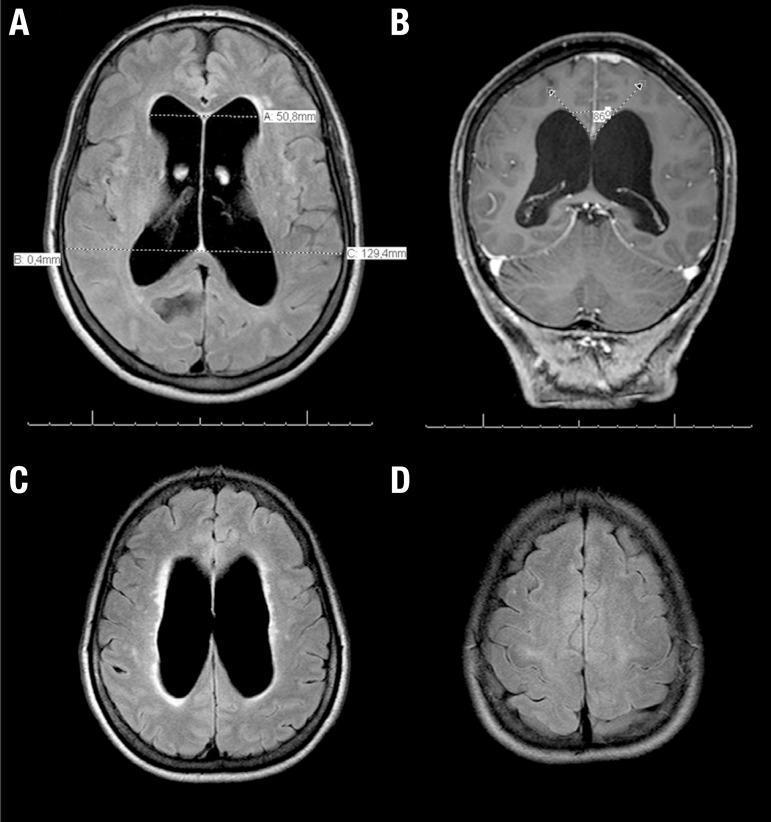
A 65-year-old woman is evaluated for worsening urinary urgency and incontinence. The patient has had no abdominal pain, dysuria, or changes in urinary frequency. On several occasions, she has urinated involuntarily, which she attributes to an inability to walk quickly to the bathroom. The patient feels unsteady while ambulating and walks slowly with small steps. Her family also reports that she has become forgetful and has difficulty planning and executing various activities that she used to perform regularly. Medical history is notable for hypertension. The patient does not use tobacco, alcohol, or illicit drugs. Vital signs are within normal limits. Cardiopulmonary, abdominal, and genitourinary examinations show no abnormalities. Neurological examination shows impaired attention and short-term memory. MRI of the brain reveals chronic white matter changes with no infarction, hemorrhage, or mass lesions. There is diffuse ventriculomegaly with no sulcal enlargement. Which of the following is the most likely underlying cause of this patient's urinary incontinence? his patient with impaired memory and cognition, unsteady gait, and urinary incontinence has ventriculomegaly without sulcal enlargement on MRI, which is characteristic of normal pressure hydrocephalus (NPH). NPH can occur due to decreased absorption of cerebrospinal fluid (CSF) by the arachnoid granulations (eg, fibrosis from previous cerebral inflammation or bleeding) with gradual accumulation of CSF in the ventricular system. The lateral ventricles expand, resulting in normal intracranial pressure and stretching the descending cortical fibers (corona radiata). Interruption of these pathways, along with impairment of cortical and subcortical function, leads to the classic triad of NPH symptoms (dementia, gait disturbance, urinary incontinence). The cerebral cortex (through the pontine micturition center) regulates the micturition reflex, which is an autonomic spinal reflex mediated by the neurons in the sacral spinal cord. In NPH, the lack of cortical inhibition results in detrusor muscle hyperactivity. This leads to urinary urgency, which can be worsened by gait abnormalities that limit a patient's ability to quickly get to a bathroom (urge incontinence). Progressive frontal lobe impairment leads to the inability to recognize urinary urge, uncontrolled urination, and a lack of concern as the disease progresses. (Choice A) Cerebellar dysfunction can cause an ataxic gait, dysarthria, and intention tremors. Memory dysfunction and urinary incontinence are more indicative of cerebral impairment. NPH typically spares cerebellar function. (Choice B) Compression of the reticular formation can occur with brainstem herniation, leading to loss of consciousness and coma. (Choice C) Impaired basal ganglia signaling is characteristic of Parkinson disease, which can result in ataxia with a slow gait. However, cogwheel rigidity and resting tremor would be prominent and dementia and urinary incontinence would not be expected until later in the disease course. (Choice D) Spinal cord damage is a common cause of incontinence with gait impairment. However, spinal cord injury also frequently causes lower extremity weakness and is not associated with cognitive impairment. Educational objective: Normal pressure hydrocephalus occurs due to decreased cerebrospinal fluid absorption, resulting in ventriculomegaly with normal intracranial pressure. This causes stretching of the descending cortical fibers (corona radiata) from the frontal lobe and contributes to the classic triad of symptoms (ie, dementia, gait abnormalities, urinary incontinence). Loss of cortical inhibition of the sacral micturition center leads to urge incontinence.
normal pressure hydrocephalus ventriculomegaly MRI corona radiata stretching
Normal Pressure Hydrocephalus (NPH) — Mechanism of Urinary Incontinence
Diagnosis: Normal Pressure Hydrocephalus
| Feature | This Patient |
|---|---|
| Gait disturbance | Unsteady, slow, small steps ("magnetic gait" / apraxic gait) |
| Cognitive impairment | Impaired attention, memory, difficulty planning |
| Urinary incontinence | Urgency-type, unable to reach bathroom in time |
Pathophysiology of NPH
- Corticospinal fibers → gait apraxia (legs affected more than arms because leg fibers run closest to the ventricles)
- Frontopontine/frontosubcortical fibers → cognitive impairment (frontal-subcortical pattern: slowed processing, apathy, impaired executive function)
- Frontal lobe fibers projecting to the pontine micturition center → loss of cortical inhibition → detrusor overactivity
- The detrusor contracts involuntarily and prematurely → urgency
- Combined with the gait disorder (inability to walk quickly to the bathroom) → urge incontinence
- Late-stage: the patient becomes indifferent to incontinence — "frontal lobe incontinence" (no awareness or concern)
Why the Other Choices Are Wrong
| Choice | Condition | Why Incorrect |
|---|---|---|
| Cerebellar dysfunction | Ataxic gait, dysarthria, intention tremor | Does not cause memory dysfunction or urinary incontinence; NPH typically spares the cerebellum |
| Reticular formation compression | Brainstem herniation → coma | This patient is alert and ambulatory; no herniation syndrome |
| Basal ganglia impairment | Parkinson disease | Would show cogwheel rigidity and resting tremor; dementia and incontinence are late and less prominent features |
| Spinal cord damage | Myelopathy | Causes lower extremity weakness, hyperreflexia, Babinski signs; does NOT cause cognitive impairment |
Clinical Correlation: Temporal Sequence of NPH Symptoms
"A slowly progressive gait disorder is usually the earliest feature, followed by impairment of mental function... and, later, sphincter incontinence."
Treatment
hey biostatistics usmle step 1 based from foundation to mastering questions how many days tro complete totatl biostats with uworld questions
USMLE Step 1 Biostatistics: Complete Beginner → UWorld Mastery
How long total? 12–14 days
Recommended Resources (in order of use)
| Phase | Resource | Why |
|---|---|---|
| Foundation | Boards and Beyond (BnB) — Biostatistics module | Best video-based foundation; Dr. Ryan explains everything from scratch, ~4–5 hours total video |
| Reference | First Aid 2024 — Biostatistics chapter | The "bible" for Step 1; use it alongside every topic as your notes anchor |
| Practice | UWorld Biostatistics + Epidemiology block | ~120–140 questions; do after foundation is solid |
| Reinforcement | Amboss Biostats (optional, if time allows) | Harder questions, great explanations |
Day-by-Day Study Plan (3–4 hrs/day)
Phase 1 — Foundations (Days 1–6)
| Day | Topics | What to Do |
|---|---|---|
| 1 | Study design basics | Observational vs. experimental; cohort, case-control, cross-sectional, RCT, case reports. BnB video + First Aid. Make a comparison table. |
| 2 | Bias & confounding | Selection bias, recall bias, lead-time bias, length-time bias, confounding, effect modification. These are very high yield on Step 1. |
| 3 | Statistical tests | t-test, ANOVA, chi-square, Fisher exact — know which test for which data type. Parametric vs. non-parametric. |
| 4 | 2×2 table mastery | This is the single most important day. Sensitivity, specificity, PPV, NPV, LR+, LR−. Draw 50+ practice 2×2 tables by hand until it is automatic. |
| 5 | Disease frequency & risk | Incidence, prevalence, relative risk (RR), odds ratio (OR), attributable risk (AR), number needed to treat (NNT), number needed to harm (NNH). |
| 6 | Statistical concepts | P-value, type I error (α), type II error (β), power (1−β), confidence intervals, null hypothesis, precision vs. accuracy. |
Phase 2 — Consolidation (Days 7–8)
| Day | Activity |
|---|---|
| 7 | Full First Aid biostatistics chapter read-through. Annotate everything. Build a master formula sheet (1–2 pages max). |
| 8 | Do your first UWorld block (40 questions, timed). Review every single explanation — correct AND incorrect. Note which topics you got wrong. |
Phase 3 — UWorld Deep Dive (Days 9–12)
| Day | Activity |
|---|---|
| 9 | UWorld block 2 (40 questions). Focus: study design + bias questions. Rewatch BnB video for any topic you miss repeatedly. |
| 10 | UWorld block 3 (40 questions). Focus: 2×2 table, sensitivity/specificity, PPV/NPV. Draw the table for every question even if you know the answer. |
| 11 | Review all marked/incorrect UWorld questions from days 8–10. Redo them without looking at explanations. |
| 12 | Final UWorld block (remaining questions or a random mixed block). Aim for ≥70% by this point. |
Phase 4 — Mastery + Wrap-Up (Days 13–14)
| Day | Activity |
|---|---|
| 13 | Do Amboss biostats questions (20–30) OR redo your weakest UWorld questions. These are harder and sharpen edge cases. |
| 14 | Review your master formula sheet. Timed self-quiz: cover the formula, recall it, write it out. Rest. |
Your Master Formula Sheet (must memorize these cold)
Sensitivity = TP / (TP + FN) → "SnNout" (high Sn rules OUT)
Specificity = TN / (TN + FP) → "SpPin" (high Sp rules IN)
PPV = TP / (TP + FP) → affected by prevalence ↑ → PPV ↑
NPV = TN / (TN + FN) → affected by prevalence ↑ → NPV ↓
RR (cohort) = [a/(a+b)] / [c/(c+d)]
OR (case-ctrl)= (a×d) / (b×c)
AR = Risk(exposed) − Risk(unexposed)
NNT = 1 / ARR
Power = 1 − β (increased by ↑ sample size, ↑ effect size)
P < 0.05 = reject null hypothesis = statistically significant
Most Tested Topics on Step 1 (prioritize these)
- 2×2 table calculations — appears on almost every exam
- Sensitivity vs. specificity — especially screening vs. confirmatory tests
- Study design identification — "which study design is described?"
- Bias recognition — especially lead-time, recall, selection, and observer bias
- NNT/NNH — always appears in clinical scenarios
- Power and sample size — type I vs. type II error
- RR vs. OR — when each is used and how to approximate
Realistic Time Estimate Summary
| Phase | Days | Hours/Day | Total Hours |
|---|---|---|---|
| Foundation (BnB + FA) | 6 | 3–4 | ~21 hrs |
| Consolidation + first UWorld | 2 | 3–4 | ~7 hrs |
| UWorld deep dive | 4 | 3–4 | ~14 hrs |
| Mastery/review | 2 | 3–4 | ~7 hrs |
| Total | 14 days | 3–4 hrs | ~49 hrs |
Key Tips
- Never skip the 2×2 table. Draw it for every question, every time, even when it feels unnecessary. It becomes muscle memory.
- Do UWorld in tutor mode first, then switch to timed mode in Phase 3 to simulate exam conditions.
- Biostats is one of the most reliably scoreable subjects on Step 1 — the formulas do not change. Time invested here directly translates to points.
- If you finish early, spend extra time on bias and study design — these are the most conceptually tricky and commonly missed topics.
make a pdf of above will start after completing neuro
USMLE Step1 Biostatistics StudyPlan
PDF Document · PDF
- Cover page with your profile (beginner, 3–4 hrs/day, 14 days)
- Recommended resources table (BnB, First Aid, UWorld, Amboss)
- Full day-by-day plan — all 4 phases, every day mapped out
- Time estimate summary with total hours
- Master formula sheet — all key formulas with mnemonics
- Colour-coded 2×2 table (TP/TN in green, FP/FN in red)
- Top 7 highest-yield topics ranked by frequency
- Key tips section with common traps
- Reminder note to start after completing Neuro
so there are almost 5 questions on multiple sclerosis checking differently i want to add all together as a pdf and you can make HY superconsice notes asusal okay ?