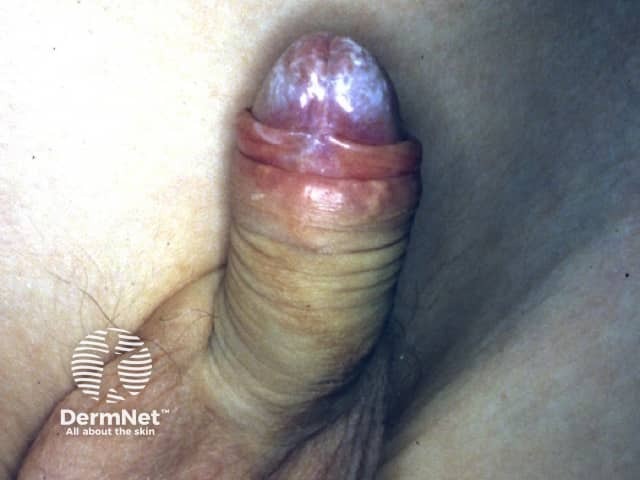
Whitish patch on glans penis in an 25 year old male
Reading File
search_medical_text
whitish patch glans penis differential diagnosis young male
search_medical_text
leukoplakia lichen sclerosus balanitis xerotica obliterans penis
search_medical_image
whitish patch glans penis lichen sclerosus leukoplakia
GradeResponse
GradeResponse
GradeResponse
Whitish Patch on Glans Penis — 25-Year-Old Male
Differential Diagnosis
| Condition | Key Features | Age Group | Malignant Potential |
|---|---|---|---|
| Candidal Balanitis | White curdy patches, itching, satellite lesions, often under foreskin | Any age | None |
| Lichen Sclerosus (BXO) | White sclerotic plaques, may scar, phimosis, meatal involvement | Any age (incl. young) | Low but present (~5%) |
| Penile Leukoplakia | White adherent patch, won't rub off | Middle-age/older | Moderate–High (precancerous) |
| Erythroplasia of Queyrat (CIS) | Usually red/velvety but can appear pale | Older males | High (carcinoma in situ) |
| HPV / Condyloma | Warts, warty white plaques | Young males | Low–moderate (HPV 16/18) |
| Psoriasis | White-silvery plaques, may be elsewhere on body | Any age | None |
| Vitiligo | Well-demarcated depigmented white area, no texture change | Any age | None |
| Bowen's Disease | Intraepithelial carcinoma, may be white or red | Older typically | High |
Most Likely in a 25-Year-Old
1. Candidal Balanitis (Most common cause overall)
- Presents as white curdy/creamy patches or plaques
- Risk factors: poor hygiene, uncircumcised, diabetes, antibiotics, immunosuppression
- Diagnosis: KOH smear, swab culture
- Treatment: topical clotrimazole/miconazole 1–2% for 1–2 weeks; systemic fluconazole 150 mg single dose if recurrent
2. Lichen Sclerosus / Balanitis Xerotica Obliterans (BXO)
- Chronic non-painful inflammatory condition affecting glans, foreskin, meatus, and urethra
- Presents as white sclerotic plaques that can cause scarring, phimosis, and urethral outflow obstruction (Bailey & Love's, p. 1471; Paediatric Urology, p. 11)
- Histology: epidermal thinning, hyalinization of upper dermis, lymphocytic infiltrate
- Treatment: ultra-potent topical steroids (clobetasol 0.05%), circumcision often required; dilatation for meatal stenosis
3. HPV-related Lesions
- Human papillomavirus is common in sexually active young males
- Can cause flat white plaques (bowenoid papulosis) or exophytic condylomata
- High-risk HPV (16, 18) carries oncogenic potential
- Treatment: imiquimod, podophyllotoxin, ablative therapy
4. Penile Leukoplakia / Early Carcinoma In Situ
- Less common at 25 but must not be missed
- White patch that cannot be wiped off
- Requires biopsy to exclude dysplasia/malignancy
Diagnostic Approach
1. Full history — sexual history, STIs, diabetes, hygiene, circumcision status
2. Physical exam — morphology (plaque/patch/wart), texture, distribution, foreskin
3. KOH prep / swab — rule out candida
4. VDRL/TPHA — rule out syphilitic patch
5. Biopsy — MANDATORY if:
- Lesion persists >2–4 weeks after empirical treatment
- Irregular borders, induration, or ulceration
- Non-healing or recurrent lesion
Key Management Principles
- Empirical antifungal is a reasonable first step in uncircumcised males with classic candidal features
- Do NOT delay biopsy for persistent, treatment-resistant, or suspicious lesions — even in young patients, premalignant conditions occur
- Refer to urology or dermatology for lesions that do not resolve with initial treatment
- Circumcision is both diagnostic and therapeutic in BXO
Bottom line: In a 25-year-old, candidal balanitis and BXO (lichen sclerosus) are the top considerations. Any persistent, treatment-unresponsive, or atypical white patch on the glans mandates biopsy to exclude penile intraepithelial neoplasia or carcinoma in situ.
This is a shared conversation. Sign in to Orris to start your own chat.