Facial paralysis diagnosis and treatment
Reading File
Finding Sources
Finding Sources
Searching Images
facial paralysis Bell's palsy diagnosis treatment
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive overview of facial paralysis — covering etiology, diagnosis, and treatment.
Facial Paralysis: Diagnosis and Treatment
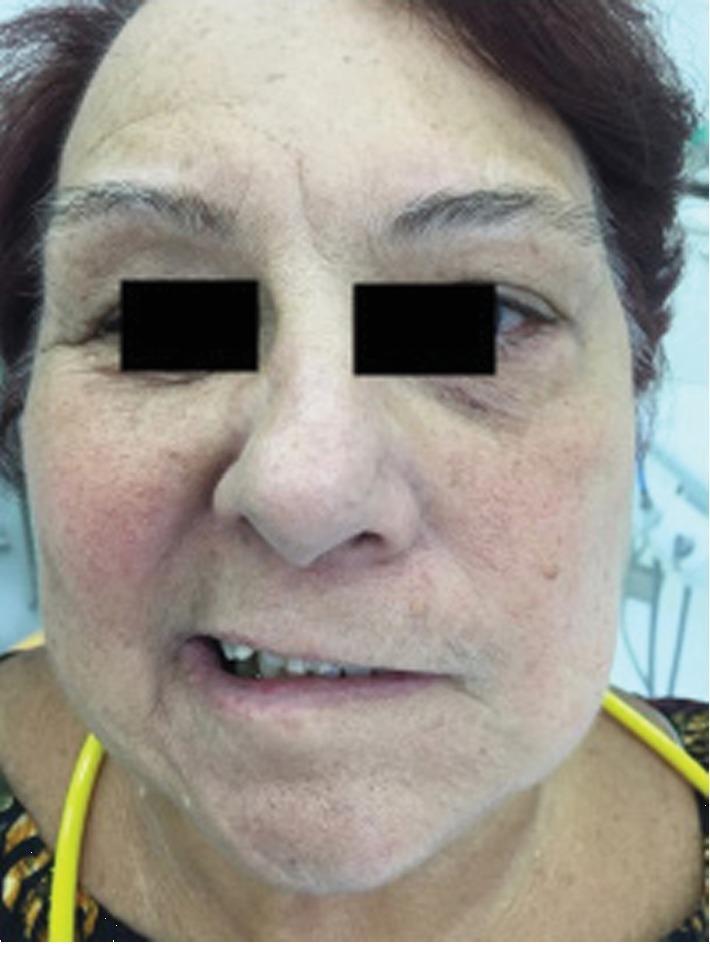
Overview
Facial paralysis results from dysfunction of the facial nerve (CN VII). The most important diagnostic principle is captured in the classic dictum: "All that palsies are not Bell." Multiple etiologies exist, each requiring a different management approach.
Etiology & Differential Diagnosis
| Category | Examples |
|---|---|
| Idiopathic | Bell palsy (most common) |
| Viral | Ramsay Hunt syndrome (VZV), HIV, Epstein-Barr |
| Bacterial/Infectious | Lyme disease, otitis media, mastoiditis, tuberculosis |
| Neoplastic | Facial nerve neuroma, parotid malignancy, metastatic disease, acoustic neuroma |
| Trauma | Temporal bone fracture, surgical injury |
| Metabolic | Diabetes, pregnancy |
| Autoimmune | Sarcoidosis (Heerfordt syndrome), Guillain-Barré, Sjögren |
| Central (UMN) | Stroke, tumor — forehead sparing is a key distinguishing feature |
Bilateral facial paralysis strongly suggests metabolic, autoimmune, or infectious disease (especially Lyme disease) and should not be attributed to Bell palsy without extensive workup.
Bell Palsy (Idiopathic Facial Paralysis)
Definition & Minimum Diagnostic Criteria (Taverner)
Bell palsy is reserved for cases meeting all four criteria:
- Paralysis or paresis of all muscle groups on one side
- Sudden onset
- Absence of CNS disease signs
- Absence of ear or cerebellopontine angle disease signs
Progressive facial paralysis is NOT Bell palsy — it mandates imaging to exclude neoplasm.
Epidemiology
- Incidence: 23–37 per 100,000/year; up to 59/100,000 in those >65 years
- Equal sex distribution; slight female predominance under age 20
- ~70% present with complete paralysis; ~30% incomplete
- Bilateral in 0.3%; recurrence in ~9%; family history in 8%
Etiology
The dominant theory is reactivation of herpes simplex virus type 1 (HSV-1) latent in the geniculate ganglion. PCR studies detected HSV-1 DNA in endoneurial fluid in 11/14 surgical cases. The long bony fallopian canal, with its narrow meatal foramen (~0.68 mm), creates a compartment where viral-induced edema causes compression and axoplasmic flow obstruction. — Cummings Otolaryngology Head and Neck Surgery; Adams and Victor's Principles of Neurology, 12th Ed.
Clinical Features
- Onset: Acute — 50% reach maximum paralysis in 48 hours; nearly all within 3–4 days
- Pain: Retroauricular pain may precede paralysis by 1–2 days
- Taste impairment: Present in most patients (lesion proximal to chorda tympani junction); resolves within ~2 weeks
- Hyperacusis: Indicates stapedius muscle paralysis
- Lagophthalmos: Inability to close the eye — risk of corneal exposure injury
- Facial numbness/fullness reported in a small number of patients
- Bell's phenomenon: Upward rotation of the eyeball on attempted eyelid closure (lower motor neuron sign)
Grading: House-Brackmann Scale
| Grade | Description |
|---|---|
| I | Normal |
| II | Mild dysfunction — slight weakness on close inspection |
| III | Moderate dysfunction — obvious but not disfiguring |
| IV | Moderately severe — disfiguring, incomplete eye closure |
| V | Severe — barely perceptible motion |
| VI | Total paralysis |
Diagnostic Evaluation
Clinical Assessment
- Distinguish upper motor neuron (UMN) vs. lower motor neuron (LMN) lesion:
- UMN: forehead sparing (bilateral cortical representation of frontalis)
- LMN: entire ipsilateral face involved, including forehead
Electrodiagnostic Testing
- Electroneurography (ENoG): Compares compound action potential amplitude bilaterally. >90% degeneration indicates poor prognosis; used 4–14 days post-onset
- Electromyography (EMG): Denervation potentials appear 10+ days post-onset. Retention of voluntary motor units beyond day 7 is a favorable sign; fibrillation potentials at 10–14 days predict poor outcome with ~80% accuracy
- Nerve conduction velocity: 37–58 m/s = good outcome; <10 m/s = poor prognosis
Imaging
- MRI with gadolinium: Enhancement of the facial nerve is common even in healthy individuals, limiting specificity. More pronounced enhancement correlates with worse prognosis
- Indicated when: progressive course, associated masses, suspected neoplasm, or atypical features
- CT temporal bone: Trauma or cholesteatoma evaluation
Additional Testing (when indicated)
- Lyme serology (endemic areas or bilateral palsy)
- ACE level (sarcoidosis)
- HIV testing
- VZV serology
Prognosis
- 70% recover completely within 1–2 months; 85% achieve near-normal function
- Early return of some motor function in days 5–7 is the most favorable prognostic sign
- Return of taste in the first week is also a good sign
- When degeneration is complete, recovery proceeds by axonal regeneration — may take 2 years or longer and is often incomplete
- Incomplete paralysis at presentation → near-universal complete recovery
Treatment
1. Corticosteroids (First-Line)
The mainstay of Bell palsy treatment. Start as early as possible (ideally within 72 hours of onset).
- Typical regimen: Prednisolone 60 mg/day × 5 days, then taper over 5 days
- Improves the probability and speed of complete recovery
2. Antiviral Agents
- Evidence is conflicting — studies differ on benefit of adding antivirals to steroids
- Acyclovir or valacyclovir is often added given the HSV-1 etiology (low risk, potential benefit)
- In Ramsay Hunt syndrome: antiviral treatment (acyclovir/valacyclovir) combined with steroids is clearly beneficial; recovery rates are significantly better with combination therapy vs. steroids alone (~16–22% full recovery with RHS vs. ~70% with Bell palsy)
3. Eye Care
- Critical to prevent corneal exposure injury due to lagophthalmos
- Artificial tears (daytime), lubricating eye ointment (nighttime), eye patching
- Moisture chamber glasses if severe lagophthalmos
4. Surgical Decompression
- Reserved for cases with >90% ENoG degeneration and absent voluntary EMG potentials
- Controversial — the evidence base is limited
- Target: decompression at the meatal foramen (labyrinthine segment)
5. Botulinum Toxin
- For persistent synkinesis post-recovery
- Orbicularis oculi injection (~40 units) effectively reduces eyelid synkinesis; lower doses preferred to avoid ptosis — Cummings Otolaryngology
6. Physical Therapy / Facial Rehabilitation
- Includes neuromuscular reeducation, mime therapy, biofeedback
- Evidence: one meta-analysis found no benefit; another found Level C support for mime therapy
- Most useful for patients with incomplete recovery
7. Facial Reanimation Surgery (Permanent Palsy)
- Static procedures: Facial slings (xenograft/muscle transfers) — restore symmetry at rest
- Dynamic procedures: Nerve grafts (hypoglossal-facial nerve anastomosis, cross-facial nerve grafts), free muscle transfer
Ramsay Hunt Syndrome (Herpes Zoster Oticus)
- Etiology: VZV reactivation in geniculate ganglion
- Triad: Facial paralysis + otalgia + vesicular eruption on pinna/external auditory canal/palate/tongue
- ~10% of cases: rash appears after initial paralysis; ~25% rash precedes paralysis (better prognosis)
- Zoster sine herpete: VZV-mediated palsy without visible rash
- Prognosis worse than Bell palsy: full recovery in only 16–22% overall; 10% after complete palsy
- Treatment: Prednisone + valacyclovir (or acyclovir) — combination is superior to steroids alone
Special Situations
| Situation | Management |
|---|---|
| Chronic otitis media / cholesteatoma | Treat the ear disease first; facial nerve recovery usually follows |
| Pregnancy | Manage as standard Bell palsy in collaboration with obstetrician |
| Lyme disease | Oral doxycycline; spontaneous recovery is common even without treatment |
| Malignant otitis externa | Aggressive IV antipseudomonal antibiotics ± surgery |
| Neonatal/birth trauma | Observation — most recover spontaneously |
Sources: Cummings Otolaryngology Head and Neck Surgery; Adams and Victor's Principles of Neurology, 12th Ed.; Bradley and Daroff's Neurology in Clinical Practice; K.J. Lee's Essential Otolaryngology
This is a shared conversation. Sign in to Orris to start your own chat.