A fistula or abscess formation near the anus in between scrotum and anus
Reading File
Finding Sources
Finding Sources
Searching Images
perianal fistula abscess scrotum anus anatomy
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
The description — a fistula or abscess between the scrotum and anus — points to a perineal/perianal fistula, most classically described as fistula-in-ano or in severe/Crohn's cases as "watering-can perineum." The location between the scrotum and anus is the perineum in males, and the condition is well-characterized. Here is a comprehensive overview:
Perianal Fistula / Abscess (Fistula-in-Ano)
What It Is
A fistula-in-ano is an abnormal tract connecting the anal canal (usually at the level of the cryptoglandular tissue) to an external opening on the perianal skin. When the external opening lies anteriorly — between the scrotum and anus in males — this represents an anterior perianal or perineal fistula.
An abscess in this region forms when the fistula tract does not drain freely, causing local pus accumulation.
Anatomy & Classification (Parks Classification)
| Type | Relation to sphincter | Notes |
|---|---|---|
| Intersphincteric | Between internal and external sphincter | Most common (~70%) |
| Transsphincteric | Crosses external sphincter | ~25% |
| Suprasphincteric | Over puborectalis | Rare |
| Extrasphincteric | Outside sphincter entirely | Rare, often iatrogenic |
Anterior fistulas that open between the scrotum and anus are often intersphincteric or transsphincteric in type.
Etiology
Common causes:
- Cryptoglandular infection — most frequent cause; an anal gland becomes infected → abscess → fistula track forms
- Crohn's disease — a major cause of complex perianal fistulas extending to the scrotum or labia ("watering-can perineum")
- Trauma, tuberculosis, malignancy, radiation, hidradenitis suppurativa
"Perianal disease is a potentially disabling complication of Crohn disease. The fistulous openings are most commonly found in the perianal skin but can occur in the groin, vulva, or scrotum." — Goldman-Cecil Medicine
Clinical Features
- Fistula: Intermittent or continuous discharge of serous or purulent material from an external opening near the anus, with an opening also sometimes palpable inside the anal canal
- Abscess: Redness, swelling, pain, and induration in the perineum; fluctuance on palpation; pain worsened by sitting, walking, or defecation
- Crohn's perianal disease: Multiple external openings, skin discoloration, hardened scarring over scrotum and perianal skin
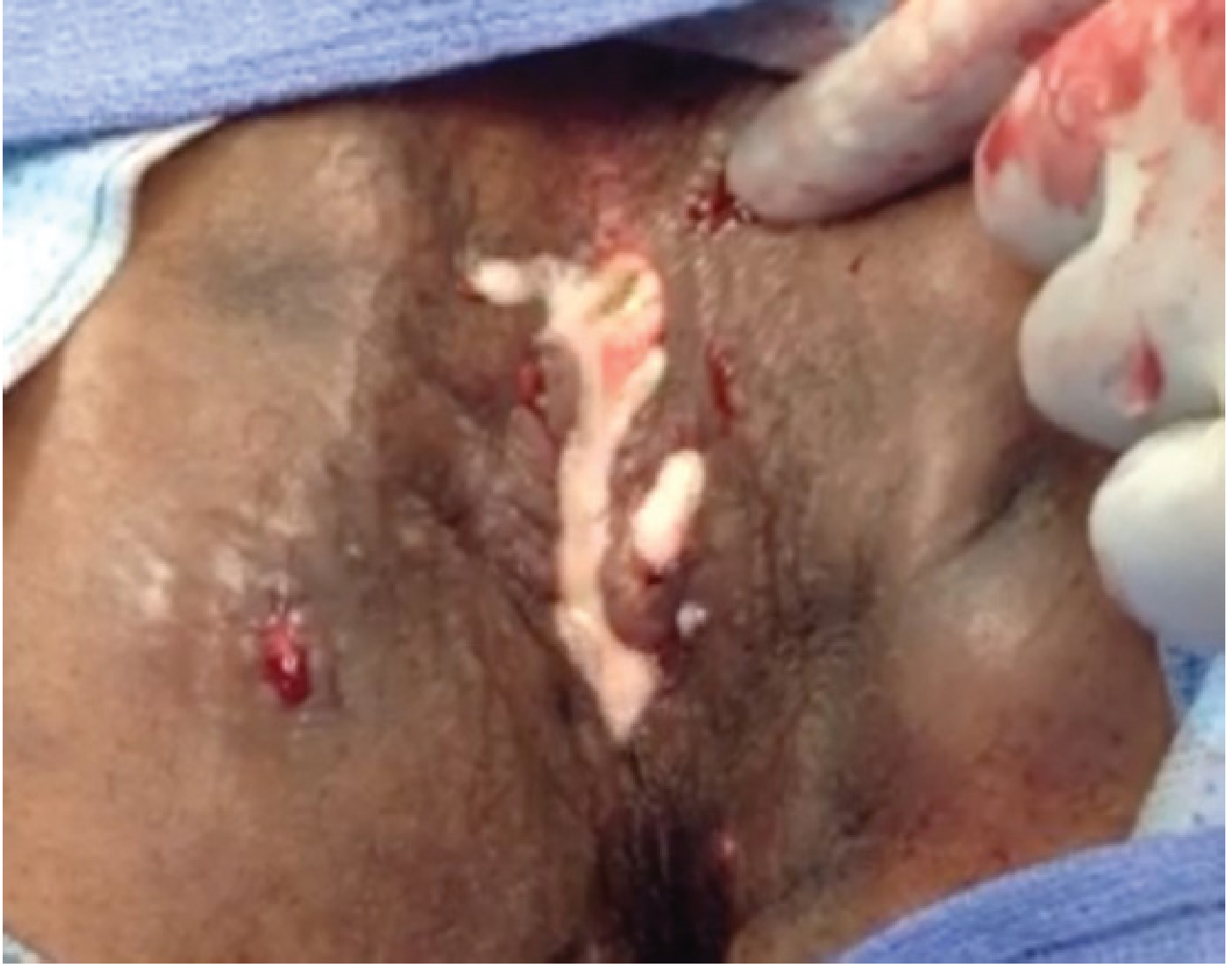
"Watering-can perineum" in Crohn's disease — hydrogen peroxide injected through one external opening produces bubbles from multiple other openings — Mulholland & Greenfield's Surgery
Evaluation
- Examination under anesthesia (EUA) — gold standard; defines internal opening, tract anatomy, and sphincter involvement
- MRI pelvis — best modality for mapping complex fistula tracts, especially in Crohn's
- CT scan — useful for associated abscess and extent of perianal sepsis
- Endoanal ultrasound — evaluates sphincter integrity
Management
Abscess
- Incision and drainage (I&D) is the immediate treatment — the incision should be placed as close to the anal verge as possible to minimize fistula tract length if one develops
- Alternatively, a small mushroom-tipped catheter can be placed in the cavity to allow continued drainage while the cavity closes
Fistula
| Scenario | Treatment |
|---|---|
| Low-lying fistula, no proctitis | Fistulotomy (laying open the tract) — definitive and effective |
| High/complex fistula | Seton placement first (drainage + prevents abscess recurrence + fibroses the tract) |
| Crohn's complex fistula | Anti-TNF agents (infliximab, adalimumab) — closure in up to 60%; also azathioprine/6-MP |
| Sphincter-sparing options | Endorectal advancement flap, LIFT procedure (ligation of intersphincteric fistula tract) — ~50–60% success |
| Adjuncts | Fibrin glue (not recommended), fistula plugs (<20% success) |
"A low-lying fistula in the absence of overt proctitis can often be treated safely with fistulotomy. When the fistula is higher or more complex, the initiation of anti-TNF agents has been reported to heal fistulas in up to 60% of patients." — Mulholland & Greenfield's Surgery
Seton Drain
A seton (e.g., Penrose drain, silicone loop) is threaded through the fistula tract:
- Maintains continuous drainage
- Prevents abscess reaccumulation
- Converts the inflammatory tract to a fibrotic one
- Protects the sphincter until definitive repair
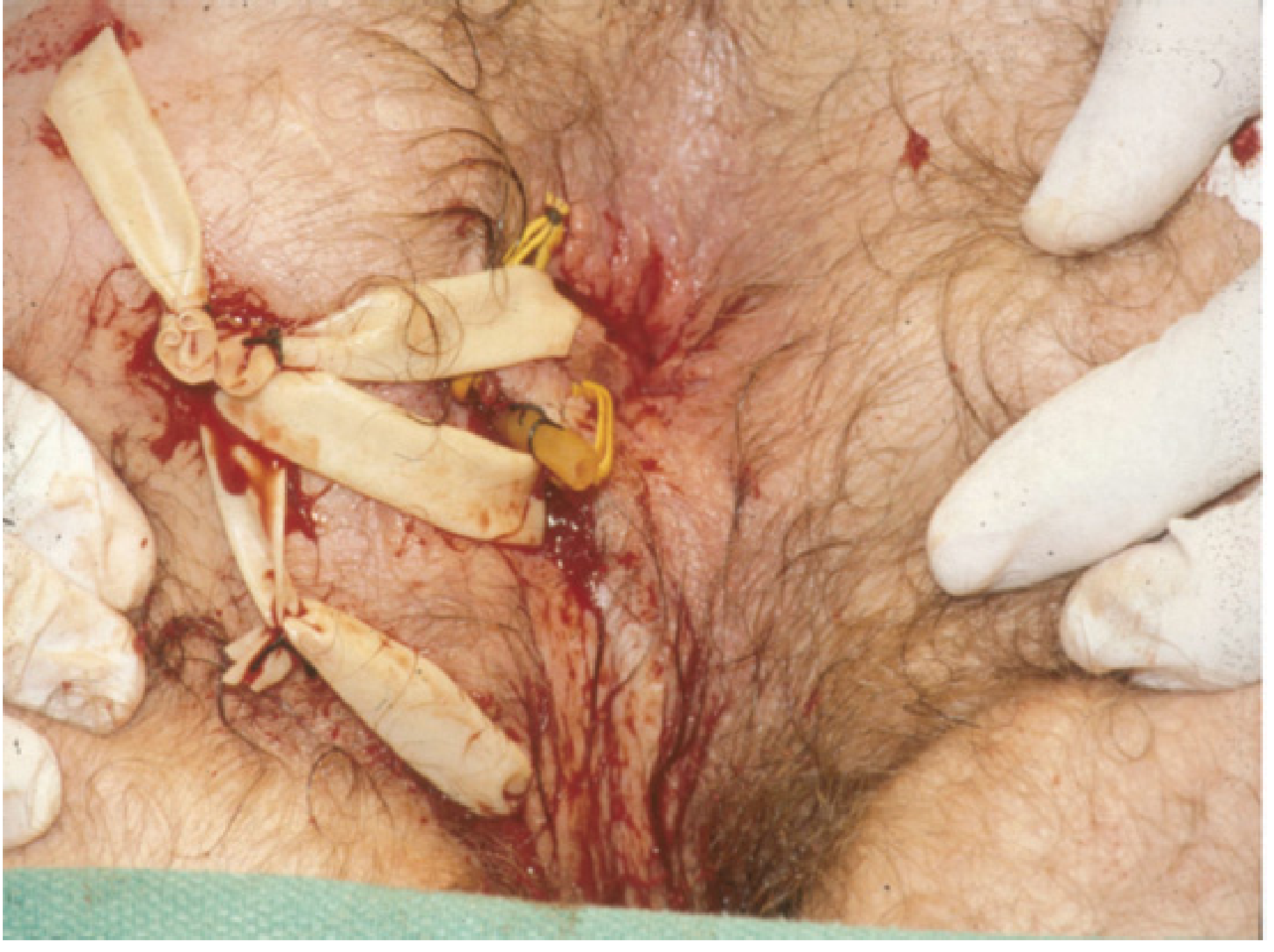
Seton (Penrose) drains placed through fistula tracts — Mulholland & Greenfield's Surgery
Special Concern: Perianal Crohn's Disease
The presence of a scrotal or perineal fistula should raise suspicion for Crohn's disease. In this setting:
- Avoid aggressive surgery (risk of non-healing wounds, sphincter damage)
- Medical therapy is central: infliximab, adalimumab, certolizumab, ustekinumab, vedolizumab, azathioprine, 6-MP
- Metronidazole + sitz baths for limited disease
- Allogeneic adipose-derived stem cells — experimental option for refractory cases
- Goal: relieve symptoms + preserve sphincter function
"Persistent severe perianal Crohn disease can result in destruction of the anal sphincter and subsequent fecal incontinence." — Goldman-Cecil Medicine
Summary: A fistula or abscess between the scrotum and anus is a perineal/perianal fistula (fistula-in-ano). It arises most often from cryptoglandular infection or Crohn's disease. Initial management is drainage (I&D for abscess, seton for fistula). Definitive treatment ranges from fistulotomy (simple, low fistulas) to sphincter-sparing procedures and biologic therapy (complex, high, or Crohn's-related fistulas).
This is a shared conversation. Sign in to Orris to start your own chat.