Venous ulcer site | Medial malleolus (gaiter area) |
| Distinguishing venous vs arterial ulcer | ABPI (>0.8 venous; <0.8 arterial) |
| KTS contraindication | Never strip if deep veins absent |
| Sclerosant used | Sodium tetradecyl sulphate / Polidocanol |
| Perthe's test — veins increase on walking | Deep vein obstruction — do NOT operate |
| Saphena varix mimics | Femoral hernia |
| CEAP C6 | Active venous ulcer |
| Babcock stripper — safe level | Groin to just below knee (not ankle — nerve risk) |
| Four-layer compression | Standard treatment for venous ulcer |
18. EXAMINATION-STYLE SHORT ANSWERS
Q: What is the Trendelenburg test and what does it demonstrate?
A: The Brodie-Trendelenburg test identifies SFJ incompetence. The patient lies supine, leg elevated to empty veins, tourniquet applied at upper thigh. On standing, if veins remain empty until tourniquet release then fill rapidly = SFJ incompetence. If veins fill from below despite tourniquet = perforator incompetence.
Q: Why is Perthe's test important before surgery?
A: It confirms patency of deep veins. If deep veins are obstructed, superficial varicose veins act as collaterals. Removing them causes venous hypertension → venous gangrene.
Q: What is the complication of stripping GSV below the knee?
A: Saphenous nerve injury, causing paraesthesia/numbness over the medial aspect of the lower leg and foot.
Q: What is neovascularisation in context of varicose veins?
A: Growth of new vessels across the ligated SFJ stump, causing recurrence. Prevented by flush ligation and some advocate excision of the SFJ rather than simple ligation.
Q: How do you differentiate a saphena varix from a femoral hernia?
A: Both have cough impulse. Saphena varix: disappears completely on lying, fluid thrill to leg veins, no bowel sounds, below and lateral to pubic tubercle. Femoral hernia: may not fully reduce, bowel sounds possible, medial to femoral vessels.
This comprehensive guide covers all MBBS examination requirements for varicose veins — anatomy, pathophysiology, CEAP classification, clinical examination with all special tests, investigations, complete management including surgery, complications, differentials with reasoning, case presentation, and surgical anatomy critical points.
This is a shared conversation. Sign in to Orris to start your own chat.