Tear film breakup test principle to detect dry eye
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have all the information needed for a comprehensive answer. Here is a structured explanation of the Tear Film Break-Up Time (BUT) test:
Tear Film Break-Up Time (BUT) Test
Principle
The tear film is a three-layered structure (lipid, aqueous, mucin) that must remain stable between blinks to protect and lubricate the ocular surface. In dry eye, this film becomes unstable — it thins and ruptures prematurely before the next blink, exposing the corneal epithelium. The BUT test quantifies this instability.
Fluorescein dye is used because it distributes uniformly throughout the aqueous layer of the tear film, making it visible under blue light. When the film ruptures, the dye-free dry spots appear as dark areas or lines against the bright green fluorescent background, signalling loss of tear film continuity.
Procedure (Step-by-Step)
- Instill fluorescein — 2% fluorescein solution or a fluorescein-impregnated strip moistened with non-preserved saline is placed into the lower fornix.
- Ask the patient to blink several times to distribute the dye evenly across the cornea.
- Examine under the slit lamp — use a broad beam with the cobalt blue filter to illuminate the fluorescein-stained tear film.
- Start timing — after the last blink, count the seconds until the first black spot or line (dry spot) appears in the fluorescein film.
- Repeat the measurement 3 times and take the average.
Interpretation
| BUT Value | Interpretation |
|---|---|
| > 10 seconds | Normal tear film stability |
| ≤ 10 seconds | Abnormal — tear film instability / dry eye |
"Decreased tear break-up time (measured from a blink to the appearance of a tear film defect, by using fluorescein stain): Less than 10 seconds indicates tear film instability." — The Wills Eye Manual, p. 171
What the Test Detects
The BUT is abnormal in two major categories of dry eye:
- Aqueous tear deficiency — reduced aqueous layer volume means the film cannot sustain itself between blinks
- Meibomian gland dysfunction (evaporative dry eye) — a deficient or abnormal lipid layer causes rapid evaporation and film rupture
In the normal eye, as the tear film breaks down, lipid-contaminated mucin is washed away by the next blink. In dry eye, this lipid-contaminated mucin accumulates as debris and particles, further destabilising the film.
— Kanski's Clinical Ophthalmology, p. 176
Slit-Lamp Appearance
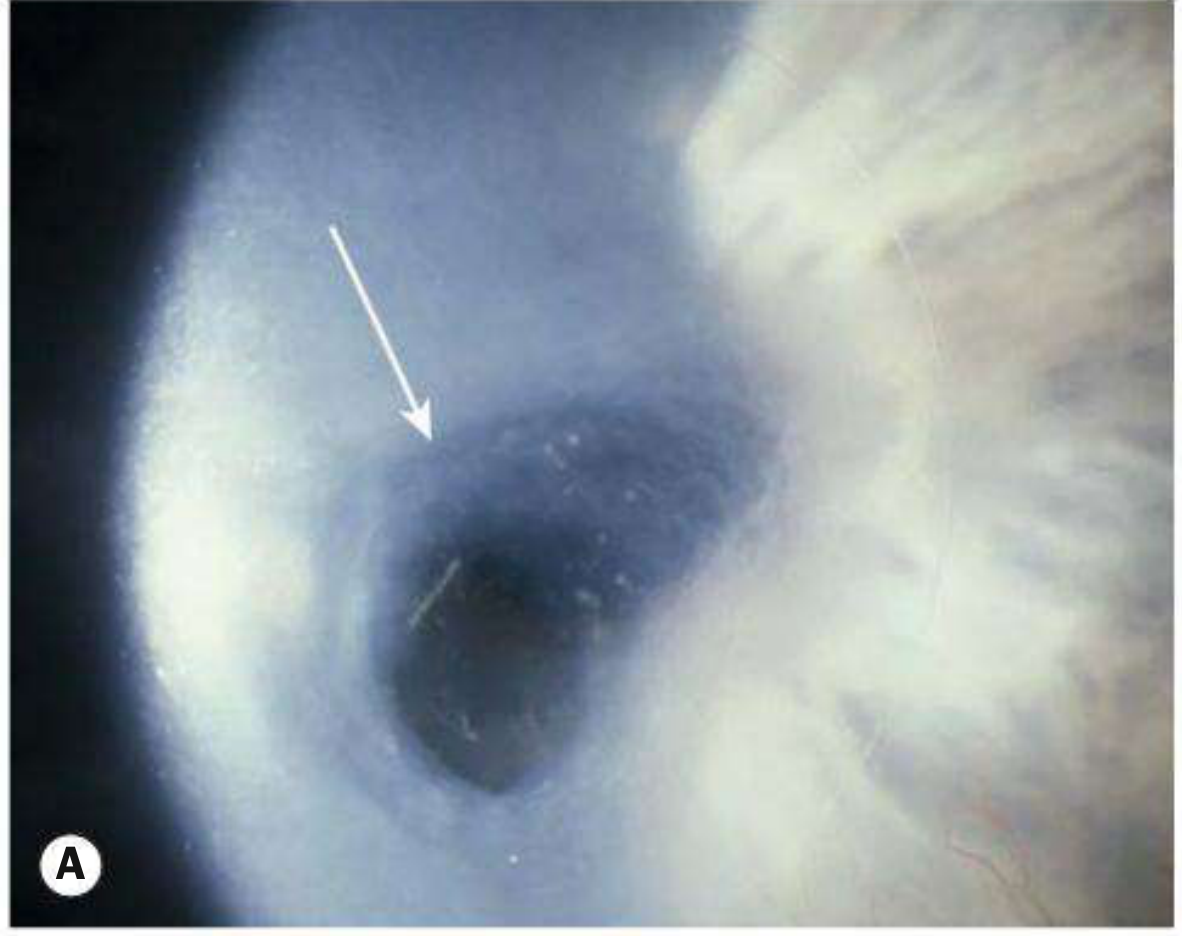
Important Clinical Notes
- Consistently early breakup at the same location may point to a focal corneal surface abnormality (e.g., epithelial basement membrane disease) rather than true tear film instability — not a positive BUT for dry eye.
- Tear defects must be randomly located for the test to be diagnostic of dry eye.
- BUT has poor correlation with symptoms, but its reliability improves with disease severity.
- BUT alone should not be used as the sole criterion; it is part of a panel that also includes the Schirmer test (aqueous production) and vital dye staining (ocular surface damage with fluorescein, rose Bengal, or lissamine green).
Context Within the Dry Eye Investigation Panel
| Test | Parameter Measured |
|---|---|
| BUT | Tear film stability |
| Schirmer test (5 min) | Aqueous tear production (< 10 mm without anaesthesia = abnormal) |
| Fluorescein / rose Bengal / lissamine green staining | Ocular surface disease severity |
| Tear osmolarity | Correlates with treatment response |
The tests are performed in this order because the Schirmer strip paper can damage the ocular surface and cause staining artefacts if done first. — Kanski's Clinical Ophthalmology, p. 177
This is a shared conversation. Sign in to Orris to start your own chat.