Skin rashes in an 55 year old diabetic male taking metformin since last 8 years
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Searching Images
granuloma annulare annular plaques forearm diabetes
Reading File
Finding Sources
Reading File
Reading File
Now I have comprehensive information. Let me compile a thorough clinical answer.
Clinical Assessment: Annular Erythematous Plaques in a 55-Year-Old Diabetic Male
Morphological Analysis of the Image
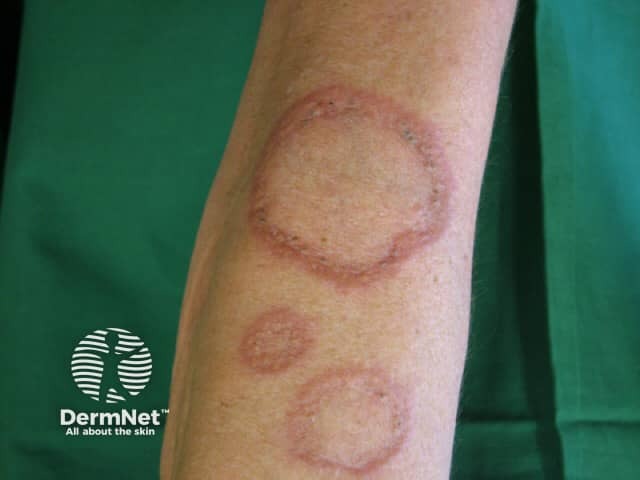
The photograph shows multiple erythematous to violaceous, annular (ring-shaped) plaques with central clearing distributed on the forearm. The lesions have raised, well-defined borders with a beaded/arcuate configuration. No significant scale, vesicles, or exudate are visible. This is the classic morphology of Granuloma Annulare (GA).
Most Likely Diagnosis: Granuloma Annulare (GA)
"The typical history is of one or more papules with centrifugal enlargement and central clearing. These annular lesions are often misdiagnosed as tinea corporis and treated unsuccessfully with topical antifungal agents." — Fitzpatrick's Dermatology, p. 595
Association with Diabetes Mellitus
This patient's 8-year history of Type 2 diabetes is highly relevant:
"Development of granuloma annulare in patients with diabetes mellitus is extensively documented... Localized and generalized as well as subcutaneous nodular and perforating forms have been observed. The histopathologic similarity between granuloma annulare and necrobiosis lipoidica diabeticorum and the coexistence of both conditions in occasional diabetic patients suggest a true association." — Fitzpatrick's Dermatology, p. 596
GA is listed among diabetes-associated skin conditions without a fully understood pathogenesis, alongside necrobiosis lipoidica and diabetic dermopathy — Fitzpatrick's Dermatology, p. 594
Metformin — Drug Reaction Consideration
GA-like drug reactions are documented with several agents. Metformin is not a commonly reported cause of classical GA; however, an interstitial granulomatous drug reaction (a distinct entity that can mimic GA) has been linked to various medications. The 8-year duration on metformin without prior rash makes a primary drug reaction less likely, but cannot be entirely excluded.
"Granuloma annulare-like drug reactions are reported for gold therapy and treatment with allopurinol, diclofenac, quinidine, intranasal calcitonin, topiramate, amlodipine, and thalidomide... An interstitial granulomatous drug reaction linked to the use of [various medications] is considered a distinct entity but may mimic granuloma annulare." — Fitzpatrick's Dermatology, p. 596
Also worth noting: Long-term metformin use causes Vitamin B12 deficiency in ~30% of patients, which can contribute to skin changes and neuropathic symptoms — though this does not produce annular plaques.
Differential Diagnosis
| Category | Conditions |
|---|---|
| Most likely | Granuloma annulare |
| Consider | Tinea corporis (ringworm), Necrobiosis lipoidica diabeticorum, Annular lichen planus |
| Rule out | Subacute cutaneous lupus, Erythema chronicum migrans (Lyme), Annular sarcoidosis, Interstitial granulomatous drug reaction |
| Infections | Tinea (KOH scraping needed), Secondary syphilis, Atypical mycobacteria |
Table adapted from Fitzpatrick's Dermatology, Table 34-1, p. 598
Recommended Workup
- Skin biopsy — confirmatory; shows palisading granulomatous inflammation with mucin deposition and necrobiotic collagen in the dermis
- KOH scrape — to exclude tinea corporis
- HbA1c / fasting glucose — assess glycemic control (poor control may worsen GA)
- Lipid panel — dyslipidemia is associated with generalized GA
- Serum B12 — rule out metformin-induced deficiency
- ANA / dsDNA — if lupus is suspected
- Consider VDRL/RPR if risk factors for syphilis are present
Treatment Options
"The usual treatment options include awaiting spontaneous resolution, topical steroids, and intralesional steroids." — Fitzpatrick's Dermatology, p. 599
| Approach | Agent |
|---|---|
| First line | Await spontaneous resolution (majority resolve within 2 years) |
| Topical | Potent topical corticosteroids ± occlusion; tacrolimus 0.1% ointment; pimecrolimus cream |
| Intralesional | Triamcinolone 2.5 mg/mL |
| Systemic (refractory) | Antimalarials (hydroxychloroquine), retinoids, dapsone, cyclosporine |
| Other | Phototherapy (PUVA/NB-UVB), cryotherapy, pulsed dye laser |
Key Clinical Points
- GA is usually asymptomatic — mild pruritus may occur
- Most localized cases self-resolve within 2 years without sequelae
- Generalized GA runs a more protracted course and warrants systemic workup
- Optimizing glycemic control is important, as diabetes may be a contributing factor
- Do not treat empirically with antifungals — often done mistakenly in GA
⚠️ This is clinical decision support based on dermatology textbooks. A formal in-person evaluation, skin biopsy, and KOH preparation are necessary to confirm the diagnosis before initiating treatment.
This is a shared conversation. Sign in to Orris to start your own chat.